Alzheimer's disease on:
[Wikipedia]
[Google]
[Amazon]
Alzheimer's disease (AD) is a
 During the final stage, known as the late-stage or severe stage, there is complete dependence on caregivers. Language is reduced to simple phrases or even single words, eventually leading to complete loss of speech. Despite the loss of verbal language abilities, people can often understand and return emotional signals. Although aggressiveness can still be present, extreme
During the final stage, known as the late-stage or severe stage, there is complete dependence on caregivers. Language is reduced to simple phrases or even single words, eventually leading to complete loss of speech. Despite the loss of verbal language abilities, people can often understand and return emotional signals. Although aggressiveness can still be present, extreme
 The
The
 Alzheimer's disease can only be definitively diagnosed with autopsy findings; in the absence of autopsy, clinical diagnoses of AD are "possible" or "probable", based on other findings. Up to 23% of those clinically diagnosed with AD may be misdiagnosed and may have pathology suggestive of another condition with symptoms that mimic those of AD.
AD is usually clinically diagnosed based on the person's
Alzheimer's disease can only be definitively diagnosed with autopsy findings; in the absence of autopsy, clinical diagnoses of AD are "possible" or "probable", based on other findings. Up to 23% of those clinically diagnosed with AD may be misdiagnosed and may have pathology suggestive of another condition with symptoms that mimic those of AD.
AD is usually clinically diagnosed based on the person's

 There are no disease-modifying treatments available to cure Alzheimer's disease and because of this, AD research has focused on interventions to prevent the onset and progression. There is no evidence that supports any particular measure in preventing Alzheimer's, and studies of measures to prevent the onset or progression have produced inconsistent results. Epidemiological studies have proposed relationships between an individual's likelihood of developing AD and modifiable factors, such as medications, lifestyle, and diet. There are some challenges in determining whether interventions for Alzheimer's disease act as a primary prevention method, preventing the disease itself, or a secondary prevention method, identifying the early stages of the disease. These challenges include duration of intervention, different stages of disease at which intervention begins, and lack of standardization of inclusion criteria regarding biomarkers specific for Alzheimer's disease. Further research is needed to determine factors that can help prevent Alzheimer's disease.
There are no disease-modifying treatments available to cure Alzheimer's disease and because of this, AD research has focused on interventions to prevent the onset and progression. There is no evidence that supports any particular measure in preventing Alzheimer's, and studies of measures to prevent the onset or progression have produced inconsistent results. Epidemiological studies have proposed relationships between an individual's likelihood of developing AD and modifiable factors, such as medications, lifestyle, and diet. There are some challenges in determining whether interventions for Alzheimer's disease act as a primary prevention method, preventing the disease itself, or a secondary prevention method, identifying the early stages of the disease. These challenges include duration of intervention, different stages of disease at which intervention begins, and lack of standardization of inclusion criteria regarding biomarkers specific for Alzheimer's disease. Further research is needed to determine factors that can help prevent Alzheimer's disease.

 Medications used to treat the cognitive problems of Alzheimer's disease include: four
Medications used to treat the cognitive problems of Alzheimer's disease include: four
lay summary
January 2009. Stopping antipsychotic use in this group of people appears to be safe.
 The ancient Greek and Roman philosophers and
The ancient Greek and Roman philosophers and
neurodegenerative disease
A neurodegenerative disease is caused by the progressive loss of structure or function of neurons, in the process known as neurodegeneration. Such neuronal damage may ultimately involve cell death. Neurodegenerative diseases include amyotrophic ...
that usually starts slowly and progressively worsens. It is the cause of 60–70% of cases of dementia
Dementia is a disorder which manifests as a set of related symptoms, which usually surfaces when the brain is damaged by injury or disease. The symptoms involve progressive impairments in memory, thinking, and behavior, which negatively affe ...
. The most common early symptom is difficulty in remembering recent events. As the disease advances, symptoms can include problems with language, disorientation (including easily getting lost), mood swing
A mood swing is an extreme or sudden change of mood. Such changes can play a positive part in promoting problem solving and in producing flexible forward planning, or be disruptive. When mood swings are severe, they may be categorized as par ...
s, loss of motivation, self-neglect
Self-neglect is a behavioral condition in which an individual neglects to attend to their basic needs, such as personal hygiene, appropriate clothing, feeding, or tending appropriately to any medical conditions they have. More generally, any lack ...
, and behavioral issues. As a person's condition declines, they often withdraw from family and society. Gradually, bodily functions are lost, ultimately leading to death. Although the speed of progression can vary, the typical life expectancy following diagnosis is three to nine years.
The cause of Alzheimer's disease is poorly understood. There are many environmental and genetic risk factor
In epidemiology, a risk factor or determinant is a variable associated with an increased risk of disease or infection.
Due to a lack of harmonization across disciplines, determinant, in its more widely accepted scientific meaning, is often ...
s associated with its development. The strongest genetic risk factor is from an allele of APOE. Other risk factors include a history of head injury
A head injury is any injury that results in trauma to the skull or brain. The terms ''traumatic brain injury'' and ''head injury'' are often used interchangeably in the medical literature. Because head injuries cover such a broad scope of inju ...
, clinical depression
Major depressive disorder (MDD), also known as clinical depression, is a mental disorder characterized by at least two weeks of pervasive low mood, low self-esteem, and loss of interest or pleasure in normally enjoyable activities. Intro ...
, and high blood pressure. The disease process is largely associated with amyloid plaques, neurofibrillary tangles, and loss of neuronal connections in the brain
A brain is an organ that serves as the center of the nervous system in all vertebrate and most invertebrate animals. It is located in the head, usually close to the sensory organs for senses such as vision. It is the most complex organ in a ve ...
. A probable diagnosis is based on the history of the illness and cognitive test
Cognitive tests are assessments of the cognitive capabilities of humans and other animals. Tests administered to humans include various forms of IQ tests; those administered to animals include the mirror test (a test of visual self-awareness) and t ...
ing with medical imaging and blood tests to rule out other possible causes. Initial symptoms are often mistaken for normal aging. Examination of brain tissue is needed for a definite diagnosis, but this can only take place after death
''After Death'' ( it, Oltre la Morte) is an Italian zombie film directed by Claudio Fragasso. The film is set on a remote island where a voodoo curse raises the dead from their graves to feast on the flesh of the living. When a boat of explor ...
. Good nutrition
Nutrition is the biochemical and physiological process by which an organism uses food to support its life. It provides organisms with nutrients, which can be metabolized to create energy and chemical structures. Failure to obtain sufficient ...
, physical activity, and engaging socially are known to be of benefit generally in aging, and these may help in reducing the risk of cognitive decline and Alzheimer's; in 2019 clinical trials were underway to look at these possibilities. There are no medications or supplements that have been shown to decrease risk.
No treatments stop or reverse its progression, though some may temporarily improve symptoms. Affected people increasingly rely on others for assistance, often placing a burden on the caregiver
A caregiver or carer is a paid or unpaid member of a person's social network who helps them with activities of daily living. Since they have no specific professional training, they are often described as informal caregivers. Caregivers most commo ...
. The pressures can include social, psychological, physical, and economic elements. Exercise programs may be beneficial with respect to activities of daily living
Activity may refer to:
* Action (philosophy), in general
* Human activity: human behavior, in sociology behavior may refer to all basic human actions, economics may study human economic activities and along with cybernetics and psychology may s ...
and can potentially improve outcomes. Behavioral problems or psychosis
Psychosis is a condition of the mind that results in difficulties determining what is real and what is not real. Symptoms may include delusions and hallucinations, among other features. Additional symptoms are incoherent speech and behavior ...
due to dementia are often treated with antipsychotic
Antipsychotics, also known as neuroleptics, are a class of psychotropic medication primarily used to manage psychosis (including delusions, hallucinations, paranoia or disordered thought), principally in schizophrenia but also in a range of ...
s, but this is not usually recommended, as there is little benefit and an increased risk of early death.
As of 2020, there were approximately 50 million people worldwide with Alzheimer's disease. It most often begins in people over 65 years of age, although up to 10% of cases are early-onset affecting those in their 30s to mid-60s. It affects about 6% of people 65 years and older, and women more often than men. The disease is named after German psychiatrist and pathologist Alois Alzheimer
Alois Alzheimer ( , , ; 14 June 1864 – 19 December 1915) was a German psychiatrist and neuropathologist and a colleague of Emil Kraepelin. Alzheimer is credited with identifying the first published case of "presenile dementia", which Kraep ...
, who first described it in 1906. Alzheimer's financial burden on society is large, with an estimated global annual cost of trillion. Alzheimer's disease is currently ranked as the seventh leading cause of death in the United States.
Signs and symptoms
The course of Alzheimer's is generally described in three stages, with a progressive pattern of cognitive and functional impairment. The three stages are described as early or mild, middle or moderate, and late or severe. The disease is known to target thehippocampus
The hippocampus (via Latin from Greek , ' seahorse') is a major component of the brain of humans and other vertebrates. Humans and other mammals have two hippocampi, one in each side of the brain. The hippocampus is part of the limbic system, ...
which is associated with memory
Memory is the faculty of the mind by which data or information is encoded, stored, and retrieved when needed. It is the retention of information over time for the purpose of influencing future action. If past events could not be remembered ...
, and this is responsible for the first symptoms of memory impairment. As the disease progresses so does the degree of memory impairment.
First symptoms
The first symptoms are often mistakenly attributed to aging orstress
Stress may refer to:
Science and medicine
* Stress (biology), an organism's response to a stressor such as an environmental condition
* Stress (linguistics), relative emphasis or prominence given to a syllable in a word, or to a word in a phrase ...
. Detailed neuropsychological test
Neuropsychological tests are specifically designed tasks that are used to measure a psychological function known to be linked to a particular brain structure or pathway. Tests are used for research into brain function and in a clinical setting f ...
ing can reveal mild cognitive difficulties up to eight years before a person fulfills the clinical criteria for diagnosis
Diagnosis is the identification of the nature and cause of a certain phenomenon. Diagnosis is used in many different disciplines, with variations in the use of logic, analytics, and experience, to determine " cause and effect". In systems engin ...
of Alzheimer's disease. These early symptoms can affect the most complex activities of daily living
Activity may refer to:
* Action (philosophy), in general
* Human activity: human behavior, in sociology behavior may refer to all basic human actions, economics may study human economic activities and along with cybernetics and psychology may s ...
. The most noticeable deficit is short term memory loss, which shows up as difficulty in remembering recently learned facts and inability to acquire new information.
Subtle problems with the executive functions
In cognitive science and neuropsychology, executive functions (collectively referred to as executive function and cognitive control) are a set of cognitive processes that are necessary for the cognitive control of behavior: selecting and suc ...
of attentiveness, planning, flexibility, and abstract thinking, or impairments in semantic memory
Semantic memory refers to general world knowledge that humans have accumulated throughout their lives. This general knowledge (word meanings, concepts, facts, and ideas) is intertwined in experience and dependent on culture. We can learn about n ...
(memory of meanings, and concept relationships) can also be symptomatic of the early stages of Alzheimer's disease. Apathy
Apathy is a lack of feeling, emotion, interest, or concern about something. It is a state of indifference, or the suppression of emotions such as concern, excitement, motivation, or passion. An apathetic individual has an absence of intere ...
and depression can be seen at this stage, with apathy remaining as the most persistent symptom throughout the course of the disease. Mild cognitive impairment
Mild cognitive impairment (MCI) is a neurocognitive disorder which involves cognitive impairments beyond those expected based on an individual's age and education but which are not significant enough to interfere with instrumental activities o ...
(MCI) is often found to be a transitional stage between normal aging and dementia
Dementia is a disorder which manifests as a set of related symptoms, which usually surfaces when the brain is damaged by injury or disease. The symptoms involve progressive impairments in memory, thinking, and behavior, which negatively affe ...
. MCI can present with a variety of symptoms, and when memory loss is the predominant symptom, it is termed amnestic MCI
Mild cognitive impairment (MCI) is a neurocognitive disorder which involves cognitive impairments beyond those expected based on an individual's age and education but which are not significant enough to interfere with instrumental activities of ...
and is frequently seen as a prodromal
In medicine, a prodrome is an early sign or symptom (or set of signs and symptoms) that often indicates the onset of a disease before more diagnostically specific signs and symptoms develop. It is derived from the Greek word ''prodromos'', meaning ...
stage of Alzheimer's disease. Amnestic MCI has a greater than 90% likelihood of being associated with Alzheimer's.
Early stage
In people with Alzheimer's disease, the increasing impairment of learning and memory eventually leads to a definitive diagnosis. In a small percentage, difficulties with language, executive functions,perception
Perception () is the organization, identification, and interpretation of sensory information in order to represent and understand the presented information or environment. All perception involves signals that go through the nervous system ...
(agnosia
Agnosia is the inability to process sensory information. Often there is a loss of ability to recognize objects, persons, sounds, shapes, or smells while the specific sense is not defective nor is there any significant memory loss. It is usually ...
), or execution of movements (apraxia
Apraxia is a motor disorder caused by damage to the brain (specifically the posterior parietal cortex or corpus callosum), which causes difficulty with motor planning to perform tasks or movements. The nature of the damage determines the disorde ...
) are more prominent than memory problems. Alzheimer's disease does not affect all memory capacities equally. Older memories of the person's life (episodic memory
Episodic memory is the memory of everyday events (such as times, location geography, associated emotions, and other contextual information) that can be explicitly stated or conjured. It is the collection of past personal experiences that occurred ...
), facts learned (semantic memory
Semantic memory refers to general world knowledge that humans have accumulated throughout their lives. This general knowledge (word meanings, concepts, facts, and ideas) is intertwined in experience and dependent on culture. We can learn about n ...
), and implicit memory
In psychology, implicit memory is one of the two main types of long-term human memory. It is acquired and used unconsciously, and can affect thoughts and behaviours. One of its most common forms is procedural memory, which allows people to perfo ...
(the memory of the body on how to do things, such as using a fork to eat or how to drink from a glass) are affected to a lesser degree than new facts or memories.
Language problems are mainly characterised by a shrinking vocabulary
A vocabulary is a set of familiar words within a person's language. A vocabulary, usually developed with age, serves as a useful and fundamental tool for communication and acquiring knowledge. Acquiring an extensive vocabulary is one of the la ...
and decreased word fluency, leading to a general impoverishment of oral and written language
A written language is the representation of a spoken or gestural language by means of a writing system. Written language is an invention in that it must be taught to children, who will pick up spoken language or sign language by exposure eve ...
. In this stage, the person with Alzheimer's is usually capable of communicating basic ideas adequately. While performing fine motor tasks such as writing, drawing, or dressing, certain movement coordination and planning difficulties (apraxia) may be present, but they are commonly unnoticed. As the disease progresses, people with Alzheimer's disease can often continue to perform many tasks independently, but may need assistance or supervision with the most cognitively demanding activities.
Middle stage
Progressive deterioration eventually hinders independence, with subjects being unable to perform most common activities of daily living. Speech difficulties become evident due to an inability to recall vocabulary, which leads to frequent incorrect word substitutions (paraphasia Paraphasia is a type of language output error commonly associated with aphasia, and characterized by the production of unintended syllables, words, or phrases during the effort to speak. Paraphasic errors are most common in patients with fluent for ...
s). Reading and writing skills are also progressively lost. Complex motor sequences become less coordinated as time passes and Alzheimer's disease progresses, so the risk of falling increases. During this phase, memory problems worsen, and the person may fail to recognise close relatives. Long-term memory
Long-term memory (LTM) is the stage of the Atkinson–Shiffrin memory model in which informative knowledge is held indefinitely. It is defined in contrast to short-term and working memory, which persist for only about 18 to 30 seconds. Long- ...
, which was previously intact, becomes impaired.
Behavioral and neuropsychiatric
Neuropsychiatry or Organic Psychiatry is a branch of medicine that deals with psychiatry as it relates to neurology, in an effort to understand and attribute behavior to the interaction of neurobiology and social psychology factors. Within neurop ...
changes become more prevalent. Common manifestations are wandering, irritability
Irritability (also called as crankiness) is the excitatory ability that living organisms have to respond to changes in their environment. The term is used for both the physiological reaction to stimuli and for the pathological, abnormal or excessi ...
and emotional lability
In medicine and psychology, emotional lability is a sign or symptom typified by exaggerated changes in mood or affect in quick succession. Sometimes the emotions expressed outwardly are very different from how the person feels on the inside. Thes ...
, leading to crying, outbursts of unpremeditated aggression, or resistance to caregiving. Sundowning can also appear. Approximately 30% of people with Alzheimer's disease develop illusionary misidentifications and other delusion
A delusion is a false fixed belief that is not amenable to change in light of conflicting evidence. As a pathology, it is distinct from a belief based on false or incomplete information, confabulation, dogma, illusion, hallucination, or som ...
al symptoms. Subjects also lose insight of their disease process and limitations ( anosognosia). Urinary incontinence
Urinary incontinence (UI), also known as involuntary urination, is any uncontrolled leakage of urine. It is a common and distressing problem, which may have a large impact on quality of life. It has been identified as an important issue in geri ...
can develop. These symptoms create stress
Stress may refer to:
Science and medicine
* Stress (biology), an organism's response to a stressor such as an environmental condition
* Stress (linguistics), relative emphasis or prominence given to a syllable in a word, or to a word in a phrase ...
for relatives and caregivers, which can be reduced by moving the person from home care to other long-term care facilities
A nursing home is a facility for the residential care of elderly or disabled people. Nursing homes may also be referred to as skilled nursing facility (SNF) or long-term care facilities. Often, these terms have slightly different meanings to i ...
.
Late stage
 During the final stage, known as the late-stage or severe stage, there is complete dependence on caregivers. Language is reduced to simple phrases or even single words, eventually leading to complete loss of speech. Despite the loss of verbal language abilities, people can often understand and return emotional signals. Although aggressiveness can still be present, extreme
During the final stage, known as the late-stage or severe stage, there is complete dependence on caregivers. Language is reduced to simple phrases or even single words, eventually leading to complete loss of speech. Despite the loss of verbal language abilities, people can often understand and return emotional signals. Although aggressiveness can still be present, extreme apathy
Apathy is a lack of feeling, emotion, interest, or concern about something. It is a state of indifference, or the suppression of emotions such as concern, excitement, motivation, or passion. An apathetic individual has an absence of intere ...
and exhaustion are much more common symptoms. People with Alzheimer's disease will ultimately not be able to perform even the simplest tasks independently; muscle mass and mobility deteriorates to the point where they are bedridden and unable to feed themselves. The cause of death is usually an external factor, such as infection of pressure ulcer
Pressure ulcers, also known as pressure sores, bed sores or pressure injuries, are localised damage to the skin and/or underlying tissue that usually occur over a bony prominence as a result of usually long-term pressure, or pressure in combi ...
s or pneumonia
Pneumonia is an inflammatory condition of the lung primarily affecting the small air sacs known as alveoli. Symptoms typically include some combination of productive or dry cough, chest pain, fever, and difficulty breathing. The severi ...
, not the disease itself.
Causes
Proteins fail to function normally. This disrupts the work of the brain cells affected and triggers a toxic cascade, ultimately leading to cell death and later brain shrinkage. Alzheimer's disease is believed to occur when abnormal amounts of amyloid beta (Aβ), accumulating extracellularly as amyloid plaques andtau
Tau (uppercase Τ, lowercase τ, or \boldsymbol\tau; el, ταυ ) is the 19th letter of the Greek alphabet, representing the voiceless dental or alveolar plosive . In the system of Greek numerals, it has a value of 300.
The name in English ...
protein
Proteins are large biomolecules and macromolecules that comprise one or more long chains of amino acid residues. Proteins perform a vast array of functions within organisms, including catalysing metabolic reactions, DNA replication, res ...
s, or intracellularly as neurofibrillary tangles, form in the brain, affecting neuronal functioning and connectivity, resulting in a progressive loss of brain function. This altered protein clearance ability is age-related, regulated by brain cholesterol, and associated with other neurodegenerative diseases.
Advances in brain imaging techniques allow researchers to see the development and spread of abnormal amyloid and tau proteins in the living brain, as well as changes in brain structure and function. Beta-amyloid is a fragment of a larger protein. When these fragments cluster together, a toxic effect appears on neurons and disrupt cell-to-cell communication. Larger deposits called amyloid plaques are thus further formed.
Tau proteins are responsible in neuron's internal support and transport system to carry nutrients and other essential materials. In Alzheimer's disease, the shape of tau proteins is altered and thus organize themselves into structures called neurofibrillary tangles. The tangles disrupt the transport system and are toxic to cells.
The cause for most Alzheimer's cases is still mostly unknown, except for 1–2% of cases where deterministic genetic differences have been identified. Several competing hypotheses attempt to explain the underlying cause; the two predominant hypotheses are the amyloid beta (Aβ) hypothesis and the cholinergic hypothesis.
The oldest hypothesis, on which most drug therapies are based, is the cholinergic hypothesis, which proposes that Alzheimer's disease is caused by reduced synthesis of the neurotransmitter acetylcholine. The loss of cholinergic neuron
A cholinergic neuron is a nerve cell which mainly uses the neurotransmitter acetylcholine (ACh) to send its messages. Many neurological systems are cholinergic. Cholinergic neurons provide the primary source of acetylcholine to the cerebral corte ...
s noted in the limbic system and cerebral cortex, is a key feature in the progression of Alzheimer's. The 1991 amyloid hypothesis postulated that extracellular amyloid beta (Aβ) deposits are the fundamental cause of the disease. Support for this postulate comes from the location of the gene for the amyloid precursor protein
Amyloid-beta precursor protein (APP) is an integral membrane protein expressed in many tissues and concentrated in the synapses of neurons. It functions as a cell surface receptor and has been implicated as a regulator of synapse format ...
(APP) on chromosome 21
Chromosome 21 is one of the 23 pairs of chromosomes in humans. Chromosome 21 is both the smallest human autosome and chromosome, with 48 million base pairs (the building material of DNA) representing about 1.5 percent of the total DNA in cells. M ...
, together with the fact that people with trisomy 21
A trisomy is a type of polysomy in which there are three instances of a particular chromosome, instead of the normal two. A trisomy is a type of aneuploidy (an abnormal number of chromosomes).
Description and causes
Most organisms that reprodu ...
(Down syndrome) who have an extra gene copy almost universally exhibit at least the earliest symptoms of Alzheimer's disease by 40 years of age. A specific isoform
A protein isoform, or "protein variant", is a member of a set of highly similar proteins that originate from a single gene or gene family and are the result of genetic differences. While many perform the same or similar biological roles, some iso ...
of apolipoprotein, APOE4, is a major genetic risk factor for Alzheimer's disease. While apolipoproteins enhance the breakdown of beta amyloid, some isoforms are not very effective at this task (such as APOE4), leading to excess amyloid buildup in the brain.
Genetic
Only 1–2% of Alzheimer's cases are inherited ( autosomal dominant). These types are known as early onset familial Alzheimer's disease, can have a very early onset, and a faster rate of progression. Early onset familial Alzheimer's disease can be attributed to mutations in one of three genes: those encoding amyloid-beta precursor protein (APP) and presenilins PSEN1 and PSEN2. Most mutations in the APP and presenilin genes increase the production of a small protein called amyloid beta (Aβ)42, which is the main component of amyloid plaques. Some of the mutations merely alter the ratio between Aβ42 and the other major forms—particularly Aβ40—without increasing Aβ42 levels. Two other genes associated with autosomal dominant Alzheimer's disease are ABCA7 and SORL1. Most cases of Alzheimer's are not inherited and are termed sporadic Alzheimer's disease, in which environmental and genetic differences may act asrisk factor
In epidemiology, a risk factor or determinant is a variable associated with an increased risk of disease or infection.
Due to a lack of harmonization across disciplines, determinant, in its more widely accepted scientific meaning, is often ...
s. Most cases of sporadic Alzheimer's disease in contrast to familial Alzheimer's disease are late-onset Alzheimer's disease (LOAD) developing after the age of 65 years. Less than 5% of sporadic Alzheimer's disease have an earlier onset. The strongest genetic risk factor for sporadic Alzheimer's disease is APOEε4. APOEε4 is one of four alleles of apolipoprotein E (APOE). APOE plays a major role in lipid-binding proteins in lipoprotein particles and the epsilon4 allele disrupts this function. Between 40 and 80% of people with Alzheimer's disease possess at least one APOEε4 allele. The APOEε4 allele increases the risk of the disease by three times in heterozygotes and by 15 times in homozygotes. Like many human diseases, environmental effects and genetic modifiers result in incomplete penetrance
Penetrance in genetics is the proportion of individuals carrying a particular variant (or allele) of a gene (the genotype) that also express an associated trait (the phenotype). In medical genetics, the penetrance of a disease-causing mutation is t ...
. For example, certain Nigerian populations do not show the relationship between dose of APOEε4 and incidence or age-of-onset for Alzheimer's disease seen in other human populations.
Allele
An allele (, ; ; modern formation from Greek ἄλλος ''állos'', "other") is a variation of the same sequence of nucleotides at the same place on a long DNA molecule, as described in leading textbooks on genetics and evolution.
::"The chro ...
s in the TREM2 gene have been associated with a 3 to 5 times higher risk of developing Alzheimer's disease.
A Japanese pedigree of familial Alzheimer's disease was found to be associated with a deletion mutation of codon 693 of APP. This mutation and its association with Alzheimer's disease was first reported in 2008, and is known as the Osaka mutation. Only homozygotes with this mutation have an increased risk of developing Alzheimer's disease. This mutation accelerates Aβ oligomerization but the proteins do not form the amyloid fibrils that aggregate into amyloid plaques, suggesting that it is the Aβ oligomerization rather than the fibrils that may be the cause of this disease. Mice expressing this mutation have all the usual pathologies of Alzheimer's disease.
Other hypotheses
 The
The tau hypothesis The biochemistry of Alzheimer's disease, the most common cause of dementia, is not yet very well understood. Alzheimer's disease (AD) has been identified as a proteopathy: a protein misfolding disease due to the accumulation of abnormally folded a ...
proposes that tau protein
The tau proteins (abbreviated from tubulin associated unit) are a group of six highly soluble protein isoforms produced by alternative splicing from the gene ''MAPT'' (microtubule-associated protein tau). They have roles primarily in maintaining ...
abnormalities initiate the disease cascade. In this model, hyperphosphorylated tau begins to pair with other threads of tau as paired helical filaments. Eventually, they form neurofibrillary tangles inside nerve cell bodies. When this occurs, the microtubules disintegrate, destroying the structure of the cell's cytoskeleton
The cytoskeleton is a complex, dynamic network of interlinking protein filaments present in the cytoplasm of all cells, including those of bacteria and archaea. In eukaryotes, it extends from the cell nucleus to the cell membrane and is com ...
which collapses the neuron's transport system.
A number of studies connect the misfolded amyloid beta and tau proteins associated with the pathology of Alzheimer's disease, as bringing about oxidative stress
Oxidative stress reflects an imbalance between the systemic manifestation of reactive oxygen species and a biological system's ability to readily detoxify the reactive intermediates or to repair the resulting damage. Disturbances in the normal ...
that leads to chronic inflammation. Sustained inflammation (neuroinflammation) is also a feature of other neurodegenerative diseases including Parkinson's disease, and ALS. Spirochete infections have also been linked to dementia. DNA damages accumulate in AD brains; reactive oxygen species
In chemistry, reactive oxygen species (ROS) are highly reactive chemicals formed from diatomic oxygen (). Examples of ROS include peroxides, superoxide, hydroxyl radical, singlet oxygen, and alpha-oxygen.
The reduction of molecular oxygen () p ...
may be the major source of this DNA damage.
Sleep disturbance
A sleep disorder, or somnipathy, is a medical disorder of an individual's sleep patterns. Some sleep disorders are severe enough to interfere with normal physical, mental, social and emotional functioning. Polysomnography and actigraphy are tests ...
s are seen as a possible risk factor for inflammation in Alzheimer's disease. Sleep problems have been seen as a consequence of Alzheimer's disease but studies suggest that they may instead be a causal factor. Sleep disturbances are thought to be linked to persistent inflammation. The cellular homeostasis
In biology, homeostasis (British also homoeostasis) (/hɒmɪə(ʊ)ˈsteɪsɪs/) is the state of steady internal, physical, and chemical conditions maintained by living systems. This is the condition of optimal functioning for the organism and ...
of biometals such as ionic copper, iron, and zinc is disrupted in Alzheimer's disease, though it remains unclear whether this is produced by or causes the changes in proteins. Smoking is a significant Alzheimer's disease risk factor. Systemic markers of the innate immune system are risk factors for late-onset Alzheimer's disease. Exposure to air pollution may be a contributing factor to the development of Alzheimer's disease.
One hypothesis posits that dysfunction of oligodendrocytes
Oligodendrocytes (), or oligodendroglia, are a type of neuroglia whose main functions are to provide support and insulation to axons in the central nervous system of jawed vertebrates, equivalent to the function performed by Schwann cells in the ...
and their associated myelin during aging contributes to axon damage, which then causes amyloid production and tau hyper-phosphorylation as a side effect.
Retrogenesis is a medical hypothesis
A hypothesis (plural hypotheses) is a proposed explanation for a phenomenon. For a hypothesis to be a scientific hypothesis, the scientific method requires that one can test it. Scientists generally base scientific hypotheses on previous obse ...
that just as the fetus goes through a process of neurodevelopment beginning with neurulation and ending with myelination, the brains of people with Alzheimer's disease go through a reverse neurodegeneration process starting with demyelination
A demyelinating disease is any disease of the nervous system in which the myelin sheath of neurons is damaged. This damage impairs the conduction of signals in the affected nerves. In turn, the reduction in conduction ability causes deficiency i ...
and death of axons (white matter) and ending with the death of grey matter. Likewise the hypothesis is, that as infants go through states of cognitive development
Cognitive development is a field of study in neuroscience and psychology focusing on a child's development in terms of information processing, conceptual resources, perceptual skill, language learning, and other aspects of the developed adult bra ...
, people with Alzheimer's disease go through the reverse process of progressive cognitive impairment
Cognitive deficit is an inclusive term to describe any characteristic that acts as a barrier to the cognition process.
The term may describe
* deficits in overall intelligence (as with intellectual disabilities),
* specific and restricted defici ...
.
The association with celiac disease
Coeliac disease (British English) or celiac disease (American English) is a long-term autoimmune disorder, primarily affecting the small intestine, where individuals develop intolerance to gluten, present in foods such as wheat, rye and barle ...
is unclear, with a 2019 study finding no increase in dementia overall in those with CD, while a 2018 review found an association with several types of dementia including Alzheimer's disease.
Pathophysiology

Neuropathology
Alzheimer's disease is characterised by loss ofneuron
A neuron, neurone, or nerve cell is an electrically excitable cell that communicates with other cells via specialized connections called synapses. The neuron is the main component of nervous tissue in all animals except sponges and placozoa. ...
s and synapses in the cerebral cortex
The cerebral cortex, also known as the cerebral mantle, is the outer layer of neural tissue of the cerebrum of the brain in humans and other mammals. The cerebral cortex mostly consists of the six-layered neocortex, with just 10% consistin ...
and certain subcortical regions. This loss results in gross atrophy of the affected regions, including degeneration in the temporal lobe
The temporal lobe is one of the four major lobes of the cerebral cortex in the brain of mammals. The temporal lobe is located beneath the lateral fissure on both cerebral hemispheres of the mammalian brain.
The temporal lobe is involved in pro ...
and parietal lobe
The parietal lobe is one of the four major lobes of the cerebral cortex in the brain of mammals. The parietal lobe is positioned above the temporal lobe and behind the frontal lobe and central sulcus.
The parietal lobe integrates sensory informa ...
, and parts of the frontal cortex and cingulate gyrus
The cingulate cortex is a part of the brain situated in the medial aspect of the cerebral cortex. The cingulate cortex includes the entire cingulate gyrus, which lies immediately above the corpus callosum, and the continuation of this in the ...
. Degeneration is also present in brainstem nuclei particularly the locus coeruleus in the pons
The pons (from Latin , "bridge") is part of the brainstem that in humans and other bipeds lies inferior to the midbrain, superior to the medulla oblongata and anterior to the cerebellum.
The pons is also called the pons Varolii ("bridge of Va ...
. Studies using MRI
Magnetic resonance imaging (MRI) is a medical imaging technique used in radiology to form pictures of the anatomy and the physiological processes of the body. MRI scanners use strong magnetic fields, magnetic field gradients, and radio waves ...
and PET
A pet, or companion animal, is an animal kept primarily for a person's company or entertainment rather than as a working animal, livestock, or a laboratory animal. Popular pets are often considered to have attractive appearances, intelligence ...
have documented reductions in the size of specific brain regions in people with Alzheimer's disease as they progressed from mild cognitive impairment to Alzheimer's disease, and in comparison with similar images from healthy older adults.
Both Aβ
Amyloid beta (Aβ or Abeta) denotes peptides of 36–43 amino acids that are the main component of the amyloid plaques found in the brains of people with Alzheimer's disease. The peptides derive from the amyloid precursor protein (APP), which ...
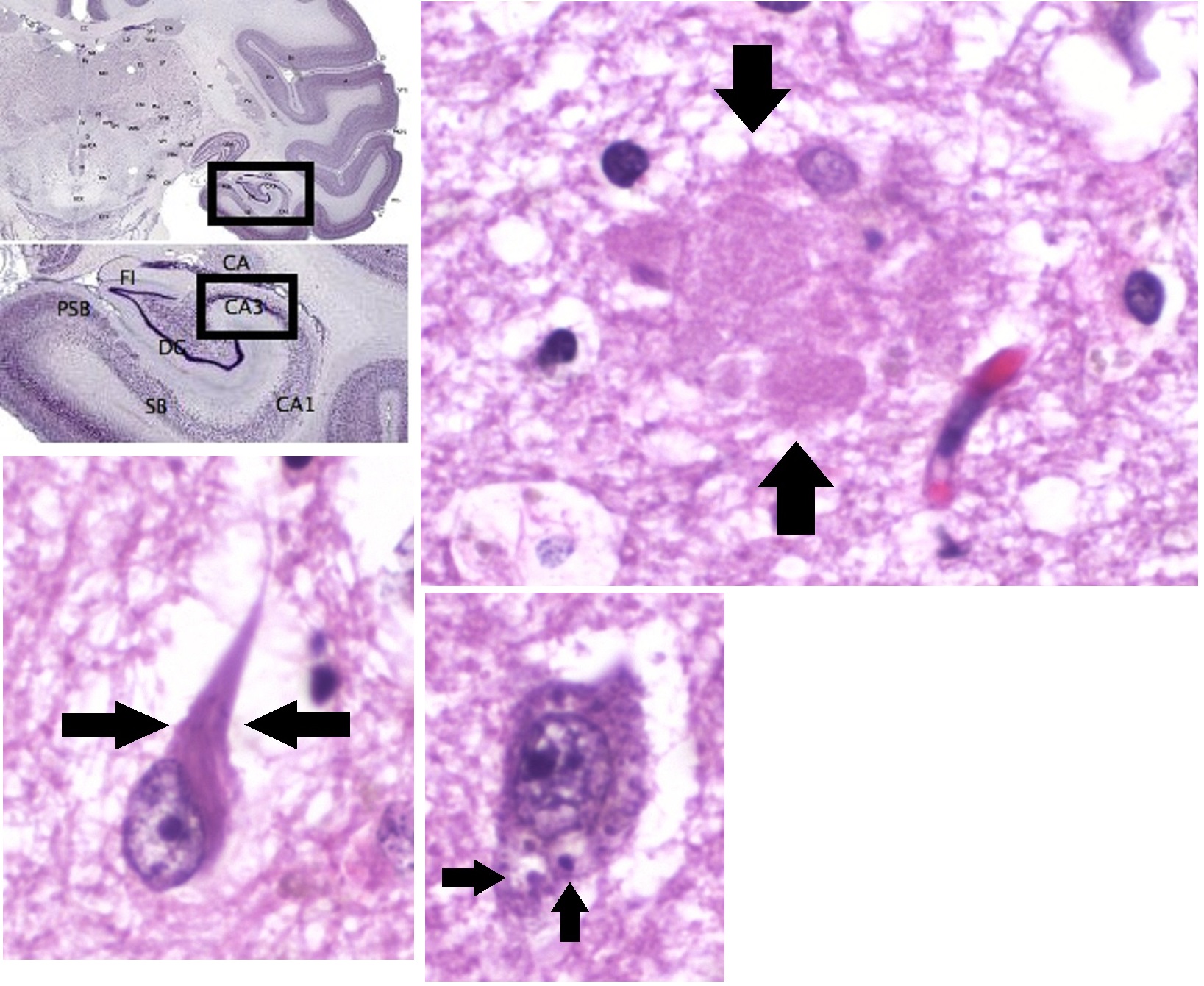
plaques and neurofibrillary tangles are clearly visible by microscopy in brains of those with Alzheimer's disease, especially in the hippocampus
The hippocampus (via Latin from Greek , ' seahorse') is a major component of the brain of humans and other vertebrates. Humans and other mammals have two hippocampi, one in each side of the brain. The hippocampus is part of the limbic system, ...
. However, Alzheimer's disease may occur without neurofibrillary tangles in the neocortex. Plaques are dense, mostly insoluble
In chemistry, solubility is the ability of a substance, the solute, to form a solution with another substance, the solvent. Insolubility is the opposite property, the inability of the solute to form such a solution.
The extent of the solubil ...
deposits of beta-amyloid peptide
Peptides (, ) are short chains of amino acids linked by peptide bonds. Long chains of amino acids are called proteins. Chains of fewer than twenty amino acids are called oligopeptides, and include dipeptides, tripeptides, and tetrapeptides.
...
and cellular material outside and around neurons. Tangles (neurofibrillary tangles) are aggregates of the microtubule-associated protein tau which has become hyperphosphorylated and accumulate inside the cells themselves. Although many older individuals develop some plaques and tangles as a consequence of aging, the brains of people with Alzheimer's disease have a greater number of them in specific brain regions such as the temporal lobe. Lewy bodies are not rare in the brains of people with Alzheimer's disease.
Biochemistry
Alzheimer's disease has been identified as a protein misfolding disease, aproteopathy
In medicine, proteinopathy (; 'pref''. protein -pathy 'suff''. disease proteinopathies ''pl''.; proteinopathic ''adj''), or proteopathy, protein conformational disorder, or protein misfolding disease refers to a class of diseases in which certa ...
, caused by the accumulation of abnormally folded amyloid beta protein into amyloid plaques, and tau protein
The tau proteins (abbreviated from tubulin associated unit) are a group of six highly soluble protein isoforms produced by alternative splicing from the gene ''MAPT'' (microtubule-associated protein tau). They have roles primarily in maintaining ...
into neurofibrillary tangles in the brain. Plaques are made up of small peptide
Peptides (, ) are short chains of amino acids linked by peptide bonds. Long chains of amino acids are called proteins. Chains of fewer than twenty amino acids are called oligopeptides, and include dipeptides, tripeptides, and tetrapeptides.
...
s, 39–43 amino acid
Amino acids are organic compounds that contain both amino and carboxylic acid functional groups. Although hundreds of amino acids exist in nature, by far the most important are the alpha-amino acids, which comprise proteins. Only 22 alpha a ...
s in length, called amyloid beta (Aβ). Amyloid beta is a fragment from the larger amyloid-beta precursor protein (APP) a transmembrane protein
A transmembrane protein (TP) is a type of integral membrane protein that spans the entirety of the cell membrane. Many transmembrane proteins function as gateways to permit the transport of specific substances across the membrane. They frequent ...
that penetrates the neuron's membrane. APP is critical to neuron growth, survival, and post-injury repair. In Alzheimer's disease, gamma secretase
Gamma secretase is a multi-subunit protease complex, itself an integral membrane protein, that cleaves single-pass transmembrane proteins at residues within the transmembrane domain. Proteases of this type are known as intramembrane proteases. Th ...
and beta secretase
Beta-secretase 1, also known as beta-site amyloid precursor protein cleaving enzyme 1, beta-site APP cleaving enzyme 1 (BACE1), membrane-associated aspartic protease 2, memapsin-2, aspartyl protease 2, and ASP2, is an enzyme that in humans is enco ...
act together in a proteolytic
Proteolysis is the breakdown of proteins into smaller polypeptides or amino acids. Uncatalysed, the hydrolysis of peptide bonds is extremely slow, taking hundreds of years. Proteolysis is typically catalysed by cellular enzymes called protease ...
process which causes APP to be divided into smaller fragments. One of these fragments gives rise to fibrils of amyloid beta, which then form clumps that deposit outside neurons in dense formations known as amyloid plaques.
Alzheimer's disease is also considered a tauopathy
Tauopathy belongs to a class of neurodegenerative diseases involving the aggregation of tau protein into neurofibrillary or gliofibrillary tangles in the human brain. Tangles are formed by hyperphosphorylation of the microtubule protein known ...
due to abnormal aggregation of the tau protein
The tau proteins (abbreviated from tubulin associated unit) are a group of six highly soluble protein isoforms produced by alternative splicing from the gene ''MAPT'' (microtubule-associated protein tau). They have roles primarily in maintaining ...
. Every neuron has a cytoskeleton
The cytoskeleton is a complex, dynamic network of interlinking protein filaments present in the cytoplasm of all cells, including those of bacteria and archaea. In eukaryotes, it extends from the cell nucleus to the cell membrane and is com ...
, an internal support structure partly made up of structures called microtubules
Microtubules are polymers of tubulin that form part of the cytoskeleton and provide structure and shape to eukaryotic cells. Microtubules can be as long as 50 micrometres, as wide as 23 to 27 nm and have an inner diameter between 11 a ...
. These microtubules act like tracks, guiding nutrients and molecules from the body of the cell to the ends of the axon
An axon (from Greek ἄξων ''áxōn'', axis), or nerve fiber (or nerve fibre: see spelling differences), is a long, slender projection of a nerve cell, or neuron, in vertebrates, that typically conducts electrical impulses known as action p ...
and back. A protein called ''tau'' stabilises the microtubules when phosphorylated
In chemistry, phosphorylation is the attachment of a phosphate group to a molecule or an ion. This process and its inverse, dephosphorylation, are common in biology and could be driven by natural selection. Text was copied from this source, wh ...
, and is therefore called a microtubule-associated protein In cell biology, microtubule-associated proteins (MAPs) are proteins that interact with the microtubules of the cellular cytoskeleton. MAPs are integral to: the stability of the cell and its internal structures and the transport of components within ...
. In Alzheimer's disease, tau undergoes chemical changes, becoming hyperphosphorylated; it then begins to pair with other threads, creating neurofibrillary tangles and disintegrating the neuron's transport system. Pathogenic tau can also cause neuronal death through transposable element
A transposable element (TE, transposon, or jumping gene) is a nucleic acid sequence in DNA that can change its position within a genome, sometimes creating or reversing mutations and altering the cell's genetic identity and genome size. Transp ...
dysregulation.
Disease mechanism
Exactly how disturbances of production and aggregation of the beta-amyloid peptide give rise to the pathology of Alzheimer's disease is not known. The amyloid hypothesis traditionally points to the accumulation of beta-amyloidpeptide
Peptides (, ) are short chains of amino acids linked by peptide bonds. Long chains of amino acids are called proteins. Chains of fewer than twenty amino acids are called oligopeptides, and include dipeptides, tripeptides, and tetrapeptides.
...
s as the central event triggering neuron degeneration. Accumulation of aggregated amyloid fibrils, which are believed to be the toxic form of the protein responsible for disrupting the cell's calcium
Calcium is a chemical element with the symbol Ca and atomic number 20. As an alkaline earth metal, calcium is a reactive metal that forms a dark oxide-nitride layer when exposed to air. Its physical and chemical properties are most similar t ...
ion
An ion () is an atom or molecule with a net electrical charge.
The charge of an electron is considered to be negative by convention and this charge is equal and opposite to the charge of a proton, which is considered to be positive by conve ...
homeostasis
In biology, homeostasis (British also homoeostasis) (/hɒmɪə(ʊ)ˈsteɪsɪs/) is the state of steady internal, physical, and chemical conditions maintained by living systems. This is the condition of optimal functioning for the organism and ...
, induces programmed cell death
Programmed cell death (PCD; sometimes referred to as cellular suicide) is the death of a cell (biology), cell as a result of events inside of a cell, such as apoptosis or autophagy. PCD is carried out in a biological process, which usually confers ...
( apoptosis). It is also known that Aβ selectively builds up in the mitochondria in the cells of Alzheimer's-affected brains, and it also inhibits certain enzyme
Enzymes () are proteins that act as biological catalysts by accelerating chemical reactions. The molecules upon which enzymes may act are called substrates, and the enzyme converts the substrates into different molecules known as products ...
functions and the utilisation of glucose
Glucose is a simple sugar with the molecular formula . Glucose is overall the most abundant monosaccharide, a subcategory of carbohydrates. Glucose is mainly made by plants and most algae during photosynthesis from water and carbon dioxide, u ...
by neurons.
Various inflammatory processes and cytokine
Cytokines are a broad and loose category of small proteins (~5–25 kDa) important in cell signaling. Cytokines are peptides and cannot cross the lipid bilayer of cells to enter the cytoplasm. Cytokines have been shown to be involved in autocrin ...
s may also have a role in the pathology of Alzheimer's disease. Inflammation
Inflammation (from la, inflammatio) is part of the complex biological response of body tissues to harmful stimuli, such as pathogens, damaged cells, or irritants, and is a protective response involving immune cells, blood vessels, and molec ...
is a general marker of tissue damage in any disease, and may be either secondary to tissue damage in Alzheimer's disease or a marker of an immunological response. There is increasing evidence of a strong interaction between the neurons and the immunological mechanisms in the brain. Obesity and systemic inflammation may interfere with immunological processes which promote disease progression.
Alterations in the distribution of different neurotrophic factor
Neurotrophic factors (NTFs) are a family of biomolecules – nearly all of which are peptides or small proteins – that support the growth, survival, and differentiation of both developing and mature neurons. Most NTFs exert their tro ...
s and in the expression of their receptors such as the brain-derived neurotrophic factor
Brain-derived neurotrophic factor (BDNF), or abrineurin, is a protein found in the and the periphery. that, in humans, is encoded by the ''BDNF'' gene. BDNF is a member of the neurotrophin family of growth factors, which are related to the canon ...
(BDNF) have been described in Alzheimer's disease.
Diagnosis
 Alzheimer's disease can only be definitively diagnosed with autopsy findings; in the absence of autopsy, clinical diagnoses of AD are "possible" or "probable", based on other findings. Up to 23% of those clinically diagnosed with AD may be misdiagnosed and may have pathology suggestive of another condition with symptoms that mimic those of AD.
AD is usually clinically diagnosed based on the person's
Alzheimer's disease can only be definitively diagnosed with autopsy findings; in the absence of autopsy, clinical diagnoses of AD are "possible" or "probable", based on other findings. Up to 23% of those clinically diagnosed with AD may be misdiagnosed and may have pathology suggestive of another condition with symptoms that mimic those of AD.
AD is usually clinically diagnosed based on the person's medical history
The medical history, case history, or anamnesis (from Greek: ἀνά, ''aná'', "open", and μνήσις, ''mnesis'', "memory") of a patient is information gained by a physician by asking specific questions, either to the patient or to other peo ...
, history from relatives, and behavioral observations. The presence of characteristic neurological
Neurology (from el, νεῦρον (neûron), "string, nerve" and the suffix -logia, "study of") is the branch of medicine dealing with the diagnosis and treatment of all categories of conditions and disease involving the brain, the spinal c ...
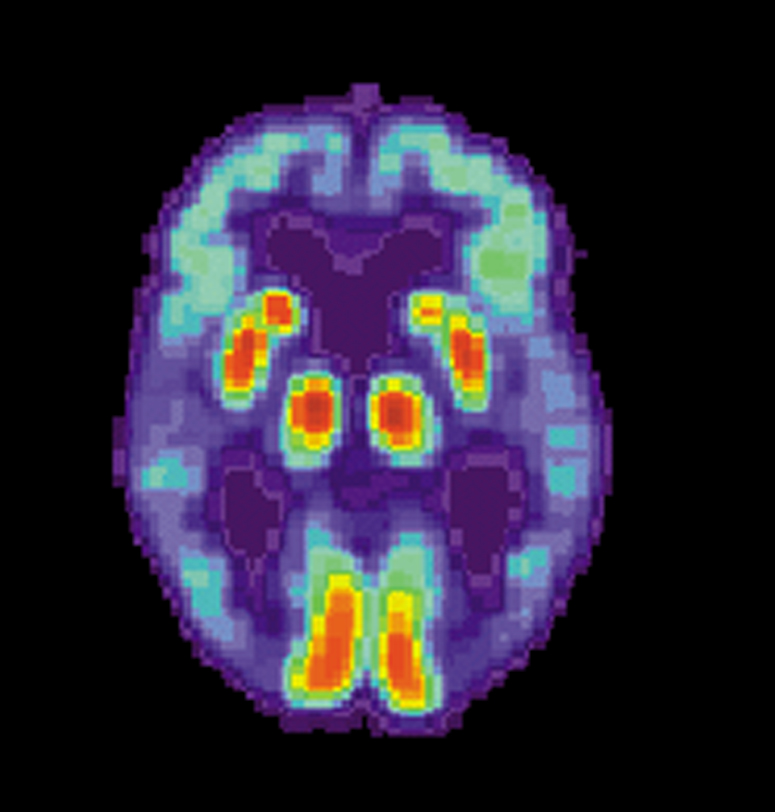
and neuropsychological features and the absence of alternative conditions supports the diagnosis. Advanced medical imaging with computed tomography (CT) or magnetic resonance imaging (MRI), and with single-photon emission computed tomography (SPECT) or positron emission tomography (PET), can be used to help exclude other cerebral pathology or subtypes of dementia. Moreover, it may predict conversion from prodromal
In medicine, a prodrome is an early sign or symptom (or set of signs and symptoms) that often indicates the onset of a disease before more diagnostically specific signs and symptoms develop. It is derived from the Greek word ''prodromos'', meaning ...
stages (mild cognitive impairment) to Alzheimer's disease. FDA-approved radiopharmaceutical
Radiopharmaceuticals, or medicinal radiocompounds, are a group of pharmaceutical drugs containing radioactive isotopes. Radiopharmaceuticals can be used as diagnostic and therapeutic agents. Radiopharmaceuticals emit radiation themselves, which ...
diagnostic agents used in PET for Alzheimer's disease are florbetapir (2012), flutemetamol (2013), florbetaben (2014), and flortaucipir (2020). Because many insurance companies in the United States do not cover this procedure, its use in clinical practice is largely limited to clinical trials .
Assessment of intellectual functioning including memory testing can further characterise the state of the disease. Medical organizations have created diagnostic criteria to ease and standardise the diagnostic process for practising physicians. Definitive diagnosis can only be confirmed with post-mortem
An autopsy (post-mortem examination, obduction, necropsy, or autopsia cadaverum) is a surgical procedure that consists of a thorough examination of a corpse by dissection to determine the cause, mode, and manner of death or to evaluate any di ...
evaluations when brain material is available and can be examined histologically
Histology,
also known as microscopic anatomy or microanatomy, is the branch of biology which studies the microscopic anatomy of biological tissues. Histology is the microscopic counterpart to gross anatomy, which looks at larger structures vis ...
for senile plaques and neurofibrillary tangles.
Criteria
There are three sets of criteria for the clinical diagnoses of the spectrum of Alzheimer's disease: the 2013 fifth edition of the '' Diagnostic and Statistical Manual of Mental Disorders'' (DSM-5
The ''Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition'' (DSM-5), is the 2013 update to the '' Diagnostic and Statistical Manual of Mental Disorders'', the taxonomic and diagnostic tool published by the American Psychiatri ...
); the National Institute on Aging
The National Institute on Aging (NIA) is a division of the U.S. National Institutes of Health (NIH), located in Bethesda, Maryland. The NIA itself is headquartered in Baltimore, Maryland.
The NIA leads a broad scientific effort to understand the ...
-Alzheimer's Association
The Alzheimer's Association was founded by Jerome H. Stone with the help of several family members in Chicago, Illinois, and incorporated on April 10, 1980, as the Alzheimer's Disease and Related Disorders Association, Inc. It is a non-profit Ame ...
(NIA-AA) definition as revised in 2011; and the International Working Group criteria as revised in 2010. Three broad time periods, which can span decades, define the progression of Alzheimer's disease from the preclinical phase, to mild cognitive impairment
Mild cognitive impairment (MCI) is a neurocognitive disorder which involves cognitive impairments beyond those expected based on an individual's age and education but which are not significant enough to interfere with instrumental activities o ...
(MCI), followed by Alzheimer's disease dementia.
Eight intellectual domains are most commonly impaired in AD—memory
Memory is the faculty of the mind by which data or information is encoded, stored, and retrieved when needed. It is the retention of information over time for the purpose of influencing future action. If past events could not be remembered ...
, language
Language is a structured system of communication. The structure of a language is its grammar and the free components are its vocabulary. Languages are the primary means by which humans communicate, and may be conveyed through a variety of ...
, perceptual skills, attention, motor skill
A motor skill is a function that involves specific movements of the body's muscles to perform a certain task. These tasks could include walking, running, or riding a bike. In order to perform this skill, the body's nervous system, muscles, and br ...
s, orientation
Orientation may refer to:
Positioning in physical space
* Map orientation, the relationship between directions on a map and compass directions
* Orientation (housing), the position of a building with respect to the sun, a concept in building de ...
, problem solving and executive function
In cognitive science and neuropsychology, executive functions (collectively referred to as executive function and cognitive control) are a set of cognitive processes that are necessary for the cognitive control of behavior: selecting and succ ...
al abilities, as listed in the fourth text revision of the DSM (DSM-IV-TR).
The DSM-5
The ''Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition'' (DSM-5), is the 2013 update to the '' Diagnostic and Statistical Manual of Mental Disorders'', the taxonomic and diagnostic tool published by the American Psychiatri ...
defines criteria for probable or possible Alzheimer's for both major and mild neurocognitive disorder. Major or mild neurocognitive disorder must be present along with at least one cognitive deficit for a diagnosis of either probable or possible AD. For major neurocognitive disorder due to Alzheimer's disease, probable Alzheimer's disease can be diagnosed if the individual has genetic evidence of Alzheimer's or if two or more acquired cognitive deficits, and a functional disability that is not from another disorder, are present. Otherwise, possible Alzheimer's disease can be diagnosed as the diagnosis follows an atypical route. For mild neurocognitive disorder due to Alzheimer's, probable Alzheimer's disease can be diagnosed if there is genetic evidence, whereas possible Alzheimer's disease can be met if all of the following are present: no genetic evidence, decline in both learning and memory, two or more cognitive deficits, and a functional disability not from another disorder.
The NIA-AA criteria are used mainly in research rather than in clinical assessments. They define Alzheimer's disease through three major stages: preclinical, mild cognitive impairment (MCI), and Alzheimer's dementia. Diagnosis in the preclinical stage is complex and focuses on asymptomatic individuals; the latter two stages describe individuals experiencing symptoms. The core clinical criteria for MCI is used along with identification of biomarkers, predominantly those for neuronal injury (mainly tau-related) and amyloid beta deposition. The core clinical criteria itself rests on the presence of cognitive impairment without the presence of comorbidities. The third stage is divided into probable and possible Alzheimer's disease dementia. In probable Alzheimer's disease dementia there is steady impairment of cognition over time and a memory-related or non-memory-related cognitive dysfunction. In possible Alzheimer's disease dementia, another causal disease such as cerebrovascular disease is present.
Techniques
Neuropsychological test
Neuropsychological tests are specifically designed tasks that are used to measure a psychological function known to be linked to a particular brain structure or pathway. Tests are used for research into brain function and in a clinical setting f ...
s including cognitive test
Cognitive tests are assessments of the cognitive capabilities of humans and other animals. Tests administered to humans include various forms of IQ tests; those administered to animals include the mirror test (a test of visual self-awareness) and t ...
s such as the Mini–Mental State Examination
The Mini–Mental State Examination (MMSE) or Folstein test is a 30-point questionnaire that is used extensively in clinical and research settings to measure cognitive impairment. It is commonly used in medicine and allied health to screen for de ...
(MMSE), the Montreal Cognitive Assessment (MoCA) and the Mini-Cog are widely used to aid in diagnosis of the cognitive impairments in AD. These tests may not always be accurate, as they lack sensitivity to mild cognitive impairment, and can be biased by language or attention problems; more comprehensive test arrays are necessary for high reliability of results, particularly in the earliest stages of the disease.
Further neurological examinations are crucial in the differential diagnosis of Alzheimer's disease and other diseases. Interviews with family members are used in assessment; caregivers can supply important information on daily living abilities and on the decrease in the person's mental function. A caregiver's viewpoint is particularly important, since a person with Alzheimer's disease is commonly unaware of their deficits. Many times, families have difficulties in the detection of initial dementia symptoms and may not communicate accurate information to a physician.
Supplemental testing can rule out other potentially treatable diagnoses and help avoid misdiagnoses. Common supplemental tests include blood tests, thyroid function tests, as well as tests to assess vitamin B12
Vitamin B12, also known as cobalamin, is a water-soluble vitamin involved in metabolism. It is one of eight B vitamins. It is required by animals, which use it as a cofactor in DNA synthesis, in both fatty acid and amino acid metabolism. It ...
levels, rule out neurosyphilis and rule out metabolic problems (including tests for kidney function, electrolyte levels and for diabetes). MRI or CT scans might also be used to rule out other potential causes of the symptoms – including tumors or strokes. Delirium and depression can be common among individuals and are important to rule out.
Psychological tests
Psychological testing is the administration of psychological tests. Psychological tests are administered by trained evaluators. A person's responses are evaluated according to carefully prescribed guidelines. Scores are thought to reflect individ ...
for depression are used, since depression can either be concurrent with Alzheimer's disease (see Depression of Alzheimer disease), an early sign of cognitive impairment, or even the cause.
Due to low accuracy, the C-PIB-PET scan is not recommended as an early diagnostic tool or for predicting the development of Alzheimer's disease when people show signs of mild cognitive impairment (MCI). The use of 18F-FDG PET scans, as a single test, to identify people who may develop Alzheimer's disease is not supported by evidence.
Prevention
 There are no disease-modifying treatments available to cure Alzheimer's disease and because of this, AD research has focused on interventions to prevent the onset and progression. There is no evidence that supports any particular measure in preventing Alzheimer's, and studies of measures to prevent the onset or progression have produced inconsistent results. Epidemiological studies have proposed relationships between an individual's likelihood of developing AD and modifiable factors, such as medications, lifestyle, and diet. There are some challenges in determining whether interventions for Alzheimer's disease act as a primary prevention method, preventing the disease itself, or a secondary prevention method, identifying the early stages of the disease. These challenges include duration of intervention, different stages of disease at which intervention begins, and lack of standardization of inclusion criteria regarding biomarkers specific for Alzheimer's disease. Further research is needed to determine factors that can help prevent Alzheimer's disease.
There are no disease-modifying treatments available to cure Alzheimer's disease and because of this, AD research has focused on interventions to prevent the onset and progression. There is no evidence that supports any particular measure in preventing Alzheimer's, and studies of measures to prevent the onset or progression have produced inconsistent results. Epidemiological studies have proposed relationships between an individual's likelihood of developing AD and modifiable factors, such as medications, lifestyle, and diet. There are some challenges in determining whether interventions for Alzheimer's disease act as a primary prevention method, preventing the disease itself, or a secondary prevention method, identifying the early stages of the disease. These challenges include duration of intervention, different stages of disease at which intervention begins, and lack of standardization of inclusion criteria regarding biomarkers specific for Alzheimer's disease. Further research is needed to determine factors that can help prevent Alzheimer's disease.
Medication
Cardiovascular risk factors, such ashypercholesterolaemia
Hypercholesterolemia, also called high cholesterol, is the presence of high levels of cholesterol in the blood. It is a form of hyperlipidemia (high levels of lipids in the blood), hyperlipoproteinemia (high levels of lipoproteins in the blood), ...
, hypertension, diabetes
Diabetes, also known as diabetes mellitus, is a group of metabolic disorders characterized by a high blood sugar level ( hyperglycemia) over a prolonged period of time. Symptoms often include frequent urination, increased thirst and increased ...
, and smoking, are associated with a higher risk of onset and worsened course of AD. The use of statin
Statins, also known as HMG-CoA reductase inhibitors, are a class of lipid-lowering medications that reduce illness and mortality in those who are at high risk of cardiovascular disease. They are the most common cholesterol-lowering drugs.
Low ...
s to lower cholesterol
Cholesterol is any of a class of certain organic molecules called lipids. It is a sterol (or modified steroid), a type of lipid. Cholesterol is biosynthesized by all animal cells and is an essential structural component of animal cell mem ...
may be of benefit in Alzheimer's. Antihypertensive and antidiabetic medications in individuals without overt cognitive impairment may decrease the risk of dementia by influencing cerebrovascular pathology. More research is needed to examine the relationship with Alzheimer's disease specifically; clarification of the direct role medications play versus other concurrent lifestyle changes (diet, exercise, smoking) is needed.
Depression is associated with an increased risk for Alzheimer's disease; management with antidepressants may provide a preventative measure.
Historically, long-term usage of non-steroidal anti-inflammatory drugs
Non-steroidal anti-inflammatory drugs (NSAID) are members of a therapeutic drug class which reduces pain, decreases inflammation, decreases fever, and prevents blood clots. Side effects depend on the specific drug, its dose and duration of ...
(NSAIDs) were thought to be associated with a reduced likelihood of developing Alzheimer's disease as it reduces inflammation; however, NSAIDs do not appear to be useful as a treatment. Additionally, because women have a higher incidence of Alzheimer's disease than men, it was once thought that estrogen deficiency during menopause was a risk factor. However, there is a lack of evidence to show that hormone replacement therapy (HRT) in menopause decreases risk of cognitive decline.
Lifestyle
Certain lifestyle activities, such as physical and cognitive exercises, higher education and occupational attainment, cigarette smoking, stress, sleep, and the management of other comorbidities, including diabetes and hypertension, may affect the risk of developing Alzheimer's. Physical exercise is associated with a decreased rate of dementia, and is effective in reducing symptom severity in those with AD. Memory and cognitive functions can be improved with aerobic exercises including brisk walking three times weekly for forty minutes. It may also induce neuroplasticity of the brain. Participating in mental exercises, such as reading, crossword puzzles, and chess have shown a potential to be preventative. Meeting the WHO recommendations for physical activity is associated with a lower risk of AD. Higher education and occupational attainment, and participation in leisure activities, contribute to a reduced risk of developing Alzheimer's, or of delaying the onset of symptoms. This is compatible with thecognitive reserve
Cognitive reserve is the mind's and brain's resistance to damage of the brain. The mind's resilience is evaluated behaviorally, whereas the neuropathological damage is evaluated histologically, although damage may be estimated using blood-based ma ...
theory, which states that some life experiences result in more efficient neural functioning providing the individual a cognitive reserve that delays the onset of dementia manifestations. Education
Education is a purposeful activity directed at achieving certain aims, such as transmitting knowledge or fostering skills and character traits. These aims may include the development of understanding, rationality, kindness, and honesty ...
delays the onset of Alzheimer's disease syndrome without changing the duration of the disease.
Cessation in smoking may reduce risk of developing Alzheimer's' disease, specifically in those who carry APOE ɛ4 allele. The increased oxidative stress caused by smoking results in downstream inflammatory or neurodegenerative processes that may increase risk of developing AD. Avoidance of smoking, counseling and pharmacotherapies to quit smoking are used, and avoidance of environmental tobacco smoke is recommended.
Alzheimer's disease is associated with sleep disorders but the precise relationship is unclear. It was once thought that as people get older, the risk of developing sleep disorders and AD independently increase, but research is examining whether sleep disorders may increase the prevalence of AD. One theory is that the mechanisms to increase clearance of toxic substances, including Aβ
Amyloid beta (Aβ or Abeta) denotes peptides of 36–43 amino acids that are the main component of the amyloid plaques found in the brains of people with Alzheimer's disease. The peptides derive from the amyloid precursor protein (APP), which ...
, are active during sleep. With decreased sleep, a person is increasing Aβ production and decreasing Aβ clearance, resulting in Aβ accumulation. Receiving adequate sleep (approximately 7–8 hours) every night has become a potential lifestyle intervention to prevent the development of AD.
Stress is a risk factor for the development of Alzheimer's. The mechanism by which stress predisposes someone to development of Alzheimer's is unclear, but it is suggested that lifetime stressors may affect a person's epigenome, leading to an overexpression or under expression of specific genes. Although the relationship of stress and Alzheimer's is unclear, strategies to reduce stress and relax the mind may be helpful strategies in preventing the progression or Alzheimer's disease. Meditation, for instance, is a helpful lifestyle change to support cognition and well-being, though further research is needed to assess long-term effects.
Management
There is no cure for Alzheimer's disease; available treatments offer relatively small symptomatic benefits but remain palliative in nature. Treatments can be divided into pharmaceutical, psychosocial, and caregiving.Pharmaceutical

acetylcholinesterase inhibitor
Acetylcholinesterase inhibitors (AChEIs) also often called cholinesterase inhibitors, inhibit the enzyme acetylcholinesterase from breaking down the neurotransmitter acetylcholine into choline and acetate, thereby increasing both the level and ...
s (tacrine
Tacrine is a centrally acting acetylcholinesterase inhibitor and indirect cholinergic agonist (parasympathomimetic). It was the first centrally acting cholinesterase inhibitor approved for the treatment of Alzheimer's disease, and was marketed un ...
, rivastigmine
Rivastigmine (sold under the trade name Exelon among others) is a cholinesterase inhibitor used for the treatment of mild to moderate Alzheimer's disease. The drug can be administered orally or via a transdermal patch; the latter form reduces t ...
, galantamine
Galantamine is used for the treatment of cognitive decline in mild to moderate Alzheimer's disease and various other memory impairments. It is an alkaloid that has been isolated from the bulbs and flowers of '' Galanthus nivalis'' (Common snowd ...
, and donepezil
Donepezil, sold under the brand name Aricept among others, is a medication used to treat dementia of the Alzheimer's type. It appears to result in a small benefit in mental function and ability to function. Use, however, has not been shown to ...
) and memantine
Memantine is a medication used to slow the progression of moderate-to-severe Alzheimer's disease. It is taken by mouth.
Common side effects include headache, constipation, sleepiness, and dizziness. Severe side effects may include blood clots ...
, an NMDA receptor antagonist
NMDA receptor antagonists are a class of drugs that work to antagonize, or inhibit the action of, the ''N''-Methyl-D-aspartate receptor ( NMDAR). They are commonly used as anesthetics for animals and humans; the state of anesthesia they induce ...
. The acetylcholinesterase inhibitors are intended for those with mild to severe Alzheimer's, whereas memantine is intended for those with moderate or severe Alzheimer's disease. The benefit from their use is small.
Reduction in the activity of the cholinergic
Cholinergic agents are compounds which mimic the action of acetylcholine and/or butyrylcholine. In general, the word " choline" describes the various quaternary ammonium salts containing the ''N'',''N'',''N''-trimethylethanolammonium cati ...
neurons is a well-known feature of Alzheimer's disease. Acetylcholinesterase inhibitors are employed to reduce the rate at which acetylcholine (ACh) is broken down, thereby increasing the concentration of ACh in the brain and combating the loss of ACh caused by the death of cholinergic neurons. There is evidence for the efficacy of these medications in mild to moderate Alzheimer's disease, and some evidence for their use in the advanced stage. The use of these drugs in mild cognitive impairment
Mild cognitive impairment (MCI) is a neurocognitive disorder which involves cognitive impairments beyond those expected based on an individual's age and education but which are not significant enough to interfere with instrumental activities o ...
has not shown any effect in a delay of the onset of Alzheimer's disease. The most common side effects
In medicine, a side effect is an effect, whether therapeutic or adverse, that is secondary to the one intended; although the term is predominantly employed to describe adverse effects, it can also apply to beneficial, but unintended, consequence ...
are nausea
Nausea is a diffuse sensation of unease and discomfort, sometimes perceived as an urge to vomit. While not painful, it can be a debilitating symptom if prolonged and has been described as placing discomfort on the chest, abdomen, or back of the ...
and vomiting
Vomiting (also known as emesis and throwing up) is the involuntary, forceful expulsion of the contents of one's stomach through the mouth and sometimes the nose.
Vomiting can be the result of ailments like food poisoning, gastroenteri ...
, both of which are linked to cholinergic excess. These side effects arise in approximately 10–20% of users, are mild to moderate in severity, and can be managed by slowly adjusting medication doses. Less common secondary effects include muscle cramp
A cramp is a sudden, involuntary, painful skeletal muscle contraction or overshortening associated with electrical activity; while generally temporary and non-damaging, they can cause significant pain and a paralysis-like immobility of the aff ...
s, decreased heart rate
Heart rate (or pulse rate) is the frequency of the heartbeat measured by the number of contractions (beats) of the heart per minute (bpm). The heart rate can vary according to the body's physical needs, including the need to absorb oxygen and excr ...
( bradycardia), decreased appetite and weight, and increased gastric acid production.
Glutamate is an excitatory neurotransmitter of the nervous system
In biology, the nervous system is the highly complex part of an animal that coordinates its actions and sensory information by transmitting signals to and from different parts of its body. The nervous system detects environmental changes ...
, although excessive amounts in the brain
A brain is an organ that serves as the center of the nervous system in all vertebrate and most invertebrate animals. It is located in the head, usually close to the sensory organs for senses such as vision. It is the most complex organ in a ve ...
can lead to cell
Cell most often refers to:
* Cell (biology), the functional basic unit of life
Cell may also refer to:
Locations
* Monastic cell, a small room, hut, or cave in which a religious recluse lives, alternatively the small precursor of a monastery ...
death through a process called excitotoxicity
In excitotoxicity, nerve cells suffer damage or death when the levels of otherwise necessary and safe neurotransmitters such as glutamate become pathologically high, resulting in excessive stimulation of receptors. For example, when glutamate ...
which consists of the overstimulation of glutamate receptors
Receptor may refer to:
*Sensory receptor, in physiology, any structure which, on receiving environmental stimuli, produces an informative nerve impulse
*Receptor (biochemistry), in biochemistry, a protein molecule that receives and responds to a n ...
. Excitotoxicity occurs not only in Alzheimer's disease, but also in other neurological diseases such as Parkinson's disease
Parkinson's disease (PD), or simply Parkinson's, is a long-term degenerative disorder of the central nervous system that mainly affects the motor system. The symptoms usually emerge slowly, and as the disease worsens, non-motor symptoms becom ...
and multiple sclerosis. Memantine
Memantine is a medication used to slow the progression of moderate-to-severe Alzheimer's disease. It is taken by mouth.
Common side effects include headache, constipation, sleepiness, and dizziness. Severe side effects may include blood clots ...
is a noncompetitive NMDA receptor antagonist
NMDA receptor antagonists are a class of drugs that work to antagonize, or inhibit the action of, the ''N''-Methyl-D-aspartate receptor ( NMDAR). They are commonly used as anesthetics for animals and humans; the state of anesthesia they induce ...
first used as an anti- influenza agent. It acts on the glutamatergic system by blocking NMDA receptors and inhibiting their overstimulation by glutamate. Memantine has been shown to have a small benefit in the treatment of moderate to severe Alzheimer's disease. Reported adverse events with memantine are infrequent and mild, including hallucination
A hallucination is a perception in the absence of an external stimulus that has the qualities of a real perception. Hallucinations are vivid, substantial, and are perceived to be located in external objective space. Hallucination is a combinati ...
s, confusion
In medicine, confusion is the quality or state of being bewildered or unclear. The term "acute mental confusion"
, dizziness
Dizziness is an imprecise term that can refer to a sense of disorientation in space, vertigo, or lightheadedness. It can also refer to disequilibrium or a non-specific feeling, such as giddiness or foolishness.
Dizziness is a common medical c ...
, headache and fatigue. The combination of memantine and donepezil has been shown to be "of statistically significant but clinically marginal effectiveness".
An extract of ''Ginkgo biloba
''Ginkgo biloba'', commonly known as ginkgo or gingko ( ), also known as the maidenhair tree, is a species of tree native to China. It is the last living species in the order Ginkgoales, which first appeared over 290 million years ago. Fossil ...
'' known as ''EGb 761'' has been used for treating Alzheimer's and other neuropsychiatric disorders. Its use is approved throughout Europe. The World Federation of Biological Psychiatry guidelines lists EGb 761 with the same weight of evidence (level B) given to acetylcholinesterase inhibitors and memantine. EGb 761 is the only one that showed improvement of symptoms in both Alzheimer's disease and vascular dementia. EGb 761 may have a role either on its own or as an add-on if other therapies prove ineffective. A 2016 review concluded that the quality of evidence from clinical trials on ''Ginkgo biloba'' has been insufficient to warrant its use for treating Alzheimer's disease.
Atypical antipsychotic
The atypical antipsychotics (AAP), also known as second generation antipsychotics (SGAs) and serotonin–dopamine antagonists (SDAs), are a group of antipsychotic drugs (antipsychotic drugs in general are also known as major tranquilizers and ne ...
s are modestly useful in reducing aggression and psychosis
Psychosis is a condition of the mind that results in difficulties determining what is real and what is not real. Symptoms may include delusions and hallucinations, among other features. Additional symptoms are incoherent speech and behavior ...
in people with Alzheimer's disease, but their advantages are offset by serious adverse effects, such as stroke, movement difficulties or cognitive decline. When used in the long-term, they have been shown to associate with increased mortality. Selay summary
January 2009. Stopping antipsychotic use in this group of people appears to be safe.
Psychosocial
Psychosocial
The psychosocial approach looks at individuals in the context of the combined influence that psychological factors and the surrounding social environment have on their physical and mental wellness and their ability to function. This approach is ...
interventions are used as an adjunct to pharmaceutical treatment and can be classified within behavior-, emotion-, cognition- or stimulation-oriented approaches.
Behavioral interventions attempt to identify and reduce the antecedents and consequences of problem behaviors. This approach has not shown success in improving overall functioning, but can help to reduce some specific problem behaviors, such as incontinence. There is a lack of high quality data on the effectiveness of these techniques in other behavior problems such as wandering. Music therapy is effective in reducing behavioral and psychological symptoms.
Emotion-oriented interventions include reminiscence therapy
Reminiscence therapy is used to counsel and support older people, and is an intervention technique with brain-injured patients and those who appear to have "Alzheimer's and other forms of cognitive disease."
A 2018 AARP article about a standalone ...
, validation therapy
Validation therapy was developed by Naomi Feil for older people with cognitive impairments and dementia. Feil's own approach classifies individuals with cognitive impairment as having one of four stages in a continuum of dementia. These stages are ...
, supportive psychotherapy, sensory integration, also called snoezelen, and simulated presence therapy. A Cochrane review has found no evidence that this is effective. Reminiscence therapy (RT) involves the discussion of past experiences individually or in group, many times with the aid of photographs, household items, music and sound recordings, or other familiar items from the past. A 2018 review of the effectiveness of RT found that effects were inconsistent, small in size and of doubtful clinical significance, and varied by setting. Simulated presence therapy (SPT) is based on attachment theories and involves playing a recording with voices of the closest relatives of the person with Alzheimer's disease. There is partial evidence indicating that SPT may reduce challenging behaviors.
The aim of cognition-oriented treatments, which include reality orientation and cognitive retraining, is the reduction of cognitive deficit
Cognitive deficit is an inclusive term to describe any characteristic that acts as a barrier to the cognition process.
The term may describe
* deficits in overall intelligence (as with intellectual disabilities),
* specific and restricted defic ...
s. Reality orientation consists of the presentation of information about time, place, or person to ease the understanding of the person about its surroundings and his or her place in them. On the other hand, cognitive retraining tries to improve impaired capacities by exercising mental abilities. Both have shown some efficacy improving cognitive capacities.
Stimulation-oriented treatments include art
Art is a diverse range of human activity, and resulting product, that involves creative or imaginative talent expressive of technical proficiency, beauty, emotional power, or conceptual ideas.
There is no generally agreed definition of wha ...
, music
Music is generally defined as the art of arranging sound to create some combination of form, harmony, melody, rhythm or otherwise expressive content. Exact definitions of music vary considerably around the world, though it is an aspe ...
and pet
A pet, or companion animal, is an animal kept primarily for a person's company or entertainment rather than as a working animal, livestock, or a laboratory animal. Popular pets are often considered to have attractive appearances, intelligence ...
therapies, exercise, and any other kind of recreational activities. Stimulation has modest support for improving behavior, mood, and, to a lesser extent, function. Nevertheless, as important as these effects are, the main support for the use of stimulation therapies is the change in the person's routine.
Caregiving
Since Alzheimer's has no cure and it gradually renders people incapable of tending to their own needs, caregiving is essentially the treatment and must be carefully managed over the course of the disease. During the early and moderate stages, modifications to the living environment and lifestyle can increasesafety
Safety is the state of being "safe", the condition of being protected from harm or other danger. Safety can also refer to the control of recognized hazards in order to achieve an acceptable level of risk.
Meanings
There are two slightly dif ...
and reduce caretaker burden. Examples of such modifications are the adherence to simplified routines, the placing of safety locks, the labeling of household items to cue the person with the disease or the use of modified daily life objects. If eating becomes problematic, food will need to be prepared in smaller pieces or even purée
A purée (or mash) is cooked food, usually vegetables, fruits or legumes, that has been ground, pressed, blended or sieved to the consistency of a creamy paste or liquid. Purées of specific foods are often known by specific names, e.g., apple ...
d. When swallowing difficulties arise, the use of feeding tube
Eating (also known as consuming) is the ingestion of food, typically to provide a heterotrophic organism with energy and to allow for growth. Animals and other heterotrophs must eat in order to survive — carnivores eat other animals, herbi ...
s may be required. In such cases, the medical efficacy and ethics of continuing feeding is an important consideration of the caregivers and family members. The use of physical restraints is rarely indicated in any stage of the disease, although there are situations when they are necessary to prevent harm to the person with Alzheimer's disease or their caregivers.
During the final stages of the disease, treatment is centred on relieving discomfort until death, often with the help of hospice.
Diet
Diet may be a modifiable risk factor for the development of Alzheimer's disease. TheMediterranean diet
The Mediterranean diet is a diet inspired by the eating habits of people who live near the Mediterranean Sea. When initially formulated in the 1960s, it drew on the cuisines of Greece, Italy, France and Spain. In decades since, it has also incor ...
, and the DASH diet
The DASH diet (Dietary Approaches to Stop Hypertension) is a dietary pattern promoted by the U.S.-based National Heart, Lung, and Blood Institute (part of the National Institutes of Health (NIH), an agency of the United States Department of Heal ...
are both associated with less cognitive decline. A different approach has been to incorporate elements of both of these diets into one known as the MIND diet The Mediterranean-DASH Intervention for Neurodegenerative Delay diet, or more commonly, the MIND diet, combines the portions of the DASH (Dietary Approaches to Stop Hypertension) diet and the Mediterranean diet. Both the DASH diet and the Mediterra ...
. Studies of individual dietary components, minerals and supplements are conflicting as to whether they prevent AD or cognitive decline.
Prognosis
The early stages of Alzheimer's disease are difficult to diagnose. A definitive diagnosis is usually made once cognitive impairment compromises daily living activities, although the person may still be living independently. The symptoms will progress from mild cognitive problems, such as memory loss through increasing stages of cognitive and non-cognitive disturbances, eliminating any possibility of independent living, especially in the late stages of the disease.Life expectancy
Life expectancy is a statistical measure of the average time an organism is expected to live, based on the year of its birth, current age, and other demographic factors like sex. The most commonly used measure is life expectancy at birth ...
of people with Alzheimer's disease is reduced. The normal life expectancy for 60 to 70 years old is 23 to 15 years; for 90 years old it is 4.5 years. Following Alzheimer's disease diagnosis it ranges from 7 to 10 years for those in their 60s and early 70s (a loss of 13 to 8 years), to only about 3 years or less (a loss of 1.5 years) for those in their 90s.
Fewer than 3% of people live more than fourteen years. Disease features significantly associated with reduced survival are an increased severity of cognitive impairment, decreased functional level, history of falls, and disturbances in the neurological examination. Other coincident diseases such as heart problems, diabetes
Diabetes, also known as diabetes mellitus, is a group of metabolic disorders characterized by a high blood sugar level ( hyperglycemia) over a prolonged period of time. Symptoms often include frequent urination, increased thirst and increased ...
, or history of alcohol abuse are also related with shortened survival. While the earlier the age at onset the higher the total survival years, life expectancy is particularly reduced when compared to the healthy population among those who are younger. Men have a less favourable survival prognosis than women.
Pneumonia
Pneumonia is an inflammatory condition of the lung primarily affecting the small air sacs known as alveoli. Symptoms typically include some combination of productive or dry cough, chest pain, fever, and difficulty breathing. The severi ...
and dehydration
In physiology, dehydration is a lack of total body water, with an accompanying disruption of metabolic processes. It occurs when free water loss exceeds free water intake, usually due to exercise, disease, or high environmental temperature. Mil ...
are the most frequent immediate causes of death brought by Alzheimer's disease, while cancer
Cancer is a group of diseases involving abnormal cell growth with the potential to invade or spread to other parts of the body. These contrast with benign tumors, which do not spread. Possible signs and symptoms include a lump, abnormal b ...
is a less frequent cause of death than in the general population.
Epidemiology
Two main measures are used inepidemiological
Epidemiology is the study and analysis of the distribution (who, when, and where), patterns and determinants of health and disease conditions in a defined population.
It is a cornerstone of public health, and shapes policy decisions and evidenc ...
studies: incidence and prevalence. Incidence is the number of new cases per unit of person-time at risk (usually number of new cases per thousand person-years); while prevalence
In epidemiology, prevalence is the proportion of a particular population found to be affected by a medical condition (typically a disease or a risk factor such as smoking or seatbelt use) at a specific time. It is derived by comparing the number o ...
is the total number of cases of the disease in the population at any given time.
Regarding incidence, cohort
Cohort or cohortes may refer to:
* Cohort (educational group), a group of students working together through the same academic curriculum
* Cohort (floating point), a set of different encodings of the same numerical value
* Cohort (military unit ...
longitudinal studies
A longitudinal study (or longitudinal survey, or panel study) is a research design that involves repeated observations of the same variables (e.g., people) over short or long periods of time (i.e., uses longitudinal data). It is often a type of obs ...
(studies where a disease-free population is followed over the years) provide rates between 10 and 15 per thousand person-years for all dementias and 5–8 for Alzheimer's disease, which means that half of new dementia cases each year are Alzheimer's disease. Advancing age is a primary risk factor for the disease and incidence rates are not equal for all ages: every 5 years after the age of 65, the risk of acquiring the disease approximately doubles, increasing from 3 to as much as 69 per thousand person years. Females with Alzheimer's disease are more common than males, but this difference is likely due to women's' longer life spans. When adjusted for age, both sexes are affected by Alzheimer's at equal rates. In the United States, the risk of dying from Alzheimer's disease in 2010 was 26% higher among the non-Hispanic white population than among the non-Hispanic black population, and the Hispanic population had a 30% lower risk than the non-Hispanic white population. However, much Alzheimer's research remains to be done in minority groups, such as the African American
African Americans (also referred to as Black Americans and Afro-Americans) are an ethnic group consisting of Americans with partial or total ancestry from sub-Saharan Africa. The term "African American" generally denotes descendants of ens ...
and the Hispanic/Latino populations. Studies have shown that these groups are underrepresented in clinical trials and do not have the same risk of developing Alzheimer's when carrying certain genetic risk factors (i.e. APOE4), compared to their caucasian counterparts.
The prevalence of Alzheimer's disease in populations is dependent upon factors including incidence and survival. Since the incidence of Alzheimer's disease increases with age, prevalence depends on the mean age of the population for which prevalence is given. In the United States in 2020, Alzheimer's dementia prevalence was estimated to be 5.3% for those in the 60–74 age group, with the rate increasing to 13.8% in the 74–84 group and to 34.6% in those greater than 85. Prevalence rates in some less developed regions around the globe are lower. As the incidence and prevalence are steadily increasing, the prevalence itself is projected to triple by 2050. As of 2020, 50 million people globally have AD, with this number expected to increase to 152 million by 2050.
History
 The ancient Greek and Roman philosophers and
The ancient Greek and Roman philosophers and physician
A physician (American English), medical practitioner (Commonwealth English), medical doctor, or simply doctor, is a health professional who practices medicine, which is concerned with promoting, maintaining or restoring health through th ...
s associated old age with increasing dementia
Dementia is a disorder which manifests as a set of related symptoms, which usually surfaces when the brain is damaged by injury or disease. The symptoms involve progressive impairments in memory, thinking, and behavior, which negatively affe ...
. It was not until 1901 that German psychiatrist Alois Alzheimer
Alois Alzheimer ( , , ; 14 June 1864 – 19 December 1915) was a German psychiatrist and neuropathologist and a colleague of Emil Kraepelin. Alzheimer is credited with identifying the first published case of "presenile dementia", which Kraep ...
identified the first case of what became known as Alzheimer's disease, named after him, in a fifty-year-old woman he called Auguste D. He followed her case until she died in 1906 when he first reported publicly on it. During the next five years, eleven similar cases were reported in the medical literature
Medical literature is the scientific literature of medicine: articles in journals and texts in books devoted to the field of medicine. Many references to the medical literature include the health care literature generally, including that of denti ...
, some of them already using the term Alzheimer's disease. The disease was first described as a distinctive disease by Emil Kraepelin
Emil Wilhelm Georg Magnus Kraepelin (; ; 15 February 1856 – 7 October 1926) was a German psychiatrist.
H. J. Eysenck's ''Encyclopedia of Psychology'' identifies him as the founder of modern scientific psychiatry, psychopharmacology and psych ...
after suppressing some of the clinical (delusions and hallucinations) and pathological features (arteriosclerotic changes) contained in the original report of Auguste D. He included ''Alzheimer's disease'', also named ''presenile'' dementia
Dementia is a disorder which manifests as a set of related symptoms, which usually surfaces when the brain is damaged by injury or disease. The symptoms involve progressive impairments in memory, thinking, and behavior, which negatively affe ...
by Kraepelin, as a subtype of ''senile dementia'' in the eighth edition of his ''Textbook of Psychiatry'', published on 1910.
For most of the 20th century, the diagnosis of Alzheimer's disease was reserved for individuals between the ages of 45 and 65 who developed symptoms of dementia. The terminology changed after 1977 when a conference on Alzheimer's disease concluded that the clinical and pathological
Pathology is the study of the causes and effects of disease or injury. The word ''pathology'' also refers to the study of disease in general, incorporating a wide range of biology research fields and medical practices. However, when used in th ...
manifestations of presenile and senile dementia were almost identical, although the authors also added that this did not rule out the possibility that they had different causes. This eventually led to the diagnosis of ''Alzheimer's disease'' independent of age. The term ''senile dementia of the Alzheimer type'' (SDAT) was used for a time to describe the condition in those over 65, with classical Alzheimer's disease being used to describe those who were younger. Eventually, the term Alzheimer's disease was formally adopted in medical nomenclature
Nomenclature (, ) is a system of names or terms, or the rules for forming these terms in a particular field of arts or sciences. The principles of naming vary from the relatively informal conventions of everyday speech to the internationally ag ...
to describe individuals of all ages with a characteristic common symptom pattern, disease course, and neuropathology
Neuropathology is the study of disease of nervous system tissue, usually in the form of either small surgical biopsies or whole-body autopsies. Neuropathologists usually work in a department of anatomic pathology, but work closely with the clini ...
.
The National Institute of Neurological and Communicative Disorders and Stroke (NINCDS) and the Alzheimer's Disease and Related Disorders Association (ADRDA, now known as the Alzheimer's Association
The Alzheimer's Association was founded by Jerome H. Stone with the help of several family members in Chicago, Illinois, and incorporated on April 10, 1980, as the Alzheimer's Disease and Related Disorders Association, Inc. It is a non-profit Ame ...
) established the most commonly used NINCDS-ADRDA Alzheimer's Criteria
The NINCDS-ADRDA Alzheimer's Criteria were proposed in 1984 by the National Institute of Neurological and Communicative Disorders and Stroke and the Alzheimer's Disease and Related Disorders Association (now known as the Alzheimer's Association) an ...
for diagnosis in 1984, extensively updated in 2007. These criteria require that the presence of cognitive impairment
Cognitive deficit is an inclusive term to describe any characteristic that acts as a barrier to the cognition process.
The term may describe
* deficits in overall intelligence (as with intellectual disabilities),
* specific and restricted defici ...
, and a suspected dementia syndrome, be confirmed by neuropsychological testing
Neuropsychological tests are specifically designed tasks that are used to measure a psychological function known to be linked to a particular brain structure or pathway. Tests are used for research into brain function and in a clinical setting f ...
for a clinical diagnosis of possible or probable Alzheimer's disease. A histopathologic confirmation including a microscopic
The microscopic scale () is the scale of objects and events smaller than those that can easily be seen by the naked eye, requiring a lens or microscope to see them clearly. In physics, the microscopic scale is sometimes regarded as the scale be ...
examination of brain tissue
The human brain is the central organ of the human nervous system, and with the spinal cord makes up the central nervous system. The brain consists of the cerebrum, the brainstem and the cerebellum. It controls most of the activities of th ...
is required for a definitive diagnosis. Good statistical reliability and validity have been shown between the diagnostic criteria and definitive histopathological confirmation.
Society and culture
Social costs
Dementia, and specifically Alzheimer's disease, may be among the most costly diseases for societies worldwide. As populations age, these costs will probably increase and become an importantsocial problem
A social issue is a problem that affects many people within a society. It is a group of common problems in present-day society and ones that many people strive to solve. It is often the consequence of factors extending beyond an individual's cont ...
and economic burden. Costs associated with AD include direct and indirect medical costs, which vary between countries depending on social care for a person with AD. Direct costs include doctor visits, hospital care, medical treatments, nursing home care, specialized equipment, and household expenses. Indirect costs include the cost of informal care and the loss in productivity
Productivity is the efficiency of production of goods or services expressed by some measure. Measurements of productivity are often expressed as a ratio of an aggregate output to a single input or an aggregate input used in a production proces ...
of informal caregivers.
In the United States , informal (family) care is estimated to constitute nearly three-fourths of caregiving for people with AD at a cost of US$234 billion per year and approximately 18.5 billion hours of care. The cost to society worldwide to care for individuals with AD is projected to increase nearly ten-fold, and reach about US$9.1 trillion by 2050.
Costs for those with more severe dementia or behavioral disturbances are higher and are related to the additional caregiving time to provide physical care.
Caregiving burden
The role of the maincaregiver
A caregiver or carer is a paid or unpaid member of a person's social network who helps them with activities of daily living. Since they have no specific professional training, they are often described as informal caregivers. Caregivers most commo ...
is often taken by the spouse or a close relative. Alzheimer's disease is known for placing a great burden on caregiver
A caregiver or carer is a paid or unpaid member of a person's social network who helps them with activities of daily living. Since they have no specific professional training, they are often described as informal caregivers. Caregivers most commo ...
s which includes social, psychological, physical, or economic aspects. Home care is usually preferred by people with Alzheimer's disease and their families. This option also delays or eliminates the need for more professional and costly levels of care. Nevertheless, two-thirds of nursing home residents have dementias.
Dementia
Dementia is a disorder which manifests as a set of related symptoms, which usually surfaces when the brain is damaged by injury or disease. The symptoms involve progressive impairments in memory, thinking, and behavior, which negatively affe ...
caregivers are subject to high rates of physical and mental disorders. Factors associated with greater psychosocial problems of the primary caregivers include having an affected person at home, the carer being a spouse, demanding behaviors of the cared person such as depression, behavioral disturbances, hallucinations, sleep problems or walking disruptions and social isolation
Social isolation is a state of complete or near-complete lack of contact between an individual and society. It differs from loneliness, which reflects temporary and involuntary lack of contact with other humans in the world. Social isolation ...
. Regarding economic problems, family caregivers often give up time from work to spend 47 hours per week on average with the person with Alzheimer's disease, while the costs of caring for them are high. Direct and indirect costs of caring for somebody with Alzheimer's average between $18,000 and $77,500 per year in the United States, depending on the study.
Cognitive behavioral therapy and the teaching of coping strategies either individually or in group have demonstrated their efficacy in improving caregivers' psychological health.
Media
Alzheimer's disease has been portrayed in films such as: ''Iris
Iris most often refers to:
*Iris (anatomy), part of the eye
*Iris (mythology), a Greek goddess
* ''Iris'' (plant), a genus of flowering plants
* Iris (color), an ambiguous color term
Iris or IRIS may also refer to:
Arts and media
Fictional ent ...
'' (2001), based on John Bayley's memoir of his wife Iris Murdoch
Dame Jean Iris Murdoch ( ; 15 July 1919 – 8 February 1999) was an Irish and British novelist and philosopher. Murdoch is best known for her novels about good and evil, sexual relationships, morality, and the power of the unconscious. Her ...
; ''The Notebook
''The Notebook'' is a 2004 American romantic drama film directed by Nick Cassavetes, with a screenplay by Jeremy Leven and Jan Sardi, based on the 1996 novel of the same name by Nicholas Sparks. The film stars Ryan Gosling and Rachel McAdams ...
'' (2004), based on Nicholas Sparks
Nicholas Charles Sparks (born December 31, 1965) is an American novelist, screenwriter, and philanthropist. He has published twenty-three novels and two non-fiction books, some of which have been ''New York Times'' bestsellers, with over 115 m ...
' 1996 novel of the same name; '' A Moment to Remember'' (2004); ''Thanmathra
''Thanmathra'' ( ml, തന്മാത്ര, en, Molecule) is a 2005 Indian Malayalam-language drama film written and directed by Blessy, based on Padmarajan's short story "Orma". It portrays the effects of Alzheimer's disease on the life of ...
'' (2005); '' Memories of Tomorrow (Ashita no Kioku)'' (2006), based on Hiroshi Ogiwara's novel of the same name; ''Away from Her
''Away from Her'' is a 2006 Canadian independent drama film written and directed by Sarah Polley and starring Julie Christie and Gordon Pinsent. Olympia Dukakis, Michael Murphy, Wendy Crewson, Alberta Watson, and Kristen Thomson are featured i ...
'' (2006), based on Alice Munro
Alice Ann Munro (; ; born 10 July 1931) is a Canadian short story writer who won the Nobel Prize in Literature in 2013. Munro's work has been described as revolutionizing the architecture of short stories, especially in its tendency to move f ...
's short story
A short story is a piece of prose fiction that typically can be read in one sitting and focuses on a self-contained incident or series of linked incidents, with the intent of evoking a single effect or mood. The short story is one of the oldest ...
'' The Bear Came over the Mountain''; '' Still Alice'' (2014), about a Columbia University
Columbia University (also known as Columbia, and officially as Columbia University in the City of New York) is a private research university in New York City. Established in 1754 as King's College on the grounds of Trinity Church in Manhatt ...
professor who has early onset Alzheimer's disease, based on Lisa Genova
Lisa Genova (born November 22, 1970) is an American neuroscientist and author. She self-published her debut novel '' Still Alice'' (2007), about a Harvard University professor who suffers early onset Alzheimer's disease. The book gained popular ...
's 2007 novel of the same name and featuring Julianne Moore
Julie Anne Smith (born December 3, 1960), known professionally as Julianne Moore, is an American actress. Prolific in film since the early 1990s, she is particularly known for her portrayals of emotionally troubled women in independent films, ...
in the title role. Documentaries on Alzheimer's disease include ''Malcolm and Barbara: A Love Story'' (1999) and ''Malcolm and Barbara: Love's Farewell'' (2007), both featuring Malcolm Pointon.
Alzheimer's disease has also been portrayed in music by English musician the Caretaker
''The Caretaker'' is a play in three acts by Harold Pinter. Although it was the sixth of his major works for stage and television, this psychological study of the confluence of power, allegiance, innocence, and corruption among two brothers a ...
in releases such as ''Persistent Repetition of Phrases
''Persistent Repetition of Phrases'' is the seventh studio album by the Caretaker, an alias of musician Leyland Kirby. Released on 1 April 2008, it was his first record to cover themes of Alzheimer's disease. The album was also the first Careta ...
'' (2008), ''An Empty Bliss Beyond This World
''An Empty Bliss Beyond This World'' is the ninth studio album by the Caretaker, an ambient music project of English musician Leyland Kirby, released on 1 June 2011 through History Always Favours the Winners.
The record is based on a study re ...
'' (2011), and ''Everywhere at the End of Time
''Everywhere at the End of Time'' is the eleventh and final recording by the Caretaker, an alias of English electronic musician Leyland Kirby. Released between 2016 and 2019, its six studio albums use degrading loops of sampled ballroom music ...
'' (20162019). Paintings depicting the disorder include the late works by American artist William Utermohlen, who drew self-portraits from 1995 to 2000 as an experiment of showing his disease through art.
Research directions
Additional research on the lifestyle effect may provide insight into neuroimaging biomarkers and better understanding of the mechanisms causing both Alzheimer's disease and early-onset AD.Treatment and prevention
There is ongoing research examining the role of specific medications in reducing the prevalence (primary prevention) and/or progression (secondary prevention) of Alzheimer's disease. The research trials investigating medications generally impactAβ
Amyloid beta (Aβ or Abeta) denotes peptides of 36–43 amino acids that are the main component of the amyloid plaques found in the brains of people with Alzheimer's disease. The peptides derive from the amyloid precursor protein (APP), which ...
plaques, inflammation, APOE, neurotransmitter receptors, neurogenesis, epigenetic regulators, growth factor
A growth factor is a naturally occurring substance capable of stimulating cell proliferation, wound healing, and occasionally cellular differentiation. Usually it is a secreted protein or a steroid hormone. Growth factors are important for regul ...
s and hormones. These studies have led to a better understanding of the disease, but none identified a prevention strategy. Experimental models are commonly used by researchers in order to understand disease mechanisms as well develop and test novel therapeutics aimed at treating Alzheimer's disease.
Antibodies are being developed that may have the ability to alter the disease course by targeting amyloid beta, such as donanemab and aducanumab. Aducanumab was approved by the FDA in 2021, but its use and effectiveness remain unclear and controversial. Although it received FDA approval, aducanumab failed to show effectiveness in people who already had Alzheimer's symptoms.
References
Further reading
* *External links
* * * {{Authority control Alzheimer's disease Aging-associated diseases Ailments of unknown cause Amyloidosis Aphasias Cognitive disorders Dementia Eponyms Herpes simplex virus–associated diseases Learning disabilities Wikipedia neurology articles ready to translate Unsolved problems in neuroscience Wikipedia medicine articles ready to translate