Chloroquine on:
[Wikipedia]
[Google]
[Amazon]
Chloroquine is a medication primarily used to prevent and treat
 Chloroquine has been used in the treatment and prevention of
Chloroquine has been used in the treatment and prevention of

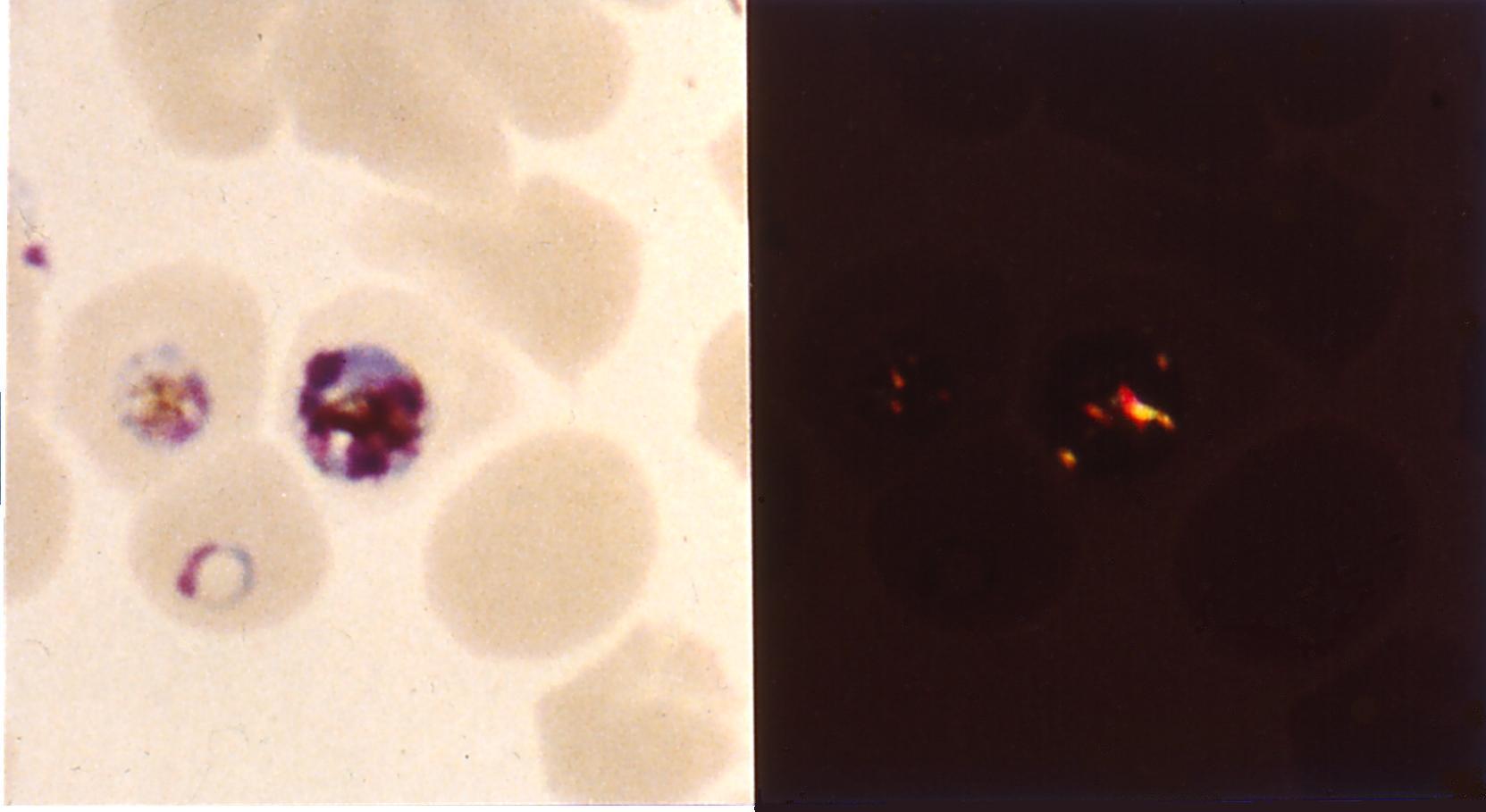 The lysosomotropic character of chloroquine is believed to account for much of its antimalarial activity; the drug concentrates in the acidic food vacuole of the parasite and interferes with essential processes. Its lysosomotropic properties further allow for its use for ''in vitro'' experiments pertaining to intracellular lipid related diseases, autophagy, and apoptosis.
Inside
The lysosomotropic character of chloroquine is believed to account for much of its antimalarial activity; the drug concentrates in the acidic food vacuole of the parasite and interferes with essential processes. Its lysosomotropic properties further allow for its use for ''in vitro'' experiments pertaining to intracellular lipid related diseases, autophagy, and apoptosis.
Inside
 By 1949, chloroquine manufacturing processes had been established to allow its widespread use.
By 1949, chloroquine manufacturing processes had been established to allow its widespread use.

In biomedicinal science, chloroquine is used for ''
malaria
Malaria is a mosquito-borne infectious disease that affects humans and other animals. Malaria causes symptoms that typically include fever, tiredness, vomiting, and headaches. In severe cases, it can cause jaundice, seizures, coma, or death. ...
in areas where malaria remains sensitive to its effects. Certain types of malaria, resistant strains, and complicated cases typically require different or additional medication. Chloroquine is also occasionally used for amebiasis
Amoebiasis, or amoebic dysentery, is an infection of the intestines caused by a parasitic amoeba ''Entamoeba histolytica''. Amoebiasis can be present with no, mild, or severe symptoms. Symptoms may include lethargy, loss of weight, colonic u ...
that is occurring outside the intestines
The gastrointestinal tract (GI tract, digestive tract, alimentary canal) is the tract or passageway of the digestive system that leads from the mouth to the anus. The GI tract contains all the major organs of the digestive system, in humans and ...
, rheumatoid arthritis
Rheumatoid arthritis (RA) is a long-term autoimmune disorder that primarily affects joints. It typically results in warm, swollen, and painful joints. Pain and stiffness often worsen following rest. Most commonly, the wrist and hands are inv ...
, and lupus erythematosus. While it has not been formally studied in pregnancy, it appears safe. It was studied to treat COVID-19
Coronavirus disease 2019 (COVID-19) is a contagious disease caused by a virus, the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). The first known case was identified in Wuhan, China, in December 2019. The disease quick ...
early in the pandemic
A pandemic () is an epidemic of an infectious disease that has spread across a large region, for instance multiple continents or worldwide, affecting a substantial number of individuals. A widespread endemic disease with a stable number of in ...
, but these studies were largely halted in the summer of 2020, and is not recommended for this purpose. It is taken by mouth.
Common side effects include muscle problems, loss of appetite, diarrhea, and skin rash. Serious side effects include problems with vision, muscle damage, seizures
An epileptic seizure, informally known as a seizure, is a period of symptoms due to abnormally excessive or synchronous neuronal activity in the brain. Outward effects vary from uncontrolled shaking movements involving much of the body with lo ...
, and low blood cell levels. Chloroquine is a member of the drug class 4-aminoquinoline. As an antimalarial, it works against the asexual form of the malaria parasite
''Plasmodium'' is a genus of unicellular eukaryotes that are obligate parasites of vertebrates and insects. The life cycles of ''Plasmodium'' species involve development in a blood-feeding insect host which then injects parasites into a verteb ...
in the stage of its life cycle within the red blood cell
Red blood cells (RBCs), also referred to as red cells, red blood corpuscles (in humans or other animals not having nucleus in red blood cells), haematids, erythroid cells or erythrocytes (from Greek ''erythros'' for "red" and ''kytos'' for "hol ...
. How it works in rheumatoid arthritis and lupus erythematosus is unclear.
Chloroquine was discovered in 1934 by Hans Andersag. It is on the World Health Organization's List of Essential Medicines. It is available as a generic medication
A generic drug is a pharmaceutical drug that contains the same chemical substance as a drug that was originally protected by chemical patents. Generic drugs are allowed for sale after the patents on the original drugs expire. Because the active ...
.
Medical uses
Malaria
 Chloroquine has been used in the treatment and prevention of
Chloroquine has been used in the treatment and prevention of malaria
Malaria is a mosquito-borne infectious disease that affects humans and other animals. Malaria causes symptoms that typically include fever, tiredness, vomiting, and headaches. In severe cases, it can cause jaundice, seizures, coma, or death. ...
from '' Plasmodium vivax'', '' P. ovale'', and '' P. malariae''. It is generally not used for ''Plasmodium falciparum
''Plasmodium falciparum'' is a unicellular protozoan parasite of humans, and the deadliest species of ''Plasmodium'' that causes malaria in humans. The parasite is transmitted through the bite of a female '' Anopheles'' mosquito and causes the ...
'' as there is widespread resistance to it.
Chloroquine has been extensively used in mass drug administrations, which may have contributed to the emergence and spread of resistance. It is recommended to check if chloroquine is still effective in the region prior to using it. In areas where resistance is present, other antimalarials
Antimalarial medications or simply antimalarials are a type of antiparasitic chemical agent, often naturally derived, that can be used to treat or to prevent malaria, in the latter case, most often aiming at two susceptible target groups, young ...
, such as mefloquine
Mefloquine, sold under the brand name Lariam among others, is a medication used to prevent or treat malaria. When used for prevention it is typically started before potential exposure and continued for several weeks after potential exposure. It ...
or atovaquone
Atovaquone, sold under the brand name Mepron, is an antimicrobial medication for the prevention and treatment of ''Pneumocystis jirovecii'' pneumonia (PCP).
Atovaquone is a chemical compound that belongs to the class of naphthoquinones. Atova ...
, may be used instead. The Centers for Disease Control and Prevention
The Centers for Disease Control and Prevention (CDC) is the national public health agency of the United States. It is a United States federal agency, under the Department of Health and Human Services, and is headquartered in Atlanta, Georg ...
recommend against treatment of malaria with chloroquine alone due to more effective combinations.
Amebiasis
In treatment ofamoebic liver abscess
A amoebic liver abscess is a type of liver abscess caused by amebiasis. It is the involvement of liver tissue by trophozoites of the organism ''Entamoeba histolytica'' and of its abscess due to necrosis.
Presentation
Approximately 90% of patien ...
, chloroquine may be used instead of or in addition to other medications in the event of failure of improvement with metronidazole
Metronidazole, sold under the brand name Flagyl among others, is an antibiotic and antiprotozoal medication. It is used either alone or with other antibiotics to treat pelvic inflammatory disease, endocarditis, and bacterial vaginosis. It is ...
or another nitroimidazole
5-Nitroimidazole is an organic compound with the formula O2NC3H2N2H. The nitro group at position 5 on the imidazole ring is the most common positional isomer. The term nitroimidazole also refers to a class of antibiotics that share similar ch ...
within 5 days or intolerance to metronidazole or a nitroimidazole.
Rheumatic disease
As it mildly suppresses theimmune system
The immune system is a network of biological processes that protects an organism from diseases. It detects and responds to a wide variety of pathogens, from viruses to parasitic worms, as well as cancer cells and objects such as wood splinte ...
, chloroquine is used in some autoimmune disorder
An autoimmune disease is a condition arising from an abnormal immune response to a functioning body part. At least 80 types of autoimmune diseases have been identified, with some evidence suggesting that there may be more than 100 types. Nearly ...
s, such as rheumatoid arthritis
Rheumatoid arthritis (RA) is a long-term autoimmune disorder that primarily affects joints. It typically results in warm, swollen, and painful joints. Pain and stiffness often worsen following rest. Most commonly, the wrist and hands are inv ...
and has an off label indication for lupus erythematosus.
Side effects
Side effects
In medicine, a side effect is an effect, whether therapeutic or adverse, that is secondary to the one intended; although the term is predominantly employed to describe adverse effects, it can also apply to beneficial, but unintended, consequenc ...
include blurred vision, nausea, vomiting, abdominal cramps, headache, diarrhea, swelling legs/ankles, shortness of breath, pale lips/nails/skin, muscle weakness, easy bruising/bleeding, hearing and mental problems.
* Unwanted/uncontrolled movements (including tongue and face twitching)
* Deafness or tinnitus.
* Nausea, vomiting, diarrhea, abdominal cramps
* Headache.
* Mental/mood changes (such as confusion, personality changes, unusual thoughts/behavior, depression, feeling being watched, hallucinating)
* Signs of serious infection (such as high fever, severe chills, persistent sore throat)
* Skin itchiness, skin color changes, hair loss, and skin rashes.
** Chloroquine-induced itching is very common among black Africans (70%), but much less common in other races. It increases with age, and is so severe as to stop compliance with drug therapy. It is increased during malaria fever; its severity is correlated to the malaria parasite load in blood. Some evidence indicates it has a genetic basis and is related to chloroquine action with opiate receptors centrally or peripherally.
* Unpleasant metallic taste
** This could be avoided by "taste-masked and controlled release" formulations such as multiple emulsions.
* Chloroquine retinopathy
Chloroquine retinopathy is a form of toxic retinopathy (damage of the retina) caused by the drugs chloroquine or hydroxychloroquine, which are sometimes used in the treatment of autoimmune disorders such as rheumatoid arthritis and systemic lupus ...
* Electrocardiographic changes
** This manifests itself as either conduction disturbances (bundle-branch block, atrioventricular block) or Cardiomyopathy
Cardiomyopathy is a group of diseases that affect the heart muscle. Early on there may be few or no symptoms. As the disease worsens, shortness of breath, feeling tired, and swelling of the legs may occur, due to the onset of heart failure. ...
– often with hypertrophy, restrictive physiology, and congestive heart failure
Heart failure (HF), also known as congestive heart failure (CHF), is a syndrome, a group of signs and symptoms caused by an impairment of the heart's blood pumping function. Symptoms typically include shortness of breath, excessive fatigue, ...
. The changes may be irreversible. Only two cases have been reported requiring heart transplantation, suggesting this particular risk is very low. Electron microscopy of cardiac biopsies show pathognomonic cytoplasmic inclusion bodies.
* Pancytopenia
Pancytopenia is a medical condition in which there is significant reduction in the number of almost all blood cells ( red blood cells, white blood cells, platelets, monocytes, lymphocytes, etc.).
If only two parameters from the complete blood ...
, aplastic anemia
Aplastic anemia is a cancer in which the body fails to make blood cells in sufficient numbers. Blood cells are produced in the bone marrow by stem cells that reside there. Aplastic anemia causes a deficiency of all blood cell types: red bloo ...
, reversible agranulocytosis
Agranulocytosis, also known as agranulosis or granulopenia, is an acute condition involving a severe and dangerous lowered white blood cell count (leukopenia, most commonly of neutrophils) and thus causing a neutropenia in the circulating blood. ...
, low blood platelets, neutropenia
Neutropenia is an abnormally low concentration of neutrophils (a type of white blood cell) in the blood. Neutrophils make up the majority of circulating white blood cells and serve as the primary defense against infections by destroying bacteri ...
''.''
Pregnancy
Chloroquine has not been shown to have any harmful effects on the fetus when used in the recommended doses for malarial prophylaxis. Small amounts of chloroquine are excreted in the breast milk of lactating women. However, this drug can be safely prescribed to infants, the effects are not harmful. Studies with mice show that radioactively tagged chloroquine passed through theplacenta
The placenta is a temporary embryonic and later fetal organ that begins developing from the blastocyst shortly after implantation. It plays critical roles in facilitating nutrient, gas and waste exchange between the physically separate mate ...
rapidly and accumulated in the fetal eyes which remained present five months after the drug was cleared from the rest of the body. Women who are pregnant or planning on getting pregnant are still advised against traveling to malaria-risk regions.
Elderly
There is not enough evidence to determine whether chloroquine is safe to be given to people aged 65 and older. Since it is cleared by the kidneys, toxicity should be monitored carefully in people with poor kidney functions.Drug interactions
Chloroquine has a number of drug–drug interactions that might be of clinical concern: *Ampicillin
Ampicillin is an antibiotic used to prevent and treat a number of bacterial infections, such as respiratory tract infections, urinary tract infections, meningitis, salmonellosis, and endocarditis. It may also be used to prevent group B str ...
- levels may be reduced by chloroquine;
* Antacids
An antacid is a substance which neutralizes stomach acidity and is used to relieve heartburn, indigestion or an upset stomach. Some antacids have been used in the treatment of constipation and diarrhea. Marketed antacids contain salts of alu ...
- may reduce absorption of chloroquine;
* Cimetidine
Cimetidine, sold under the brand name Tagamet among others, is a histamine H2 receptor antagonist that inhibits stomach acid production. It is mainly used in the treatment of heartburn and peptic ulcers.
The development of longer-acting H2 r ...
- may inhibit metabolism of chloroquine; increasing levels of chloroquine in the body;
* Cyclosporine- levels may be increased by chloroquine; and
* Mefloquine
Mefloquine, sold under the brand name Lariam among others, is a medication used to prevent or treat malaria. When used for prevention it is typically started before potential exposure and continued for several weeks after potential exposure. It ...
- may increase risk of convulsions.
Overdose
Chloroquine, in overdose, has a risk of death of about 20%. It is rapidly absorbed from the gut with an onset of symptoms generally within an hour. Symptoms of overdose may include sleepiness, vision changes,seizures
An epileptic seizure, informally known as a seizure, is a period of symptoms due to abnormally excessive or synchronous neuronal activity in the brain. Outward effects vary from uncontrolled shaking movements involving much of the body with lo ...
, stopping of breathing, and heart problems such as ventricular fibrillation
Ventricular fibrillation (V-fib or VF) is an abnormal heart rhythm in which the ventricles of the heart quiver. It is due to disorganized electrical activity. Ventricular fibrillation results in cardiac arrest with loss of consciousness and n ...
and low blood pressure. Low blood potassium may also occur.
While the usual dose of chloroquine used in treatment is 10 mg/kg, toxicity begins to occur at 20 mg/kg, and death may occur at 30 mg/kg. In children as little as a single tablet can cause problems.
Treatment recommendations include early mechanical ventilation
Mechanical ventilation, assisted ventilation or intermittent mandatory ventilation (IMV), is the medical term for using a machine called a ventilator to fully or partially provide artificial ventilation. Mechanical ventilation helps move a ...
, cardiac monitoring, and activated charcoal
"Activated" is a song by English singer Cher Lloyd. It was released on 22 July 2016 through Vixen Records. The song was made available to stream exclusively on ''Rolling Stone'' a day before to release (on 21 July 2016).
Background
In an inter ...
. Intravenous fluids
Intravenous therapy (abbreviated as IV therapy) is a medical technique that administers fluids, medications and nutrients directly into a person's vein. The intravenous route of administration is commonly used for rehydration or to provide nutri ...
and vasopressor
An antihypotensive agent, also known as a vasopressor agent or simply vasopressor, or pressor, is any substance, whether endogenous or a medication, that tends to raise low blood pressure. Some antihypotensive drugs act as vasoconstrictors to i ...
s may be required with epinephrine
Adrenaline, also known as epinephrine, is a hormone and medication which is involved in regulating visceral functions (e.g., respiration). It appears as a white microcrystalline granule. Adrenaline is normally produced by the adrenal glands and ...
being the vasopressor of choice. Seizures may be treated with benzodiazepines
Benzodiazepines (BZD, BDZ, BZs), sometimes called "benzos", are a class of depressant drugs whose core chemical structure is the fusion of a benzene ring and a diazepine ring. They are prescribed to treat conditions such as anxiety disorders, ...
. Intravenous potassium chloride
Potassium chloride (KCl, or potassium salt) is a metal halide salt composed of potassium and chlorine. It is odorless and has a white or colorless vitreous crystal appearance. The solid dissolves readily in water, and its solutions have a salt ...
may be required, however this may result in high blood potassium later in the course of the disease. Dialysis has not been found to be useful.
Pharmacology
Absorption of chloroquine is rapid and primarily happens in the gastrointestinal tract. It is widely distributed in body tissues. Protein binding in plasma ranges from 46% to 79%. Its metabolism is partially hepatic, giving rise to its main metabolite, desethylchloroquine. Its excretion is ≥50% as unchanged drug in urine, where acidification of urine increases its elimination. It has a very high volume of distribution, as it diffuses into the body'sadipose tissue
Adipose tissue, body fat, or simply fat is a loose connective tissue composed mostly of adipocytes. In addition to adipocytes, adipose tissue contains the stromal vascular fraction (SVF) of cells including preadipocytes, fibroblasts, vascular ...
.
Accumulation of the drug may result in deposits that can lead to blurred vision and blindness
Visual impairment, also known as vision impairment, is a medical definition primarily measured based on an individual's better eye visual acuity; in the absence of treatment such as correctable eyewear, assistive devices, and medical treatment� ...
. It and related quinine
Quinine is a medication used to treat malaria and babesiosis. This includes the treatment of malaria due to '' Plasmodium falciparum'' that is resistant to chloroquine when artesunate is not available. While sometimes used for nocturnal leg ...
s have been associated with cases of retina
The retina (from la, rete "net") is the innermost, light-sensitive layer of tissue of the eye of most vertebrates and some molluscs. The optics of the eye create a focused two-dimensional image of the visual world on the retina, which the ...
l toxicity, particularly when provided at higher doses for longer times. With long-term doses, routine visits to an ophthalmologist
Ophthalmology ( ) is a surgical subspecialty within medicine that deals with the diagnosis and treatment of eye disorders.
An ophthalmologist is a physician who undergoes subspecialty training in medical and surgical eye care. Following a med ...
are recommended.
Chloroquine is also a lysosomotropic agent, meaning it accumulates preferentially in the lysosomes of cells in the body. The pKa for the quinoline nitrogen of chloroquine is 8.5, meaning it is about 10% deprotonated at physiological pH (per the Henderson-Hasselbalch equation). This decreases to about 0.2% at a lysosomal pH of 4.6. Because the deprotonated form is more membrane-permeable than the protonated form, a quantitative "trapping" of the compound in lysosomes results.
Mechanism of action

Malaria
 The lysosomotropic character of chloroquine is believed to account for much of its antimalarial activity; the drug concentrates in the acidic food vacuole of the parasite and interferes with essential processes. Its lysosomotropic properties further allow for its use for ''in vitro'' experiments pertaining to intracellular lipid related diseases, autophagy, and apoptosis.
Inside
The lysosomotropic character of chloroquine is believed to account for much of its antimalarial activity; the drug concentrates in the acidic food vacuole of the parasite and interferes with essential processes. Its lysosomotropic properties further allow for its use for ''in vitro'' experiments pertaining to intracellular lipid related diseases, autophagy, and apoptosis.
Inside red blood cell
Red blood cells (RBCs), also referred to as red cells, red blood corpuscles (in humans or other animals not having nucleus in red blood cells), haematids, erythroid cells or erythrocytes (from Greek ''erythros'' for "red" and ''kytos'' for "hol ...
s, the malarial parasite
Parasitism is a close relationship between species, where one organism, the parasite, lives on or inside another organism, the host, causing it some harm, and is adapted structurally to this way of life. The entomologist E. O. Wilson h ...
, which is then in its asexual lifecycle
Life cycle, life-cycle, or lifecycle may refer to:
Science and academia
*Biological life cycle, the sequence of life stages that an organism undergoes from birth to reproduction ending with the production of the offspring
*Life-cycle hypothesis, ...
stage, must degrade hemoglobin
Hemoglobin (haemoglobin BrE) (from the Greek word αἷμα, ''haîma'' 'blood' + Latin ''globus'' 'ball, sphere' + ''-in'') (), abbreviated Hb or Hgb, is the iron-containing oxygen-transport metalloprotein present in red blood cells (erythroc ...
to acquire essential amino acids, which the parasite requires to construct its own protein and for energy metabolism. Digestion is carried out in a vacuole of the parasitic cell.
Hemoglobin is composed of a protein unit (digested by the parasite) and a heme unit (not used by the parasite). During this process, the parasite releases the toxic and soluble molecule heme
Heme, or haem (pronounced / hi:m/ ), is a precursor to hemoglobin, which is necessary to bind oxygen in the bloodstream. Heme is biosynthesized in both the bone marrow and the liver.
In biochemical terms, heme is a coordination complex "consis ...
. The heme moiety consists of a porphyrin ring called Fe(II)-protoporphyrin IX (FP). To avoid destruction by this molecule, the parasite biocrystallizes heme to form hemozoin
Haemozoin is a disposal product formed from the digestion of blood by some blood-feeding parasites. These hematophagous organisms such as malaria parasites (''Plasmodium spp.''), '' Rhodnius'' and ''Schistosoma'' digest haemoglobin and release hi ...
, a nontoxic molecule. Hemozoin collects in the digestive vacuole as insoluble crystals.
Chloroquine enters the red blood cell by simple diffusion, inhibiting the parasite cell and digestive vacuole. Chloroquine then becomes protonated (to CQ2+), as the digestive vacuole is known to be acidic (pH 4.7); chloroquine then cannot leave by diffusion. Chloroquine caps hemozoin molecules to prevent further biocrystallization
Biocrystallization is the formation of crystals from organic macromolecules by living organisms. This may be a stress response, a normal part of metabolism such as processes that dispose of waste compounds, or a pathology. Template mediated crysta ...
of heme, thus leading to heme buildup. Chloroquine binds to heme (or FP) to form the FP-chloroquine complex; this complex is highly toxic to the cell and disrupts membrane function. Action of the toxic FP-chloroquine and FP results in cell lysis and ultimately parasite cell autodigestion. Parasites that do not form hemozoin are therefore resistant to chloroquine.
Resistance in malaria
Since the first documentation of ''P. falciparum'' chloroquine resistance in the 1950s, resistant strains have appeared throughout East and West Africa, Southeast Asia, and South America. The effectiveness of chloroquine against ''P. falciparum'' has declined as resistant strains of the parasite evolved. Resistant parasites are able to rapidly remove chloroquine from the digestive vacuole using a transmembrane pump. Chloroquine-resistant parasites pump chloroquine out at 40 times the rate of chloroquine-sensitive parasites; the pump is coded by the ''P. falciparum'' chloroquine resistance transporter (''PfCRT'') gene. The natural function of the chloroquine pump is to transport peptides: mutations to the pump that allow it to pump chloroquine out impairs its function as a peptide pump and comes at a cost to the parasite, making it less fit. Resistant parasites also frequently have mutation in the ABC transporter ''P. falciparum'' multidrug resistance (''PfMDR1'') gene, although these mutations are thought to be of secondary importance compared to ''PfCRT''. An altered chloroquine-transporter protein, ''CG2'' has been associated with chloroquine resistance, but other mechanisms of resistance also appear to be involved. Verapamil, a Ca2+ channel blocker, has been found to restore both the chloroquine concentration ability and sensitivity to this drug. Other agents which have been shown to reverse chloroquine resistance in malaria arechlorpheniramine
Chlorphenamine (CP, CPM), also known as chlorpheniramine, is an antihistamine used to treat the symptoms of allergic conditions such as allergic rhinitis (hay fever). It is taken by mouth. The medication takes effect within two hours and lasts ...
, gefitinib, imatinib
Imatinib, sold under the brand names Gleevec and Glivec (both marketed worldwide by Novartis) among others, is an oral chemotherapy medication used to treat cancer. Imatinib is a small molecule inhibitor targeting multiple receptor tyrosine kin ...
, tariquidar
Tariquidar (INN/USAN
280px, "Samguk Sagi" Book 04. Silla's Records. In 512, Usan-guk(于山國)was Ulleungdo(鬱陵島)
Usan-guk, or the State of Usan, occupied Ulleung-do and the adjacent islands during the Korean Three Kingdoms ...
and zosuquidar
Zosuquidar (development code LY-335979) is an experimental antineoplastic drug. Zosquidir inhibits P-glycoproteins. Other drugs with this mechanism include tariquidar and laniquidar. P-glycoproteins are trans-membrane proteins that pump fo ...
.
chloroquine is still effective against poultry malaria in Thailand
Thailand ( ), historically known as Siam () and officially the Kingdom of Thailand, is a country in Southeast Asia, located at the centre of the Indochinese Peninsula, spanning , with a population of almost 70 million. The country is b ...
. Sohsuebngarm et al. 2014 test '' P. gallinaceum'' at Chulalongkorn University and find the parasite is not resistant. Sertraline
Sertraline, sold under the brand name Zoloft among others, is an antidepressant of the selective serotonin reuptake inhibitor (SSRI) class. The efficacy of sertraline for depression is similar to that of other antidepressants, and the diffe ...
, fluoxetine
Fluoxetine, sold under the brand names Prozac and Sarafem, among others, is an antidepressant of the selective serotonin reuptake inhibitor (SSRI) class. It is used for the treatment of major depressive disorder, obsessive–compulsive diso ...
and paroxetine reverse chloroquine resistance, making resistant biotypes susceptible if used in a cotreatment.
Antiviral
Chloroquine hasantiviral
Antiviral drugs are a class of medication used for treating viral infections. Most antivirals target specific viruses, while a broad-spectrum antiviral is effective against a wide range of viruses. Unlike most antibiotics, antiviral drugs do n ...
effects against some viruses. It increases late endosomal and lysosomal pH, resulting in impaired release of the virus from the endosome or lysosome – release of the virus requires a low pH. The virus is therefore unable to release its genetic material into the cell and replicate.
Chloroquine also seems to act as a zinc ionophore that allows extracellular zinc to enter the cell and inhibit viral RNA-dependent RNA polymerase
In molecular biology, RNA polymerase (abbreviated RNAP or RNApol), or more specifically DNA-directed/dependent RNA polymerase (DdRP), is an enzyme that synthesizes RNA from a DNA template.
Using the enzyme helicase, RNAP locally opens th ...
.
Other
Chloroquine inhibitsthiamine
Thiamine, also known as thiamin and vitamin B1, is a vitamin, an essential micronutrient, that cannot be made in the body. It is found in food and commercially synthesized to be a dietary supplement or medication. Phosphorylated forms of thi ...
uptake. It acts specifically on the transporter SLC19A3.
Against rheumatoid arthritis
Rheumatoid arthritis (RA) is a long-term autoimmune disorder that primarily affects joints. It typically results in warm, swollen, and painful joints. Pain and stiffness often worsen following rest. Most commonly, the wrist and hands are inv ...
, it operates by inhibiting lymphocyte
A lymphocyte is a type of white blood cell (leukocyte) in the immune system of most vertebrates. Lymphocytes include natural killer cells (which function in cell-mediated, cytotoxic innate immunity), T cells (for cell-mediated, cytotoxic a ...
proliferation, phospholipase A2
The enzyme phospholipase A2 (EC 3.1.1.4, PLA2, systematic name phosphatidylcholine 2-acylhydrolase) catalyse the cleavage of fatty acids in position 2 of phospholipids, hydrolyzing the bond between the second fatty acid “tail” and the glyc ...
, antigen presentation in dendritic cells, release of enzyme
Enzymes () are proteins that act as biological catalysts by accelerating chemical reactions. The molecules upon which enzymes may act are called substrates, and the enzyme converts the substrates into different molecules known as products ...
s from lysosome
A lysosome () is a membrane-bound organelle found in many animal cells. They are spherical vesicles that contain hydrolytic enzymes that can break down many kinds of biomolecules. A lysosome has a specific composition, of both its membrane p ...
s, release of reactive oxygen species from macrophage
Macrophages (abbreviated as M φ, MΦ or MP) ( el, large eaters, from Greek ''μακρός'' (') = large, ''φαγεῖν'' (') = to eat) are a type of white blood cell of the immune system that engulfs and digests pathogens, such as cancer ce ...
s, and production of IL-1.
History
InPeru
, image_flag = Flag of Peru.svg
, image_coat = Escudo nacional del Perú.svg
, other_symbol = Great Seal of the State
, other_symbol_type = National seal
, national_motto = "Firm and Happy f ...
, the indigenous people extracted the bark of the ''Cinchona
''Cinchona'' (pronounced or ) is a genus of flowering plants in the family Rubiaceae containing at least 23 species of trees and shrubs. All are native to the tropical Andean forests of western South America. A few species are reportedly nat ...
'' tree ('' Cinchona officinalis'') and used the extract to fight chills and fever in the seventeenth century. In 1633 this herbal medicine was introduced in Europe, where it was given the same use and also began to be used against malaria. The quinoline antimalarial drug quinine
Quinine is a medication used to treat malaria and babesiosis. This includes the treatment of malaria due to '' Plasmodium falciparum'' that is resistant to chloroquine when artesunate is not available. While sometimes used for nocturnal leg ...
was isolated from the extract in 1820.
After World War I, the German government sought alternatives to quinine. Chloroquine, a synthetic analogue with the same mechanism of action
In pharmacology, the term mechanism of action (MOA) refers to the specific biochemical interaction through which a drug substance produces its pharmacological effect. A mechanism of action usually includes mention of the specific molecular targ ...
was discovered in 1934, by Hans Andersag and coworkers at the Bayer
Bayer AG (, commonly pronounced ; ) is a German multinational pharmaceutical and biotechnology company and one of the largest pharmaceutical companies in the world. Headquartered in Leverkusen, Bayer's areas of business include pharmaceutic ...
laboratories, who named it Resochin. It was ignored for a decade, because it was considered too toxic for human use. Instead, in World War II, the German Africa Corps
The Afrika Korps or German Africa Corps (, }; DAK) was the German expeditionary force in Africa during the North African Campaign of World War II. First sent as a holding force to shore up the Italian defense of its African colonies, the ...
used the chloroquine analogue 3-methyl-chloroquine, known as Sontochin. After Allied forces arrived in Tunis, Sontochin fell into the hands of Americans, who sent the material back to the United States for analysis, leading to renewed interest in chloroquine. United States government-sponsored clinical trials for antimalarial drug development showed unequivocally that chloroquine has a significant therapeutic value as an antimalarial drug. It was introduced into clinical practice in 1947 for the prophylactic treatment of malaria.
Chemical synthesis
The first synthesis of chloroquine was disclosed in a patent filed byIG Farben
Interessengemeinschaft Farbenindustrie AG (), commonly known as IG Farben (German for 'IG Dyestuffs'), was a German chemical and pharmaceutical conglomerate. Formed in 1925 from a merger of six chemical companies— BASF, Bayer, Hoechst, Agf ...
in 1937. In the final step, 4,7-dichloroquinoline was reacted with 1-diethylamino-4-aminopentane.
: Society and culture

Formulations
Chloroquine comes in tablet form as the phosphate, sulfate, and hydrochloride salts. Chloroquine is usually dispensed as the phosphate.Names
Brand names include Chloroquine FNA, Resochin, Dawaquin, and Lariago.Other animals
Chloroquine, in various chemical forms, is used to treat and control surface growth of anemones and algae, and many protozoan infections in aquariums, e.g. the fish parasite ''Amyloodinium ocellatum
''Amyloodinium ocellatum'' (Brown, 1931) is a cosmopolitan distribution, cosmopolitan ectoparasite dinoflagellate of numerous aquatic organisms living in brackish and seawater environments. The dinoflagellate is Endemism, endemic in temperate an ...
''. It is also used in poultry malaria.
Research
Chloroquine was proposed as a treatment forSARS
Severe acute respiratory syndrome (SARS) is a viral respiratory disease of zoonotic origin caused by the severe acute respiratory syndrome coronavirus (SARS-CoV or SARS-CoV-1), the first identified strain of the SARS coronavirus species, ''seve ...
, with ''in vitro
''In vitro'' (meaning in glass, or ''in the glass'') studies are performed with microorganisms, cells, or biological molecules outside their normal biological context. Colloquially called " test-tube experiments", these studies in biology a ...
'' tests inhibiting the SARS-CoV virus. In October 2004, a published report stated that chloroquine acts as an effective inhibitor of the replication of the severe acute respiratory syndrome coronavirus ( SARS-CoV) in vitro. In August 2005, a peer-reviewed study confirmed and expanded upon the results.
Chloroquine was being considered in 2003, in pre-clinical models as a potential agent against chikungunya
Chikungunya is an infection caused by the ''Chikungunya virus'' (CHIKV). Symptoms include fever and joint pains. These typically occur two to twelve days after exposure. Other symptoms may include headache, muscle pain, joint swelling, and a r ...
fever.
COVID-19
Other
The radiosensitizing and chemosensitizing properties of chloroquine are being evaluated for anticancer strategies in humans.In biomedicinal science, chloroquine is used for ''
in vitro
''In vitro'' (meaning in glass, or ''in the glass'') studies are performed with microorganisms, cells, or biological molecules outside their normal biological context. Colloquially called " test-tube experiments", these studies in biology a ...
'' experiments to inhibit lysosomal degradation of protein products. Chloroquine and its modified forms have also been evaluated as treatment options for inflammatory conditions like rheumatoid arthritis and inflammatory bowel disease.
References
External links
* * * {{Authority control 1934 introductions Antimalarial agents Chloroarenes CYP2D6 inhibitors AstraZeneca brands Diethylamino compounds HERG blocker Quinolines World Health Organization essential medicines Wikipedia medicine articles ready to translate German inventions of the Nazi period Disease-modifying antirheumatic drugs