Ebola, also known as Ebola virus disease (EVD) and Ebola hemorrhagic fever (EHF), is a
viral hemorrhagic fever
Viral hemorrhagic fevers (VHFs) are a diverse group of animal and human illnesses in which fever and hemorrhage are caused by a viral infection. VHFs may be caused by five distinct families of RNA viruses: the families '' Filoviridae'', ''Flav ...
in humans and other
primate
Primates are a diverse order of mammals. They are divided into the strepsirrhines, which include the lemurs, galagos, and lorisids, and the haplorhines, which include the tarsiers and the simians (monkeys and apes, the latter including huma ...
s, caused by
ebolavirus
The genus ''Ebolavirus'' (- or ; - or ) is a virological taxon included in the family '' Filoviridae'' (filament-shaped viruses), order ''Mononegavirales''. The members of this genus are called ebolaviruses, and encode their genome in the for ...
es.
[ Symptoms typically start anywhere between two days and three weeks after becoming infected with the virus. The first symptoms are usually ]fever
Fever, also referred to as pyrexia, is defined as having a body temperature, temperature above the human body temperature, normal range due to an increase in the body's temperature Human body temperature#Fever, set point. There is not a single ...
, sore throat
Sore throat, also known as throat pain, is pain or irritation of the throat. Usually, causes of sore throat include
* viral infections
* group A streptococcal infection (GAS) bacterial infection
* pharyngitis (inflammation of the throat)
* to ...
, muscle pain
Myalgia (also called muscle pain and muscle ache in layman's terms) is the medical term for muscle pain. Myalgia is a symptom of many diseases. The most common cause of acute myalgia is the overuse of a muscle or group of muscles; another like ...
, and headache
Headache is the symptom of pain in the face, head, or neck. It can occur as a migraine, tension-type headache, or cluster headache. There is an increased risk of depression in those with severe headaches.
Headaches can occur as a result ...
s.[ These are usually followed by ]vomiting
Vomiting (also known as emesis and throwing up) is the involuntary, forceful expulsion of the contents of one's stomach through the mouth and sometimes the nose.
Vomiting can be the result of ailments like food poisoning, gastroenteri ...
, diarrhoea
Diarrhea, also spelled diarrhoea, is the condition of having at least three loose, liquid, or watery bowel movements each day. It often lasts for a few days and can result in dehydration due to fluid loss. Signs of dehydration often begin wi ...
, rash
A rash is a change of the human skin which affects its color, appearance, or texture.
A rash may be localized in one part of the body, or affect all the skin. Rashes may cause the skin to change color, itch, become warm, bumpy, chapped, dry, cr ...
and decreased liver
The liver is a major Organ (anatomy), organ only found in vertebrates which performs many essential biological functions such as detoxification of the organism, and the Protein biosynthesis, synthesis of proteins and biochemicals necessary for ...
and kidney
The kidneys are two reddish-brown bean-shaped organs found in vertebrates. They are located on the left and right in the retroperitoneal space, and in adult humans are about in length. They receive blood from the paired renal arteries; blood ...
function,[ at which point, some people begin to bleed both internally and externally.][ Death is often due to shock from fluid loss, and typically occurs between six and 16 days after the first symptoms appear.]body fluid
Body fluids, bodily fluids, or biofluids, sometimes body liquids, are liquids within the human body. In lean healthy adult men, the total body water is about 60% (60–67%) of the total body weight; it is usually slightly lower in women (52-55% ...
s, such as blood
Blood is a body fluid in the circulatory system of humans and other vertebrates that delivers necessary substances such as nutrients and oxygen to the cells, and transports metabolic waste products away from those same cells. Blood in the c ...
from infected humans or other animals,[ or from contact with items that have recently been contaminated with infected body fluids.][ There have been no documented cases, either in nature or under laboratory conditions, of the disease spreading through the air between humans or other ]primate
Primates are a diverse order of mammals. They are divided into the strepsirrhines, which include the lemurs, galagos, and lorisids, and the haplorhines, which include the tarsiers and the simians (monkeys and apes, the latter including huma ...
s.semen
Semen, also known as seminal fluid, is an organic bodily fluid created to contain spermatozoa. It is secreted by the gonads (sexual glands) and other sexual organs of male or hermaphroditic animals and can fertilize the female ovum. Semen i ...
or breast milk
Breast milk (sometimes spelled as breastmilk) or mother's milk is milk produced by mammary glands located in the breast of a human female. Breast milk is the primary source of nutrition for newborns, containing fat, protein, carbohydrates ( lacto ...
may continue to carry the virus for anywhere between several weeks to several months.Fruit bat
Megabats constitute the family Pteropodidae of the order Chiroptera (bats). They are also called fruit bats, Old World fruit bats, or—especially the genera '' Acerodon'' and ''Pteropus''—flying foxes. They are the only member of the ...
s are believed to be the normal carrier in nature; they are able to spread the virus without being affected by it.[ The symptoms of Ebola may resemble those of several other diseases, including ]malaria
Malaria is a mosquito-borne infectious disease that affects humans and other animals. Malaria causes symptoms that typically include fever, tiredness, vomiting, and headaches. In severe cases, it can cause jaundice, seizures, coma, or death. S ...
, cholera
Cholera is an infection of the small intestine by some strains of the bacterium ''Vibrio cholerae''. Symptoms may range from none, to mild, to severe. The classic symptom is large amounts of watery diarrhea that lasts a few days. Vomiting and ...
, typhoid fever
Typhoid fever, also known as typhoid, is a disease caused by '' Salmonella'' serotype Typhi bacteria. Symptoms vary from mild to severe, and usually begin six to 30 days after exposure. Often there is a gradual onset of a high fever over several ...
, meningitis
Meningitis is acute or chronic inflammation of the protective membranes covering the brain and spinal cord, collectively called the meninges. The most common symptoms are fever, headache, and neck stiffness. Other symptoms include confusion or ...
and other viral hemorrhagic fevers.[ Diagnosis is confirmed by testing blood samples for the presence of viral ]RNA
Ribonucleic acid (RNA) is a polymeric molecule essential in various biological roles in coding, decoding, regulation and expression of genes. RNA and deoxyribonucleic acid ( DNA) are nucleic acids. Along with lipids, proteins, and carbohydra ...
, viral antibodies
An antibody (Ab), also known as an immunoglobulin (Ig), is a large, Y-shaped protein used by the immune system to identify and neutralize foreign objects such as pathogenic bacteria and viruses. The antibody recognizes a unique molecule of the ...
or the virus itself.[ including rapid detection, ]contact tracing
In public health, contact tracing is the process of identifying persons who may have been exposed to an infected person ("contacts") and subsequent collection of further data to assess transmission. By tracing the contacts of infected individua ...
of those exposed, quick access to laboratory services, care for those infected, and proper disposal of the dead through cremation
Cremation is a method of Disposal of human corpses, final disposition of a Cadaver, dead body through Combustion, burning.
Cremation may serve as a funeral or post-funeral rite and as an alternative to burial. In some countries, including India ...
or burial.[ Samples of body fluids and tissues from people with the disease should be handled with extreme caution.][ Prevention measures include wearing proper protective clothing and ]washing hands
Hand washing (or handwashing), also known as hand hygiene, is the act of cleaning one's hands with soap or handwash and water to remove viruses/bacteria/microorganisms, dirt, grease, or other harmful and unwanted substances stuck to the hand ...
when around a person with the disease,[ and limiting the spread of the disease from infected animals to humans – by wearing protective clothing while handling potentially infected bushmeat, and by cooking bushmeat thoroughly before eating it.][ An ]Ebola vaccine
Ebola vaccines are vaccines either approved or in development to prevent Ebola. As of 2022, there are only vaccines against the Zaire ebolavirus. The first vaccine to be approved in the United States was rVSV-ZEBOV in December 2019. It had be ...
was approved in the United States in December 2019.atoltivimab/maftivimab/odesivimab
Atoltivimab/maftivimab/odesivimab, sold under the brand name Inmazeb, is a fixed-dose combination of three monoclonal antibodies for the treatment of '' Zaire ebolavirus'' (Ebola virus). It contains atoltivimab, maftivimab, and odesivimab-eb ...
and ansuvimab
Ansuvimab, sold under the brand name Ebanga, is a monoclonal antibody medication for the treatment of ''Zaire ebolavirus'' (Ebolavirus) infection.
The most common symptoms include fever, tachycardia (fast heart rate), diarrhea, vomiting, hypote ...
) are associated with improved outcomes.[ These include ]oral rehydration therapy
Oral rehydration therapy (ORT) is a type of fluid replacement used to prevent and treat dehydration, especially due to diarrhea. It involves drinking water with modest amounts of sugar and salts, specifically sodium and potassium. Oral rehydrat ...
(drinking slightly sweetened and salty water) or giving intravenous fluids, and treating symptoms.[ In October 2020, Atoltivimab/maftivimab/odesivimab (Inmazeb) was approved for medical use in the United States to treat the disease caused by ''Zaire ebolavirus''.]
History and name
The disease was first identified in 1976, in two simultaneous outbreaks: one in Nzara (a town in South Sudan
South Sudan (; din, Paguot Thudän), officially the Republic of South Sudan ( din, Paankɔc Cuëny Thudän), is a landlocked country in East Africa. It is bordered by Ethiopia, Sudan, Central African Republic, Democratic Republic of the C ...
) and the other in Yambuku
Yambuku is a small village in Mongala Province in northern Democratic Republic of the Congo. It was the center of the first documented outbreak of Ebola virus disease, in 1976, with the World Health Organization identifying a man from Yambuku as ...
(the Democratic Republic of the Congo
The Democratic Republic of the Congo (french: République démocratique du Congo (RDC), colloquially "La RDC" ), informally Congo-Kinshasa, DR Congo, the DRC, the DROC, or the Congo, and formerly and also colloquially Zaire, is a country in ...
), a village near the Ebola River
The Ebola River ( or ), also commonly known by its indigenous name Legbala, is the headstream of the Mongala River, a tributary of the Congo River, in northern Democratic Republic of the Congo. It is roughly in length.
The name ''Ebola'' is a F ...
, from which the disease takes its name.Ebola outbreaks
This list of Ebola outbreaks records the known occurrences of Ebola virus disease, a highly infectious and acutely lethal Virus, viral disease that has afflicted humans and animals primarily in equatorial Africa. The pathogens responsible for ...
occur intermittently in tropical regions of sub-Saharan Africa
Sub-Saharan Africa is, geographically, the area and regions of the continent of Africa that lies south of the Sahara. These include West Africa, East Africa, Central Africa, and Southern Africa. Geopolitically, in addition to the List of sov ...
.[ Between 1976 and 2012, according to the ]World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level of h ...
, there were 24 outbreaks of Ebola resulting in a total of 2,387 cases, and 1,590 deaths.
Signs and symptoms
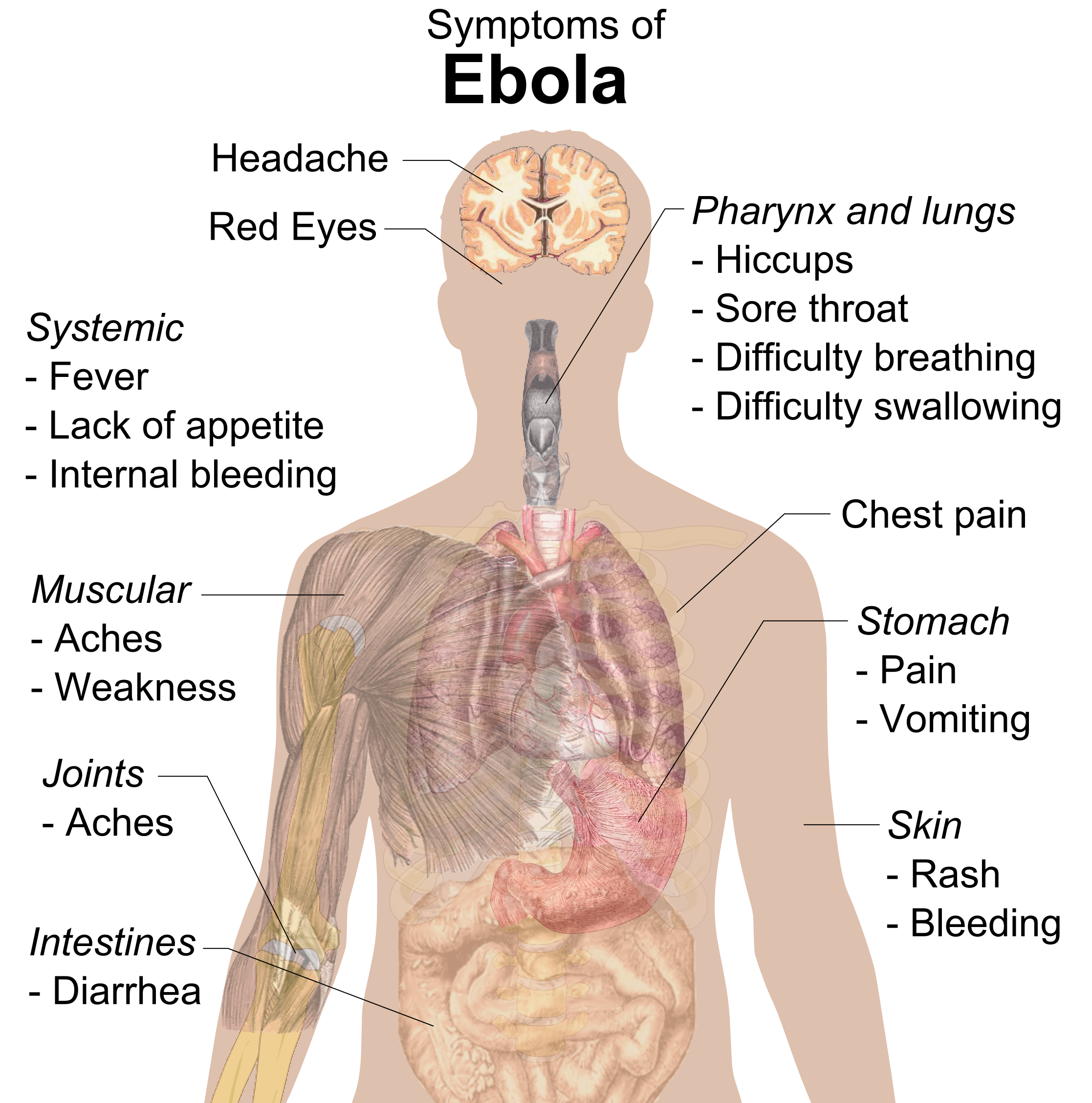
Onset
The length of time between exposure to the virus and the development of symptoms (incubation period
Incubation period (also known as the latent period or latency period) is the time elapsed between exposure to a pathogenic organism, a chemical, or radiation, and when symptoms and signs are first apparent. In a typical infectious disease, the in ...
) is between 2 and 21 days,influenza
Influenza, commonly known as "the flu", is an infectious disease caused by influenza viruses. Symptoms range from mild to severe and often include fever, runny nose, sore throat, muscle pain, headache, coughing, and fatigue. These symptoms ...
-like stage characterised by fatigue, fever
Fever, also referred to as pyrexia, is defined as having a body temperature, temperature above the human body temperature, normal range due to an increase in the body's temperature Human body temperature#Fever, set point. There is not a single ...
, weakness
Weakness is a symptom of a number of different conditions. The causes are many and can be divided into conditions that have true or perceived muscle weakness. True muscle weakness is a primary symptom of a variety of skeletal muscle diseases, i ...
, decreased appetite
Anorexia is a medical term for a loss of appetite. While the term in non-scientific publications is often used interchangeably with anorexia nervosa, many possible causes exist for a loss of appetite, some of which may be harmless, while others ...
, muscular pain, joint pain
Arthralgia (from Greek ''arthro-'', joint + ''-algos'', pain) literally means ''joint pain''. Specifically, arthralgia is a symptom of injury, infection, illness (in particular arthritis), or an allergic reaction to medication.
According to MeSH, ...
, headache, and sore throat.diarrhoea
Diarrhea, also spelled diarrhoea, is the condition of having at least three loose, liquid, or watery bowel movements each day. It often lasts for a few days and can result in dehydration due to fluid loss. Signs of dehydration often begin wi ...
, abdominal pain, and sometimes hiccups
A hiccup (scientific name ''singultus'', from a Latin word meaning "to catch one's breath while sobbing"; also spelled hiccough) is an involuntary contraction (myoclonic jerk) of the diaphragm that may repeat several times per minute. The hic ...
.dehydration
In physiology, dehydration is a lack of total body water, with an accompanying disruption of metabolic processes. It occurs when free water loss exceeds free water intake, usually due to exercise, disease, or high environmental temperature. Mil ...
.shortness of breath
Shortness of breath (SOB), also medically known as dyspnea (in AmE) or dyspnoea (in BrE), is an uncomfortable feeling of not being able to breathe well enough. The American Thoracic Society defines it as "a subjective experience of breathing disc ...
and chest pain may occur, along with swelling, headaches
Headache is the symptom of pain in the face, head, or neck. It can occur as a migraine, tension-type headache, or cluster headache. There is an increased risk of depression in those with severe headaches.
Headaches can occur as a result ...
, and confusion
In medicine, confusion is the quality or state of being bewildered or unclear. The term "acute mental confusion" .[ In about half of the cases, the skin may develop a ]maculopapular rash
A maculopapular rash is a type of rash characterized by a flat, red area on the skin that is covered with small confluent bumps. It may only appear red in lighter-skinned people. The term "maculopapular" is a compound: '' macules'' are small, flat ...
, a flat red area covered with small bumps, five to seven days after symptoms begin.
Bleeding
In some cases, internal and external bleeding may occur.vomiting blood
Hematemesis is the vomiting of blood. It is always an important sign. It can be confused with hemoptysis (coughing up blood) or epistaxis (nosebleed), which are more common. The source is generally the upper gastrointestinal tract, typically abo ...
, coughing up of blood, or blood in stool. Bleeding into the skin may create petechia
A petechia () is a small red or purple spot (≤4 mm in diameter) that can appear on the skin, conjunctiva, retina, and Mucous membrane, mucous membranes which is caused by haemorrhage of capillaries. The word is derived from Italian , 'freckle,' ...
e, purpura
Purpura () is a condition of red or purple discolored spots on the skin that do not blanch on applying pressure. The spots are caused by bleeding underneath the skin secondary to platelet disorders, vascular disorders, coagulation disorders, ...
, ecchymoses
A bruise, also known as a contusion, is a type of hematoma of tissue, the most common cause being capillaries damaged by trauma, causing localized bleeding that extravasates into the surrounding interstitial tissues. Most bruises occur clos ...
or haematomas (especially around needle injection sites).gastrointestinal tract
The gastrointestinal tract (GI tract, digestive tract, alimentary canal) is the tract or passageway of the digestive system that leads from the mouth to the anus. The GI tract contains all the major organ (biology), organs of the digestive syste ...
.
Recovery or death
Recovery may begin between seven and 14 days after first symptoms.[ Death, if it occurs, follows typically six to sixteen days from first symptoms and is often due to shock from fluid loss.][ In general, bleeding often indicates a worse outcome, and blood loss may result in death.]coma
A coma is a deep state of prolonged unconsciousness in which a person cannot be awakened, fails to respond normally to painful stimuli, light, or sound, lacks a normal wake-sleep cycle and does not initiate voluntary actions. Coma patients exhi ...
near the end of life.[
Those who survive often have ongoing muscular and joint pain, liver inflammation, and decreased hearing, and may have continued tiredness, continued weakness, decreased appetite, and difficulty returning to pre-illness weight.]antibodies
An antibody (Ab), also known as an immunoglobulin (Ig), is a large, Y-shaped protein used by the immune system to identify and neutralize foreign objects such as pathogenic bacteria and viruses. The antibody recognizes a unique molecule of the ...
against Ebola that last at least 10 years, but it is unclear whether they are immune to additional infections.
Cause
EVD in humans is caused by four of six viruses of the genus ''Ebolavirus
The genus ''Ebolavirus'' (- or ; - or ) is a virological taxon included in the family '' Filoviridae'' (filament-shaped viruses), order ''Mononegavirales''. The members of this genus are called ebolaviruses, and encode their genome in the for ...
''. The four are Bundibugyo virus (BDBV), Sudan virus (SUDV), Taï Forest virus (TAFV) and one simply called Ebola virus
''Zaire ebolavirus'', more commonly known as Ebola virus (; EBOV), is one of six known species within the genus ''Ebolavirus''. Four of the six known ebolaviruses, including EBOV, cause a severe and often fatal hemorrhagic fever in humans and ot ...
(EBOV, formerly Zaire Ebola virus).Zaire ebolavirus
''Zaire ebolavirus'', more commonly known as Ebola virus (; EBOV), is one of six known species within the genus '' Ebolavirus''. Four of the six known ebolaviruses, including EBOV, cause a severe and often fatal hemorrhagic fever in humans and o ...
'', is the most dangerous of the known EVD-causing viruses, and is responsible for the largest number of outbreaks.Reston virus
Reston virus (RESTV) is one of six known viruses within the genus '' Ebolavirus''. Reston virus causes Ebola virus disease in non-human primates; unlike the other five ebolaviruses, it is not known to cause disease in humans, but has caused asymp ...
(RESTV) and Bombali virus (BOMV), are not thought to cause disease in humans, but have caused disease in other primates.marburgvirus
The genus ''Marburgvirus'' is the taxonomic home of ''Marburg marburgvirus'', whose members are the two known marburgviruses, Marburg virus (MARV) and Ravn virus (RAVV). Both viruses cause Marburg virus disease in humans and nonhuman primate ...
es.
Virology
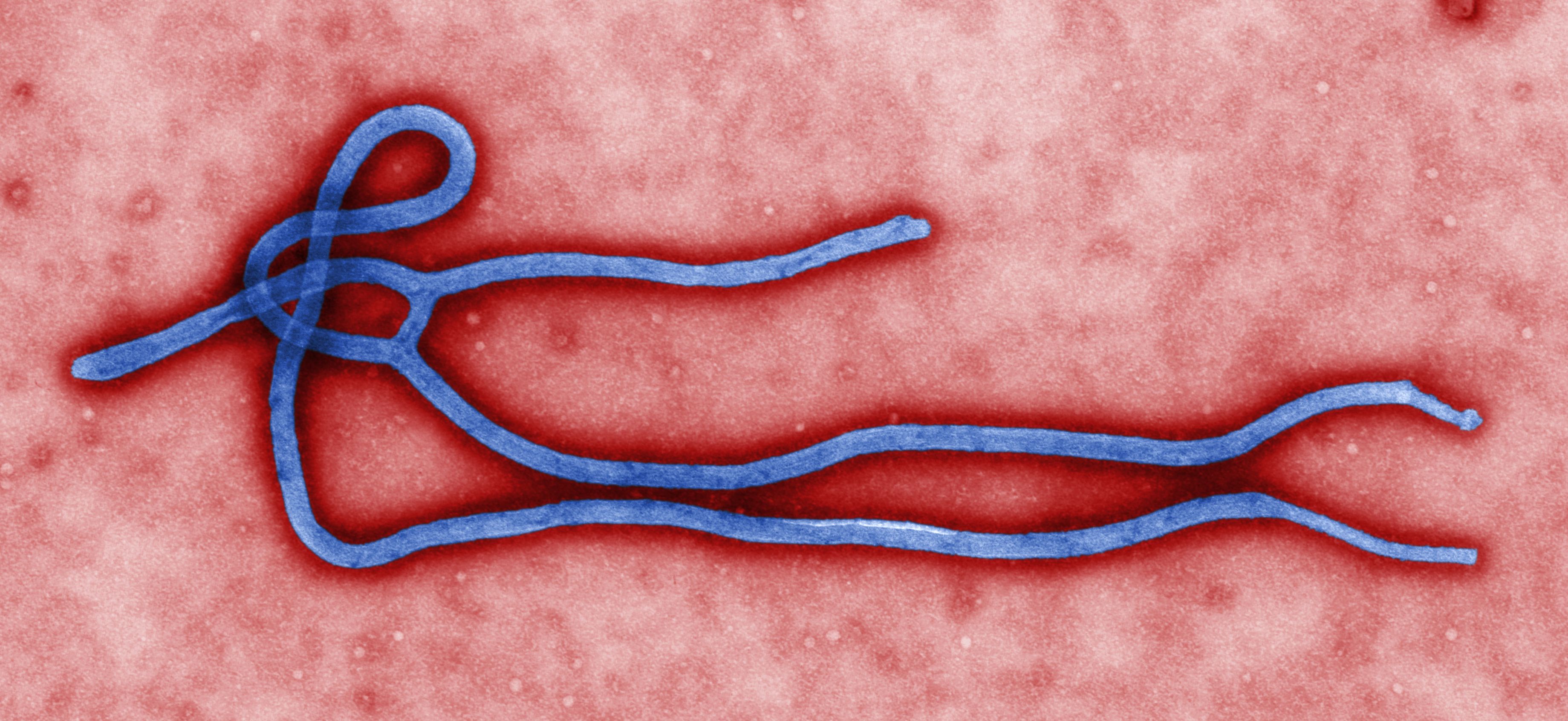 Ebolaviruses contain single-stranded, non-infectious
Ebolaviruses contain single-stranded, non-infectious RNA
Ribonucleic acid (RNA) is a polymeric molecule essential in various biological roles in coding, decoding, regulation and expression of genes. RNA and deoxyribonucleic acid ( DNA) are nucleic acids. Along with lipids, proteins, and carbohydra ...
genome
In the fields of molecular biology and genetics, a genome is all the genetic information of an organism. It consists of nucleotide sequences of DNA (or RNA in RNA viruses). The nuclear genome includes protein-coding genes and non-coding ge ...
s.gene
In biology, the word gene (from , ; "...Wilhelm Johannsen coined the word gene to describe the Mendelian units of heredity..." meaning ''generation'' or ''birth'' or ''gender'') can have several different meanings. The Mendelian gene is a ba ...
s including 3'-UTR-''NP''-''VP35''-''VP40''-''GP''-''VP30''-''VP24''-''L''- 5'-UTR.sequence
In mathematics, a sequence is an enumerated collection of objects in which repetitions are allowed and order matters. Like a set, it contains members (also called ''elements'', or ''terms''). The number of elements (possibly infinite) is calle ...
and the number and location of gene overlaps. As with all filovirus
''Filoviridae'' () is a family of single-stranded negative-sense RNA viruses in the order ''Mononegavirales''. Two members of the family that are commonly known are Ebola virus and Marburg virus. Both viruses, and some of their lesser known re ...
es, ebolavirus virions are filamentous particles that may appear in the shape of a shepherd's crook, of a "U" or of a "6," and they may be coiled, toroid or branched.life cycle
Life cycle, life-cycle, or lifecycle may refer to:
Science and academia
*Biological life cycle, the sequence of life stages that an organism undergoes from birth to reproduction ending with the production of the offspring
* Life-cycle hypothesis ...
is thought to begin with a virion attaching to specific cell-surface receptors
The cell membrane (also known as the plasma membrane (PM) or cytoplasmic membrane, and historically referred to as the plasmalemma) is a biological membrane that separates and protects the interior of all cells from the outside environment ( ...
such as C-type lectin
A C-type lectin (CLEC) is a type of carbohydrate-binding protein known as a lectin. The C-type designation is from their requirement for calcium for binding. Proteins that contain C-type lectin domains have a diverse range of functions including c ...
s, DC-SIGN
DC-SIGN (Dendritic Cell-Specific Intercellular adhesion molecule-3-Grabbing Non-integrin) also known as CD209 ( Cluster of Differentiation 209) is a protein which in humans is encoded by the ''CD209'' gene.
DC-SIGN is a C-type lectin receptor pr ...
, or integrin
Integrins are transmembrane receptors that facilitate cell-cell and cell-extracellular matrix (ECM) adhesion. Upon ligand binding, integrins activate signal transduction pathways that mediate cellular signals such as regulation of the cell cycle, ...
s, which is followed by fusion of the viral envelope with cellular membranes.endosome
Endosomes are a collection of intracellular sorting organelles in eukaryotic cells. They are parts of endocytic membrane transport pathway originating from the trans Golgi network. Molecules or ligands internalized from the plasma membrane can ...
s and lysosome
A lysosome () is a membrane-bound organelle found in many animal cells. They are spherical vesicles that contain hydrolytic enzymes that can break down many kinds of biomolecules. A lysosome has a specific composition, of both its membrane pr ...
s where the viral envelope glycoprotein GP is cleaved.RNA polymerase
In molecular biology, RNA polymerase (abbreviated RNAP or RNApol), or more specifically DNA-directed/dependent RNA polymerase (DdRP), is an enzyme that synthesizes RNA from a DNA template.
Using the enzyme helicase, RNAP locally opens the ...
, encoded by the ''L'' gene, partially uncoats the nucleocapsid and transcribes the genes into positive-strand mRNA
In molecular biology, messenger ribonucleic acid (mRNA) is a single-stranded molecule of RNA that corresponds to the genetic sequence of a gene, and is read by a ribosome in the process of Protein biosynthesis, synthesizing a protein.
mRNA is ...
s, which are then translated
Translation is the communication of the meaning of a source-language text by means of an equivalent target-language text. The English language draws a terminological distinction (which does not exist in every language) between ''transla ...
into structural and nonstructural proteins. The most abundant protein produced is the nucleoprotein, whose concentration in the host cell determines when L switches from gene transcription to genome replication. Replication of the viral genome results in full-length, positive-strand antigenomes that are, in turn, transcribed into genome copies of negative-strand virus progeny.cell membrane
The cell membrane (also known as the plasma membrane (PM) or cytoplasmic membrane, and historically referred to as the plasmalemma) is a biological membrane that separates and protects the interior of all cells from the outside environment ( ...
. Virions bud
In botany, a bud is an undeveloped or embryonic shoot and normally occurs in the axil of a leaf or at the tip of a stem. Once formed, a bud may remain for some time in a dormant condition, or it may form a shoot immediately. Buds may be spec ...
off from the cell, gaining their envelopes from the cellular membrane from which they bud. The mature progeny particles then infect other cells to repeat the cycle. The genetics of the Ebola virus are difficult to study because of EBOV's virulent characteristics.
Transmission
 It is believed that between people, Ebola disease spreads only by direct contact with the blood or other
It is believed that between people, Ebola disease spreads only by direct contact with the blood or other body fluid
Body fluids, bodily fluids, or biofluids, sometimes body liquids, are liquids within the human body. In lean healthy adult men, the total body water is about 60% (60–67%) of the total body weight; it is usually slightly lower in women (52-55% ...
s of a person who has developed symptoms of the disease.semen
Semen, also known as seminal fluid, is an organic bodily fluid created to contain spermatozoa. It is secreted by the gonads (sexual glands) and other sexual organs of male or hermaphroditic animals and can fertilize the female ovum. Semen i ...
.[ The WHO states that only people who are very sick are able to spread Ebola disease in ]saliva
Saliva (commonly referred to as spit) is an extracellular fluid produced and secreted by salivary glands in the mouth. In humans, saliva is around 99% water, plus electrolytes, mucus, white blood cells, epithelial cells (from which DNA can be ...
, and the virus has not been reported to be transmitted through sweat. Most people spread the virus through blood, feces and vomit. Entry points for the virus include the nose, mouth, eyes, open wounds, cuts and abrasions.droplets
A drop or droplet is a small column of liquid, bounded completely or almost completely by free surfaces. A drop may form when liquid accumulates at the lower end of a tube or other surface boundary, producing a hanging drop called a pendant d ...
; however, this is believed to occur only when a person is very sick.[ Contact with surfaces or objects contaminated by the virus, particularly needles and syringes, may also transmit the infection.][
The Ebola virus may be able to persist for more than three months in the semen after recovery, which could lead to infections via ]sexual intercourse
Sexual intercourse (or coitus or copulation) is a sexual activity typically involving the insertion and thrusting of the penis into the vagina for sexual pleasure or reproduction.Sexual intercourse most commonly means penile–vaginal penetrat ...
.[ Virus persistence in semen for over a year has been recorded in a national screening programme. Ebola may also occur in the breast milk of women after recovery, and it is not known when it is safe to breastfeed again.][ The virus was also found in the eye of one patient in 2014, two months after it was cleared from his blood. Otherwise, people who have recovered are not infectious.][
The potential for widespread infections in countries with medical systems capable of observing correct medical isolation procedures is considered low.]embalming
Embalming is the art and science of preserving human remains by treating them (in its modern form with chemicals) to forestall decomposition. This is usually done to make the deceased suitable for public or private viewing as part of the funeral ...
are at risk.[ Of the cases of Ebola infections in Guinea during the 2014 outbreak, 69% are believed to have been contracted via unprotected (or unsuitably protected) contact with infected corpses during certain Guinean burial rituals.][ This risk is particularly common in parts of Africa where the disease mostly occurs and health systems function poorly. There has been transmission in hospitals in some African countries that reuse hypodermic needles. Some health-care centres caring for people with the disease do not have running water.][ and airborne transmission has only been demonstrated in very strict laboratory conditions, and then only from pigs to primates, but not from primates to primates.][ Other possible methods of transmission are being studied.]
Initial case
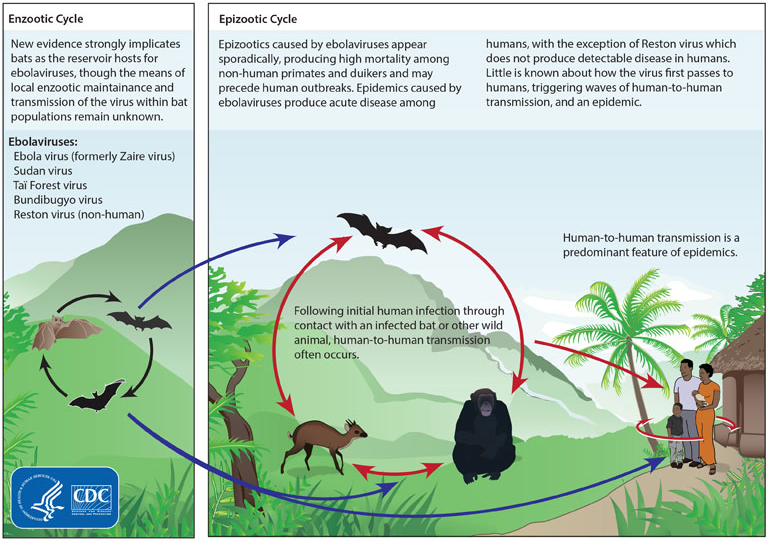
 Although it is not entirely clear how Ebola initially spreads from animals to humans, the spread is believed to involve direct contact with an infected wild animal or fruit bat.
Although it is not entirely clear how Ebola initially spreads from animals to humans, the spread is believed to involve direct contact with an infected wild animal or fruit bat.[ Besides bats, other wild animals that are sometimes infected with EBOV include several species of monkeys such as ]baboon
Baboons are primates comprising the genus ''Papio'', one of the 23 genera of Old World monkeys. There are six species of baboon: the hamadryas baboon, the Guinea baboon, the olive baboon, the yellow baboon, the Kinda baboon and the chacma ba ...
s, great apes
The Hominidae (), whose members are known as the great apes or hominids (), are a taxonomic family of primates that includes eight extant species in four genera: '' Pongo'' (the Bornean, Sumatran and Tapanuli orangutan); ''Gorilla'' (the ...
( chimpanzees and gorilla
Gorillas are herbivorous, predominantly ground-dwelling great apes that inhabit the tropical forests of equatorial Africa. The genus ''Gorilla'' is divided into two species: the eastern gorilla and the western gorilla, and either four or fi ...
s), and duikers
A duiker is a small to medium-sized brown antelope native to sub-Saharan Africa, found in heavily wooded areas. The 22 extant species, including three sometimes considered to be subspecies of the other species, form the subfamily Cephalophinae ...
(a species of antelope
The term antelope is used to refer to many species of even-toed ruminant that are indigenous to various regions in Africa and Eurasia.
Antelope comprise a wastebasket taxon defined as any of numerous Old World grazing and browsing hoofed mammals ...
).[ Fruit production, animal behavior and other factors may trigger outbreaks among animal populations.]
Reservoir
The natural reservoir
In infectious disease ecology and epidemiology, a natural reservoir, also known as a disease reservoir or a reservoir of infection, is the population of organisms or the specific environment in which an infectious pathogen naturally lives and r ...
for Ebola has yet to be confirmed; however, bat
Bats are mammals of the order Chiroptera.''cheir'', "hand" and πτερόν''pteron'', "wing". With their forelimbs adapted as wings, they are the only mammals capable of true and sustained flight. Bats are more agile in flight than most ...
s are considered to be the most likely candidate.Hypsignathus monstrosus
The hammer-headed bat ('), also known as hammer-headed fruit bat and big-lipped bat, is a megabat widely distributed in West and Central Africa. It is the only member of the genus ''Hypsignathus'', which is part of the tribe Epomophorini along w ...
'', ''Epomops franqueti
Franquet's epauletted fruit bat (''Epomops franqueti'') is a species of megabat in the family Pteropodidae, and is one of three different species of epauletted bats. Franquet's epauletted fruit bat has a range of habitats, varying from Subsaharan ...
'' and ''Myonycteris torquata
''Myonycteris'' (collared bat) is a genus of bat in the family Pteropodidae.
It contains the following species:Simmons, 2005, p. 328
Genus ''Myonycteris''
* São Tomé collared fruit bat, ''Myonycteris brachycephala''
* East African little ...
'') were found to possibly carry the virus without getting sick. , whether other animals are involved in its spread is not known.arthropod
Arthropods (, (gen. ποδός)) are invertebrate animals with an exoskeleton, a Segmentation (biology), segmented body, and paired jointed appendages. Arthropods form the phylum Arthropoda. They are distinguished by their jointed limbs and Arth ...
s, rodent
Rodents (from Latin , 'to gnaw') are mammals of the order Rodentia (), which are characterized by a single pair of continuously growing incisors in each of the upper and lower jaws. About 40% of all mammal species are rodents. They are na ...
s, and birds have also been considered possible viral reservoirs.Gabon
Gabon (; ; snq, Ngabu), officially the Gabonese Republic (french: République gabonaise), is a country on the west coast of Central Africa. Located on the equator, it is bordered by Equatorial Guinea to the northwest, Cameroon to the north ...
and the Republic of the Congo
The Republic of the Congo (french: République du Congo, ln, Republíki ya Kongó), also known as Congo-Brazzaville, the Congo Republic or simply either Congo or the Congo, is a country located in the western coast of Central Africa to the w ...
, immunoglobulin G (IgG) immune defense molecules indicative of Ebola infection were found in three bat species; at various periods of study, between 2.2 and 22.6% of bats were found to contain both RNA sequences and IgG molecules indicating Ebola infection. Antibodies against Zaire and Reston viruses have been found in fruit bats in Bangladesh
Bangladesh (}, ), officially the People's Republic of Bangladesh, is a country in South Asia. It is the eighth-most populous country in the world, with a population exceeding 165 million people in an area of . Bangladesh is among the mos ...
, suggesting that these bats are also potential hosts of the virus and that the filoviruses are present in Asia.arthropod
Arthropods (, (gen. ποδός)) are invertebrate animals with an exoskeleton, a Segmentation (biology), segmented body, and paired jointed appendages. Arthropods form the phylum Arthropoda. They are distinguished by their jointed limbs and Arth ...
s sampled from regions of EBOV outbreaks, no Ebola virus was detected apart from some genetic traces found in six rodents (belonging to the species '' Mus setulosus'' and ''Praomys
''Praomys'' is a genus of rodent in the family Muridae endemic to Sub-Saharan Africa. It contains the following species:
* '' Praomys coetzeei''
* Dalton's mouse, ''Praomys daltoni''
* De Graaff's soft-furred mouse, ''Praomys degraaffi''
* Der ...
'') and one shrew
Shrews (family Soricidae) are small mole-like mammals classified in the order Eulipotyphla. True shrews are not to be confused with treeshrews, otter shrews, elephant shrews, West Indies shrews, or marsupial shrews, which belong to different fa ...
('' Sylvisorex ollula'') collected from the Central African Republic
The Central African Republic (CAR; ; , RCA; , or , ) is a landlocked country in Central Africa. It is bordered by Chad to the north, Sudan to the northeast, South Sudan to the southeast, the DR Congo to the south, the Republic of th ...
.Deforestation
Deforestation or forest clearance is the removal of a forest or stand of trees from land that is then converted to non-forest use. Deforestation can involve conversion of forest land to farms, ranches, or urban use. The most concentrated d ...
has been mentioned as a possible contributor to recent outbreaks, including the West African Ebola virus epidemic
The 2013–2016 epidemic of Ebola virus disease, centered in Western Africa, was the most widespread outbreak of the disease in history. It caused major loss of life and socioeconomic disruption in the region, mainly in Guinea, Liberia and S ...
. Index cases of EVD have often been close to recently deforested lands.
Pathophysiology
 Like other
Like other filoviruses
''Filoviridae'' () is a family of single-stranded negative-sense RNA viruses in the order ''Mononegavirales''. Two members of the family that are commonly known are Ebola virus and Marburg virus. Both viruses, and some of their lesser known re ...
, EBOV replicates very efficiently in many cells, producing large amounts of virus in monocyte
Monocytes are a type of leukocyte or white blood cell. They are the largest type of leukocyte in blood and can differentiate into macrophages and conventional dendritic cells. As a part of the vertebrate innate immune system monocytes also ...
s, macrophage
Macrophages (abbreviated as M φ, MΦ or MP) ( el, large eaters, from Greek ''μακρός'' (') = large, ''φαγεῖν'' (') = to eat) are a type of white blood cell of the immune system that engulfs and digests pathogens, such as cancer cel ...
s, dendritic cells and other cells including liver cells
A hepatocyte is a cell of the main parenchymal tissue of the liver. Hepatocytes make up 80% of the liver's mass.
These cells are involved in:
* Protein synthesis
* Protein storage
* Transformation of carbohydrates
* Synthesis of cholesterol, ...
, fibroblasts, and adrenal gland cells.endothelial cells
The endothelium is a single layer of squamous endothelial cells that line the interior surface of blood vessels and lymphatic vessels. The endothelium forms an interface between circulating blood or lymph in the lumen and the rest of the vessel ...
(cells lining the inside of blood vessels), liver cells, and several types of immune cells such as macrophages, monocytes, and dendritic cells are the main targets of attack.lymph node
A lymph node, or lymph gland, is a kidney-shaped organ of the lymphatic system and the adaptive immune system. A large number of lymph nodes are linked throughout the body by the lymphatic vessels. They are major sites of lymphocytes that inclu ...
s where further reproduction of the virus takes place.lymphatic system
The lymphatic system, or lymphoid system, is an organ system in vertebrates that is part of the immune system, and complementary to the circulatory system. It consists of a large network of lymphatic vessels, lymph nodes, lymphatic or lymphoid o ...
and spread throughout the body.programmed cell death
Programmed cell death (PCD; sometimes referred to as cellular suicide) is the death of a cell (biology), cell as a result of events inside of a cell, such as apoptosis or autophagy. PCD is carried out in a biological process, which usually confers ...
.white blood cell
White blood cells, also called leukocytes or leucocytes, are the cell (biology), cells of the immune system that are involved in protecting the body against both infectious disease and foreign invaders. All white blood cells are produced and de ...
s, such as lymphocyte
A lymphocyte is a type of white blood cell (leukocyte) in the immune system of most vertebrates. Lymphocytes include natural killer cells (which function in cell-mediated, cytotoxic innate immunity), T cells (for cell-mediated, cytotoxic ad ...
s, also undergo programmed cell death leading to an abnormally low concentration of lymphocytes in the blood.blood vessel
The blood vessels are the components of the circulatory system that transport blood throughout the human body. These vessels transport blood cells, nutrients, and oxygen to the tissues of the body. They also take waste and carbon dioxide away ...
injury can be attributed to EBOV glycoprotein
Glycoproteins are proteins which contain oligosaccharide chains covalently attached to amino acid side-chains. The carbohydrate is attached to the protein in a cotranslational or posttranslational modification. This process is known as glycos ...
s. This damage occurs due to the synthesis of Ebola virus glycoprotein
Glycoproteins are proteins which contain oligosaccharide chains covalently attached to amino acid side-chains. The carbohydrate is attached to the protein in a cotranslational or posttranslational modification. This process is known as glycos ...
(GP), which reduces the availability of specific integrin
Integrins are transmembrane receptors that facilitate cell-cell and cell-extracellular matrix (ECM) adhesion. Upon ligand binding, integrins activate signal transduction pathways that mediate cellular signals such as regulation of the cell cycle, ...
s responsible for cell adhesion to the intercellular structure and causes liver damage, leading to improper clotting. The widespread bleeding
Bleeding, hemorrhage, haemorrhage or blood loss, is blood escaping from the circulatory system from damaged blood vessels. Bleeding can occur internally, or externally either through a natural opening such as the mouth, nose, ear, urethra, vag ...
that occurs in affected people causes swelling and shock due to loss of blood volume.coagulation cascade
Coagulation, also known as clotting, is the process by which blood changes from a liquid to a gel, forming a blood clot. It potentially results in hemostasis, the cessation of blood loss from a damaged vessel, followed by repair. The mechanism ...
due to excessive tissue factor production by macrophages and monocytes.glycoprotein
Glycoproteins are proteins which contain oligosaccharide chains covalently attached to amino acid side-chains. The carbohydrate is attached to the protein in a cotranslational or posttranslational modification. This process is known as glycos ...
, small soluble glycoprotein (sGP or GP) is synthesised. EBOV replication overwhelms protein synthesis of infected cells and the host immune defences. The GP forms a trimeric complex, which tethers the virus to the endothelial cells. The sGP forms a dimeric protein that interferes with the signalling of neutrophils, another type of white blood cell. This enables the virus to evade the immune system by inhibiting early steps of neutrophil activation.
Immune system evasion
Filoviral infection also interferes with proper functioning of the innate immune system.interferon-alpha
The type-I interferons (IFN) are cytokines which play essential roles in inflammation, immunoregulation, tumor cells recognition, and T-cell responses. In the human genome, a cluster of thirteen functional IFN genes is located at the 9p21.3 cyt ...
, interferon-beta
The type-I interferons (IFN) are cytokines which play essential roles in inflammation, immunoregulation, tumor cells recognition, and T-cell responses. In the human genome, a cluster of thirteen functional IFN genes is located at the 9p21.3 cyto ...
, and interferon gamma
Interferon gamma (IFN-γ) is a dimerized soluble cytokine that is the only member of the type II class of interferons. The existence of this interferon, which early in its history was known as immune interferon, was described by E. F. Wheeloc ...
.cytosol
The cytosol, also known as cytoplasmic matrix or groundplasm, is one of the liquids found inside cells (intracellular fluid (ICF)). It is separated into compartments by membranes. For example, the mitochondrial matrix separates the mitochondri ...
(such as RIG-I
RIG-I (retinoic acid-inducible gene I) is a cytosolic pattern recognition receptor (PRR) responsible for the type-1 interferon (IFN1) response. RIG-I is an essential molecule in the innate immune system for recognizing cells that have been infect ...
and MDA5
MDA5 (melanoma differentiation-associated protein 5) is a RIG-I-like receptor dsRNA helicase enzyme that is encoded by the ''IFIH1'' gene in humans. MDA5 is part of the RIG-I-like receptor (RLR) family, which also includes RIG-I and LGP2, and ...
) or outside of the cytosol (such as Toll-like receptor 3 (TLR3), TLR7
Toll-like receptor 7, also known as TLR7, is a protein that in humans is encoded by the ''TLR7'' gene. Orthologs are found in mammals and birds. It is a member of the toll-like receptor (TLR) family and detects single stranded RNA.
Function
T ...
, TLR8
Toll-like receptor 8 is a protein that in humans is encoded by the ''TLR8'' gene. TLR8 has also been designated as CD288 (cluster of differentiation 288). It is a member of the toll-like receptor (TLR) family.
Function
TLR8 seems to function d ...
and TLR9
Toll-like receptor 9 is a protein that in humans is encoded by the ''TLR9'' gene. TLR9 has also been designated as CD289 (cluster of differentiation 289). It is a member of the toll-like receptor (TLR) family. TLR9 is an important receptor expresse ...
) recognise infectious molecules associated with the virus.IFNAR1
Interferon-alpha/beta receptor alpha chain is a protein that in humans is encoded by the ''IFNAR1'' gene.
Function
The protein encoded by this gene is a type I membrane protein that forms one of the two chains of a receptor for type I interfer ...
and IFNAR2
Interferon-alpha/beta receptor beta chain is a protein that in humans is encoded by the ''IFNAR2'' gene.
Function
The protein encoded by this gene is a type I membrane protein that forms one of the two chains of a receptor for interferons al ...
receptors expressed on the surface of a neighbouring cell.STAT1
Signal transducer and activator of transcription 1 (STAT1) is a transcription factor which in humans is encoded by the ''STAT1'' gene. It is a member of the STAT protein family.
Function
All STAT molecules are phosphorylated by receptor associ ...
and STAT2 are activated and move to the cell's nucleus.
Diagnosis
When EVD is suspected, travel, work history, and exposure to wildlife are important factors with respect to further diagnostic efforts.
Laboratory testing
Possible non-specific laboratory indicators of EVD include a low platelet count; an initially decreased white blood cell count followed by an increased white blood cell count; elevated levels of the liver enzymes alanine aminotransferase
Alanine transaminase (ALT) is a transaminase enzyme (). It is also called alanine aminotransferase (ALT or ALAT) and was formerly called serum glutamate-pyruvate transaminase or serum glutamic-pyruvic transaminase (SGPT) and was first character ...
(ALT) and aspartate aminotransferase
Aspartate transaminase (AST) or aspartate aminotransferase, also known as AspAT/ASAT/AAT or (serum) glutamic oxaloacetic transaminase (GOT, SGOT), is a pyridoxal phosphate (PLP)-dependent transaminase enzyme () that was first described by Arthur ...
(AST); and abnormalities in blood clotting often consistent with disseminated intravascular coagulation (DIC) such as a prolonged prothrombin time
The prothrombin time (PT) – along with its derived measures of prothrombin ratio (PR) and international normalized ratio (INR) – is an assay for evaluating the ''extrinsic'' pathway and common pathway of coagulation. This blood test is als ...
, partial thromboplastin time
The partial thromboplastin time (PTT), also known as the activated partial thromboplastin time (aPTT or APTT), is a blood test that characterizes coagulation of the blood. A historical name for this measure is the kaolin-cephalin clotting time ( ...
, and bleeding time
Bleeding time is a medical test done on someone to assess their platelets function. It involves making a patient bleed, then timing how long it takes for them to stop bleeding using a stopwatch or other suitable devices.
The term template bleedin ...
.RNA
Ribonucleic acid (RNA) is a polymeric molecule essential in various biological roles in coding, decoding, regulation and expression of genes. RNA and deoxyribonucleic acid ( DNA) are nucleic acids. Along with lipids, proteins, and carbohydra ...
or proteins, or detecting antibodies
An antibody (Ab), also known as an immunoglobulin (Ig), is a large, Y-shaped protein used by the immune system to identify and neutralize foreign objects such as pathogenic bacteria and viruses. The antibody recognizes a unique molecule of the ...
against the virus in a person's blood.[ Isolating the virus by ]cell culture
Cell culture or tissue culture is the process by which cells are grown under controlled conditions, generally outside of their natural environment. The term "tissue culture" was coined by American pathologist Montrose Thomas Burrows. This te ...
, detecting the viral RNA by polymerase chain reaction
The polymerase chain reaction (PCR) is a method widely used to rapidly make millions to billions of copies (complete or partial) of a specific DNA sample, allowing scientists to take a very small sample of DNA and amplify it (or a part of it) t ...
(PCR)enzyme-linked immunosorbent assay
The enzyme-linked immunosorbent assay (ELISA) (, ) is a commonly used analytical biochemistry assay, first described by Eva Engvall and Peter Perlmann in 1971. The assay uses a solid-phase type of enzyme immunoassay (EIA) to detect the presence ...
(ELISA) are methods best used in the early stages of the disease and also for detecting the virus in human remains.[ Detecting antibodies against the virus is most reliable in the later stages of the disease and in those who recover.]IgG antibodies
Immunoglobulin G (Ig G) is a type of antibody. Representing approximately 75% of serum antibodies in humans, IgG is the most common type of antibody found in blood circulation. IgG molecules are created and released by plasma B cells. Each IgG ...
can be detected six to 18 days after symptom onset.real-time PCR
A real-time polymerase chain reaction (real-time PCR, or qPCR) is a laboratory technique of molecular biology based on the polymerase chain reaction (PCR). It monitors the amplification of a targeted DNA molecule during the PCR (i.e., in real ...
and ELISA.[ It is able to confirm Ebola in 92% of those affected and rule it out in 85% of those not affected.]
Differential diagnosis
Early symptoms of EVD may be similar to those of other diseases common in Africa, including malaria
Malaria is a mosquito-borne infectious disease that affects humans and other animals. Malaria causes symptoms that typically include fever, tiredness, vomiting, and headaches. In severe cases, it can cause jaundice, seizures, coma, or death. S ...
and dengue fever.Marburg virus disease
Marburg virus disease (MVD; formerly Marburg hemorrhagic fever) is a viral hemorrhagic fever in humans and primates caused by either of the two Marburgviruses: Marburg virus (MARV) and Ravn virus (RAVV). Its clinical symptoms are very similar t ...
, Crimean–Congo haemorrhagic fever, and Lassa fever
Lassa fever, also known as Lassa hemorrhagic fever (LHF), is a type of viral hemorrhagic fever caused by the Lassa virus. Many of those infected by the virus do not develop symptoms. When symptoms occur they typically include fever, weakness, ...
.differential diagnosis
In healthcare, a differential diagnosis (abbreviated DDx) is a method of analysis of a patient's history and physical examination to arrive at the correct diagnosis. It involves distinguishing a particular disease or condition from others that p ...
is extensive and requires consideration of many other infectious diseases such as typhoid fever
Typhoid fever, also known as typhoid, is a disease caused by '' Salmonella'' serotype Typhi bacteria. Symptoms vary from mild to severe, and usually begin six to 30 days after exposure. Often there is a gradual onset of a high fever over several ...
, shigellosis
Shigellosis is an infection of the intestines caused by ''Shigella'' bacteria. Symptoms generally start one to two days after exposure and include diarrhea, fever, abdominal pain, and feeling the need to pass stools even when the bowels are emp ...
, rickettsial diseases, cholera
Cholera is an infection of the small intestine by some strains of the bacterium ''Vibrio cholerae''. Symptoms may range from none, to mild, to severe. The classic symptom is large amounts of watery diarrhea that lasts a few days. Vomiting and ...
, sepsis
Sepsis, formerly known as septicemia (septicaemia in British English) or blood poisoning, is a life-threatening condition that arises when the body's response to infection causes injury to its own tissues and organs. This initial stage is follo ...
, borreliosis
Lyme disease, also known as Lyme borreliosis, is a vector-borne disease caused by the ''Borrelia'' bacterium, which is spread by ticks in the genus ''Ixodes''. The most common sign of infection is an expanding red rash, known as erythema migran ...
, EHEC enteritis, leptospirosis, scrub typhus
Scrub typhus or bush typhus is a form of typhus caused by the intracellular parasite '' Orientia tsutsugamushi'', a Gram-negative α-proteobacterium of family Rickettsiaceae first isolated and identified in 1930 in Japan.[plague
Plague or The Plague may refer to:
Agriculture, fauna, and medicine
*Plague (disease), a disease caused by ''Yersinia pestis''
* An epidemic of infectious disease (medical or agricultural)
* A pandemic caused by such a disease
* A swarm of pe ...]
, Q fever
Q fever or query fever is a disease caused by infection with ''Coxiella burnetii'', a bacterium that affects humans and other animals. This organism is uncommon, but may be found in cattle, sheep, goats, and other domestic mammals, including ...
, candidiasis
Candidiasis is a fungal infection due to any type of '' Candida'' (a type of yeast). When it affects the mouth, in some countries it is commonly called thrush. Signs and symptoms include white patches on the tongue or other areas of the mouth ...
, histoplasmosis
Histoplasmosis is a fungal infection caused by '' Histoplasma capsulatum''. Symptoms of this infection vary greatly, but the disease affects primarily the lungs. Occasionally, other organs are affected; called disseminated histoplasmosis, it can ...
, trypanosomiasis
Trypanosomiasis or trypanosomosis is the name of several diseases in vertebrates caused by parasitic protozoan trypanosomes of the genus ''Trypanosoma''. In humans this includes African trypanosomiasis and Chagas disease. A number of other diseas ...
, visceral
In biology, an organ is a collection of tissues joined in a structural unit to serve a common function. In the hierarchy of life, an organ lies between tissue and an organ system. Tissues are formed from same type cells to act together in a ...
leishmaniasis, measles, and viral hepatitis
Viral hepatitis is liver inflammation due to a viral infection. It may present in acute form as a recent infection with relatively rapid onset, or in chronic form.
The most common causes of viral hepatitis are the five unrelated hepatotropic vi ...
among others.
Non-infectious diseases that may result in symptoms similar to those of EVD include acute promyelocytic leukaemia, haemolytic uraemic syndrome
Hemolysis or haemolysis (), also known by several other names, is the rupturing ( lysis) of red blood cells (erythrocytes) and the release of their contents (cytoplasm) into surrounding fluid (e.g. blood plasma). Hemolysis may occur in vivo ...
, snake envenomation
A snakebite is an injury caused by the bite of a snake, especially a venomous snake. A common sign of a bite from a venomous snake is the presence of two puncture wounds from the animal's fangs. Sometimes venom injection from the bite may occu ...
, clotting factor deficiencies/platelet disorders, thrombotic thrombocytopenic purpura
Thrombotic thrombocytopenic purpura (TTP) is a blood disorder that results in blood clots forming in small blood vessels throughout the body. This results in a low platelet count, low red blood cells due to their breakdown, and often kidney, h ...
, hereditary haemorrhagic telangiectasia
Hereditary hemorrhagic telangiectasia (HHT), also known as Osler–Weber–Rendu disease and Osler–Weber–Rendu syndrome, is a rare autosomal dominant genetic disorder that leads to abnormal blood vessel formation in the skin, mucous membranes, ...
, Kawasaki disease
Kawasaki disease is a syndrome of unknown cause that results in a fever and mainly affects children under 5 years of age. It is a form of vasculitis, where blood vessels become inflamed throughout the body. The fever typically lasts for more th ...
, and warfarin
Warfarin, sold under the brand name Coumadin among others, is a medication that is used as an anticoagulant (blood thinner). It is commonly used to prevent blood clots such as deep vein thrombosis and pulmonary embolism, and to prevent st ...
poisoning.
Prevention
Vaccines
An Ebola vaccine
Ebola vaccines are vaccines either approved or in development to prevent Ebola. As of 2022, there are only vaccines against the Zaire ebolavirus. The first vaccine to be approved in the United States was rVSV-ZEBOV in December 2019. It had be ...
, rVSV-ZEBOV
Recombinant vesicular stomatitis virus–Zaire Ebola virus (rVSV-ZEBOV), also known as Ebola Zaire vaccine live and sold under the brand name Ervebo, is an Ebola vaccine for adults that prevents Ebola caused by the Zaire ebolavirus. When used ...
, was approved in the United States in December 2019.[ It was studied in Guinea between 2014 and 2016.][ More than 100,000 people have been vaccinated against Ebola .
]
Infection control
 Community awareness of the benefits on survival chances of admitting cases early is important for the infected and infection control
Community awareness of the benefits on survival chances of admitting cases early is important for the infected and infection control
Caregivers
 People who care for those infected with Ebola should wear protective clothing including masks, gloves, gowns and goggles.
People who care for those infected with Ebola should wear protective clothing including masks, gloves, gowns and goggles.[ The U.S. ]Centers for Disease Control
The Centers for Disease Control and Prevention (CDC) is the national public health agency of the United States. It is a United States federal agency, under the Department of Health and Human Services, and is headquartered in Atlanta, Georgi ...
(CDC) recommend that the protective gear leaves no skin exposed.[ These measures are also recommended for those who may handle objects contaminated by an infected person's body fluids.][ In 2014, the CDC began recommending that medical personnel receive training on the proper suit-up and removal of ]personal protective equipment
Personal protective equipment (PPE) is protective clothing, helmets, goggles, or other garments or equipment designed to protect the wearer's body from injury or infection. The hazards addressed by protective equipment include physical, elec ...
(PPE); in addition, a designated person, appropriately trained in biosafety, should be watching each step of these procedures to ensure they are done correctly.
Patients and household members
The infected person should be in barrier-isolation from other people.[ All equipment, medical waste, patient waste and surfaces that may have come into contact with body fluids need to be ]disinfected
A disinfectant is a chemical substance or compound used to inactivate or destroy microorganisms on inert surfaces. Disinfection does not necessarily kill all microorganisms, especially resistant bacterial spores; it is less effective than st ...
.Doctors Without Borders
Doctor or The Doctor may refer to:
Personal titles
* Doctor (title), the holder of an accredited academic degree
* A medical practitioner, including:
** Physician
** Surgeon
** Dentist
** Veterinary physician
** Optometrist
*Other roles
** ...
.
Disinfection
Ebolaviruses can be eliminated with heat (heating for 30 to 60 minutes at 60 °C or boiling for five minutes). To disinfect
A disinfectant is a chemical substance or compound used to inactivate or destroy microorganisms on inert surfaces. Disinfection does not necessarily kill all microorganisms, especially resistant bacterial spores; it is less effective than ste ...
surfaces, some lipid solvents such as some alcohol-based products, detergents, sodium hypochlorite (bleach) or calcium hypochlorite
Calcium hypochlorite is an inorganic compound with formula Ca(OCl)2. It is the main active ingredient of commercial products called bleaching powder, chlorine powder, or chlorinated lime, used for water treatment and as a bleaching agent. Thi ...
(bleaching powder), and other suitable disinfectants may be used at appropriate concentrations.
General population
Education of the general public about the risk factors for Ebola infection and of the protective measures individuals may take to prevent infection is recommended by the World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level of h ...
.[ These measures include avoiding direct contact with infected people and regular ]hand washing
Hand washing (or handwashing), also known as hand hygiene, is the act of cleaning one's hands with soap or handwash and water to remove viruses/bacteria/microorganisms, dirt, grease, or other harmful and unwanted substances stuck to the hands ...
using soap and water.
Bushmeat
Bushmeat, an important source of protein in the diet of some Africans, should be handled and prepared with appropriate protective clothing and thoroughly cooked before consumption.[ Some research suggests that an outbreak of Ebola disease in the wild animals used for consumption may result in a corresponding human outbreak. Since 2003, such animal outbreaks have been monitored to predict and prevent Ebola outbreaks in humans.]
Corpses, burial
If a person with Ebola disease dies, direct contact with the body should be avoided.
Transport, travel, contact
Transportation crews are instructed to follow a certain isolation procedure, should anyone exhibit symptoms resembling EVD.[ In October 2014, the CDC defined four risk levels used to determine the level of 21-day monitoring for symptoms and restrictions on public activities.][
* having been in a country with widespread Ebola disease transmission and having no known exposure (low risk); or having been in that country more than 21 days ago (no risk)
* encounter with a person showing symptoms; but not within three feet of the person with Ebola without wearing PPE; and no direct contact with body fluids
* having had brief skin contact with a person showing symptoms of Ebola disease when the person was believed to be not very contagious (low risk)
* in countries without widespread Ebola disease transmission: direct contact with a person showing symptoms of the disease while wearing PPE (low risk)
* contact with a person with Ebola disease before the person was showing symptoms (no risk).
The CDC recommends monitoring for the symptoms of Ebola disease for those both at "low risk" and at higher risk.][
]
Laboratory
In laboratories where diagnostic testing is carried out, biosafety level 4-equivalent containment is required.[
]
Isolation
Isolation refers to separating those who are sick from those who are not. Quarantine
A quarantine is a restriction on the movement of people, animals and goods which is intended to prevent the spread of disease or pests. It is often used in connection to disease and illness, preventing the movement of those who may have been ...
refers to separating those who may have been exposed to a disease until they either show signs of the disease or are no longer at risk. Quarantine, also known as enforced isolation, is usually effective in decreasing spread.
Contact tracing
Contact tracing
In public health, contact tracing is the process of identifying persons who may have been exposed to an infected person ("contacts") and subsequent collection of further data to assess transmission. By tracing the contacts of infected individua ...
is considered important to contain an outbreak. It involves finding everyone who had close contact with infected individuals and monitoring them for signs of illness for 21 days. If any of these contacts comes down with the disease, they should be isolated, tested and treated. Then the process is repeated, tracing the contacts' contacts.
Management
two treatments (atoltivimab/maftivimab/odesivimab
Atoltivimab/maftivimab/odesivimab, sold under the brand name Inmazeb, is a fixed-dose combination of three monoclonal antibodies for the treatment of '' Zaire ebolavirus'' (Ebola virus). It contains atoltivimab, maftivimab, and odesivimab-eb ...
and ansuvimab
Ansuvimab, sold under the brand name Ebanga, is a monoclonal antibody medication for the treatment of ''Zaire ebolavirus'' (Ebolavirus) infection.
The most common symptoms include fever, tachycardia (fast heart rate), diarrhea, vomiting, hypote ...
) are associated with improved outcomes.[ The U.S. ]Food and Drug Administration
The United States Food and Drug Administration (FDA or US FDA) is a List of United States federal agencies, federal agency of the United States Department of Health and Human Services, Department of Health and Human Services. The FDA is respon ...
(FDA) advises people to be careful of advertisements making unverified or fraudulent claims of benefits supposedly gained from various anti-Ebola products.Food and Drug Administration
The United States Food and Drug Administration (FDA or US FDA) is a List of United States federal agencies, federal agency of the United States Department of Health and Human Services, Department of Health and Human Services. The FDA is respon ...
(FDA) approved atoltivimab/maftivimab/odesivimab with an indication for the treatment of infection caused by ''Zaire ebolavirus''.[ ]
Standard support
 Treatment is primarily supportive in nature.
Treatment is primarily supportive in nature.[ Rehydration may be via the ]oral
The word oral may refer to:
Relating to the mouth
* Relating to the mouth, the first portion of the alimentary canal that primarily receives food and liquid
**Oral administration of medicines
** Oral examination (also known as an oral exam or or ...
or intravenous
Intravenous therapy (abbreviated as IV therapy) is a medical technique that administers fluids, medications and nutrients directly into a person's vein. The intravenous route of administration is commonly used for rehydration or to provide nutrie ...
route.[ These measures may include ]pain management
Pain management is an aspect of medicine and health care involving relief of pain (pain relief, analgesia, pain control) in various dimensions, from acute and simple to chronic and challenging. Most physicians and other health professionals pr ...
, and treatment for nausea
Nausea is a diffuse sensation of unease and discomfort, sometimes perceived as an urge to vomit. While not painful, it can be a debilitating symptom if prolonged and has been described as placing discomfort on the chest, abdomen, or back of the ...
, fever
Fever, also referred to as pyrexia, is defined as having a body temperature, temperature above the human body temperature, normal range due to an increase in the body's temperature Human body temperature#Fever, set point. There is not a single ...
, and anxiety
Anxiety is an emotion which is characterized by an unpleasant state of inner turmoil and includes feelings of dread over anticipated events. Anxiety is different than fear in that the former is defined as the anticipation of a future threat wh ...
.[ The ]World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level of h ...
(WHO) recommends avoiding aspirin
Aspirin, also known as acetylsalicylic acid (ASA), is a nonsteroidal anti-inflammatory drug (NSAID) used to reduce pain, fever, and/or inflammation, and as an antithrombotic. Specific inflammatory conditions which aspirin is used to treat inc ...
or ibuprofen for pain management, due to the risk of bleeding associated with these medications.
Blood products such as packed red blood cells
Packed red blood cells, also known as packed cells, are red blood cells that have been separated for blood transfusion. The packed cells are typically used in anemia that is either causing symptoms or when the hemoglobin is less than usually 70� ...
, platelet
Platelets, also called thrombocytes (from Greek θρόμβος, "clot" and κύτος, "cell"), are a component of blood whose function (along with the coagulation factors) is to react to bleeding from blood vessel injury by clumping, thereby ini ...
s, or fresh frozen plasma
Fresh frozen plasma (FFP) is a blood product made from the liquid portion of whole blood. It is used to treat conditions in which there are low blood clotting factors (INR > 1.5) or low levels of other blood proteins. It may also be used as the re ...
may also be used.[ Other regulators of coagulation have also been tried including heparin in an effort to prevent disseminated intravascular coagulation and ]clotting factors
Coagulation, also known as clotting, is the process by which blood changes from a liquid to a gel, forming a blood clot. It potentially results in hemostasis, the cessation of blood loss from a damaged vessel, followed by repair. The mechanism o ...
to decrease bleeding.[ ]Antimalarial medication
Antimalarial medications or simply antimalarials are a type of antiparasitic chemical agent, often naturally derived, that can be used to treat or to prevent malaria, in the latter case, most often aiming at two susceptible target groups, young c ...
s and antibiotics
An antibiotic is a type of antimicrobial substance active against bacteria. It is the most important type of antibacterial agent for fighting bacterial infections, and antibiotic medications are widely used in the treatment and prevention o ...
are often used before the diagnosis is confirmed,[ though there is no evidence to suggest such treatment helps. Several experimental treatments are being studied.]
Intensive care
Intensive care
Intensive care medicine, also called critical care medicine, is a medical specialty that deals with seriously or critically ill patients who have, are at risk of, or are recovering from conditions that may be life-threatening. It includes pro ...
is often used in the developed world.kidney failure
Kidney failure, also known as end-stage kidney disease, is a medical condition in which the kidneys can no longer adequately filter waste products from the blood, functioning at less than 15% of normal levels. Kidney failure is classified as eit ...
, and extracorporeal membrane oxygenation may be used for lung dysfunction.
Prognosis
EVD has a risk of death in those infected of between 25% and 90%.Republic of the Congo
The Republic of the Congo (french: République du Congo, ln, Republíki ya Kongó), also known as Congo-Brazzaville, the Congo Republic or simply either Congo or the Congo, is a country located in the western coast of Central Africa to the w ...
outbreak.
Early admission significantly increases survival rates
Death, if it occurs, follows typically six to sixteen days after symptoms appear and is often due to low blood pressure from fluid loss.[ Early supportive care to prevent dehydration may reduce the risk of death.]miscarriage
Miscarriage, also known in medical terms as a spontaneous abortion and pregnancy loss, is the death of an embryo or fetus before it is able to survive independently. Miscarriage before 6 weeks of gestation is defined by ESHRE as biochemical lo ...
s, skin peeling, or hair loss
Hair loss, also known as alopecia or baldness, refers to a loss of hair from part of the head or body. Typically at least the head is involved. The severity of hair loss can vary from a small area to the entire body. Inflammation or scar ...
.light sensitivity Photosensitivity is the amount to which an object reacts upon receiving photons, especially visible light. In medicine, the term is principally used for abnormal reactions of the skin, and two types are distinguished, photoallergy and phototoxicity ...
, excess tearing, and vision loss
Visual impairment, also known as vision impairment, is a medical definition primarily measured based on an individual's better eye visual acuity; in the absence of treatment such as correctable eyewear, assistive devices, and medical treatment� ...
have been described.
Ebola can stay in some body parts like the eyes,meningitis
Meningitis is acute or chronic inflammation of the protective membranes covering the brain and spinal cord, collectively called the meninges. The most common symptoms are fever, headache, and neck stiffness. Other symptoms include confusion or ...
has been reported many months after recovery, .
A study of 44 survivors of the Ebola virus in Sierra Leone
Sierra Leone,)]. officially the Republic of Sierra Leone, is a country on the southwest coast of West Africa. It is bordered by Liberia to the southeast and Guinea surrounds the northern half of the nation. Covering a total area of , Sierra ...
reported musculoskeletal pain in 70%, headache in 48%, and eye problems in 14%.
Epidemiology
The disease typically occurs in outbreaks in tropical regions of Sub-Saharan Africa
Sub-Saharan Africa is, geographically, the area and regions of the continent of Africa that lies south of the Sahara. These include West Africa, East Africa, Central Africa, and Southern Africa. Geopolitically, in addition to the List of sov ...
.Ebola virus epidemic in West Africa
The 2013–2016 epidemic of Ebola virus disease, centered in Western Africa, was the most widespread outbreak of the disease in history. It caused major loss of life and socioeconomic disruption in the region, mainly in Guinea, Liberia and S ...
, which caused a large number of deaths in Guinea
Guinea ( ),, fuf, 𞤘𞤭𞤲𞤫, italic=no, Gine, wo, Gine, nqo, ߖߌ߬ߣߍ߫, bm, Gine officially the Republic of Guinea (french: République de Guinée), is a coastal country in West Africa. It borders the Atlantic Ocean to the we ...
, Sierra Leone
Sierra Leone,)]. officially the Republic of Sierra Leone, is a country on the southwest coast of West Africa. It is bordered by Liberia to the southeast and Guinea surrounds the northern half of the nation. Covering a total area of , Sierra ...
, and Liberia
Liberia (), officially the Republic of Liberia, is a country on the West African coast. It is bordered by Sierra Leone to Liberia–Sierra Leone border, its northwest, Guinea to its north, Ivory Coast to its east, and the Atlantic Ocean ...
.
1976
Sudan
 The first known outbreak of EVD was identified only after the fact. It occurred between June and November 1976, in
The first known outbreak of EVD was identified only after the fact. It occurred between June and November 1976, in Nzara, South Sudan
Nzara is a town in Western Equatoria State. It lies to the northwest of Yambio by road, and is 25 km (15m) from the border with the DR Congo.
Nzara was industrial center of the Azande Scheme also known as, Equatoria Project Scheme duri ...
Sudan
Sudan ( or ; ar, السودان, as-Sūdān, officially the Republic of the Sudan ( ar, جمهورية السودان, link=no, Jumhūriyyat as-Sūdān), is a country in Northeast Africa. It shares borders with the Central African Republic t ...
), and was caused by Sudan virus (SUDV). The Sudan outbreak infected 284 people and killed 151. The first identifiable case in Sudan occurred on 27 June in a storekeeper in a cotton factory in Nzara, who was hospitalised on 30 June and died on 6 July.Zaire
Zaire (, ), officially the Republic of Zaire (french: République du Zaïre, link=no, ), was a Congolese state from 1971 to 1997 in Central Africa that was previously and is now again known as the Democratic Republic of the Congo. Zaire was, ...
.
Zaire
 On 26 August 1976, the second outbreak of EVD began in
On 26 August 1976, the second outbreak of EVD began in Yambuku
Yambuku is a small village in Mongala Province in northern Democratic Republic of the Congo. It was the center of the first documented outbreak of Ebola virus disease, in 1976, with the World Health Organization identifying a man from Yambuku as ...
, a small rural village in Mongala District
Mongala District (french: District du Mongala, nl, District Mongala) was a district of the Belgian Congo and the Democratic Republic of the Congo. It went through various changes in extent. It covered roughly the same area as the present Mongala ...
in northern Zaire
Zaire (, ), officially the Republic of Zaire (french: République du Zaïre, link=no, ), was a Congolese state from 1971 to 1997 in Central Africa that was previously and is now again known as the Democratic Republic of the Congo. Zaire was, ...
(now known as the Democratic Republic of the Congo
The Democratic Republic of the Congo (french: République démocratique du Congo (RDC), colloquially "La RDC" ), informally Congo-Kinshasa, DR Congo, the DRC, the DROC, or the Congo, and formerly and also colloquially Zaire, is a country in ...
).genus
Genus ( plural genera ) is a taxonomic rank used in the biological classification of extant taxon, living and fossil organisms as well as Virus classification#ICTV classification, viruses. In the hierarchy of biological classification, genus com ...
''Ebolavirus'' than in the first Sudan outbreak. The first person infected with the disease was the village school's headmaster Mabalo Lokela, who began displaying symptoms on 26 August 1976.Central African Republic
The Central African Republic (CAR; ; , RCA; , or , ) is a landlocked country in Central Africa. It is bordered by Chad to the north, Sudan to the northeast, South Sudan to the southeast, the DR Congo to the south, the Republic of th ...
, after visiting the Ebola River
The Ebola River ( or ), also commonly known by its indigenous name Legbala, is the headstream of the Mongala River, a tributary of the Congo River, in northern Democratic Republic of the Congo. It is roughly in length.
The name ''Ebola'' is a F ...
between 12 and 22 August. He was originally believed to have malaria
Malaria is a mosquito-borne infectious disease that affects humans and other animals. Malaria causes symptoms that typically include fever, tiredness, vomiting, and headaches. In severe cases, it can cause jaundice, seizures, coma, or death. S ...
and was given quinine
Quinine is a medication used to treat malaria and babesiosis. This includes the treatment of malaria due to '' Plasmodium falciparum'' that is resistant to chloroquine when artesunate is not available. While sometimes used for nocturnal le ...
. However, his symptoms continued to worsen, and he was admitted to Yambuku Mission Hospital on 5 September. Lokela died on 8 September 14 days after he began displaying symptoms.Mobutu Sese Seko
Mobutu Sese Seko Kuku Ngbendu Wa Za Banga (; born Joseph-Désiré Mobutu; 14 October 1930 – 7 September 1997) was a Congolese politician and military officer who was the president of Zaire from 1965 to 1997 (known as the Democratic Republic o ...
declared the entire region, including Yambuku and the country's capital, Kinshasa
Kinshasa (; ; ln, Kinsásá), formerly Léopoldville ( nl, Leopoldstad), is the capital and largest city of the Democratic Republic of the Congo. Once a site of fishing and trading villages situated along the Congo River, Kinshasa is now one o ...
, a quarantine zone. No-one was permitted to enter or leave the area, and roads, waterways, and airfields were placed under martial law
Martial law is the imposition of direct military control of normal civil functions or suspension of civil law by a government, especially in response to an emergency where civil forces are overwhelmed, or in an occupied territory.
Use
Marti ...
. Schools, businesses and social organisations were closed.Jean-Jacques Muyembe-Tamfum
Jean-Jacques Muyembe is a Congolese microbiologist. He is the general director of the Democratic Republic of the Congo Institut National pour la Recherche Biomedicale (''INRB''). He was part of team at the Yambuku Catholic Mission Hospital that ...
, one of the discoverers of Ebola. Muyembe took a blood sample from a Belgian nun; this sample would eventually be used by Peter Piot
Sir Peter Karel, Baron Piot, (born 17 February 1949) is a Belgian-British microbiologist known for his research into Ebola and AIDS.
After helping discover the Ebola virus in 1976 and leading efforts to contain the first-ever recorded Ebola epi ...
to identify the previously unknown Ebola virus. Muyembe was also the first scientist to come into direct contact with the disease and survive. Researchers from the Centers for Disease Control and Prevention
The Centers for Disease Control and Prevention (CDC) is the national public health agency of the United States. It is a United States federal agency, under the Department of Health and Human Services, and is headquartered in Atlanta, Georgi ...
(CDC), including Piot, co-discoverer of Ebola, later arrived to assess the effects of the outbreak, observing that "the whole region was in panic."[
During this outbreak, Ngoy Mushola recorded the first clinical description of EVD in ]Yambuku
Yambuku is a small village in Mongala Province in northern Democratic Republic of the Congo. It was the center of the first documented outbreak of Ebola virus disease, in 1976, with the World Health Organization identifying a man from Yambuku as ...
, where he wrote the following in his daily log: "The illness is characterised with a high temperature of about , haematemesis
Hematemesis is the vomiting of blood. It is always an important sign. It can be confused with hemoptysis (coughing up blood) or epistaxis (nosebleed), which are more common. The source is generally the upper gastrointestinal tract, typically abo ...
, diarrhoea with blood, retrosternal abdominal pain, prostration with 'heavy' articulations, and rapid evolution death after a mean of three days."
The virus responsible for the initial outbreak, first thought to be the Marburg virus
Marburg virus (MARV) is a hemorrhagic fever virus of the ''Filoviridae'' family of viruses and a member of the species '' Marburg marburgvirus'', genus ''Marburgvirus''. It causes Marburg virus disease in primates, a form of viral hemorrhagic f ...
, was later identified as a new type of virus related to the genus ''Marburgvirus
The genus ''Marburgvirus'' is the taxonomic home of ''Marburg marburgvirus'', whose members are the two known marburgviruses, Marburg virus (MARV) and Ravn virus (RAVV). Both viruses cause Marburg virus disease in humans and nonhuman primate ...
''. Virus strain samples isolated from both outbreaks were named "Ebola virus" after the Ebola River
The Ebola River ( or ), also commonly known by its indigenous name Legbala, is the headstream of the Mongala River, a tributary of the Congo River, in northern Democratic Republic of the Congo. It is roughly in length.
The name ''Ebola'' is a F ...
, near the first-identified viral outbreak site in Zaire.[ Reports conflict about who initially coined the name: either Karl Johnson of the American CDC team][
]
1995–2014
 The second major outbreak occurred in Zaire (now the
The second major outbreak occurred in Zaire (now the Democratic Republic of the Congo
The Democratic Republic of the Congo (french: République démocratique du Congo (RDC), colloquially "La RDC" ), informally Congo-Kinshasa, DR Congo, the DRC, the DROC, or the Congo, and formerly and also colloquially Zaire, is a country in ...
, DRC), in 1995, affecting 315 and killing 254.Uganda
}), is a landlocked country in East Africa
East Africa, Eastern Africa, or East of Africa, is the eastern subregion of the African continent. In the United Nations Statistics Division scheme of geographic regions, 10-11-(16*) territor ...
had an outbreak infecting 425 and killing 224; in this case, the Sudan virus was found to be the Ebola species responsible for the outbreak.genus
Genus ( plural genera ) is a taxonomic rank used in the biological classification of extant taxon, living and fossil organisms as well as Virus classification#ICTV classification, viruses. In the hierarchy of biological classification, genus com ...
''Ebolavirus'' outbreak to date.Bundibugyo District
Bundibugyo District is a district in the Western Region of Uganda, bordering the Democratic Republic of the Congo (DRC). The town of Bundibugyo is where both the district headquarters and the Bwamba Kingdom seat ( Obudhingiya Bwa Bwamba) are l ...
in Western Uganda. After confirming samples tested by the United States National Reference Laboratories and the Centers for Disease Control, the World Health Organization (WHO) confirmed the presence of a new species of genus
Genus ( plural genera ) is a taxonomic rank used in the biological classification of extant taxon, living and fossil organisms as well as Virus classification#ICTV classification, viruses. In the hierarchy of biological classification, genus com ...
''Ebolavirus'', which was tentatively named Bundibugyo. The WHO reported 149 cases of this new strain and 37 of those led to deaths.bush meat
Bushmeat is meat from wildlife species that are hunted for human consumption, most often referring to the meat of game in Africa. Bushmeat represents
a primary source of animal protein and a cash-earning commodity for inhabitants of humid tro ...
hunted by local villagers around the towns of Isiro and Viadana.EBOV
''Zaire ebolavirus'', more commonly known as Ebola virus (; EBOV), is one of six known species within the genus ''Ebolavirus''. Four of the six known ebolaviruses, including EBOV, cause a severe and often fatal hemorrhagic fever in humans and ot ...
species, the Zaire species.Zaire
Zaire (, ), officially the Republic of Zaire (french: République du Zaïre, link=no, ), was a Congolese state from 1971 to 1997 in Central Africa that was previously and is now again known as the Democratic Republic of the Congo. Zaire was, ...
.
2013–2016 West Africa
 In March 2014, the
In March 2014, the World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level of h ...
(WHO) reported a major Ebola outbreak in Guinea
Guinea ( ),, fuf, 𞤘𞤭𞤲𞤫, italic=no, Gine, wo, Gine, nqo, ߖߌ߬ߣߍ߫, bm, Gine officially the Republic of Guinea (french: République de Guinée), is a coastal country in West Africa. It borders the Atlantic Ocean to the we ...
, a West African nation.[
] The disease rapidly spread to the neighbouring countries of Liberia
Liberia (), officially the Republic of Liberia, is a country on the West African coast. It is bordered by Sierra Leone to Liberia–Sierra Leone border, its northwest, Guinea to its north, Ivory Coast to its east, and the Atlantic Ocean ...
and Sierra Leone
Sierra Leone,)]. officially the Republic of Sierra Leone, is a country on the southwest coast of West Africa. It is bordered by Liberia to the southeast and Guinea surrounds the northern half of the nation. Covering a total area of , Sierra ...
. It was the largest Ebola outbreak ever documented, and the first recorded in the region.Doctors Without Borders
Doctor or The Doctor may refer to:
Personal titles
* Doctor (title), the holder of an accredited academic degree
* A medical practitioner, including:
** Physician
** Surgeon
** Dentist
** Veterinary physician
** Optometrist
*Other roles
** ...
reported the situation in Liberia's capital, Monrovia
Monrovia () is the capital city of the West African country of Liberia. Founded in 1822, it is located on Cape Mesurado on the Atlantic coast and as of the 2008 census had 1,010,970 residents, home to 29% of Liberia’s total population. As the ...
, was "catastrophic" and "deteriorating daily". They reported that fears of Ebola among staff members and patients had shut down much of the city's health system, leaving many people without medical treatment for other conditions. In September 2014, it was estimated that the countries' capacity for treating Ebola patients was insufficient by the equivalent of 2,122 beds; by December there were a sufficient number of beds to treat and isolate all reported Ebola cases, although the uneven distribution of cases was causing serious shortfalls in some areas.
In September 2014, it was estimated that the countries' capacity for treating Ebola patients was insufficient by the equivalent of 2,122 beds; by December there were a sufficient number of beds to treat and isolate all reported Ebola cases, although the uneven distribution of cases was causing serious shortfalls in some areas.
2014 spread outside West Africa
On 19 September, Eric Duncan flew from his native Liberia to Texas; five days later he began showing symptoms and visited a hospital but was sent home. His condition worsened and he returned to the hospital on 28 September, where he died on 8 October. Health officials confirmed a diagnosis of Ebola on 30 September – the first case in the United States.
In early October, Teresa Romero, a 44-year-old Spanish nurse, contracted Ebola after caring for a priest who had been repatriated from West Africa. This was the first transmission of the virus to occur outside Africa. Romero tested negative for the disease on 20 October, suggesting that she may have recovered from Ebola infection.
On 12 October, the Centers for Disease Control and Prevention
The Centers for Disease Control and Prevention (CDC) is the national public health agency of the United States. It is a United States federal agency, under the Department of Health and Human Services, and is headquartered in Atlanta, Georgi ...
(CDC) confirmed that a nurse in Texas, Nina Pham
Four laboratory-confirmed cases of Ebola virus disease (commonly known as "Ebola") occurred in the United States in 2014. Eleven cases were reported, including these four cases and seven cases medically evacuated from other countries. The first ...
, who had treated Duncan tested positive for the Ebola virus, the first known case of transmission in the United States.Médecins Sans Frontières
(MSF; pronounced ), also known as Doctors Without Borders, is a humanitarian medical non-governmental organisation (NGO) or charity of French origin known for its projects in conflict zones and in countries affected by endemic diseases. M ...
and tested positive for Ebola on 23 October. The person recovered and was discharged from Bellevue Hospital
Bellevue Hospital (officially NYC Health + Hospitals/Bellevue and formerly known as Bellevue Hospital Center) is a hospital in New York City and the oldest public hospital in the United States. One of the largest hospitals in the United States ...
on 11 November.Atlanta
Atlanta ( ) is the capital and most populous city of the U.S. state of Georgia. It is the seat of Fulton County, the most populous county in Georgia, but its territory falls in both Fulton and DeKalb counties. With a population of 498,715 ...
, Georgia reported that a technician had been exposed to Ebola.
On 29 December 2014, Pauline Cafferkey
Pauline Cafferkey is a Scottish nurse and aid worker who contracted Ebola virus disease in 2014 while working in Sierra Leone as part of the medical aid effort during the West African Ebola virus epidemic. She survived the illness.
Initial adm ...
, a British nurse who had just returned to Glasgow
Glasgow ( ; sco, Glesca or ; gd, Glaschu ) is the most populous city in Scotland and the fourth-most populous city in the United Kingdom, as well as being the 27th largest city by population in Europe. In 2020, it had an estimated popul ...
from Sierra Leone, was diagnosed with Ebola at Glasgow's Gartnavel General Hospital
Gartnavel General Hospital is a teaching hospital in the West End of Glasgow, Scotland. The hospital is located next to the Great Western Road, between Hyndland, Anniesland and Kelvindale. Hyndland railway station is adjacent to the hospital. ...
.RAF Northolt
("Ready to carry or to fight")
, pushpin_map = Greater London
, pushpin_label = RAF Northolt
, pushpin_map_caption = Shown within Greater London
, coordinates =
, type = Royal Air Force station
, code =
, site_area =
, height =
, owners ...
, then to the specialist high-level isolation unit
In hospitals and other medical facilities, an isolation ward is a separate ward used to isolate patients with infectious diseases. Several wards for individual patients are usually placed together in an isolation unit.
Design
In an isolation un ...
at the Royal Free Hospital
The Royal Free Hospital (also known simply as the Royal Free) is a major teaching hospital in the Hampstead area of the London Borough of Camden. The hospital is part of the Royal Free London NHS Foundation Trust, which also runs services at Barn ...
in London
London is the capital and largest city of England and the United Kingdom, with a population of just under 9 million. It stands on the River Thames in south-east England at the head of a estuary down to the North Sea, and has been a majo ...
for longer-term treatment.
2017 Democratic Republic of the Congo
On 11 May 2017, the DRC Ministry of Public Health notified the WHO about an outbreak of Ebola. Four people died, and four people survived; five of these eight cases were laboratory-confirmed. A total of 583 contacts were monitored. On 2 July 2017, the WHO declared the end of the outbreak.
2018 Équateur province
On 14 May 2018, the World Health Organization reported that "the Democratic Republic of Congo reported 39 suspected, probable or confirmed cases of Ebola between 4 April and 13 May, including 19 deaths."Bikoro
Bikoro is a market town in Équateur Province in the Democratic Republic of the Congo, lying on Lake Tumba, south of Mbandaka.
It is the administrative center of Bikoro Territory.
In 2012, the estimated population was 7,426.
Bikoro was the ...
, Iboko, and Wangata
Wangata is a commune in the city of Mbandaka, the capital of Équateur province, in the Democratic Republic of Congo.
References
{{DRCongo-geo-stub
Mbandaka ...
areas in Equateur province,Mbandaka
Mbandaka (, formerly known as Coquilhatville in French, or Coquilhatstad in Dutch) is a city on the Congo River in the Democratic Republic of Congo located near the confluence of the Congo and Ruki rivers. It is the capital of Équateur Provin ...
. The DRC Ministry of Public Health approved the use of an experimental vaccine. On 13 May 2018, WHO Director-General Tedros Adhanom Ghebreyesus
Tedros Adhanom Ghebreyesus ( ti, ቴዎድሮስ አድሓኖም ገብረኢየሱስ, sometimes spelt ti, ቴድሮስ ኣድሓኖም ገብረየሱስ, label=none; born 3 March 1965) is an Ethiopian public health official, researcher, and ...
visited Bikoro. Reports emerged that maps of the area were inaccurate, not so much hampering medical providers as epidemiologist
Epidemiology is the study and analysis of the distribution (who, when, and where), patterns and determinants of health and disease conditions in a defined population.
It is a cornerstone of public health, and shapes policy decisions and evidenc ...
s and officials trying to assess the outbreak and containment efforts. The 2018 outbreak in the DRC was declared over on 24 July 2018.[
]
2018–2020 Kivu
On 1 August 2018, the world's 10th Ebola outbreak was declared in North Kivu
North Kivu (french: link=no, Nord-Kivu) is a province bordering Lake Kivu in the eastern Democratic Republic of the Congo.
Its capital is Goma.
North Kivu borders the provinces of Ituri to the north, Tshopo to the northwest, Maniema to the s ...
province of the Democratic Republic of the Congo. It was the first Ebola outbreak in a military conflict zone, with thousands of refugees in the area. By November 2018, nearly 200 Congolese had died of Ebola, about half of them from the city of Beni
is a Japanese R&B singer, who debuted in 2004 under the Avex Trax label. In 2008, Arashiro left Avex Trax and transferred to Universal Music Japan where she started to perform as simply Beni (stylized as BENI).
She was initially best known fo ...
, where armed groups are fighting over the region's mineral wealth, impeding medical relief efforts.
By March 2019, this became the second largest Ebola outbreak ever recorded, with more than 1,000 cases and insecurity continuing to be the major resistance to providing an adequate response.Uganda
}), is a landlocked country in East Africa
East Africa, Eastern Africa, or East of Africa, is the eastern subregion of the African continent. In the United Nations Statistics Division scheme of geographic regions, 10-11-(16*) territor ...
.
In July 2019, an infected man travelled to Goma
Goma is the capital of North Kivu province in the eastern Democratic Republic of the Congo. It is located on the northern shore of Lake Kivu, next to the Rwandan city of Gisenyi. The lake and the two cities are in the Albertine Rift, the ...
, home to more than two million people. One week later, on 17 July 2019, the WHO declared the Ebola outbreak a global health emergency, the fifth time such a declaration has been made by the organisation. A government spokesman said that half of the Ebola cases are unidentified, and he added that the current outbreak could last up to three years.
On 25 June 2020, the second biggest EVD outbreak ever was declared over.
2020 Équateur province
On 1 June 2020, the Congolese health ministry announced a new DRC outbreak of Ebola in Mbandaka
Mbandaka (, formerly known as Coquilhatville in French, or Coquilhatstad in Dutch) is a city on the Congo River in the Democratic Republic of Congo located near the confluence of the Congo and Ruki rivers. It is the capital of Équateur Provin ...
, Équateur Province Équateur, French for equator, may refer to:
Places
* Province of Équateur, a province of the Democratic Republic of the Congo since 2015
* Équateur (former province), a former province of the Democratic Republic of the Congo, 1966–2015
* Équ ...
, a region along the Congo River. Genome sequencing suggests that this outbreak, the 11th outbreak since the virus was first discovered in the country in 1976, is unrelated to the one in North Kivu Province or the previous outbreak in the same area in 2018. It was reported that six cases had been identified; four of the people had died. It is expected that more people will be identified as surveillance activities increase. By 15 June the case count had increased to 17 with 11 deaths, with more than 2,500 people having been vaccinated. The 11th EVD outbreak was officially declared over on 19 November 2020. By the time the Équateur outbreak ended, it had 130 confirmed cases with 75 recoveries and 55 deaths.
2021
North Kivu
On 7 February 2021, the Congolese health ministry announced a new case of Ebola near Butembo, North Kivu detected a day before. The case was a 42-year-old woman who had symptoms of Ebola in Biena on 1 February 2021. A few days after, she died in a hospital in Butembo. The WHO said that more than 70 people with contact with the woman had been tracked.
Guinea
In February 2021, Dr Sakoba Keita, head of Guinea's national health agency confirmed that three people had died of Ebola in the south-eastern region near the city of Nzérékoré. A further five people also tested positive. Keita also confirmed more testing was underway, and attempts to trace and isolate further cases had begun. On 14 February, the Guinean government declared an Ebola epidemic. The outbreak may have started following reactivation of a latent case in a survivor of an earlier outbreak.
Ivory Coast
On 14 August 2021, The Ministry of Health of Cote d’Ivoire
Ivory Coast, also known as Côte d'Ivoire, officially the Republic of Côte d'Ivoire, is a country on the southern coast of West Africa. Its capital is Yamoussoukro, in the centre of the country, while its largest city and economic centre is ...
confirmed the country's first case of Ebola since 1994. This came after the Institut Pasteur in Cote d'Ivoire confirmed the Ebola Virus Disease in samples collected from a patient, who was hospitalized in the commercial capital of Abidjan
Abidjan ( , ; N'Ko script, N’ko: ߊߓߌߖߊ߲߬) is the economic capital of the Ivory Coast. As of the Demographics of Ivory Coast, 2021 census, Abidjan's population was 6.3 million, which is 21.5 percent of overall population of the country, ...
, after arriving from Guinea.
However, on 31 August 2021, the WHO found that, after further tests in a laboratory in Lyon
Lyon,, ; Occitan: ''Lion'', hist. ''Lionés'' also spelled in English as Lyons, is the third-largest city and second-largest metropolitan area of France. It is located at the confluence of the rivers Rhône and Saône, to the northwest of t ...
, the patient did not have Ebola. The cause of her disease is still being analyzed.
2022
On 23 April 2022, a case of Ebola was confirmed in the DRC in the Equateur province. The case was a 31-year-old man whose symptoms began on 5 April, but did not seek treatment for over a week. On 21 April, he was admitted to an Ebola treatment centre and died later that day. By 24 May 2022, there were 5 recorded deaths in the DRC. On 15 August, the fifth case was buried, and the outbreak was declared over, 42 days after, on 4 July 2022.
In September 2022, Uganda reported 7 cases infected with the Ebola Sudan strain, but by mid-October the count had increased to 63.
In November 2022 (present), the outbreak in Uganda continued - still without a vaccine.
Society and culture
Weaponisation
''Ebolavirus'' is classified as a biosafety level 4 agent, as well as a Category A bioterrorism agent by the Centers for Disease Control and Prevention.biological warfare
Biological warfare, also known as germ warfare, is the use of biological toxins or infectious agents such as bacteria, viruses, insects, and fungi with the intent to kill, harm or incapacitate humans, animals or plants as an act of war. ...
,Biopreparat
The All-Union Science Production Association Biopreparat (russian: Биопрепарат, p=bʲɪəprʲɪpɐˈrat, lit: "biological preparation") was the Soviet agency created in April 1974, which spearheaded the largest and most sophisticated ...
for such use, but might be difficult to prepare as a weapon of mass destruction
A weapon of mass destruction (WMD) is a chemical, biological, radiological, nuclear, or any other weapon that can kill and bring significant harm to numerous individuals or cause great damage to artificial structures (e.g., buildings), natu ...
because the virus becomes ineffective quickly in open air.
Literature
Richard Preston
Richard Preston (born August 5, 1954) is a writer for ''The New Yorker'' and bestselling author who has written books about infectious disease, bioterrorism, redwoods and other subjects, as well as fiction.
Biography
Preston was born in Cambri ...
's 1995 best-selling
A bestseller is a book or other media noted for its top selling status, with bestseller lists published by newspapers, magazines, and book store chains. Some lists are broken down into classifications and specialties (novel, nonfiction book, cookb ...
book, ''The Hot Zone
''The Hot Zone: A Terrifying True Story'' is a best-selling 1994 nonfiction thriller by Richard Preston about the origins and incidents involving viral hemorrhagic fevers, particularly ebolaviruses and marburgviruses. The basis of the book ...
'', dramatised the Ebola outbreak in Reston, Virginia.
William Close
William Taliaferro Close (June 7, 1924 – January 15, 2009) was an American surgeon who played a major role in stemming a 1976 outbreak of the Ebola virus in Zaire, the first major outbreak of the viral hemorrhagic fever in Central Africa, a ...
's 1995 ''Ebola: A Documentary Novel of Its First Explosion'' and 2002 ''Ebola: Through the Eyes of the People'' focused on individuals' reactions to the 1976 Ebola outbreak in Zaire.
Tom Clancy
Thomas Leo Clancy Jr. (April 12, 1947 – October 1, 2013) was an American novelist. He is best known for his technically detailed espionage and military science, military-science storylines set during and after the Cold War. Seventeen of ...
's 1996 novel, '' Executive Orders'', involves a Middle East
The Middle East ( ar, الشرق الأوسط, ISO 233: ) is a geopolitical region commonly encompassing Arabian Peninsula, Arabia (including the Arabian Peninsula and Bahrain), Anatolia, Asia Minor (Asian part of Turkey except Hatay Pro ...
ern terrorist attack on the United States using an airborne form of a deadly Ebola virus strain named "Ebola Mayinga" (see Mayinga N'Seka
Mayinga N'Seka (1954 – October 19, 1976 in Kinshasa) was a nurse in Zaïre, now Democratic Republic of the Congo. She died from Ebola virus disease during the 1976 epidemic in Zaïre. She has been incorrectly identified as the index case by se ...
).
As the Ebola virus epidemic in West Africa developed in 2014, a number of popular self-published and well-reviewed books containing sensational and misleading information about the disease appeared in electronic and printed formats. The authors of some such books admitted that they lacked medical credentials and were not technically qualified to give medical advice. The World Health Organization and the United Nations stated that such misinformation had contributed to the spread of the disease.
Other animals
Wild animals
Ebola has a high mortality rate among primates.
Domestic animals
In 2012, it was demonstrated that the virus can travel without contact from pigs to nonhuman primates, although the same study failed to achieve transmission in that manner between primates.scavenge
Scavengers are animals that consume Corpse decomposition, dead organisms that have died from causes other than predation or have been killed by other predators. While scavenging generally refers to carnivores feeding on carrion, it is also a h ...
for food, and they sometimes eat EBOV-infected animals and also the corpses of humans. A 2005 survey of dogs during an EBOV outbreak found that although they remain asymptomatic, about 32 percent of dogs closest to an outbreak showed a seroprevalence
Seroprevalence is the number of persons in a population who test positive for a specific disease based on serology (blood serum) specimens; often presented as a percent of the total specimens tested or as a proportion per 100,000 persons tested. As ...
for EBOV versus nine percent of those farther away.
Reston virus
In late 1989, Hazelton Research Products' Reston Quarantine Unit in Reston, Virginia
Reston is a census-designated place in Fairfax County, Virginia and a principal city of the Washington metropolitan area. As of the 2020 U.S. Census, Reston's population was 63,226.
Founded in 1964, Reston was influenced by the Garden City movem ...
, had an outbreak of fatal illness amongst certain lab monkeys. This lab outbreak was initially diagnosed as simian haemorrhagic fever virus
''Deltaarterivirus hemfev'', formerly ''Simian hemorrhagic fever virus'' or ''simian haemorrhagic fever virus'' (SHFV), is a highly pathogenic virus in monkeys. It is a positive-stranded RNA virus classified in the family ''Arteriviridae''. It ...
(SHFV) and occurred amongst a shipment of crab-eating macaque
The crab-eating macaque (''Macaca fascicularis''), also known as the long-tailed macaque and referred to as the cynomolgus monkey in laboratories, is a cercopithecine primate native to Southeast Asia. A species of macaque, the crab-eating macaqu ...
monkeys imported from the Philippines. Hazelton's veterinary pathologist in Reston sent tissue samples from dead animals to the (USAMRIID) at Fort Detrick, Maryland
Fort Detrick () is a United States Army Futures Command installation located in Frederick, Maryland. Historically, Fort Detrick was the center of the U.S. biological weapons program from 1943 to 1969. Since the discontinuation of that program, i ...
, where an ELISA
The enzyme-linked immunosorbent assay (ELISA) (, ) is a commonly used analytical biochemistry assay, first described by Eva Engvall and Peter Perlmann in 1971. The assay uses a solid-phase type of enzyme immunoassay (EIA) to detect the presence ...
test indicated the antibodies present in the tissue were a response to Ebola virus and not SHFV.filoviruses
''Filoviridae'' () is a family of single-stranded negative-sense RNA viruses in the order ''Mononegavirales''. Two members of the family that are commonly known are Ebola virus and Marburg virus. Both viruses, and some of their lesser known re ...
similar in appearance, in crystalloid aggregates and as single filaments with a shepherd's hook, to Ebola in the tissue samples sent from Hazelton Research Products' Reston Quarantine Unit.US Army
The United States Army (USA) is the land service branch of the United States Armed Forces. It is one of the eight U.S. uniformed services, and is designated as the Army of the United States in the U.S. Constitution.Article II, section 2, cla ...
team headquartered at USAMRIID euthanised
Animal euthanasia ( euthanasia from el, εὐθανασία; "good death") is the act of killing an animal or allowing it to die by withholding extreme medical measures. Reasons for euthanasia include incurable (and especially painful) conditi ...
the surviving monkeys, and brought all the dead monkeys to Fort Detrick for study by the Army's veterinary pathologists and virologists, and eventual disposal under safe conditions.pathogen
In biology, a pathogen ( el, πάθος, "suffering", "passion" and , "producer of") in the oldest and broadest sense, is any organism or agent that can produce disease. A pathogen may also be referred to as an infectious agent, or simply a germ ...
icity in monkeys, when the handlers did not become ill, the CDC concluded that the virus had a very low pathogenicity to humans.primate
Primates are a diverse order of mammals. They are divided into the strepsirrhines, which include the lemurs, galagos, and lorisids, and the haplorhines, which include the tarsiers and the simians (monkeys and apes, the latter including huma ...
s in Pennsylvania, Texas, and Italy,sodium hypochlorite
Sodium hypochlorite (commonly known in a dilute solution as bleach) is an Inorganic chemistry, inorganic chemical compound with the chemical formula, formula NaOCl (or NaClO), comprising a sodium cation () and a hypochlorite anion (or ). It may ...
or detergents should be effective in inactivating the ''Reston ebolavirus''. Pigs that have been infected with RESTV tend to show symptoms of the disease.
Research
Treatments
 , no medication has been proven safe and effective for treating Ebola. By the time the
, no medication has been proven safe and effective for treating Ebola. By the time the Ebola virus epidemic in West Africa
The 2013–2016 epidemic of Ebola virus disease, centered in Western Africa, was the most widespread outbreak of the disease in history. It caused major loss of life and socioeconomic disruption in the region, mainly in Guinea, Liberia and S ...
began in 2013, there were at least nine different candidate treatments. Several trials were conducted in late 2014, and early 2015, but some were abandoned due to lack of efficacy or lack of people to study.
, two experimental treatments known as atoltivimab/maftivimab/odesivimab
Atoltivimab/maftivimab/odesivimab, sold under the brand name Inmazeb, is a fixed-dose combination of three monoclonal antibodies for the treatment of '' Zaire ebolavirus'' (Ebola virus). It contains atoltivimab, maftivimab, and odesivimab-eb ...
and ansuvimab
Ansuvimab, sold under the brand name Ebanga, is a monoclonal antibody medication for the treatment of ''Zaire ebolavirus'' (Ebolavirus) infection.
The most common symptoms include fever, tachycardia (fast heart rate), diarrhea, vomiting, hypote ...
were found to be 90% effective.
Diagnostic tests
The diagnostic tests currently available require specialised equipment and highly trained personnel. Since there are few suitable testing centres in West Africa, this leads to delay in diagnosis.
On 29 November 2014, a new 15-minute Ebola test was reported that if successful, "not only gives patients a better chance of survival, but it prevents transmission of the virus to other people." The new equipment, about the size of a laptop and solar-powered, allows testing to be done in remote areas.
On 29 December 2014, the U.S. Food and Drug Administration
The United States Food and Drug Administration (FDA or US FDA) is a List of United States federal agencies, federal agency of the United States Department of Health and Human Services, Department of Health and Human Services. The FDA is respon ...
(FDA) approved the LightMix Ebola Zaire rRT-PCR test for patients with symptoms of Ebola.
Disease models
Animal models and in particular non-human primates are being used to study different aspects of Ebola virus disease. Developments in organ-on-a-chip
An organ-on-a-chip (OOC) is a multi-channel 3-D microfluidic cell culture, integrated circuit (chip) that simulates the activities, mechanics and physiological response of an entire organ or an organ system, a type of artificial organ. It cons ...
technology have led to a chip-based model for Ebola haemorrhagic syndrome.
See also
* Bibliography of Ebola
Notes
References
* ''The article uses public domain text from the CDC as cited.''
Bibliography
*
*
*
*
*
*
*
*
External links
Ebola (Ebola Virus Disease)
nbsp;– Centers for Disease Control and Prevention, Viral Special Pathogens Branch.
Health topics: Ebola virus disease
nbsp;– World Health Organization.
Videos: Ebola outbreak response
nbsp;– World Health Organization.
*
Ebola: What You Need to Know
nbsp;– ''Scientific American
''Scientific American'', informally abbreviated ''SciAm'' or sometimes ''SA'', is an American popular science magazine. Many famous scientists, including Albert Einstein and Nikola Tesla, have contributed articles to it. In print since 1845, it i ...
'' articles related to Ebola; note these are general reading articles, they are not scientific peer-reviewed research articles.
{{Authority control
Animal viral diseases
Arthropod-borne viral fevers and viral haemorrhagic fevers
Articles containing video clips
Bat virome
Biological weapons
Health in Africa
Hemorrhagic fevers
Wikipedia medicine articles ready to translate
Wikipedia infectious disease articles ready to translate
Sexually transmitted diseases and infections
Tropical diseases
Virus-related cutaneous conditions
West African Ebola virus epidemic
Wikipedia pages referenced by the press
Zoonoses
so:Ebola virus disease

 Ebolaviruses contain single-stranded, non-infectious
Ebolaviruses contain single-stranded, non-infectious 
 It is believed that between people, Ebola disease spreads only by direct contact with the blood or other
It is believed that between people, Ebola disease spreads only by direct contact with the blood or other  Community awareness of the benefits on survival chances of admitting cases early is important for the infected and infection control
Community awareness of the benefits on survival chances of admitting cases early is important for the infected and infection control
 People who care for those infected with Ebola should wear protective clothing including masks, gloves, gowns and goggles. The U.S.
People who care for those infected with Ebola should wear protective clothing including masks, gloves, gowns and goggles. The U.S.  Treatment is primarily supportive in nature. Early supportive care with rehydration and symptomatic treatment improves survival. Rehydration may be via the
Treatment is primarily supportive in nature. Early supportive care with rehydration and symptomatic treatment improves survival. Rehydration may be via the  The first known outbreak of EVD was identified only after the fact. It occurred between June and November 1976, in
The first known outbreak of EVD was identified only after the fact. It occurred between June and November 1976, in  On 26 August 1976, the second outbreak of EVD began in
On 26 August 1976, the second outbreak of EVD began in  The second major outbreak occurred in Zaire (now the
The second major outbreak occurred in Zaire (now the  In March 2014, the
In March 2014, the  , no medication has been proven safe and effective for treating Ebola. By the time the
, no medication has been proven safe and effective for treating Ebola. By the time the