A computed tomography scan (CT scan), formerly called computed axial tomography scan (CAT scan), is a
medical imaging
Medical imaging is the technique and process of imaging the interior of a body for clinical analysis and medical intervention, as well as visual representation of the function of some organs or tissues (physiology). Medical imaging seeks to revea ...
technique used to obtain detailed internal images of the body. The personnel that perform CT scans are called
radiographer
Radiographers, also known as radiology technologists, radiologic technologists, diagnostic radiographers and medical radiation technologists, are healthcare professionals who specialise in the imaging of human anatomy for the diagnosis and tr ...
s or radiology technologists.
CT scanners use a rotating
X-ray tube and a row of detectors placed in a
gantry to measure X-ray
attenuations by different tissues inside the body. The multiple
X-ray
An X-ray (also known in many languages as R├Čntgen radiation) is a form of high-energy electromagnetic radiation with a wavelength shorter than those of ultraviolet rays and longer than those of gamma rays. Roughly, X-rays have a wavelength ran ...
measurements taken from different angles are then processed on a computer using
tomographic reconstruction algorithms to produce
tomographic (cross-sectional) images (virtual "slices") of a body. CT scans can be used in patients with metallic implants or pacemakers, for whom
magnetic resonance imaging
Magnetic resonance imaging (MRI) is a medical imaging technique used in radiology to generate pictures of the anatomy and the physiological processes inside the body. MRI scanners use strong magnetic fields, magnetic field gradients, and ...
(MRI) is
contraindicated.
Since its development in the 1970s, CT scanning has proven to be a versatile imaging technique. While CT is most prominently used in
medical diagnosis
Medical diagnosis (abbreviated Dx, Dx, or Ds) is the process of determining which disease or condition explains a person's symptoms and signs. It is most often referred to as a diagnosis with the medical context being implicit. The information ...
, it can also be used to form images of non-living objects. The 1979
Nobel Prize in Physiology or Medicine
The Nobel Prize in Physiology or Medicine () is awarded yearly by the Nobel Assembly at the Karolinska Institute for outstanding discoveries in physiology or medicine. The Nobel Prize is not a single prize, but five separate prizes that, acco ...
was awarded jointly to South African-American physicist
Allan MacLeod Cormack and British electrical engineer
Godfrey Hounsfield "for the development of computer-assisted tomography".
Types
On the basis of image acquisition and procedures, various type of scanners are available in the market.
Sequential CT
Sequential CT, also known as step-and-shoot CT, is a type of scanning method in which the CT table moves stepwise. The table increments to a particular location and then stops which is followed by the
X-ray tube rotation and acquisition of a slice. The table then increments again, and another slice is taken. The table movement stops while taking slices. This results in an increased time of scanning.
Spiral CT
Spinning tube, commonly called
spiral CT, or helical CT, is an imaging technique in which an entire
X-ray tube is spun around the central axis of the area being scanned. These are the dominant type of scanners on the market because they have been manufactured longer and offer a lower cost of production and purchase. The main limitation of this type of CT is the bulk and inertia of the equipment (X-ray tube assembly and detector array on the opposite side of the circle) which limits the speed at which the equipment can spin. Some designs use two X-ray sources and detector arrays offset by an angle, as a technique to improve temporal resolution.
Electron beam tomography
Electron beam tomography (EBT) is a specific form of CT in which a large enough X-ray tube is constructed so that only the path of the
electron
The electron (, or in nuclear reactions) is a subatomic particle with a negative one elementary charge, elementary electric charge. It is a fundamental particle that comprises the ordinary matter that makes up the universe, along with up qua ...
s, travelling between the
cathode
A cathode is the electrode from which a conventional current leaves a polarized electrical device such as a lead-acid battery. This definition can be recalled by using the mnemonic ''CCD'' for ''Cathode Current Departs''. Conventional curren ...
and
anode
An anode usually is an electrode of a polarized electrical device through which conventional current enters the device. This contrasts with a cathode, which is usually an electrode of the device through which conventional current leaves the devic ...
of the X-ray tube, are spun using
deflection coils. This type had a major advantage since sweep speeds can be much faster, allowing for less blurry imaging of moving structures, such as the heart and arteries. Fewer scanners of this design have been produced when compared with spinning tube types, mainly due to the higher cost associated with building a much larger X-ray tube and detector array and limited anatomical coverage.
Dual energy CT
Dual energy CT, also known as spectral CT, is an advancement of computed Tomography in which two energies are used to create two sets of data. A dual energy CT may employ dual source, single source with dual detector layer, single source with energy switching methods to get two different sets of data.
* Dual source CT is an advanced scanner with a two X-ray tube detector system, unlike conventional single tube systems. These two detector systems are mounted on a single gantry at 90┬░ in the same plane.
Dual source CT scanners allow fast scanning with higher temporal resolution by acquiring a full CT slice in only half a rotation. Fast imaging reduces motion blurring at high heart rates and potentially allowing for shorter breath-hold time. This is particularly useful for ill patients having difficulty holding their breath or unable to take heart-rate lowering medication.
* Single source with energy switching is another mode of dual energy CT in which a single tube is operated at two different energies by switching the energies frequently.
CT perfusion imaging

CT perfusion imaging is a specific form of CT to assess flow through
blood vessel
Blood vessels are the tubular structures of a circulatory system that transport blood throughout many Animal, animalsŌĆÖ bodies. Blood vessels transport blood cells, nutrients, and oxygen to most of the Tissue (biology), tissues of a Body (bi ...
s whilst injecting a
contrast agent.
Blood flow, blood transit time, and organ blood volume, can all be calculated with reasonable
sensitivity and specificity.
This type of CT may be used on the
heart
The heart is a muscular Organ (biology), organ found in humans and other animals. This organ pumps blood through the blood vessels. The heart and blood vessels together make the circulatory system. The pumped blood carries oxygen and nutrie ...
, although sensitivity and specificity for detecting abnormalities are still lower than for other forms of CT. This may also be used on the
brain
The brain is an organ (biology), organ that serves as the center of the nervous system in all vertebrate and most invertebrate animals. It consists of nervous tissue and is typically located in the head (cephalization), usually near organs for ...
, where CT perfusion imaging can often detect poor brain perfusion well before it is detected using a conventional spiral CT scan.
This is better for
stroke
Stroke is a medical condition in which poor cerebral circulation, blood flow to a part of the brain causes cell death. There are two main types of stroke: brain ischemia, ischemic, due to lack of blood flow, and intracranial hemorrhage, hemor ...
diagnosis than other CT types.
PET CT

Positron emission tomographyŌĆōcomputed tomography is a hybrid CT modality which combines, in a single gantry, a
positron emission tomography
Positron emission tomography (PET) is a functional imaging technique that uses radioactive substances known as radiotracers to visualize and measure changes in metabolic processes, and in other physiological activities including blood flow, r ...
(PET) scanner and an X-ray computed tomography (CT) scanner, to acquire sequential images from both devices in the same session, which are combined into a single superposed (
co-registered) image. Thus,
functional imaging
Functional imaging (or physiological imaging) is a medical imaging technique of detecting or measuring changes in metabolism, blood flow, regional chemical composition, and absorption.
As opposed to structural imaging, functional imaging center ...
obtained by PET, which depicts the spatial distribution of metabolic or biochemical activity in the body can be more precisely aligned or correlated with anatomic imaging obtained by CT scanning.
PET-CT gives both anatomical and functional details of an organ under examination and is helpful in detecting different type of cancers.
Medical use
Since its introduction in the 1970s, CT has become an important tool in
medical imaging
Medical imaging is the technique and process of imaging the interior of a body for clinical analysis and medical intervention, as well as visual representation of the function of some organs or tissues (physiology). Medical imaging seeks to revea ...
to supplement conventional
X-ray
An X-ray (also known in many languages as R├Čntgen radiation) is a form of high-energy electromagnetic radiation with a wavelength shorter than those of ultraviolet rays and longer than those of gamma rays. Roughly, X-rays have a wavelength ran ...
imaging and
medical ultrasonography
Medical ultrasound includes Medical diagnosis, diagnostic techniques (mainly medical imaging, imaging) using ultrasound, as well as therapeutic ultrasound, therapeutic applications of ultrasound. In diagnosis, it is used to create an image of ...
. It has more recently been used for
preventive medicine or
screening for disease, for example,
CT colonography for people with a high risk of
colon cancer, or full-motion heart scans for people with a high risk of heart disease. Several institutions offer
full-body scans for the general population although this practice goes against the advice and official position of many professional organizations in the field primarily due to the
radiation dose applied.
The use of CT scans has increased dramatically over the last two decades in many countries.
An estimated 72 million scans were performed in the United States in 2007 and more than 80 million in 2015.
Head

CT scanning of the head is typically used to detect
infarction
Infarction is tissue death (necrosis) due to Ischemia, inadequate blood supply to the affected area. It may be caused by Thrombosis, artery blockages, rupture, mechanical compression, or vasoconstriction. The resulting lesion is referred to as a ...
(
stroke
Stroke is a medical condition in which poor cerebral circulation, blood flow to a part of the brain causes cell death. There are two main types of stroke: brain ischemia, ischemic, due to lack of blood flow, and intracranial hemorrhage, hemor ...
),
tumors
A neoplasm () is a type of abnormal and excessive growth of tissue. The process that occurs to form or produce a neoplasm is called neoplasia. The growth of a neoplasm is uncoordinated with that of the normal surrounding tissue, and persists ...
,
calcifications,
haemorrhage, and bone
trauma. Of the above,
hypodense (dark) structures can indicate
edema and infarction, hyperdense (bright) structures indicate calcifications and haemorrhage and bone trauma can be seen as disjunction in bone windows. Tumors can be detected by the swelling and anatomical distortion they cause, or by surrounding edema. CT scanning of the head is also used in CT-
guided stereotactic surgery and
radiosurgery for treatment of intracranial tumors,
arteriovenous malformations, and other surgically treatable conditions using a device known as the
N-localizer.
Neck
Contrast CT is generally the initial study of choice for
neck masses in adults.
[ This topic last updated: Dec 04, 2017.] CT of the thyroid plays an important role in the evaluation of
thyroid cancer
Thyroid cancer is cancer that develops from the tissues of the thyroid gland. It is a disease in which cells grow abnormally and have the potential to spread to other parts of the body. Symptoms can include swelling or a lump in the neck, ...
.
CT scans often incidentally find thyroid abnormalities, and so is often the preferred investigation modality for thyroid abnormalities.
Lungs
A CT scan can be used for detecting both acute and chronic changes in the
lung parenchyma
file:emphysema, bullous, subpleural and honeycomb fibrosis (4563270966).jpg, upright=1.6, Lung parenchyma showing damage due to large subpleural Focal lung pneumatosis, bullae.
Parenchyma () is the bulk of functional substance in an animal org ...
, the tissue of the
lung
The lungs are the primary Organ (biology), organs of the respiratory system in many animals, including humans. In mammals and most other tetrapods, two lungs are located near the Vertebral column, backbone on either side of the heart. Their ...
s. It is particularly helpful because normal two-dimensional X-rays do not show such defects. A variety of techniques are used, depending on the suspected abnormality. For evaluation of chronic interstitial processes such as
emphysema, and
fibrosis, thin sections with high spatial frequency reconstructions are used; often scans are performed both on inspiration and expiration. This special technique is called
high resolution CT that produces a sampling of the lung, and not continuous images.
Bronchial wall thickening can be seen on lung CTs and generally (but not always) implies inflammation of the
bronchi.
An
incidentally found nodule in the absence of symptoms (sometimes referred to as an
incidentaloma) may raise concerns that it might represent a tumor, either
benign or
malignant
Malignancy () is the tendency of a medical condition to become progressively worse; the term is most familiar as a characterization of cancer.
A ''malignant'' tumor contrasts with a non-cancerous benign tumor, ''benign'' tumor in that a malig ...
. Perhaps persuaded by fear, patients and doctors sometimes agree to an intensive schedule of CT scans, sometimes up to every three months and beyond the recommended guidelines, in an attempt to do surveillance on the nodules.
[, which cites
*
*
*
*] However, established guidelines advise that patients without a prior history of cancer and whose solid nodules have not grown over a two-year period are unlikely to have any malignant cancer.
For this reason, and because no research provides supporting evidence that intensive surveillance gives better outcomes, and because of risks associated with having CT scans, patients should not receive CT screening in excess of those recommended by established guidelines.
Angiography
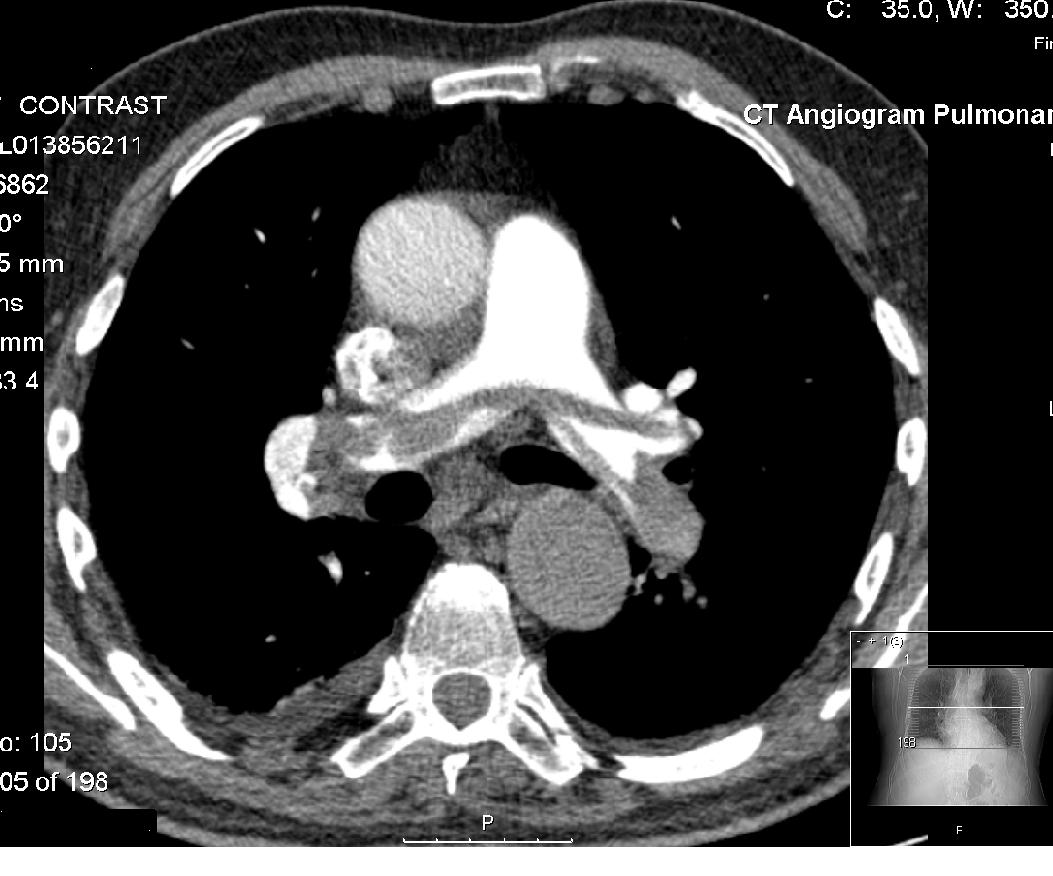
Computed tomography angiography
Computed tomography angiography (also called CT angiography or CTA) is a computed tomography technique used for angiographyŌĆöthe visualization of arteries and veinsŌĆöthroughout the human body. Using contrast injected into the blood vessels, im ...
(CTA) is a type of
contrast CT to visualize the
arteries and
vein
Veins () are blood vessels in the circulatory system of humans and most other animals that carry blood towards the heart. Most veins carry deoxygenated blood from the tissues back to the heart; exceptions are those of the pulmonary and feta ...
s throughout the body. This ranges from arteries serving the
brain
The brain is an organ (biology), organ that serves as the center of the nervous system in all vertebrate and most invertebrate animals. It consists of nervous tissue and is typically located in the head (cephalization), usually near organs for ...
to those bringing blood to the
lung
The lungs are the primary Organ (biology), organs of the respiratory system in many animals, including humans. In mammals and most other tetrapods, two lungs are located near the Vertebral column, backbone on either side of the heart. Their ...
s,
kidney
In humans, the kidneys are two reddish-brown bean-shaped blood-filtering organ (anatomy), organs that are a multilobar, multipapillary form of mammalian kidneys, usually without signs of external lobulation. They are located on the left and rig ...
s,
arms and
leg
A leg is a weight-bearing and locomotive anatomical structure, usually having a columnar shape. During locomotion, legs function as "extensible struts". The combination of movements at all joints can be modeled as a single, linear element cap ...
s. An example of this type of exam is
CT pulmonary angiogram (CTPA) used to diagnose
pulmonary embolism
Pulmonary embolism (PE) is a blockage of an pulmonary artery, artery in the lungs by a substance that has moved from elsewhere in the body through the bloodstream (embolism). Symptoms of a PE may include dyspnea, shortness of breath, chest pain ...
(PE). It employs computed tomography and an
iodine-based contrast agent to obtain an image of the
pulmonary arteries
A pulmonary artery is an artery in the pulmonary circulation that carries deoxygenated blood from the right side of the heart to the lungs. The largest pulmonary artery is the ''main pulmonary artery'' or ''pulmonary trunk'' from the heart, and ...
. CT scans can reduce the risk of angiography by providing clinicians with more information about the positioning and number of clots prior to the procedure.
Cardiac
A CT scan of the heart is performed to gain knowledge about cardiac or coronary anatomy. Traditionally, cardiac CT scans are used to detect, diagnose, or follow up
coronary artery disease
Coronary artery disease (CAD), also called coronary heart disease (CHD), or ischemic heart disease (IHD), is a type of cardiovascular disease, heart disease involving Ischemia, the reduction of blood flow to the cardiac muscle due to a build-up ...
.
More recently CT has played a key role in the fast-evolving field of
transcatheter structural heart interventions, more specifically in the transcatheter repair and replacement of heart valves.
The main forms of cardiac CT scanning are:
*
Coronary CT angiography (CCTA): the use of CT to assess the
coronary arteries
The coronary arteries are the arteries, arterial blood vessels of coronary circulation, which transport oxygenated blood to the Cardiac muscle, heart muscle. The heart requires a continuous supply of oxygen to function and survive, much like any ...
of the
heart
The heart is a muscular Organ (biology), organ found in humans and other animals. This organ pumps blood through the blood vessels. The heart and blood vessels together make the circulatory system. The pumped blood carries oxygen and nutrie ...
. The subject receives an
intravenous injection of
radiocontrast
Radiocontrast agents are substances used to enhance the visibility of internal structures in X-ray-based imaging techniques such as computed tomography (contrast CT), projectional radiography, and fluoroscopy. Radiocontrast agents are typically iod ...
, and then the heart is scanned using a high-speed CT scanner, allowing radiologists to assess the extent of occlusion in the coronary arteries, usually to diagnose coronary artery disease.
*
Coronary CT calcium scan: also used for the assessment of severity of coronary artery disease. Specifically, it looks for calcium deposits in the coronary arteries that can narrow arteries and increase the risk of a heart attack.
A typical coronary CT calcium scan is done without the use of radiocontrast, but it can possibly be done from contrast-enhanced images as well.
To better visualize the anatomy, post-processing of the images is common.
Most common are multiplanar reconstructions (MPR) and
volume rendering. For more complex anatomies and procedures, such as heart valve interventions, a true
3D reconstruction or a 3D print is created based on these CT images to gain a deeper understanding.
Abdomen and pelvis
CT is an accurate technique for diagnosis of
abdominal diseases such as
Crohn's disease
Crohn's disease is a type of inflammatory bowel disease (IBD) that may affect any segment of the gastrointestinal tract. Symptoms often include abdominal pain, diarrhea, fever, abdominal distension, and weight loss. Complications outside of the ...
, GIT bleeding, and diagnosis and staging of cancer, as well as follow-up after cancer treatment to assess response. It is commonly used to investigate
acute abdominal pain.
Non-contrast-enhanced CT scans are the gold standard for diagnosing
kidney stone disease
Kidney stone disease (known as nephrolithiasis, renal calculus disease, or urolithiasis) is a crystallopathy and occurs when there are too many minerals in the urine and not enough liquid or hydration. This imbalance causes tiny pieces of cry ...
. They allow clinicians to estimate the size, volume, and density of stones, helping to guide further treatment; with size being especially important in predicting the time to spontaneous passage of a stone.
Axial skeleton and extremities
For the
axial skeleton and
extremities, CT is often used to image complex
fractures
Fracture is the appearance of a crack or complete separation of an object or material into two or more pieces under the action of stress (mechanics), stress. The fracture of a solid usually occurs due to the development of certain displacemen ...
, especially ones around joints, because of its ability to reconstruct the area of interest in multiple planes. Fractures, ligamentous injuries, and
dislocations can easily be recognized with a 0.2 mm resolution. With modern dual-energy CT scanners, new areas of use have been established, such as aiding in the diagnosis of
gout
Gout ( ) is a form of inflammatory arthritis characterized by recurrent attacks of pain in a red, tender, hot, and Joint effusion, swollen joint, caused by the deposition of needle-like crystals of uric acid known as monosodium urate crysta ...
.
Biomechanical use
CT is used in
biomechanics to quickly reveal the geometry, anatomy,
density
Density (volumetric mass density or specific mass) is the ratio of a substance's mass to its volume. The symbol most often used for density is ''Žü'' (the lower case Greek letter rho), although the Latin letter ''D'' (or ''d'') can also be u ...
and
elastic moduli of biological tissues.
Other uses
Industrial use
Industrial CT scanning (industrial computed tomography) is a process which uses X-ray equipment to produce 3D representations of components both externally and internally. Industrial CT scanning has been used in many areas of industry for internal inspection of components. Some of the key uses for CT scanning have been flaw detection, failure analysis, metrology, assembly analysis, image-based finite element methods and reverse engineering applications. CT scanning is also employed in the imaging and conservation of museum artifacts.
Aviation security
CT scanning has also found an application in transport security (predominantly
airport security) where it is currently used in a materials analysis context for explosives detection
CTX (explosive-detection device) and is also under consideration for automated baggage/parcel security scanning using
computer vision
Computer vision tasks include methods for image sensor, acquiring, Image processing, processing, Image analysis, analyzing, and understanding digital images, and extraction of high-dimensional data from the real world in order to produce numerical ...
based object recognition algorithms that target the detection of specific threat items based on 3D appearance (e.g. guns, knives, liquid containers).
Its usage in airport security pioneered at
Shannon Airport in March 2022 has ended the ban on liquids over 100 ml there, a move that
Heathrow Airport plans for a full roll-out on 1 December 2022 and the TSA spent $781.2 million on an order for over 1,000 scanners, ready to go live in the summer.
Geological use
X-ray CT is used in geological studies to quickly reveal materials inside a drill core. Dense minerals such as pyrite and barite appear brighter and less dense components such as clay appear dull in CT images.
Paleontological use
Traditional methods of studying fossils are often destructive, such as the use of thin sections and physical preparation. X-ray CT is used in paleontology to non-destructively visualize fossils in 3D. This has many advantages. For example, we can look at fragile structures that might never otherwise be able to be studied. In addition, one can freely move around models of fossils in virtual 3D space to inspect it without damaging the fossil.
Cultural heritage use
X-ray CT and
micro-CT can also be used for the conservation and preservation of objects of cultural heritage. For many fragile objects, direct research and observation can be damaging and can degrade the object over time. Using CT scans, conservators and researchers are able to determine the material composition of the objects they are exploring, such as the position of ink along the layers of a scroll, without any additional harm. These scans have been optimal for research focused on the workings of the
Antikythera mechanism
The Antikythera mechanism ( , ) is an Ancient Greece, Ancient Greek hand-powered orrery (model of the Solar System). It is the oldest known example of an Analog computer, analogue computer. It could be used to predict astronomy, astronomical ...
or the text hidden inside the charred outer layers of the
En-Gedi Scroll. However, they are not optimal for every object subject to these kinds of research questions, as there are certain artifacts like the
Herculaneum papyri in which the material composition has very little variation along the inside of the object. After scanning these objects, computational methods can be employed to examine the insides of these objects, as was the case with the virtual unwrapping of the
En-Gedi scroll and the
Herculaneum papyri. Micro-CT has also proved useful for analyzing more recent artifacts such as still-sealed historic correspondence that employed the technique of
letterlocking (complex folding and cuts) that provided a "tamper-evident locking mechanism". Further examples of use cases in archaeology is imaging the contents of sarcophagi or ceramics.
Recently, CWI in Amsterdam has collaborated with Rijksmuseum to investigate art object inside details in the framework called IntACT.
Microorganism research
Varied types of fungus can degrade wood to different degrees, one Belgium research group has been used X-ray CT 3 dimension with sub-micron resolution unveiled fungi can penetrate micropores of 0.6 ╬╝m under certain conditions.
Timber sawmill
Sawmills use industrial CT scanners to detect round defects, for instance knots, to improve total value of timber productions. Most sawmills are planning to incorporate this robust detection tool to improve productivity in the long run, however initial investment cost is high.
Interpretation of results
Presentation
The result of a CT scan is a volume of
voxels, which may be presented to a human observer by various methods, which broadly fit into the following categories:
*Slices (of varying thickness). Thin slice is generally regarded as planes representing a thickness of less than 3
mm.
Thick slice is generally regarded as planes representing a thickness between 3 mm and 5 mm.
*Projection, including
maximum intensity projection and ''average intensity projection''
*
Volume rendering (VR)
Technically, all volume renderings become projections when viewed on a
2-dimensional display, making the distinction between projections and volume renderings a bit vague. The epitomes of volume rendering models feature a mix of for example coloring and shading in order to create realistic and observable representations.
Two-dimensional CT images are conventionally rendered so that the view is as though looking up at it from the patient's feet.
Hence, the left side of the image is to the patient's right and vice versa, while anterior in the image also is the patient's anterior and vice versa. This left-right interchange corresponds to the view that physicians generally have in reality when positioned in front of patients.
Grayscale
Pixel
In digital imaging, a pixel (abbreviated px), pel, or picture element is the smallest addressable element in a Raster graphics, raster image, or the smallest addressable element in a dot matrix display device. In most digital display devices, p ...
s in an image obtained by CT scanning are displayed in terms of relative
radiodensity. The pixel itself is displayed according to the mean
attenuation
In physics, attenuation (in some contexts, extinction) is the gradual loss of flux intensity through a Transmission medium, medium. For instance, dark glasses attenuate sunlight, lead attenuates X-rays, and water and air attenuate both light and ...
of the tissue(s) that it corresponds to on a scale from +3,071 (most attenuating) to ŌłÆ1,024 (least attenuating) on the
Hounsfield scale. A
pixel
In digital imaging, a pixel (abbreviated px), pel, or picture element is the smallest addressable element in a Raster graphics, raster image, or the smallest addressable element in a dot matrix display device. In most digital display devices, p ...
is a two dimensional unit based on the matrix size and the field of view. When the CT slice thickness is also factored in, the unit is known as a
voxel, which is a three-dimensional unit. Water has an attenuation of 0
Hounsfield units (HU), while air is ŌłÆ1,000 HU, cancellous bone is typically +400 HU, and cranial bone can reach 2,000 HU. The attenuation of metallic implants depends on the atomic number of the element used: Titanium usually has an amount of +1000 HU, iron steel can completely block the X-ray and is, therefore, responsible for well-known line-artifacts in computed tomograms. Artifacts are caused by abrupt transitions between low- and high-density materials, which results in data values that exceed the dynamic range of the processing electronics.
Windowing
CT data sets have a very high
dynamic range which must be reduced for display or printing. This is typically done via a process of "windowing", which maps a range (the "window") of pixel values to a grayscale ramp. For example, CT images of the brain are commonly viewed with a window extending from 0 HU to 80 HU. Pixel values of 0 and lower, are displayed as black; values of 80 and higher are displayed as white; values within the window are displayed as a gray intensity proportional to position within the window. The window used for display must be matched to the X-ray density of the object of interest, in order to optimize the visible detail. Window width and window level parameters are used to control the windowing of a scan.
Multiplanar reconstruction and projections

Multiplanar reconstruction (MPR) is the process of converting data from one
anatomical plane
An anatomical plane is a hypothetical plane used to transect the body, in order to describe the location of structures or the direction of movements.
In human anatomy and non-human anatomy, four principal planes are used: the median plane, ...
(usually
transverse) to other planes. It can be used for thin slices as well as projections. Multiplanar reconstruction is possible as present CT scanners provide almost
isotropic
In physics and geometry, isotropy () is uniformity in all orientations. Precise definitions depend on the subject area. Exceptions, or inequalities, are frequently indicated by the prefix ' or ', hence '' anisotropy''. ''Anisotropy'' is also ...
resolution.
MPR is used almost in every scan. The spine is frequently examined with it. An image of the spine in axial plane can only show one vertebral bone at a time and cannot show its relation with other vertebral bones. By reformatting the data in other planes, visualization of the relative position can be achieved in sagittal and coronal plane.
New software allows the reconstruction of data in non-orthogonal (oblique) planes, which help in the visualization of organs which are not in orthogonal planes. It is better suited for visualization of the anatomical structure of the bronchi as they do not lie orthogonal to the direction of the scan.
Curved-plane reconstruction (or curved planar reformation = CPR) is performed mainly for the evaluation of vessels. This type of reconstruction helps to straighten the bends in a vessel, thereby helping to visualize a whole vessel in a single image or in multiple images. After a vessel has been "straightened", measurements such as cross-sectional area and length can be made. This is helpful in preoperative assessment of a surgical procedure.
For 2D projections used in
radiation therapy
Radiation therapy or radiotherapy (RT, RTx, or XRT) is a therapy, treatment using ionizing radiation, generally provided as part of treatment of cancer, cancer therapy to either kill or control the growth of malignancy, malignant cell (biology), ...
for quality assurance and planning of
external beam radiotherapy, including digitally reconstructed radiographs, see
Beam's eye view.
Volume rendering

A threshold value of radiodensity is set by the operator (e.g., a level that corresponds to bone). With the help of
edge detection image processing algorithms a 3D model can be constructed from the initial data and displayed on screen. Various thresholds can be used to get multiple models, each anatomical component such as muscle, bone and cartilage can be differentiated on the basis of different colours given to them. However, this mode of operation cannot show interior structures.
Surface rendering is limited technique as it displays only the surfaces that meet a particular threshold density, and which are towards the viewer. However, In volume rendering, transparency, colours and
shading are used which makes it easy to present a volume in a single image. For example, Pelvic bones could be displayed as semi-transparent, so that, even viewing at an oblique angle one part of the image does not hide another.
Image quality

Dose versus image quality
An important issue within radiology today is how to reduce the radiation dose during CT examinations without compromising the image quality. In general, higher radiation doses result in higher-resolution images,
while lower doses lead to increased image noise and unsharp images. However, increased dosage raises the adverse side effects, including the risk of
radiation-induced cancer ŌĆō a four-phase abdominal CT gives the same radiation dose as 300 chest X-rays. Several methods that can reduce the exposure to ionizing radiation during a CT scan exist.
[Barkan, O; Weill, J; Averbuch, A; Dekel, S]
"Adaptive Compressed Tomography Sensing"
. In Proceedings of the IEEE Conference on Computer Vision and Pattern Recognition 2013 (pp. 2195ŌĆō2202).
# New software technology can significantly reduce the required radiation dose. New
iterative tomographic reconstruction algorithms (''e.g.'',
iterative Sparse Asymptotic Minimum Variance) could offer
super-resolution without requiring higher radiation dose.
# Individualize the examination and adjust the radiation dose to the body type and body organ examined. Different body types and organs require different amounts of radiation.
# Higher resolution is not always suitable, such as detection of small pulmonary masses.
Artifacts
Although images produced by CT are generally faithful representations of the scanned volume, the technique is susceptible to a number of
artifacts, such as the following:
;: Streaks are often seen around materials that block most X-rays, such as metal or bone. Numerous factors contribute to these streaks: under sampling, photon starvation, motion, beam hardening, and
Compton scatter. This type of artifact commonly occurs in the posterior fossa of the brain, or if there are metal implants. The streaks can be reduced using newer reconstruction techniques.
Approaches such as metal artifact reduction (MAR) can also reduce this artifact.
MAR techniques include spectral imaging, where CT images are taken with
photons of different energy levels, and then synthesized into
monochromatic
A monochrome or monochromatic image, object or palette is composed of one color (or values of one color). Images using only shades of grey are called grayscale (typically digital) or black-and-white (typically analog). In physics, mon ...
images with special software such as GSI (Gemstone Spectral Imaging).
;Partial volume effect: This appears as "blurring" of edges. It is due to the scanner being unable to differentiate between a small amount of high-density material (e.g., bone) and a larger amount of lower density (e.g., cartilage). The reconstruction assumes that the X-ray attenuation within each voxel is homogeneous; this may not be the case at sharp edges. This is most commonly seen in the z-direction (craniocaudal direction), due to the conventional use of highly
anisotropic
Anisotropy () is the structural property of non-uniformity in different directions, as opposed to isotropy. An anisotropic object or pattern has properties that differ according to direction of measurement. For example, many materials exhibit ver ...
voxels, which have a much lower out-of-plane resolution, than in-plane resolution. This can be partially overcome by scanning using thinner slices, or an isotropic acquisition on a modern scanner.
;Ring artifact: Probably the most common mechanical artifact, the image of one or many "rings" appears within an image. They are usually caused by the variations in the response from individual elements in a two dimensional X-ray detector due to defect or miscalibration.
Ring artifacts can largely be reduced by intensity normalization, also referred to as flat field correction.
Remaining rings can be suppressed by a transformation to polar space, where they become linear stripes.
A comparative evaluation of ring artefact reduction on X-ray tomography images showed that the method of Sijbers and Postnov can effectively suppress ring artefacts.
;Noise: This appears as grain on the image and is caused by a low signal to noise ratio. This occurs more commonly when a thin slice thickness is used. It can also occur when the power supplied to the X-ray tube is insufficient to penetrate the anatomy.
;Windmill: Streaking appearances can occur when the detectors intersect the reconstruction plane. This can be reduced with filters or a reduction in pitch.
;Beam hardening: This can give a "cupped appearance" when grayscale is visualized as height. It occurs because conventional sources, like X-ray tubes emit a polychromatic spectrum. Photons of higher
photon energy levels are typically attenuated less. Because of this, the mean energy of the spectrum increases when passing the object, often described as getting "harder". This leads to an effect increasingly underestimating material thickness, if not corrected. Many algorithms exist to correct for this artifact. They can be divided into mono- and multi-material methods.
Advantages
CT scanning has several advantages over traditional
two-dimensional
A two-dimensional space is a mathematical space with two dimensions, meaning points have two degrees of freedom: their locations can be locally described with two coordinates or they can move in two independent directions. Common two-dimension ...
medical
radiography
Radiography is an imaging technology, imaging technique using X-rays, gamma rays, or similar ionizing radiation and non-ionizing radiation to view the internal form of an object. Applications of radiography include medical ("diagnostic" radiog ...
. First, CT eliminates the superimposition of images of structures outside the area of interest. Second, CT scans have greater
image resolution
Image resolution is the level of detail of an image. The term applies to digital images, film images, and other types of images. "Higher resolution" means more image detail.
Image resolution can be measured in various ways. Resolution quantifies ...
, enabling examination of finer details. CT can distinguish between
tissues that differ in
radiographic density by 1% or less. Third, CT scanning enables multiplanar reformatted imaging: scan data can be visualized in the
transverse (or axial),
coronal, or
sagittal
The sagittal plane (; also known as the longitudinal plane) is an anatomical plane that divides the body into right and left sections. It is perpendicular to the transverse plane, transverse and coronal plane, coronal planes. The plane may be in ...
plane, depending on the diagnostic task.
The improved resolution of CT has permitted the development of new investigations. For example, CT
angiography
Angiography or arteriography is a medical imaging technique used to visualize the inside, or lumen, of blood vessels and organs of the body, with particular interest in the arteries, veins, and the heart chambers. Modern angiography is perfo ...
avoids the invasive insertion of a
catheter
In medicine, a catheter ( ) is a thin tubing (material), tube made from medical grade materials serving a broad range of functions. Catheters are medical devices that can be inserted in the body to treat diseases or perform a surgical procedure. ...
. CT scanning can perform a
virtual colonoscopy with greater accuracy and less discomfort for the patient than a traditional
colonoscopy
Colonoscopy () or coloscopy () is a medical procedure involving the Endoscopy, endoscopic examination of the large bowel (colon) and the distal portion of the small bowel. This examination is performed using either a Charge-coupled device, CCD ...
.
Virtual colonography is far more accurate than a
barium enema for detection of tumors and uses a lower radiation dose.
CT is a moderate-to-high
radiation
In physics, radiation is the emission or transmission of energy in the form of waves or particles through space or a material medium. This includes:
* ''electromagnetic radiation'' consisting of photons, such as radio waves, microwaves, infr ...
diagnostic technique. The radiation dose for a particular examination depends on multiple factors: volume scanned, patient build, number and type of scan protocol, and desired resolution and image quality. Two helical CT scanning parameters, tube current and pitch, can be adjusted easily and have a profound effect on radiation. CT scanning is more accurate than two-dimensional radiographs in evaluating anterior interbody fusion, although they may still over-read the extent of fusion.
Adverse effects
Cancer
The
radiation
In physics, radiation is the emission or transmission of energy in the form of waves or particles through space or a material medium. This includes:
* ''electromagnetic radiation'' consisting of photons, such as radio waves, microwaves, infr ...
used in CT scans can damage body cells, including
DNA molecules, which can lead to
radiation-induced cancer.
The radiation doses received from CT scans is variable. Compared to the lowest dose X-ray techniques, CT scans can have 100 to 1,000 times higher dose than conventional X-rays.
[Redberg, Rita F., and Smith-Bindman, Rebecca]
"We Are Giving Ourselves Cancer"
, ''New York Times'', January 30, 2014 However, a lumbar spine X-ray has a similar dose as a head CT. Articles in the media often exaggerate the relative dose of CT by comparing the lowest-dose X-ray techniques (chest X-ray) with the highest-dose CT techniques. In general, a routine abdominal CT has a radiation dose similar to three years of average
background radiation.
Large scale population-based studies have consistently demonstrated that low dose radiation from CT scans has impacts on cancer incidence in a variety of cancers.
For example, in a large population-based Australian cohort it was found that up to 3.7% of brain cancers were caused by CT scan radiation.
Some experts project that in the future, between three and five percent of all cancers would result from medical imaging.
An Australian study of 10.9 million people reported that the increased incidence of cancer after CT scan exposure in this cohort was mostly due to irradiation. In this group, one in every 1,800 CT scans was followed by an excess cancer. If the lifetime risk of developing cancer is 40% then the absolute risk rises to 40.05% after a CT. The risks of CT scan radiation are especially important in patients undergoing recurrent CT scans within a short time span of one to five years.
Some experts note that CT scans are known to be "overused," and "there is distressingly little evidence of better health outcomes associated with the current high rate of scans."
On the other hand, a recent paper analyzing the data of patients who received high
cumulative doses showed a high degree of appropriate use.
This creates an important issue of cancer risk to these patients. Moreover, a highly significant finding that was previously unreported is that some patients received >100 mSv dose from CT scans in a single day,
which counteracts existing criticisms some investigators may have on the effects of protracted versus acute exposure.
There are contrarian views and the debate is ongoing. Some studies have shown that publications indicating an increased risk of cancer from typical doses of body CT scans are plagued with serious methodological limitations and several highly improbable results, concluding that no evidence indicates such low doses cause any long-term harm.
One study estimated that as many as 0.4% of cancers in the United States resulted from CT scans, and that this may have increased to as much as 1.5 to 2% based on the rate of CT use in 2007.
Others dispute this estimate, as there is no consensus that the low levels of radiation used in CT scans cause damage. Lower radiation doses are used in many cases, such as in the investigation of renal colic.
A person's age plays a significant role in the subsequent risk of cancer.
Estimated lifetime cancer mortality risks from an abdominal CT of a one-year-old is 0.1%, or 1:1000 scans.
The risk for someone who is 40 years old is half that of someone who is 20 years old with substantially less risk in the elderly.
The
International Commission on Radiological Protection estimates that the risk to a fetus being exposed to 10
mGy (a unit of radiation exposure) increases the rate of cancer before 20 years of age from 0.03% to 0.04% (for reference a CT pulmonary angiogram exposes a fetus to 4 mGy).
A 2012 review did not find an association between medical radiation and cancer risk in children noting however the existence of limitations in the evidences over which the review is based. CT scans can be performed with different settings for lower exposure in children with most manufacturers of CT scans as of 2007 having this function built in.
Furthermore, certain conditions can require children to be exposed to multiple CT scans.
Current recommendations are to inform patients of the risks of CT scanning.
However, employees of imaging centers tend not to communicate such risks unless patients ask.
Contrast reactions
In the United States half of CT scans are
contrast CTs using intravenously injected
radiocontrast agent
Radiocontrast agents are substances used to enhance the visibility of internal structures in X-ray-based imaging techniques such as computed tomography (contrast CT), projectional radiography, and fluoroscopy. Radiocontrast agents are typically iod ...
s.
The most common reactions from these agents are mild, including nausea, vomiting, and an itching rash. Severe life-threatening reactions may rarely occur.
Overall reactions occur in 1 to 3% with
nonionic contrast and 4 to 12% of people with
ionic contrast.
Skin rashes may appear within a week to 3% of people.
The old
radiocontrast agent
Radiocontrast agents are substances used to enhance the visibility of internal structures in X-ray-based imaging techniques such as computed tomography (contrast CT), projectional radiography, and fluoroscopy. Radiocontrast agents are typically iod ...
s caused
anaphylaxis in 1% of cases while the newer, low-osmolar agents cause reactions in 0.01ŌĆō0.04% of cases.
Death occurs in about 2 to 30 people per 1,000,000 administrations, with newer agents being safer.
There is a higher risk of mortality in those who are female, elderly or in poor health, usually secondary to either anaphylaxis or
acute kidney injury.
The contrast agent may induce
contrast-induced nephropathy.
This occurs in 2 to 7% of people who receive these agents, with greater risk in those who have preexisting
kidney failure,
preexisting
diabetes
Diabetes mellitus, commonly known as diabetes, is a group of common endocrine diseases characterized by sustained high blood sugar levels. Diabetes is due to either the pancreas not producing enough of the hormone insulin, or the cells of th ...
, or reduced intravascular volume. People with mild kidney impairment are usually advised to ensure full hydration for several hours before and after the injection. For moderate kidney failure, the use of
iodinated contrast should be avoided; this may mean using an alternative technique instead of CT. Those with severe
kidney failure requiring
dialysis require less strict precautions, as their kidneys have so little function remaining that any further damage would not be noticeable and the dialysis will remove the contrast agent; it is normally recommended, however, to arrange dialysis as soon as possible following contrast administration to minimize any adverse effects of the contrast.
In addition to the use of intravenous contrast, orally administered contrast agents are frequently used when examining the abdomen. These are frequently the same as the intravenous contrast agents, merely diluted to approximately 10% of the concentration. However, oral alternatives to iodinated contrast exist, such as very dilute (0.5ŌĆō1% w/v)
barium sulfate
Barium sulfate (or sulphate) is the inorganic compound with the chemical formula Ba SO4. It is a white crystalline solid that is odorless and insoluble in water. It occurs in nature as the mineral barite, which is the main commercial source of ...
suspensions. Dilute barium sulfate has the advantage that it does not cause allergic-type reactions or kidney failure, but cannot be used in patients with suspected bowel perforation or suspected bowel injury, as leakage of barium sulfate from damaged bowel can cause fatal
peritonitis.
Side effects from
contrast agents, administered
intravenously in some CT scans, might impair
kidney
In humans, the kidneys are two reddish-brown bean-shaped blood-filtering organ (anatomy), organs that are a multilobar, multipapillary form of mammalian kidneys, usually without signs of external lobulation. They are located on the left and rig ...
performance in patients with
kidney disease
Kidney disease, or renal disease, technically referred to as nephropathy, is damage to or disease of a kidney. Nephritis is an Inflammation, inflammatory kidney disease and has several types according to the location of the inflammation. Infla ...
, although this risk is now believed to be lower than previously thought.
Scan dose
The table reports average radiation exposures; however, there can be a wide variation in radiation doses between similar scan types, where the highest dose could be as much as 22 times higher than the lowest dose.
A typical plain film X-ray involves radiation dose of 0.01 to 0.15 mGy, while a typical CT can involve 10ŌĆō20 mGy for specific organs, and can go up to 80 mGy for certain specialized CT scans.
For purposes of comparison, the world average dose rate from naturally occurring sources of
background radiation is 2.4
mSv per year, equal for practical purposes in this application to 2.4 mGy per year.
While there is some variation, most people (99%) received less than 7 mSv per year as background radiation. Medical imaging as of 2007 accounted for half of the radiation exposure of those in the United States with CT scans making up two thirds of this amount.
In the United Kingdom it accounts for 15% of radiation exposure.
The average radiation dose from medical sources is Ōēł0.6 mSv per person globally as of 2007.
Those in the nuclear industry in the United States are limited to doses of 50 mSv a year and 100 mSv every 5 years.
Lead
Lead () is a chemical element; it has Chemical symbol, symbol Pb (from Latin ) and atomic number 82. It is a Heavy metal (elements), heavy metal that is density, denser than most common materials. Lead is Mohs scale, soft and Ductility, malleabl ...
is the main material used by radiography personnel for
shielding against scattered X-rays.
Radiation dose units
The radiation dose reported in the
gray or mGy unit is proportional to the amount of energy that the irradiated body part is expected to absorb, and the physical effect (such as DNA
double strand breaks) on the cells' chemical bonds by X-ray radiation is proportional to that energy.
The
sievert
The sievert (symbol: SvPlease note there are two non-SI units that use the same Sv abbreviation: the sverdrup and svedberg.) is a derived unit in the International System of Units (SI) intended to represent the stochastic health risk of ionizin ...
unit is used in the report of the
effective dose. The sievert unit, in the context of CT scans, does not correspond to the actual radiation dose that the scanned body part absorbs but to another radiation dose of another scenario, the whole body absorbing the other radiation dose and the other radiation dose being of a magnitude, estimated to have the same probability to induce cancer as the CT scan. Thus, as is shown in the table above, the actual radiation that is absorbed by a scanned body part is often much larger than the effective dose suggests. A specific measure, termed the
computed tomography dose index (CTDI), is commonly used as an estimate of the radiation absorbed dose for tissue within the scan region, and is automatically computed by medical CT scanners.
The
equivalent dose is the effective dose of a case, in which the whole body would actually absorb the same radiation dose, and the sievert unit is used in its report. In the case of non-uniform radiation, or radiation given to only part of the body, which is common for CT examinations, using the local equivalent dose alone would overstate the biological risks to the entire organism.
Effects of radiation
Most adverse health effects of radiation exposure may be grouped in two general categories:
*deterministic effects (harmful tissue reactions) due in large part to the killing/malfunction of cells following high doses;
*stochastic effects, i.e., cancer and heritable effects involving either cancer development in exposed individuals owing to mutation of somatic cells or heritable disease in their offspring owing to mutation of reproductive (germ) cells.
The added lifetime risk of developing cancer by a single abdominal CT of 8 mSv is estimated to be 0.05%, or 1 one in 2,000.
Because of increased susceptibility of fetuses to radiation exposure, the radiation dosage of a CT scan is an important consideration in the choice of
medical imaging in pregnancy
Medical imaging in pregnancy may be Indication (medicine), indicated because of complications of pregnancy, pregnancy complications, intercurrent disease in pregnancy, intercurrent diseases or routine prenatal care.
Options
Options for medical ...
.
Excess doses
In October, 2009, the US
Food and Drug Administration
The United States Food and Drug Administration (FDA or US FDA) is a List of United States federal agencies, federal agency of the United States Department of Health and Human Services, Department of Health and Human Services. The FDA is respo ...
(FDA) initiated an investigation of brain perfusion CT (PCT) scans, based on
radiation burns caused by incorrect settings at one particular facility for this particular type of CT scan. Over 200 patients were exposed to radiation at approximately eight times the expected dose for an 18-month period; over 40% of them lost patches of hair. This event prompted a call for increased CT quality assurance programs. It was noted that "while unnecessary radiation exposure should be avoided, a medically needed CT scan obtained with appropriate acquisition parameter has benefits that outweigh the radiation risks."
Similar problems have been reported at other centers.
These incidents are believed to be due to
human error
Human error is an action that has been done but that was "not intended by the actor; not desired by a set of rules or an external observer; or that led the task or system outside its acceptable limits".Senders, J.W. and Moray, N.P. (1991) Human Er ...
.
Procedure
CT scan procedure varies according to the type of the study and the organ being imaged. The patient lies on the CT table and the centering of the table is done according to the body part. The IV line is established in case of contrast-enhanced CT. After selecting proper and rate of contrast from the pressure injector, the scout is taken to localize and plan the scan. Once the plan is selected, the contrast is given. The raw data is processed according to the study and proper windowing is done to make scans easy to diagnose.
Preparation
Patient preparation may vary according to the type of scan. The general patient preparation includes.
# Signing the
informed consent
Informed consent is an applied ethics principle that a person must have sufficient information and understanding before making decisions about accepting risk. Pertinent information may include risks and benefits of treatments, alternative treatme ...
.
# Removal of metallic objects and jewelry from the region of interest.
# Changing to the hospital gown according to hospital protocol.
#
Checking of kidney function, especially
creatinine and
urea
Urea, also called carbamide (because it is a diamide of carbonic acid), is an organic compound with chemical formula . This amide has two Amine, amino groups (ŌĆō) joined by a carbonyl functional group (ŌĆōC(=O)ŌĆō). It is thus the simplest am ...
levels (in case of
CECT).
Mechanism
Computed tomography operates by using an
X-ray generator that rotates around the object;
X-ray detectors are positioned on the opposite side of the circle from the X-ray source. As the X-rays pass through the patient, they are attenuated differently by various tissues according to the tissue density. A visual representation of the raw data obtained is called a sinogram, yet it is not sufficient for interpretation. Once the scan data has been acquired, the data must be processed using a form of
tomographic reconstruction, which produces a series of cross-sectional images. These cross-sectional images are made up of small units of pixels or voxels.
Pixel
In digital imaging, a pixel (abbreviated px), pel, or picture element is the smallest addressable element in a Raster graphics, raster image, or the smallest addressable element in a dot matrix display device. In most digital display devices, p ...
s in an image obtained by CT scanning are displayed in terms of relative
radiodensity. The pixel itself is displayed according to the mean
attenuation
In physics, attenuation (in some contexts, extinction) is the gradual loss of flux intensity through a Transmission medium, medium. For instance, dark glasses attenuate sunlight, lead attenuates X-rays, and water and air attenuate both light and ...
of the tissue(s) that it corresponds to on a scale from +3,071 (most attenuating) to ŌłÆ1,024 (least attenuating) on the
Hounsfield scale. A
pixel
In digital imaging, a pixel (abbreviated px), pel, or picture element is the smallest addressable element in a Raster graphics, raster image, or the smallest addressable element in a dot matrix display device. In most digital display devices, p ...
is a two dimensional unit based on the matrix size and the field of view. When the CT slice thickness is also factored in, the unit is known as a
voxel, which is a three-dimensional unit.
Water has an attenuation of 0
Hounsfield units (HU), while air is ŌłÆ1,000 HU, cancellous bone is typically +400 HU, and cranial bone can reach 2,000 HU or more (os temporale) and can cause
artifacts. The attenuation of metallic implants depends on the atomic number of the element used: Titanium usually has an amount of +1000 HU, iron steel can completely extinguish the X-ray and is, therefore, responsible for well-known line-artifacts in computed tomograms. Artifacts are caused by abrupt transitions between low- and high-density materials, which results in data values that exceed the dynamic range of the processing electronics. Two-dimensional CT images are conventionally rendered so that the view is as though looking up at it from the patient's feet.
[Computerized Tomography chapter](_blank)
at University of Connecticut Health Center. Hence, the left side of the image is to the patient's right and vice versa, while anterior in the image also is the patient's anterior and vice versa. This left-right interchange corresponds to the view that physicians generally have in reality when positioned in front of patients.
Initially, the images generated in CT scans were in the
transverse (axial)
anatomical plane
An anatomical plane is a hypothetical plane used to transect the body, in order to describe the location of structures or the direction of movements.
In human anatomy and non-human anatomy, four principal planes are used: the median plane, ...
, perpendicular to the long axis of the body. Modern scanners allow the scan data to be reformatted as images in other
planes.
Digital geometry processing can generate a
three-dimensional
In geometry, a three-dimensional space (3D space, 3-space or, rarely, tri-dimensional space) is a mathematical space in which three values (''coordinates'') are required to determine the position (geometry), position of a point (geometry), poi ...
image of an object inside the body from a series of two-dimensional
radiographic images taken by
rotation around a fixed axis
Rotation around a fixed axis or axial rotation is a special case of rotational motion around an ''axis of rotation'' fixed, stationary, or static in three-dimensional space. This type of motion excludes the possibility of the instantaneous axis ...
.
These cross-sectional images are widely used for medical
diagnosis
Diagnosis (: diagnoses) is the identification of the nature and cause of a certain phenomenon. Diagnosis is used in a lot of different academic discipline, disciplines, with variations in the use of logic, analytics, and experience, to determine " ...
and
therapy
A therapy or medical treatment is the attempted remediation of a health problem, usually following a medical diagnosis. Both words, ''treatment'' and ''therapy'', are often abbreviated tx, Tx, or Tx.
As a rule, each therapy has indications a ...
.
Contrast
Contrast media
A contrast agent (or contrast medium) is a substance used to increase the contrast of structures or fluids within the body in medical imaging. Contrast agents absorb or alter external electromagnetism or ultrasound, which is different from radio ...
used for X-ray CT, as well as for
plain film X-ray, are called
radiocontrast
Radiocontrast agents are substances used to enhance the visibility of internal structures in X-ray-based imaging techniques such as computed tomography (contrast CT), projectional radiography, and fluoroscopy. Radiocontrast agents are typically iod ...
s. Radiocontrasts for CT are, in general, iodine-based. This is useful to highlight structures such as blood vessels that otherwise would be difficult to delineate from their surroundings. Using contrast material can also help to obtain functional information about tissues. Often, images are taken both with and without radiocontrast.
History
The history of X-ray computed tomography goes back to at least 1917 with the mathematical theory of the
Radon transform.
In October 1963,
William H. Oldendorf received a U.S. patent for a "radiant energy apparatus for investigating selected areas of interior objects obscured by dense material".
The first commercially viable CT scanner was invented by
Godfrey Hounsfield in 1972.
It is often claimed that revenues from the sales of The Beatles' records in the 1960s helped fund the development of the first CT scanner at EMI. The first production X-ray CT machines were in fact called EMI scanners.
Etymology
The word ''tomography'' is derived from the
Greek 'slice' and 'to write'. Computed tomography was originally known as the "EMI scan" as it was developed in the early 1970s at a research branch of
EMI, a company best known today for its music and recording business. It was later known as ''computed axial tomography'' (''CAT'' or ''CT scan'') and ''body section r├Čntgenography''.
The term ''CAT scan'' is no longer in technical use because current CT scans enable for multiplanar reconstructions. This makes ''CT scan'' the most appropriate term, which is used by
radiologist
Radiology ( ) is the medical specialty that uses medical imaging to diagnose diseases and guide treatment within the bodies of humans and other animals. It began with radiography (which is why its name has a root referring to radiation), but tod ...
s in common vernacular as well as in textbooks and scientific papers.
In
Medical Subject Headings
Medical Subject Headings (MeSH) is a comprehensive controlled vocabulary for the purpose of indexing Academic journal, journal articles and books in the Life science, life sciences. It serves as a thesaurus of index terms that facilitates searc ...
(MeSH), ''computed axial tomography'' was used from 1977 to 1979, but the current indexing explicitly includes ''X-ray'' in the title.
The term
''sinogram'' was introduced by Paul Edholm and Bertil Jacobson in 1975.
Society and culture
Campaigns
In response to increased concern by the public and the ongoing progress of best practices, the Alliance for Radiation Safety in Pediatric Imaging was formed within the
Society for Pediatric Radiology. In concert with the
American Society of Radiologic Technologists, the
American College of Radiology and the
American Association of Physicists in Medicine, the Society for Pediatric Radiology developed and launched the Image Gently Campaign which is designed to maintain high-quality imaging studies while using the lowest doses and best radiation safety practices available on pediatric patients. This initiative has been endorsed and applied by a growing list of various professional medical organizations around the world and has received support and assistance from companies that manufacture equipment used in Radiology.
Following upon the success of the ''Image Gently'' campaign, the American College of Radiology, the Radiological Society of North America, the American Association of Physicists in Medicine and the American Society of Radiologic Technologists have launched a similar campaign to address this issue in the adult population called ''Image Wisely''.
The
World Health Organization
The World Health Organization (WHO) is a list of specialized agencies of the United Nations, specialized agency of the United Nations which coordinates responses to international public health issues and emergencies. It is headquartered in Gen ...
and
International Atomic Energy Agency
The International Atomic Energy Agency (IAEA) is an intergovernmental organization that seeks to promote the peaceful use of nuclear technology, nuclear energy and to inhibit its use for any military purpose, including nuclear weapons. It was ...
(IAEA) of the United Nations have also been working in this area and have ongoing projects designed to broaden best practices and lower patient radiation dose.
Prevalence
Use of CT has increased dramatically over the last two decades.
An estimated 72 million scans were performed in the United States in 2007,
accounting for close to half of the total per-capita dose rate from radiologic and nuclear medicine procedures. Of the CT scans, six to eleven percent are done in children,
an increase of seven to eightfold from 1980.
Similar increases have been seen in Europe and Asia.
In Calgary, Canada, 12.1% of people who present to the emergency with an urgent complaint received a CT scan, most commonly either of the head or of the abdomen. The percentage who received CT, however, varied markedly by the
emergency physician who saw them from 1.8% to 25%. In the emergency department in the United States, CT or
MRI imaging is done in 15% of people who present with
injuries as of 2007 (up from 6% in 1998).
The increased use of CT scans has been the greatest in two fields: screening of adults (screening CT of the lung in smokers, virtual colonoscopy, CT cardiac screening, and whole-body CT in asymptomatic patients) and CT imaging of children. Shortening of the scanning time to around 1 second, eliminating the strict need for the subject to remain still or be sedated, is one of the main reasons for the large increase in the pediatric population (especially for the diagnosis of
appendicitis
Appendicitis is inflammation of the Appendix (anatomy), appendix. Symptoms commonly include right lower abdominal pain, nausea, vomiting, fever and anorexia (symptom), decreased appetite. However, approximately 40% of people do not have these t ...
).
As of 2007, in the United States a proportion of CT scans are performed unnecessarily.
Some estimates place this number at 30%.
There are a number of reasons for this including: legal concerns, financial incentives, and desire by the public.
For example, some healthy people avidly pay to receive full-body CT scans as
screening. In that case, it is not at all clear that the benefits outweigh the risks and costs. Deciding whether and how to treat
incidentalomas is complex, radiation exposure is not negligible, and the money for the scans involves
opportunity cost
In microeconomic theory, the opportunity cost of a choice is the value of the best alternative forgone where, given limited resources, a choice needs to be made between several mutually exclusive alternatives. Assuming the best choice is made, ...
.
Manufacturers
Major manufacturers of CT scanning devices and equipment are:
*
Canon Medical Systems Corporation
*
Fujifilm Healthcare
*
GE HealthCare
*
Neusoft Medical Systems
*
Philips
Koninklijke Philips N.V. (), simply branded Philips, is a Dutch multinational health technology company that was founded in Eindhoven in 1891. Since 1997, its world headquarters have been situated in Amsterdam, though the Benelux headquarter ...
*
Siemens Healthineers
*
United Imaging
Research
Photon-counting computed tomography is a CT technique currently under development. Typical CT scanners use energy integrating detectors; photons are measured as a voltage on a capacitor which is proportional to the X-rays detected. However, this technique is susceptible to noise and other factors which can affect the linearity of the voltage to X-ray intensity relationship. Photon counting detectors (PCDs) are still affected by noise but it does not change the measured counts of photons. PCDs have several potential advantages, including improving signal (and contrast) to noise ratios, reducing doses, improving spatial resolution, and through use of several energies, distinguishing multiple contrast agents. PCDs have only recently become feasible in CT scanners due to improvements in detector technologies that can cope with the volume and rate of data required. As of February 2016, photon counting CT is in use at three sites. Some early research has found the dose reduction potential of photon counting CT for breast imaging to be very promising. In view of recent findings of high cumulative doses to patients from recurrent CT scans, there has been a push for scanning technologies and techniques that reduce ionising radiation doses to patients to sub-
milliSievert (sub-mSv in the literature) levels during the CT scan process, a goal that has been lingering.
See also
*
Barium sulfate suspension
*
Cone beam computed tomography
*
Dosimetry
*
Tomosynthesis
*
Virtopsy
*
X-ray microtomography
*
Xenon-enhanced CT scanning
References
External links
Development of CT imagingĆöPPT by David Platten
*
*
{{DEFAULTSORT:Computed Tomography
1972 introductions
Articles containing video clips
Diagnostic medical imaging
Medical tests
Multidimensional signal processing
Radiology
 CT perfusion imaging is a specific form of CT to assess flow through
CT perfusion imaging is a specific form of CT to assess flow through  Positron emission tomographyŌĆōcomputed tomography is a hybrid CT modality which combines, in a single gantry, a
Positron emission tomographyŌĆōcomputed tomography is a hybrid CT modality which combines, in a single gantry, a  CT scanning of the head is typically used to detect
CT scanning of the head is typically used to detect  Multiplanar reconstruction (MPR) is the process of converting data from one
Multiplanar reconstruction (MPR) is the process of converting data from one  A threshold value of radiodensity is set by the operator (e.g., a level that corresponds to bone). With the help of edge detection image processing algorithms a 3D model can be constructed from the initial data and displayed on screen. Various thresholds can be used to get multiple models, each anatomical component such as muscle, bone and cartilage can be differentiated on the basis of different colours given to them. However, this mode of operation cannot show interior structures.
Surface rendering is limited technique as it displays only the surfaces that meet a particular threshold density, and which are towards the viewer. However, In volume rendering, transparency, colours and shading are used which makes it easy to present a volume in a single image. For example, Pelvic bones could be displayed as semi-transparent, so that, even viewing at an oblique angle one part of the image does not hide another.
A threshold value of radiodensity is set by the operator (e.g., a level that corresponds to bone). With the help of edge detection image processing algorithms a 3D model can be constructed from the initial data and displayed on screen. Various thresholds can be used to get multiple models, each anatomical component such as muscle, bone and cartilage can be differentiated on the basis of different colours given to them. However, this mode of operation cannot show interior structures.
Surface rendering is limited technique as it displays only the surfaces that meet a particular threshold density, and which are towards the viewer. However, In volume rendering, transparency, colours and shading are used which makes it easy to present a volume in a single image. For example, Pelvic bones could be displayed as semi-transparent, so that, even viewing at an oblique angle one part of the image does not hide another.