Coronavirus disease 2019 (COVID-19) is a
contagious disease
A contagious disease is an infectious disease that is readily spread (that is, communicated) by transmission of a pathogen through contact (direct or indirect) with an infected person.
A disease is often known to be contagious before medical s ...
caused by a
virus
A virus is a submicroscopic infectious agent that replicates only inside the living cells of an organism. Viruses infect all life forms, from animals and plants to microorganisms, including bacteria and archaea.
Since Dmitri Ivanovsky's 1 ...
, the
severe acute respiratory syndrome coronavirus 2
Severe acute respiratory syndrome coronavirus 2 (SARS‑CoV‑2) is a strain of coronavirus that causes COVID-19 (coronavirus disease 2019), the respiratory illness responsible for the ongoing COVID-19 pandemic. The virus previously had a No ...
(SARS-CoV-2). The first known case was
identified in Wuhan, China, in December 2019.
The disease quickly spread worldwide, resulting in the
COVID-19 pandemic
The COVID-19 pandemic, also known as the coronavirus pandemic, is an ongoing global pandemic of coronavirus disease 2019 (COVID-19) caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). The novel virus was first identif ...
.
The
symptoms of COVID‑19
Signs and symptoms are the observed or detectable signs, and experienced symptoms of an illness, injury, or condition. A sign for example may be a higher or lower temperature than normal, raised or lowered blood pressure or an abnormality showin ...
are variable but often include fever, cough, headache, fatigue,
breathing difficulties
Shortness of breath (SOB), also medically known as dyspnea (in AmE) or dyspnoea (in BrE), is an uncomfortable feeling of not being able to breathe well enough. The American Thoracic Society defines it as "a subjective experience of breathing di ...
,
loss of smell, and
loss of taste. Symptoms may begin one to fourteen days
after exposure to the virus. At least a third of people who are infected
do not develop noticeable symptoms. Of those who develop symptoms noticeable enough to be classified as patients, most (81%) develop mild to moderate symptoms (up to mild
pneumonia
Pneumonia is an inflammatory condition of the lung primarily affecting the small air sacs known as alveoli. Symptoms typically include some combination of productive or dry cough, chest pain, fever, and difficulty breathing. The severity ...
), while 14% develop severe symptoms (
dyspnea
Shortness of breath (SOB), also medically known as dyspnea (in AmE) or dyspnoea (in BrE), is an uncomfortable feeling of not being able to breathing, breathe well enough. The American Thoracic Society defines it as "a subjective experience of brea ...
,
hypoxia, or more than 50% lung involvement on imaging), and 5% develop critical symptoms (
respiratory failure
Respiratory failure results from inadequate gas exchange by the respiratory system, meaning that the arterial oxygen, carbon dioxide, or both cannot be kept at normal levels. A drop in the oxygen carried in the blood is known as hypoxemia; a rise ...
,
shock
Shock may refer to:
Common uses Collective noun
*Shock, a historic commercial term for a group of 60, see English numerals#Special names
* Stook, or shock of grain, stacked sheaves
Healthcare
* Shock (circulatory), circulatory medical emergen ...
, or
multiorgan dysfunction).
Older people
Old age refers to ages nearing or surpassing the life expectancy of human beings, and is thus the end of the human life cycle. Terms and euphemisms for people at this age include old people, the elderly (worldwide usage), OAPs (British usage ...
are at a higher risk of developing severe symptoms. Some people continue to experience a range of effects (
long COVID
Long COVID or long-haul COVID (also known as post-COVID-19 syndrome, post-COVID-19 condition, post-acute sequelae of COVID-19 (PASC), or chronic COVID syndrome (CCS)) is a condition characterized by long-term health problems persisting or appe ...
) for months after recovery, and damage to organs has been observed.
Multi-year studies are underway to further investigate the long-term effects of the disease.
when people breathe air contaminated by droplets and small
airborne
Airborne or Airborn may refer to:
Arts, entertainment, and media
Films
* ''Airborne'' (1962 film), a 1962 American film directed by James Landis
* ''Airborne'' (1993 film), a comedy–drama film
* ''Airborne'' (1998 film), an action film sta ...
particles containing the virus. The risk of breathing these is highest when people are in close proximity, but they can be inhaled over longer distances, particularly indoors. Transmission can also occur if contaminated fluids are splashed or sprayed in the eyes, nose, or mouth, or, more rarely, via contaminated surfaces. People remain contagious for up to 20 days and can spread the virus even if they do not develop symptoms.
to detect the virus's
nucleic acid
Nucleic acids are biopolymers, macromolecules, essential to all known forms of life. They are composed of nucleotides, which are the monomers made of three components: a 5-carbon sugar, a phosphate group and a nitrogenous base. The two main cl ...
include
real-time reverse transcription polymerase chain reaction (rRTPCR),
transcription-mediated amplification
Transcription-mediated amplification (TMA) is an isothermal (does not change the nucleic acid temperature), single-tube nucleic acid amplification system utilizing two enzymes, RNA polymerase and reverse transcriptase.
"Amplification" means crea ...
,
and
reverse transcription loop-mediated isothermal amplification
Reverse transcription loop-mediated isothermal amplification (RT-LAMP) is a one step nucleic acid amplification method to multiply specific sequences of RNA. It is used to diagnose infectious disease caused by RNA viruses.
It combines LAMP DNA- ...
(RTLAMP)
from a
nasopharyngeal swab
A nasopharyngeal swab is a device used for collecting a sample of nasal secretions from the back of the nose and throat. The sample is then analyzed for the presence of organisms or other clinical markers for disease. This diagnostic method is c ...
.
Several
COVID-19 vaccine
A COVID19 vaccine is a vaccine intended to provide acquired immunity against severe acute respiratory syndrome coronavirus 2 (SARS‑CoV‑2), the virus that causes coronavirus disease 2019 ( COVID19).
Prior to the COVID19 pandemic, an e ...
s have been approved and distributed in various countries, which have initiated
mass vaccination campaigns. Other
preventive measures include
physical or social distancing,
quarantining, ventilation of indoor spaces,
use of face masks or coverings in public, covering coughs and sneezes,
hand washing
Hand washing (or handwashing), also known as hand hygiene, is the act of cleaning one's hands with soap, soap or handwash and water to remove viruses/bacteria/microorganisms, dirt, grease, or other harmful and unwanted substances stuck to the ...
, and keeping unwashed hands away from the face. While work is underway to
develop drugs that inhibit the virus, the primary
treatment is symptomatic. Management involves the
treatment of symptoms through
supportive care
Symptomatic treatment, supportive care, supportive therapy, or palliative treatment is any medical therapy of a disease that only affects its symptoms, not the underlying cause. It is usually aimed at reducing the signs and symptoms for the comfor ...
,
isolation, and
experimental measures.
Nomenclature
During the initial outbreak in
Wuhan
Wuhan (, ; ; ) is the capital of Hubei, Hubei Province in the China, People's Republic of China. It is the largest city in Hubei and the most populous city in Central China, with a population of over eleven million, the List of cities in China ...
, the virus and disease were commonly referred to as "coronavirus" and "Wuhan coronavirus", with the disease sometimes called "Wuhan pneumonia". In the past, many diseases have been named after geographical locations, such as the
Spanish flu
The 1918–1920 influenza pandemic, commonly known by the misnomer Spanish flu or as the Great Influenza epidemic, was an exceptionally deadly global influenza pandemic caused by the H1N1 influenza A virus. The earliest documented case was ...
,
Middle East respiratory syndrome
Middle East respiratory syndrome (MERS) is a viral respiratory infection caused by ''Middle East respiratory syndrome–related coronavirus'' (MERS-CoV). Symptoms may range from none, to mild, to severe. Typical symptoms include fever, cough, ...
, and
Zika virus
''Zika virus'' (ZIKV; pronounced or ) is a member of the virus family ''Flaviviridae''. It is spread by daytime-active ''Aedes'' mosquitoes, such as '' A. aegypti'' and '' A. albopictus''. Its name comes from the Ziika Forest of Uganda, whe ...
.
In January 2020, the
World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level of h ...
(WHO) recommended 2019-nCoV and 2019-nCoV acute respiratory disease as interim names for the virus and disease per 2015 guidance and international guidelines against using geographical locations or groups of people in disease and virus names to prevent
social stigma
Social stigma is the disapproval of, or discrimination against, an individual or group based on perceived characteristics that serve to distinguish them from other members of a society. Social stigmas are commonly related to culture, gender, rac ...
.
The official names COVID‑19 and SARS-CoV-2 were issued by the WHO on 11 February 2020 with COVID-19 being shorthand for "coronavirus disease 2019".
The WHO additionally uses "the COVID‑19 virus" and "the virus responsible for COVID‑19" in public communications.
Signs and symptoms
Cause
COVID‑19 is caused by infection with a
strain
Strain may refer to:
Science and technology
* Strain (biology), variants of plants, viruses or bacteria; or an inbred animal used for experimental purposes
* Strain (chemistry), a chemical stress of a molecule
* Strain (injury), an injury to a mu ...
of
coronavirus
Coronaviruses are a group of related RNA viruses that cause diseases in mammals and birds. In humans and birds, they cause respiratory tract infections that can range from mild to lethal. Mild illnesses in humans include some cases of the com ...
known as 'Severe Acute Respiratory Syndrome coronavirus 2' (
SARS-CoV-2
Severe acute respiratory syndrome coronavirus 2 (SARS‑CoV‑2) is a strain of coronavirus that causes COVID-19 (coronavirus disease 2019), the respiratory illness responsible for the ongoing COVID-19 pandemic. The virus previously had a ...
).
Transmission

Virology

Severe acute respiratory syndrome coronavirus2 (SARS-CoV-2) is a
novel
A novel is a relatively long work of narrative fiction, typically written in prose and published as a book. The present English word for a long work of prose fiction derives from the for "new", "news", or "short story of something new", itsel ...
severe acute respiratory syndrome coronavirus. It was first isolated from three people with pneumonia connected to the
cluster
may refer to:
Science and technology Astronomy
* Cluster (spacecraft), constellation of four European Space Agency spacecraft
* Asteroid cluster, a small asteroid family
* Cluster II (spacecraft), a European Space Agency mission to study t ...
of acute respiratory illness cases in Wuhan.
All structural features of the novel SARS-CoV-2 virus particle occur in related
coronavirus
Coronaviruses are a group of related RNA viruses that cause diseases in mammals and birds. In humans and birds, they cause respiratory tract infections that can range from mild to lethal. Mild illnesses in humans include some cases of the com ...
es in nature.
Outside the human body, the virus is destroyed by household soap, which bursts its
protective bubble.
SARS-CoV-2 is closely related to the original
SARS-CoV
Severe acute respiratory syndrome coronavirus 1 (SARS-CoV-1; or Severe acute respiratory syndrome coronavirus, SARS-CoV) is a strain of coronavirus that causes severe acute respiratory syndrome (SARS), the respiratory illness responsible for ...
.
It is thought to have an animal (
zoonotic
A zoonosis (; plural zoonoses) or zoonotic disease is an infectious disease of humans caused by a pathogen (an infectious agent, such as a bacterium, virus, parasite or prion) that has jumped from a non-human (usually a vertebrate) to a human. ...
) origin. Genetic analysis has revealed that the coronavirus genetically clusters with the genus ''
Betacoronavirus
''Betacoronavirus'' (β-CoVs or Beta-CoVs) is one of four genera (''Alpha''-, ''Beta-'', '' Gamma-'', and '' Delta-'') of coronaviruses. Member viruses are enveloped, positive-strand RNA viruses that infect mammals (of which humans are part). ...
'', in subgenus
''Sarbecovirus'' (lineage B) together with two bat-derived strains. It is 96% identical at the whole
genome
In the fields of molecular biology and genetics, a genome is all the genetic information of an organism. It consists of nucleotide sequences of DNA (or RNA in RNA viruses). The nuclear genome includes protein-coding genes and non-coding ge ...
level to other bat coronavirus samples (BatCov
RaTG13
Bat coronavirus RaTG13 is a SARS-like betacoronavirus that infects the horseshoe bat '' Rhinolophus affinis''. It was discovered in 2013 in bat droppings from a mining cave near the town of Tongguan in Mojiang county in Yunnan, China. In Februar ...
).
The structural proteins of SARS-CoV-2 include
membrane glycoprotein
Glycoproteins are proteins which contain oligosaccharide chains covalently attached to amino acid side-chains. The carbohydrate is attached to the protein in a cotranslational or posttranslational modification. This process is known as glycosy ...
(M),
envelope protein
A viral envelope is the outermost layer of many types of viruses. It protects the genetic material in their life cycle when traveling between host cells. Not all viruses have envelopes.
Numerous human pathogenic viruses in circulation are encase ...
(E),
nucleocapsid protein (N), and the
spike protein
In virology, a spike protein or peplomer protein is a protein that forms a large structure known as a spike or peplomer projecting from the surface of an enveloped virus. as cited in The proteins are usually glycoproteins that form dimers or ...
(S). The M protein of SARS-CoV-2 is about 98% similar to the M protein of bat SARS-CoV, maintains around 98% homology with pangolin SARS-CoV, and has 90% homology with the M protein of SARS-CoV; whereas, the similarity is only around 38% with the M protein of MERS-CoV.
SARS-CoV-2 variants
The many thousands of SARS-CoV-2 variants are grouped into either
clade
A clade (), also known as a monophyletic group or natural group, is a group of organisms that are monophyletic – that is, composed of a common ancestor and all its lineal descendants – on a phylogenetic tree. Rather than the English term, ...
s or
lineages.
The WHO, in collaboration with partners, expert networks, national authorities, institutions and researchers, have established nomenclature systems for naming and tracking SARS-CoV-2 genetic lineages by
GISAID
GISAID (Global Initiative on Sharing Avian Influenza Data) is a global science initiative and primary source established in 2008 that provides open access to genomic data of influenza viruses and the coronavirus responsible for the COVID-19 pan ...
,
Nextstrain
Nextstrain is a collaboration between researchers in Seattle, United States and Basel, Switzerland which provides a collection of open-source tools for visualising the genetics behind the spread of viral outbreaks.
Its aim is to support public he ...
and
Pango
Pango (stylized as Παν語) is a text (i.e. glyph) layout engine library which works with the HarfBuzz shaping engine for displaying multi-language text.
Full-function rendering of text and cross-platform support is achieved when Pango is us ...
. The expert group convened by the WHO recommended the labelling of variants using letters of the
Greek alphabet
The Greek alphabet has been used to write the Greek language since the late 9th or early 8th century BCE. It is derived from the earlier Phoenician alphabet, and was the earliest known alphabetic script to have distinct letters for vowels as we ...
, for example,
Alpha
Alpha (uppercase , lowercase ; grc, ἄλφα, ''álpha'', or ell, άλφα, álfa) is the first letter of the Greek alphabet. In the system of Greek numerals, it has a value of one. Alpha is derived from the Phoenician letter aleph , whic ...
,
Beta
Beta (, ; uppercase , lowercase , or cursive ; grc, βῆτα, bē̂ta or ell, βήτα, víta) is the second letter of the Greek alphabet. In the system of Greek numerals, it has a value of 2. In Modern Greek, it represents the voiced labiod ...
,
Delta
Delta commonly refers to:
* Delta (letter) (Δ or δ), a letter of the Greek alphabet
* River delta, at a river mouth
* D ( NATO phonetic alphabet: "Delta")
* Delta Air Lines, US
* Delta variant of SARS-CoV-2 that causes COVID-19
Delta may also ...
, and
Gamma
Gamma (uppercase , lowercase ; ''gámma'') is the third letter of the Greek alphabet. In the system of Greek numerals it has a value of 3. In Ancient Greek, the letter gamma represented a voiced velar stop . In Modern Greek, this letter re ...
, giving the justification that they "will be easier and more practical to discussed by non-scientific audiences."
Nextstrain
Nextstrain is a collaboration between researchers in Seattle, United States and Basel, Switzerland which provides a collection of open-source tools for visualising the genetics behind the spread of viral outbreaks.
Its aim is to support public he ...
divides the variants into five clades (19A, 19B, 20A, 20B, and 20C), while
GISAID
GISAID (Global Initiative on Sharing Avian Influenza Data) is a global science initiative and primary source established in 2008 that provides open access to genomic data of influenza viruses and the coronavirus responsible for the COVID-19 pan ...
divides them into seven (L, O, V, S, G, GH, and GR).
The Pango tool groups variants into
lineages, with many circulating lineages being classed under the B.1 lineage.
Several notable variants of SARS-CoV-2 emerged throughout 2020.
Cluster 5
Cluster 5 is a designation used by the Danish Statens Serum Institut for a virus variant described by the institute in autumn 2020, in connection with investigations of SARS-CoV-2 infection among mink and humans in the north of Jutland, Denmark. ...
emerged among
mink
Mink are dark-colored, semiaquatic, carnivorous mammals of the genera ''Neogale'' and '' Mustela'' and part of the family Mustelidae, which also includes weasels, otters, and ferrets. There are two extant species referred to as "mink": the A ...
s and mink farmers in
Denmark
)
, song = ( en, "King Christian stood by the lofty mast")
, song_type = National and royal anthem
, image_map = EU-Denmark.svg
, map_caption =
, subdivision_type = Sovereign state
, subdivision_name = Danish Realm, Kingdom of Denmark
...
. After strict quarantines and a mink euthanasia campaign, the cluster was assessed to no longer be circulating among humans in Denmark as of 1 February 2021.
, there are five dominant variants of SARS-CoV-2 spreading among global populations: the
Alpha variant
The Alpha variant (B.1.1.7) was a SARS-CoV-2 variant of concern. It was estimated to be 40–80% more transmissible than the wild-type SARS-CoV-2 (with most estimates occupying the middle to higher end of this range). It was first detecte ...
(B.1.1.7, formerly called the UK variant), first found in London and Kent, the
Beta variant
The Beta variant, (B.1.351), was a variant of SARS-CoV-2, the virus that causes COVID-19. One of several SARS-CoV-2 variants initially believed to be of particular importance, it was first detected in the Nelson Mandela Bay metropolitan are ...
(B.1.351, formerly called the South Africa variant), the
Gamma variant (P.1, formerly called the Brazil variant), the
Delta variant
The Delta variant (B.1.617.2) was a variant of SARS-CoV-2, the virus that causes COVID-19. It was first detected in India in late 2020. The Delta variant was named on 31 May 2021 and had spread to over 179 countries by 22 November 2021. The ...
(B.1.617.2, formerly called the India variant), and the
Omicron variant
Omicron (B.1.1.529) is a variant of SARS-CoV-2 first reported to the World Health Organization (WHO) by the Network for Genomics Surveillance in South Africa on 24 November 2021. It was first detected in Botswana and has spread to become the ...
(B.1.1.529), which had spread to 57 countries as of 7 December.
Pathophysiology

The SARS-CoV-2 virus can infect a wide range of cells and systems of the body. COVID‑19 is most known for affecting the upper respiratory tract (sinuses, nose, and throat) and the lower respiratory tract (windpipe and lungs).
The lungs are the organs most affected by COVID‑19 because the virus accesses host cells via the
receptor
Receptor may refer to:
* Sensory receptor, in physiology, any structure which, on receiving environmental stimuli, produces an informative nerve impulse
*Receptor (biochemistry), in biochemistry, a protein molecule that receives and responds to a ...
for the enzyme
angiotensin-converting enzyme 2
Angiotensin-converting enzyme 2 (ACE2) is an enzyme that can be found either attached to the membrane of cells (mACE2) in the intestines, kidney, testis, gallbladder, and heart or in a soluble form (sACE2). Both membrane bound and soluble ACE2 a ...
(ACE2), which is most abundant on the surface of
type II alveolar cells of the lungs. The virus uses a special surface glycoprotein called a "
spike
Spike, spikes, or spiking may refer to:
Arts, entertainment, and media
Books
* ''The Spike'' (novel), a novel by Arnaud de Borchgrave
* ''The Spike'' (book), a nonfiction book by Damien Broderick
* ''The Spike'', a starship in Peter F. Hamilto ...
" to connect to the ACE2 receptor and enter the host cell.
Respiratory tract
Following viral entry, COVID‑19 infects the ciliated epithelium of the nasopharynx and upper airways.
Nervous system
One common symptom, loss of smell, results from
infection of the support cells of the olfactory epithelium, with subsequent damage to the
olfactory neurons
An olfactory receptor neuron (ORN), also called an olfactory sensory neuron (OSN), is a sensory neuron within the olfactory system.
Structure
Humans have between 10 and 20 million olfactory receptor neurons (ORNs). In vertebrates, ORNs are b ...
.
The involvement of both the central and peripheral nervous system in COVID‑19 has been reported in many medical publications.
It is clear that many people with
COVID-19 exhibit neurological or mental health issues. The virus is not detected in the
central nervous system
The central nervous system (CNS) is the part of the nervous system consisting primarily of the brain and spinal cord. The CNS is so named because the brain integrates the received information and coordinates and influences the activity of all par ...
(CNS) of the majority of COVID-19 patients with
neurological issues. However, SARS-CoV-2 has been detected at low levels in the brains of those who have died from COVID‑19, but these results need to be confirmed.
While virus has been detected in
cerebrospinal fluid
Cerebrospinal fluid (CSF) is a clear, colorless body fluid found within the tissue that surrounds the brain and spinal cord of all vertebrates.
CSF is produced by specialised ependymal cells in the choroid plexus of the ventricles of the bra ...
of autopsies, the exact mechanism by which it invades the CNS remains unclear and may first involve invasion of peripheral nerves given the low levels of ACE2 in the brain. The virus may also enter the bloodstream from the lungs and cross the blood–brain barrier to gain access to the CNS, possibly within an infected white blood cell.

Research conducted when Alpha was the dominant variant has suggested COVID-19 may cause brain damage. It is unknown if such damage is temporary or permanent, and whether Omicron has similar effects. Observed individuals infected with COVID-19 (most with mild cases) experienced an additional 0.2% to 2% of brain tissue lost in regions of the brain connected to the sense of smell compared with uninfected individuals, and the overall effect on the brain was equivalent on average to at least one extra year of normal ageing; infected individuals also scored lower on several cognitive tests. All effects were more pronounced among older ages.
Gastrointestinal tract
The virus also affects gastrointestinal organs as ACE2 is abundantly expressed in the
gland
In animals, a gland is a group of cells in an animal's body that synthesizes substances (such as hormones) for release into the bloodstream (endocrine gland) or into cavities inside the body or its outer surface (exocrine gland).
Structure
De ...
ular cells of
gastric
The stomach is a muscular, hollow organ in the gastrointestinal tract of humans and many other animals, including several invertebrates. The stomach has a dilated structure and functions as a vital organ in the digestive system. The stomach i ...
,
duodenal
The duodenum is the first section of the small intestine in most higher vertebrates, including mammals, reptiles, and birds. In fish, the divisions of the small intestine are not as clear, and the terms anterior intestine or proximal intestine ...
and
rectal
The rectum is the final straight portion of the large intestine in humans and some other mammals, and the gut in others. The adult human rectum is about long, and begins at the rectosigmoid junction (the end of the sigmoid colon) at the le ...
epithelium
Epithelium or epithelial tissue is one of the four basic types of animal tissue, along with connective tissue, muscle tissue and nervous tissue. It is a thin, continuous, protective layer of compactly packed cells with a little intercellul ...
as well as
endothelial
The endothelium is a single layer of squamous endothelial cells that line the interior surface of blood vessels and lymphatic vessels. The endothelium forms an interface between circulating blood or lymph in the lumen and the rest of the vessel ...
cells and
enterocyte
Enterocytes, or intestinal absorptive cells, are simple columnar epithelial cells which line the inner surface of the small and large intestines. A glycocalyx surface coat contains digestive enzymes. Microvilli on the apical surface increase its ...
s of the
small intestine
The small intestine or small bowel is an organ in the gastrointestinal tract where most of the absorption of nutrients from food takes place. It lies between the stomach and large intestine, and receives bile and pancreatic juice through the p ...
.
Cardiovascular system
The virus can cause
acute myocardial injury and chronic damage to the
cardiovascular system
The blood circulatory system is a system of organs that includes the heart, blood vessels, and blood which is circulated throughout the entire body of a human or other vertebrate. It includes the cardiovascular system, or vascular system, tha ...
.
An acute cardiac injury was found in 12% of infected people admitted to the hospital in Wuhan, China,
and is more frequent in severe disease. Rates of cardiovascular symptoms are high, owing to the systemic inflammatory response and immune system disorders during disease progression, but acute myocardial injuries may also be related to ACE2 receptors in the heart.
ACE2 receptors are highly expressed in the heart and are involved in heart function.
A high incidence of
thrombosis
Thrombosis (from Ancient Greek "clotting") is the formation of a blood clot inside a blood vessel, obstructing the flow of blood through the circulatory system. When a blood vessel (a vein or an artery) is injured, the body uses platelets (thro ...
and
venous thromboembolism
Venous thrombosis is blockage of a vein caused by a thrombus (blood clot). A common form of venous thrombosis is deep vein thrombosis (DVT), when a blood clot forms in the deep veins. If a thrombus breaks off (embolizes) and flows to the lungs to ...
occurs in people transferred to
intensive care unit
220px, Intensive care unit
An intensive care unit (ICU), also known as an intensive therapy unit or intensive treatment unit (ITU) or critical care unit (CCU), is a special department of a hospital or health care facility that provides intensiv ...
s with COVID‑19 infections, and may be related to poor prognosis. Blood vessel dysfunction and clot formation (as suggested by high
D-dimer
D-dimer (or D dimer) is a fibrin degradation product (or FDP), a small protein fragment present in the blood after a blood clot is degraded by fibrinolysis. It is so named because it contains two D fragments of the fibrin protein joined by a cross ...
levels caused by blood clots) may have a significant role in mortality, incidences of clots leading to
pulmonary embolism
Pulmonary embolism (PE) is a blockage of an pulmonary artery, artery in the lungs by a substance that has moved from elsewhere in the body through the bloodstream (embolism). Symptoms of a PE may include dyspnea, shortness of breath, chest pain p ...
s, and
ischaemic events within the brain found as complications leading to death in people infected with COVID‑19.
[ Infection may initiate a chain of vasoconstrictive responses within the body, including pulmonary vasoconstriction a possible mechanism in which oxygenation decreases during pneumonia.]arterioles
An arteriole is a small-diameter blood vessel in the microcirculation that extends and branches out from an artery and leads to capillaries.
Arterioles have muscular walls (usually only one to two layers of smooth muscle cells) and are the primar ...
and capillaries
A capillary is a small blood vessel from 5 to 10 micrometres (μm) in diameter. Capillaries are composed of only the tunica intima, consisting of a thin wall of simple squamous endothelial cells. They are the smallest blood vessels in the body: ...
was found in brain tissue samples of people who died from COVID‑19.
COVID‑19 may also cause substantial structural changes to blood cell
A blood cell, also called a hematopoietic cell, hemocyte, or hematocyte, is a cell produced through hematopoiesis and found mainly in the blood. Major types of blood cells include red blood cells (erythrocytes), white blood cells (leukocytes), ...
s, sometimes persisting for months after hospital discharge. A low level of blood lymphocytes may result from the virus acting through ACE2-related entry into lymphocytes.
Other organs
Another common cause of death is complications related to the kidney
The kidneys are two reddish-brown bean-shaped organs found in vertebrates. They are located on the left and right in the retroperitoneal space, and in adult humans are about in length. They receive blood from the paired renal arteries; blood ...
s.
Immunopathology
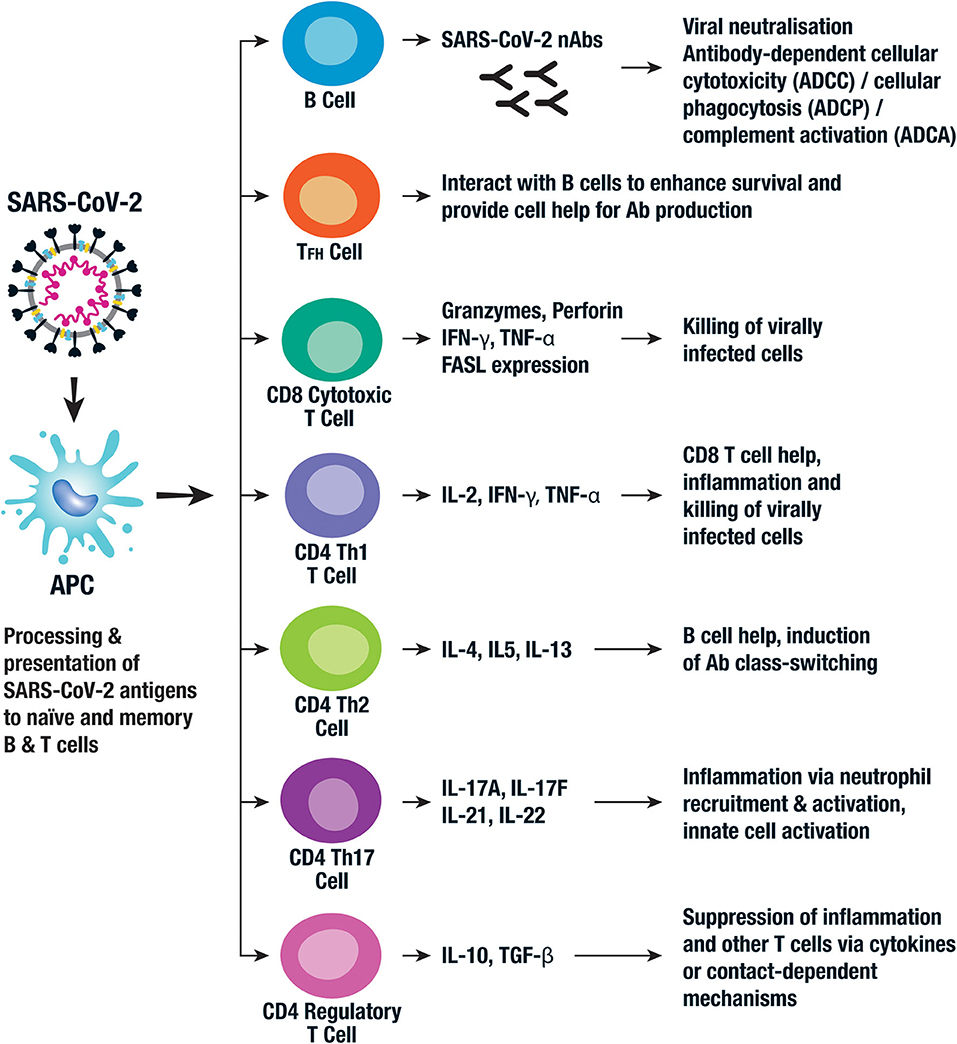 Although SARS-CoV-2 has a tropism for ACE2-expressing epithelial cells of the respiratory tract, people with severe COVID‑19 have symptoms of systemic hyperinflammation. Clinical laboratory findings of elevated IL2, IL7, IL6,
Although SARS-CoV-2 has a tropism for ACE2-expressing epithelial cells of the respiratory tract, people with severe COVID‑19 have symptoms of systemic hyperinflammation. Clinical laboratory findings of elevated IL2, IL7, IL6, granulocyte-macrophage colony-stimulating factor
Granulocyte-macrophage colony-stimulating factor (GM-CSF), also known as colony-stimulating factor 2 (CSF2), is a monomeric glycoprotein secreted by macrophages, T cells, mast cells, natural killer cells, endothelial cells and fibroblasts that ...
(GMCSF), interferon gamma-induced protein10 (IP10), monocyte chemoattractant protein1 (MCP1), macrophage inflammatory protein 1alpha (MIP1alpha), and tumour necrosis factor
The tumor necrosis factor (TNF) superfamily is a protein superfamily of type II transmembrane proteins containing TNF homology domain and forming trimers. Members of this superfamily can be released from the cell membrane by extracellular pro ...
(TNFα) indicative of cytokine release syndrome
Cytokine release syndrome (CRS) is a form of systemic inflammatory response syndrome (SIRS) that can be triggered by a variety of factors such as infections and certain drugs. It refers to cytokine storm syndromes (CSS) and occurs when large numb ...
(CRS) suggest an underlying immunopathology.Interferon alpha
The type-I interferons (IFN) are cytokines which play essential roles in inflammation, immunoregulation, tumor cells recognition, and T cell, T-cell responses. In the human genome, a cluster of thirteen functional IFN genes is located at the 9p2 ...
plays a complex, Janus-faced role in the pathogenesis of COVID-19. Although it promotes the elimination of virus-infected cells, it also upregulates the expression of ACE-2, thereby facilitating the SARS-Cov2 virus to enter cells and to replicate. A competition of negative feedback loops (via protective effects of interferon alpha) and positive feedback loops (via upregulation of ACE-2) is assumed to determine the fate of patients suffering from COVID-19.
Additionally, people with COVID‑19 and acute respiratory distress syndrome
Acute respiratory distress syndrome (ARDS) is a type of respiratory failure characterized by rapid onset of widespread inflammation in the lungs. Symptoms include shortness of breath (dyspnea), rapid breathing (tachypnea), and bluish skin colo ...
(ARDS) have classical serum biomarkers
In biomedical contexts, a biomarker, or biological marker, is a measurable indicator of some biological state or condition. Biomarkers are often measured and evaluated using blood, urine, or soft tissues to examine normal biological processes, p ...
of CRS, including elevated C-reactive protein
C-reactive protein (CRP) is an annular (ring-shaped) pentameric protein found in blood plasma, whose circulating concentrations rise in response to inflammation. It is an acute-phase protein of hepatic origin that increases following interleukin-6 ...
(CRP), lactate dehydrogenase
Lactate dehydrogenase (LDH or LD) is an enzyme found in nearly all living cells. LDH catalyzes the conversion of lactate to pyruvate and back, as it converts NAD+ to NADH and back. A dehydrogenase is an enzyme that transfers a hydride from on ...
(LDH), D-dimer
D-dimer (or D dimer) is a fibrin degradation product (or FDP), a small protein fragment present in the blood after a blood clot is degraded by fibrinolysis. It is so named because it contains two D fragments of the fibrin protein joined by a cross ...
, and ferritin
Ferritin is a universal intracellular protein that stores iron and releases it in a controlled fashion. The protein is produced by almost all living organisms, including archaea, bacteria, algae, higher plants, and animals. It is the primary ' ...
.
Systemic inflammation results in vasodilation
Vasodilation is the widening of blood vessels. It results from relaxation of smooth muscle cells within the vessel walls, in particular in the large veins, large arteries, and smaller arterioles. The process is the opposite of vasoconstriction, ...
, allowing inflammatory lymphocytic and monocytic infiltration of the lung and the heart. In particular, pathogenic GM-CSF-secreting T cells were shown to correlate with the recruitment of inflammatory IL-6-secreting monocyte
Monocytes are a type of leukocyte or white blood cell. They are the largest type of leukocyte in blood and can differentiate into macrophages and conventional dendritic cells. As a part of the vertebrate innate immune system monocytes also inf ...
s and severe lung pathology in people with COVID‑19. Lymphocytic infiltrates have also been reported at autopsy.
Viral and host factors
Virus proteins
 Multiple viral and host factors affect the pathogenesis of the virus. The S-protein, otherwise known as the spike protein, is the viral component that attaches to the host receptor via the
Multiple viral and host factors affect the pathogenesis of the virus. The S-protein, otherwise known as the spike protein, is the viral component that attaches to the host receptor via the ACE2
Angiotensin-converting enzyme 2 (ACE2) is an enzyme that can be found either attached to the membrane of cells (mACE2) in the intestines, kidney, testis, gallbladder, and heart or in a soluble form (sACE2). Both membrane bound and soluble ACE2 a ...
receptors. It includes two subunits: S1 and S2. S1 determines the virus-host range and cellular tropism via the receptor-binding domain. S2 mediates the membrane fusion of the virus to its potential cell host via the H1 and HR2, which are heptad repeat
The heptad repeat is an example of a structural motif that consists of a repeating pattern of seven amino acids:
''a b c d e f g''
H P P H C P C
where H represents hydrophobic residues, C represents, typically, charged residues, and P repre ...
regions. Studies have shown that S1 domain induced IgG
Immunoglobulin G (Ig G) is a type of antibody. Representing approximately 75% of serum antibodies in humans, IgG is the most common type of antibody found in blood circulation. IgG molecules are created and released by plasma B cells. Each IgG ...
and IgA antibody levels at a much higher capacity. It is the focus spike proteins expression that are involved in many effective COVID‑19 vaccines.
Host factors
Human angiotensin converting enzyme 2
Angiotensin-converting enzyme 2 (ACE2) is an enzyme that can be found either attached to the membrane of cells (mACE2) in the intestines, kidney, testis, gallbladder, and heart or in a soluble form (sACE2). Both membrane bound and soluble ACE2 a ...
(hACE2) is the host factor that SARS-CoV-2 virus targets causing COVID‑19. Theoretically, the usage of angiotensin receptor blockers
Angiotensin II receptor blockers (ARBs), formally angiotensin II receptor type 1 (AT1) antagonists, also known as angiotensin receptor blockers, angiotensin II receptor antagonists, or AT1 receptor antagonists, are a group of pharmaceuticals tha ...
(ARB) and ACE inhibitor
Angiotensin-converting-enzyme inhibitors (ACE inhibitors) are a class of medication used primarily for the treatment of hypertension, high blood pressure and heart failure. They work by causing relaxation of blood vessels as well as a decrease i ...
s upregulating ACE2 expression might increase morbidity
A disease is a particular abnormal condition that negatively affects the structure or function of all or part of an organism, and that is not immediately due to any external injury. Diseases are often known to be medical conditions that a ...
with COVID‑19, though animal data suggest some potential protective effect of ARB; however no clinical studies have proven susceptibility or outcomes. Until further data is available, guidelines and recommendations for hypertensive patients remain.
The effect of the virus on ACE2 cell surfaces leads to leukocytic infiltration, increased blood vessel permeability, alveolar wall permeability, as well as decreased secretion of lung surfactants. These effects cause the majority of the respiratory symptoms. However, the aggravation of local inflammation causes a cytokine storm eventually leading to a systemic inflammatory response syndrome
Systemic inflammatory response syndrome (SIRS) is an inflammatory state affecting the whole body. It is the body's response to an infectious or noninfectious insult. Although the definition of SIRS refers to it as an "inflammatory" response, i ...
.
Among healthy adults not exposed to SARS-CoV-2, about 35% have CD4+ T cells that recognise the SARS-CoV-2 S protein (particularly the S2 subunit) and about 50% react to other proteins of the virus, suggesting cross-reactivity
Cross-reactivity, in a general sense, is the reactivity of an observed agent which initiates reactions outside the main reaction expected. This has implications for any kind of test or assay, including diagnostic tests in medicine, and can be a ...
from previous common cold
The common cold or the cold is a viral infectious disease of the upper respiratory tract that primarily affects the respiratory mucosa of the nose, throat, sinuses, and larynx. Signs and symptoms may appear fewer than two days after exposu ...
s caused by other coronaviruses.
It is unknown whether different persons use similar antibody genes in response to COVID‑19.
Host cytokine response
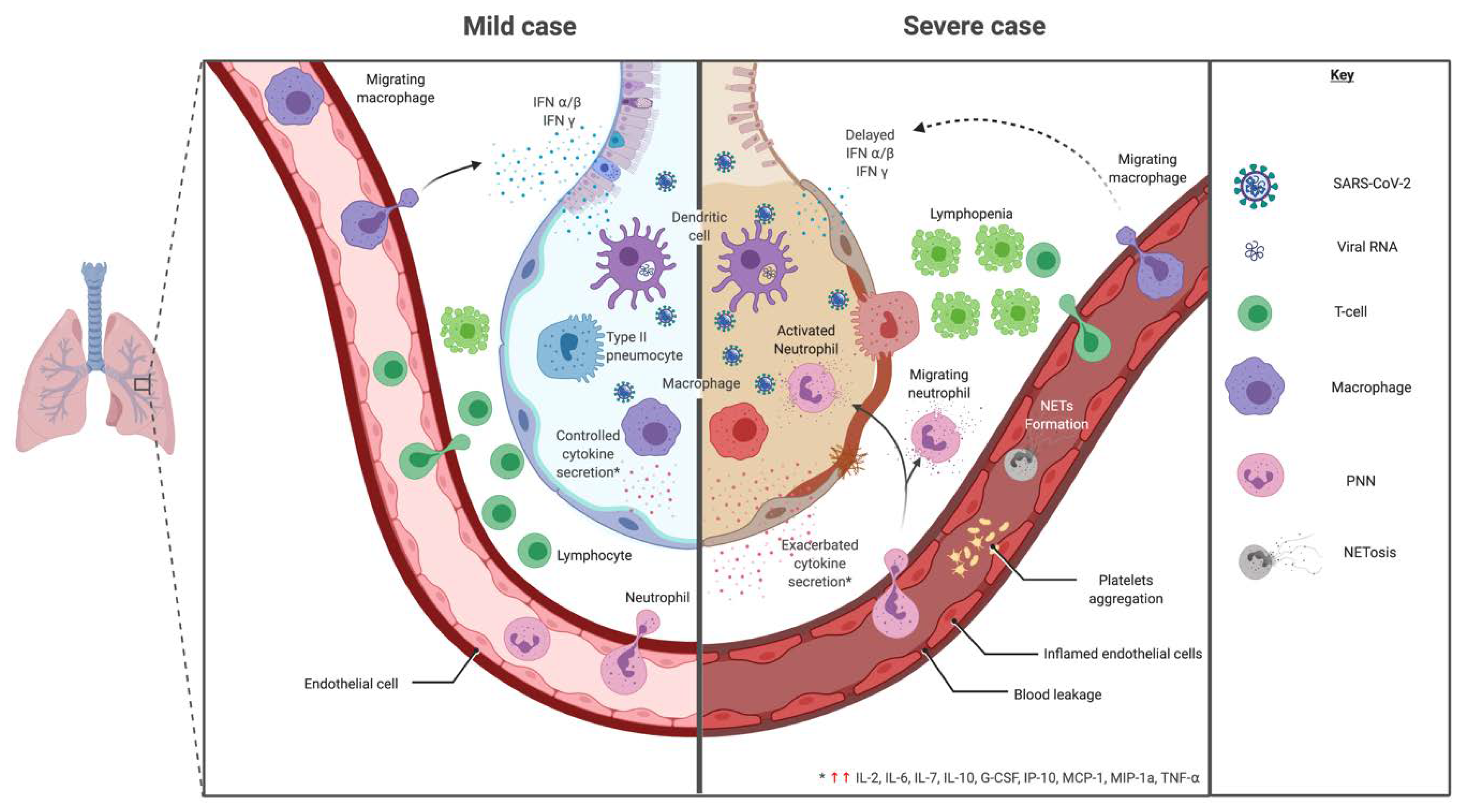 The severity of the inflammation can be attributed to the severity of what is known as the
The severity of the inflammation can be attributed to the severity of what is known as the cytokine storm
A cytokine storm, also called hypercytokinemia, is a physiological reaction in humans and other animals in which the innate immune system causes an uncontrolled and excessive release of pro-inflammatory signaling molecules called cytokines. Norm ...
.interferon-gamma
Interferon gamma (IFN-γ) is a dimerized soluble cytokine that is the only member of the type II class of interferons. The existence of this interferon, which early in its history was known as immune interferon, was described by E. F. Wheelock ...
, interferon-inducible protein 10, and monocyte chemoattractant protein1 were all associated with COVID‑19 disease severity. Treatment has been proposed to combat the cytokine storm as it remains to be one of the leading causes of morbidity
A disease is a particular abnormal condition that negatively affects the structure or function of all or part of an organism, and that is not immediately due to any external injury. Diseases are often known to be medical conditions that a ...
and mortality in COVID‑19 disease.
A cytokine storm is due to an acute hyperinflammatory response that is responsible for clinical illness in an array of diseases but in COVID‑19, it is related to worse prognosis and increased fatality. The storm causes acute respiratory distress syndrome, blood clotting events such as strokes, myocardial infarction, encephalitis
Encephalitis is inflammation of the brain. The severity can be variable with symptoms including reduction or alteration in consciousness, headache, fever, confusion, a stiff neck, and vomiting. Complications may include seizures, hallucinations, ...
, acute kidney injury
Acute kidney injury (AKI), previously called acute renal failure (ARF), is a sudden decrease in kidney function that develops within 7 days, as shown by an increase in serum creatinine or a decrease in urine output, or both.
Causes of AKI are cla ...
, and vasculitis
Vasculitis is a group of disorders that destroy blood vessels by inflammation. Both arteries and veins are affected. Lymphangitis (inflammation of lymphatic vessels) is sometimes considered a type of vasculitis. Vasculitis is primarily caused b ...
. The production of IL-1, IL-2
The Ilyushin Il-2 (Russian: Илью́шин Ил-2) is a ground-attack plane that was produced by the Soviet Union in large numbers during the Second World War. The word ''shturmovík'' ( Cyrillic: штурмовик), the generic Russian term ...
, IL-6, TNF-alpha
Tumor necrosis factor (TNF, cachexin, or cachectin; formerly known as tumor necrosis factor alpha or TNF-α) is an adipokine and a cytokine. TNF is a member of the TNF superfamily, which consists of various transmembrane proteins with a homolog ...
, and interferon-gamma
Interferon gamma (IFN-γ) is a dimerized soluble cytokine that is the only member of the type II class of interferons. The existence of this interferon, which early in its history was known as immune interferon, was described by E. F. Wheelock ...
, all crucial components of normal immune responses, inadvertently become the causes of a cytokine storm. The cells of the central nervous system
The central nervous system (CNS) is the part of the nervous system consisting primarily of the brain and spinal cord. The CNS is so named because the brain integrates the received information and coordinates and influences the activity of all par ...
, the microglia, neuron
A neuron, neurone, or nerve cell is an electrically excitable cell that communicates with other cells via specialized connections called synapses. The neuron is the main component of nervous tissue in all animals except sponges and placozoa. N ...
s, and astrocyte
Astrocytes (from Ancient Greek , , "star" + , , "cavity", "cell"), also known collectively as astroglia, are characteristic star-shaped glial cells in the brain and spinal cord. They perform many functions, including biochemical control of e ...
s, are also involved in the release of pro-inflammatory cytokine An inflammatory cytokine or proinflammatory cytokine is a type of signaling molecule (a cytokine) that is secreted from immune cells like helper T cells (Th) and macrophages, and certain other cell types that promote inflammation. They include in ...
s affecting the nervous system, and effects of cytokine storms toward the CNS are not uncommon.
Pregnancy response
There are many unknowns for pregnant women during the COVID-19 pandemic. Given that they are prone to have complications and severe disease infection with other types of coronaviruses, they have been identified as a vulnerable group and advised to take supplementary preventive measures.vaccinated
A vaccine is a biological preparation that provides active acquired immunity to a particular infectious or malignant disease. The safety and effectiveness of vaccines has been widely studied and verified.[< ...]
.
Diagnosis
COVID‑19 can provisionally be diagnosed on the basis of symptoms and confirmed using reverse transcription polymerase chain reaction
Reverse transcription polymerase chain reaction (RT-PCR) is a laboratory technique combining reverse transcription of RNA into DNA (in this context called complementary DNA or cDNA) and amplification of specific DNA targets using polymerase cha ...
(RT-PCR) or other nucleic acid
Nucleic acids are biopolymers, macromolecules, essential to all known forms of life. They are composed of nucleotides, which are the monomers made of three components: a 5-carbon sugar, a phosphate group and a nitrogenous base. The two main cl ...
testing of infected secretions.antibodies
An antibody (Ab), also known as an immunoglobulin (Ig), is a large, Y-shaped protein used by the immune system to identify and neutralize foreign objects such as pathogenic bacteria and viruses. The antibody recognizes a unique molecule of the ...
produced by the body in response to the infection.
Viral testing
The standard methods of testing for presence of SARS-CoV-2 are nucleic acid test
A nucleic acid test (NAT) is a technique used to detect a particular nucleic acid sequence and thus usually to detect and identify a particular species or subspecies of organism, often a virus or bacterium that acts as a pathogen in blood, tissu ...
s,nasopharyngeal swab
A nasopharyngeal swab is a device used for collecting a sample of nasal secretions from the back of the nose and throat. The sample is then analyzed for the presence of organisms or other clinical markers for disease. This diagnostic method is c ...
; however, a nasal swab or sputum sample may also be used.Public Health England
Public Health England (PHE) was an executive agency of the Department of Health and Social Care in England which began operating on 1 April 2013 to protect and improve health and wellbeing and reduce health inequalities. Its formation came as a ...
and approved for use in the UK.University of Oxford
, mottoeng = The Lord is my light
, established =
, endowment = £6.1 billion (including colleges) (2019)
, budget = £2.145 billion (2019–20)
, chancellor ...
's CEBM has pointed to mounting evidence
Imaging
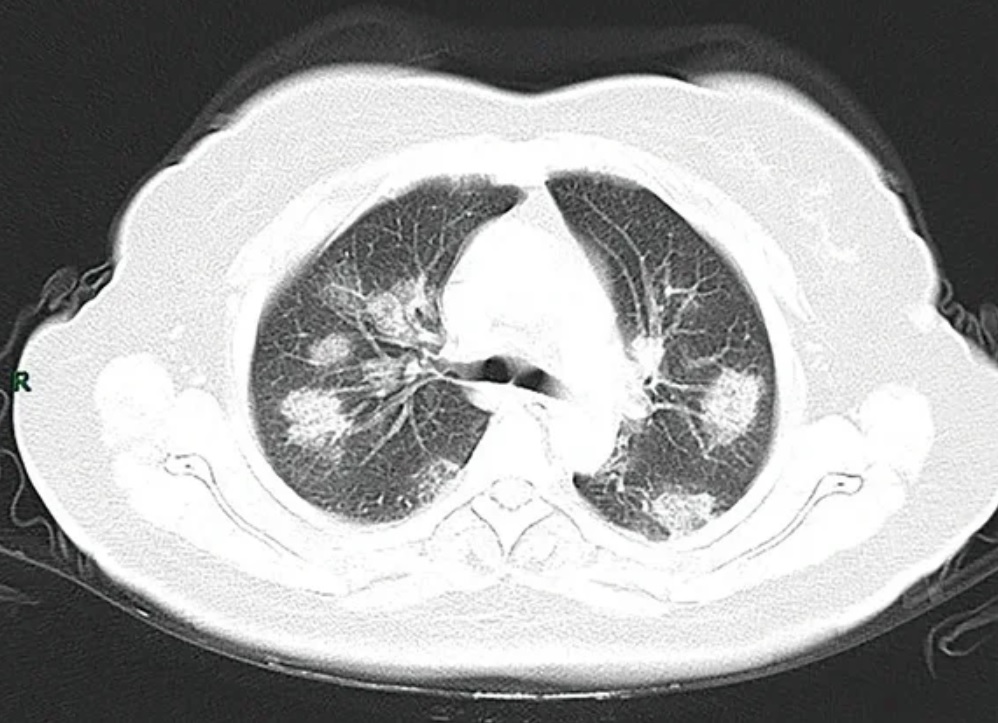

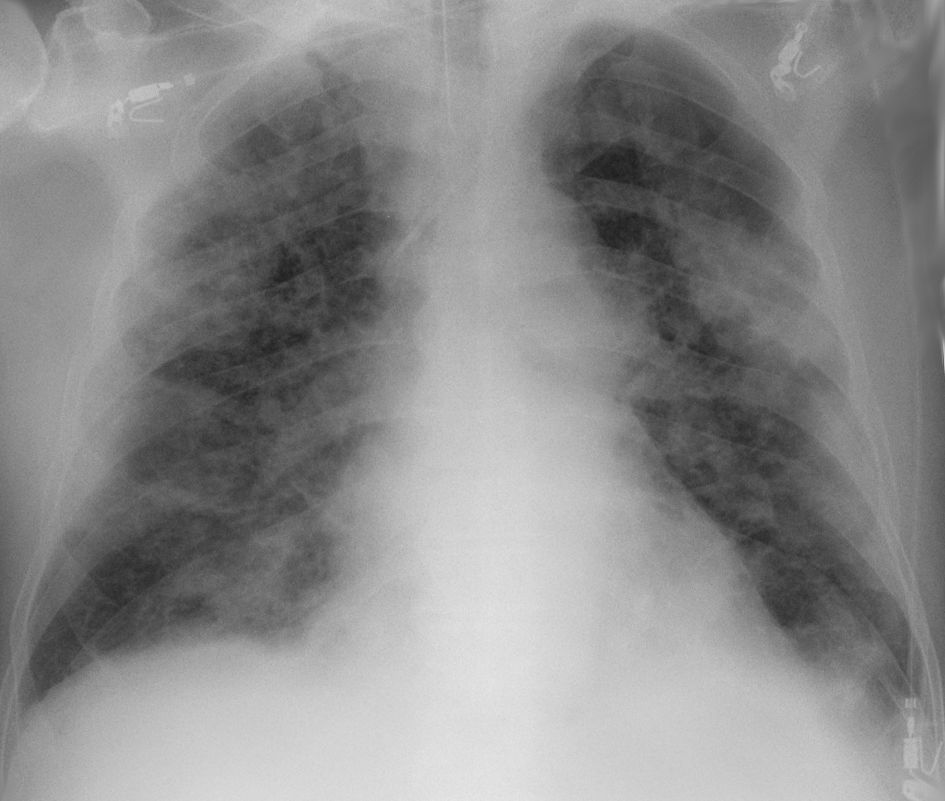 Chest CT scans may be helpful to diagnose COVID‑19 in individuals with a high clinical suspicion of infection but are not recommended for routine screening.
Chest CT scans may be helpful to diagnose COVID‑19 in individuals with a high clinical suspicion of infection but are not recommended for routine screening.ground-glass opacities
Ground-glass opacity (GGO) is a finding seen on chest x-ray (radiograph) or computed tomography (CT) imaging of the lungs. It is typically defined as an area of hazy opacification (x-ray) or increased attenuation (CT) due to air displacement ...
with a peripheral, asymmetric, and posterior distribution are common in early infection.crazy paving
Crazy paving is a means of hard-surfacing used outdoors, most frequently in gardens. Paving stones of irregular size and shape are laid in a haphazard manner sometimes with mortar filling the gaps between.
The method originated in ancient R ...
(lobular septal thickening with variable alveolar filling), and consolidation may appear as the disease progresses.radiographs
Radiography is an imaging technique using X-rays, gamma rays, or similar ionizing radiation and non-ionizing radiation to view the internal form of an object. Applications of radiography include medical radiography ("diagnostic" and "therapeut ...
and computed tomography (CT) of people who are symptomatic include asymmetric peripheral ground-glass opacities without pleural effusion
A pleural effusion is accumulation of excessive fluid in the pleural space, the potential space that surrounds each lung.
Under normal conditions, pleural fluid is secreted by the parietal pleural capillaries at a rate of 0.6 millilitre per kilog ...
s.adenovirus
Adenoviruses (members of the family ''Adenoviridae'') are medium-sized (90–100 nm), nonenveloped (without an outer lipid bilayer) viruses with an icosahedral nucleocapsid containing a double-stranded DNA genome. Their name derives from the ...
, imaging without confirmation by rRT-PCR is of limited specificity in identifying COVID‑19.
Coding
In late 2019, the WHO assigned emergency ICD-10
ICD-10 is the 10th revision of the International Statistical Classification of Diseases and Related Health Problems (ICD), a medical classification list by the World Health Organization (WHO). It contains codes for diseases, signs and symptoms, ...
disease codes U07.1 for deaths from lab-confirmed SARS-CoV-2 infection and U07.2 for deaths from clinically or epidemiologically diagnosed COVID‑19 without lab-confirmed SARS-CoV-2 infection.
Pathology
The main pathological findings at autopsy are:
* Macroscopy: pericarditis
Pericarditis is inflammation of the pericardium, the fibrous sac surrounding the heart. Symptoms typically include sudden onset of sharp chest pain, which may also be felt in the shoulders, neck, or back. The pain is typically less severe when sit ...
, lung consolidation
A pulmonary consolidation is a region of normally compressible lung tissue that has filled with liquid instead of air. The condition is marked by induration (swelling or hardening of normally soft tissue) of a normally aerated lung. It is conside ...
and pulmonary oedema
Pulmonary edema, also known as pulmonary congestion, is excessive liquid accumulation in the tissue and air spaces (usually alveoli) of the lungs. It leads to impaired gas exchange and may cause hypoxemia and respiratory failure. It is due to ...
exudation
An exudate is a fluid emitted by an organism through pores or a wound, a process known as exuding or exudation.
''Exudate'' is derived from ''exude'' 'to ooze' from Latin ''exsūdāre'' 'to (ooze out) sweat' (''ex-'' 'out' and ''sūdāre'' 'to ...
, minor fibrin
Fibrin (also called Factor Ia) is a fibrous, non-globular protein involved in the clotting of blood. It is formed by the action of the protease thrombin on fibrinogen, which causes it to polymerize. The polymerized fibrin, together with platele ...
exudationhyperplasia
Hyperplasia (from ancient Greek ὑπέρ ''huper'' 'over' + πλάσις ''plasis'' 'formation'), or hypergenesis, is an enlargement of an organ or tissue caused by an increase in the amount of organic tissue that results from cell proliferati ...
, large atypical pneumocytes, interstitial inflammation
Inflammation (from la, wikt:en:inflammatio#Latin, inflammatio) is part of the complex biological response of body tissues to harmful stimuli, such as pathogens, damaged cells, or Irritation, irritants, and is a protective response involving im ...
with lymphocytic
A lymphocyte is a type of white blood cell (leukocyte) in the immune system of gnathostomata, most vertebrates. Lymphocytes include natural killer cells (which function in cell-mediated immunity, cell-mediated, cytotoxicity, cytotoxic innate imm ...
infiltration
Infiltration may refer to:
Science, medicine, and engineering
*Infiltration (hydrology), downward movement of water into soil
*Infiltration (HVAC), a heating, ventilation, and air conditioning term for air leakage into buildings
*Infiltration (me ...
and multinucleated giant cell formationalveolar Alveolus (; pl. alveoli, adj. alveolar) is a general anatomical term for a concave cavity or pit.
Uses in anatomy and zoology
* Pulmonary alveolus, an air sac in the lungs
** Alveolar cell or pneumocyte
** Alveolar duct
** Alveolar macrophage
* ...
exudates
An exudate is a fluid emitted by an organism through pores or a wound, a process known as exuding or exudation.
''Exudate'' is derived from ''exude'' 'to ooze' from Latin ''exsūdāre'' 'to (ooze out) sweat' (''ex-'' 'out' and ''sūdāre'' 'to ...
. DAD is the cause of acute respiratory distress syndrome
Acute respiratory distress syndrome (ARDS) is a type of respiratory failure characterized by rapid onset of widespread inflammation in the lungs. Symptoms include shortness of breath (dyspnea), rapid breathing (tachypnea), and bluish skin colo ...
(ARDS) and severe hypoxaemia
Hypoxemia is an abnormally low level of oxygen in the blood. More specifically, it is oxygen deficiency in artery, arterial blood. Hypoxemia has many causes, and often causes Hypoxia (medical), hypoxia as the blood is not supplying enough oxygen ...
.organisation
An organization or organisation (Commonwealth English; see spelling differences), is an entity—such as a company, an institution, or an association—comprising one or more people and having a particular purpose.
The word is derived from ...
of exudate
An exudate is a fluid emitted by an organism through pores or a wound, a process known as exuding or exudation.
''Exudate'' is derived from ''exude'' 'to ooze' from Latin ''exsūdāre'' 'to (ooze out) sweat' (''ex-'' 'out' and ''sūdāre'' 'to ...
s in alveolar cavities and pulmonary interstitial fibrosisBAL
Bal may refer to:
* Bal (surname), a Dutch, Indian, and Turkish surname
* Bal, Iran (disambiguation)
* Bal, Zira, a village in Punjab, India
* ''Bal'' (film), a 2010 Turkish film
* Bäl, a settlement on the Swedish island of Gotland
* 8678 Bä ...
* Blood and vessels: disseminated intravascular coagulation (DIC); leukoerythroblastic reaction, endotheliitis Endotheliitis is an immune response within the endothelium in blood vessels, in which they become inflamed. The condition can cause oedema of the surrounding tissue, including the stroma, and can cause irritation and pain. If it is within the corn ...
,hemophagocytosis
Hemophagocytosis is phagocytosis by histiocytes of erythrocytes, leukocytes, platelets, and their precursors in bone marrow and other tissues.
It is part of the presentation of hemophagocytic lymphohistiocytosis
Hemophagocytic lymphohistiocyto ...
cardiac muscle cell
Cardiac muscle (also called heart muscle, myocardium, cardiomyocytes and cardiac myocytes) is one of three types of vertebrate muscle tissues, with the other two being skeletal muscle and smooth muscle. It is an involuntary, striated muscle th ...
necrosissteatosis
Steatosis, also called fatty change, is abnormal retention of fat (lipids) within a cell or organ. Steatosis most often affects the liver – the primary organ of lipid metabolism – where the condition is commonly referred to as fatty liver disea ...
infarction
Infarction is tissue death (necrosis) due to inadequate blood supply to the affected area. It may be caused by artery blockages, rupture, mechanical compression, or vasoconstriction. The resulting lesion is referred to as an infarct
(from the ...
white pulp
White pulp is a histological designation for regions of the spleen (named because it appears whiter than the surrounding red pulp on gross section), that encompasses approximately 25% of splenic tissue. White pulp consists entirely of lymphoid ti ...
depletion.
Prevention
 Preventive measures to reduce the chances of infection include getting vaccinated, staying at home, wearing a mask in public, avoiding crowded places, keeping distance from others, ventilating indoor spaces, managing potential exposure durations, washing hands with soap and water often and for at least twenty seconds, practising good respiratory hygiene, and avoiding touching the eyes, nose, or mouth with unwashed hands.
Preventive measures to reduce the chances of infection include getting vaccinated, staying at home, wearing a mask in public, avoiding crowded places, keeping distance from others, ventilating indoor spaces, managing potential exposure durations, washing hands with soap and water often and for at least twenty seconds, practising good respiratory hygiene, and avoiding touching the eyes, nose, or mouth with unwashed hands.COVID‑19 vaccine
A COVID19 vaccine is a vaccine intended to provide acquired immunity against severe acute respiratory syndrome coronavirus 2 (SARS‑CoV‑2), the virus that causes coronavirus disease 2019 (COVID19).
Prior to the COVID19 pandemic, an esta ...
was granted regulatory approval on 2December 2020 by the UK medicines regulator MHRA.emergency use authorization
An Emergency Use Authorization (EUA) in the United States is an authorization granted to the Food and Drug Administration (FDA) under sections of the Federal Food, Drug, and Cosmetic Act as added to and amended by various Act of Congress, Acts of ...
(EUA) status by the US FDA
The United States Food and Drug Administration (FDA or US FDA) is a federal agency of the Department of Health and Human Services. The FDA is responsible for protecting and promoting public health through the control and supervision of food ...
, and in several other countries.National Institutes of Health
The National Institutes of Health, commonly referred to as NIH (with each letter pronounced individually), is the primary agency of the United States government responsible for biomedical and public health research. It was founded in the late ...
guidelines do not recommend any medication for prevention of COVID‑19, before or after exposure to the SARS-CoV-2 virus, outside the setting of a clinical trial.curve
In mathematics, a curve (also called a curved line in older texts) is an object similar to a line (geometry), line, but that does not have to be Linearity, straight.
Intuitively, a curve may be thought of as the trace left by a moving point (ge ...
".
Vaccine

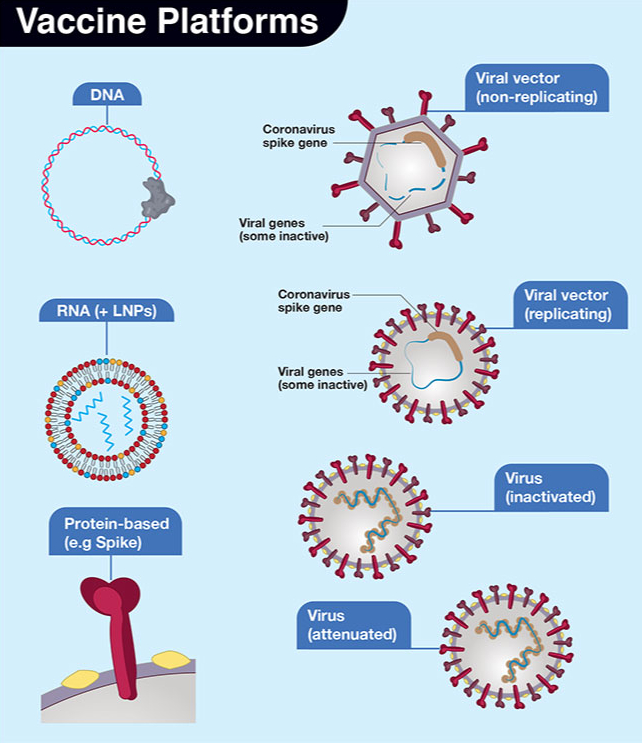
Face masks and respiratory hygiene
 The WHO and the US CDC recommend individuals wear non-medical face coverings in public settings where there is an increased risk of transmission and where social distancing measures are difficult to maintain.
The WHO and the US CDC recommend individuals wear non-medical face coverings in public settings where there is an increased risk of transmission and where social distancing measures are difficult to maintain.respirator
A respirator is a device designed to protect the wearer from inhaling hazardous atmospheres including fumes, vapours, gases and particulate matter such as dusts and airborne pathogens such as viruses. There are two main categories of respi ...
s at least as protective as NIOSH
The National Institute for Occupational Safety and Health (NIOSH, ) is the United States federal agency responsible for conducting research and making recommendations for the prevention of work-related injury and illness. NIOSH is part of the C ...
-certified N95 or equivalent, in addition to other personal protective equipment
Personal protective equipment (PPE) is protective clothing, helmets, goggles, or other garments or equipment designed to protect the wearer's body from injury or infection. The hazards addressed by protective equipment include physical, elec ...
.
Indoor ventilation and avoiding crowded indoor spaces
The CDC recommends that crowded indoor spaces should be avoided.ventilation
Ventilation may refer to:
* Ventilation (physiology), the movement of air between the environment and the lungs via inhalation and exhalation
** Mechanical ventilation, in medicine, using artificial methods to assist breathing
*** Ventilator, a m ...
and air filtration
A particulate air filter is a device composed of fibrous, or porous materials which removes solid particulates such as dust, pollen, mold, and bacteria from the air. Filters containing an adsorbent or catalyst such as charcoal (carbon) may also ...
in public spaces to help clear out infectious aerosols.ventilation
Ventilation may refer to:
* Ventilation (physiology), the movement of air between the environment and the lungs via inhalation and exhalation
** Mechanical ventilation, in medicine, using artificial methods to assist breathing
*** Ventilator, a m ...
. The risk of COVID‑19 infection increases especially in spaces where people engage in physical exertion or raise their voice (e.g., exercising, shouting, singing) as this increases exhalation of respiratory droplets. Prolonged exposure to these conditions, typically more than 15 minutes, leads to higher risk of infection.Displacement ventilation Displacement ventilation (DV) It is a room air distribution strategy where conditioned outdoor air is supplied at a low velocity from air supply diffusers located near floor level and extracted above the occupied zone, usually at ceiling height.
S ...
with large natural inlets can move stale air directly to the exhaust in laminar flow
In fluid dynamics, laminar flow is characterized by fluid particles following smooth paths in layers, with each layer moving smoothly past the adjacent layers with little or no mixing. At low velocities, the fluid tends to flow without lateral mi ...
while significantly reducing the concentration of droplets and particles. Passive ventilation
Passive ventilation is the process of supplying air to and removing air from an indoor space without using mechanical systems. It refers to the flow of external air to an indoor space as a result of pressure differences arising from natural forces ...
reduces energy consumption and maintenance costs but may lack controllability Controllability is an important property of a control system, and the controllability property plays a crucial role in many control problems, such as stabilization of unstable systems by feedback, or optimal control.
Controllability and observabil ...
and heat recovery
Heat recovery ventilation (HRV), also known as mechanical ventilation heat recovery (MVHR), is an energy recovery ventilation system which works between two air sources at different temperatures. Heat recovery is a method which is used to reduce ...
. Displacement ventilation can also be achieved mechanically with higher energy and maintenance costs. The use of large ducts and openings helps to prevent mixing in closed environments. Recirculation and mixing should be avoided because recirculation prevents dilution of harmful particles and redistributes possibly contaminated air, and mixing increases the concentration and range of infectious particles and keeps larger particles in the air.
Hand-washing and hygiene
 Thorough hand hygiene after any cough or sneeze is required.
Thorough hand hygiene after any cough or sneeze is required.hand sanitiser
Hand sanitizer (also known as hand antiseptic, hand disinfectant, hand rub, or handrub) is a liquid, gel or foam generally used to kill many viruses/bacteria/microorganisms on the hands. In most settings, hand washing with soap and water is gen ...
with at least 60% alcohol. For areas where commercial hand sanitisers are not readily available, the WHO provides two formulations for local production. In these formulations, the antimicrobial activity arises from ethanol
Ethanol (abbr. EtOH; also called ethyl alcohol, grain alcohol, drinking alcohol, or simply alcohol) is an organic compound. It is an Alcohol (chemistry), alcohol with the chemical formula . Its formula can be also written as or (an ethyl ...
or isopropanol
Isopropyl alcohol (IUPAC name propan-2-ol and also called isopropanol or 2-propanol) is a colorless, flammable organic compound with a pungent alcoholic odor. As an isopropyl group linked to a hydroxyl group (chemical formula ) it is the simple ...
. Hydrogen peroxide
Hydrogen peroxide is a chemical compound with the formula . In its pure form, it is a very pale blue liquid that is slightly more viscous than water. It is used as an oxidizer, bleaching agent, and antiseptic, usually as a dilute solution (3%� ...
is used to help eliminate bacterial spores
An endospore is a dormant, tough, and non-reproductive structure produced by some bacteria in the phylum Bacillota. The name "endospore" is suggestive of a spore or seed-like form (''endo'' means 'within'), but it is not a true spore (i.e., ...
in the alcohol; it is "not an active substance for hand antisepsis
An antiseptic (from Greek ἀντί ''anti'', "against" and σηπτικός ''sēptikos'', "putrefactive") is an antimicrobial substance or compound that is applied to living tissue/skin to reduce the possibility of infection, sepsis, or putr ...
." Glycerol
Glycerol (), also called glycerine in British English and glycerin in American English, is a simple triol compound. It is a colorless, odorless, viscous liquid that is sweet-tasting and non-toxic. The glycerol backbone is found in lipids known ...
is added as a humectant.
Social distancing
Social distancing (also known as physical distancing) includes infection control
Infection prevention and control is the discipline concerned with preventing healthcare-associated infections; a practical rather than academic sub-discipline of epidemiology. In Northern Europe, infection prevention and control is expanded from ...
actions intended to slow the spread of the disease by minimising close contact between individuals. Methods include quarantines; travel restrictions; and the closing of schools, workplaces, stadiums, theatres, or shopping centres. Individuals may apply social distancing methods by staying at home, limiting travel, avoiding crowded areas, using no-contact greetings, and physically distancing themselves from others. Many governments are mandating or recommending social distancing in regions affected by the outbreak.
Surface cleaning
After being expelled from the body, coronaviruses can survive on surfaces for hours to days. If a person touches the dirty surface, they may deposit the virus at the eyes, nose, or mouth where it can enter the body and cause infection.antimicrobial resistance
Antimicrobial resistance (AMR) occurs when microbes evolve mechanisms that protect them from the effects of antimicrobials. All classes of microbes can evolve resistance. Fungi evolve antifungal resistance. Viruses evolve antiviral resistance. ...
through the use of inappropriate cleaning products and processes.UV light
Ultraviolet (UV) is a form of electromagnetic radiation with wavelength from 10 nm (with a corresponding frequency around 30 PHz) to 400 nm (750 THz), shorter than that of visible light, but longer than X-rays. UV radiation i ...
in sunlight
Sunlight is a portion of the electromagnetic radiation given off by the Sun, in particular infrared, visible, and ultraviolet light. On Earth, sunlight is scattered and filtered through Earth's atmosphere, and is obvious as daylight when t ...
.room temperature
Colloquially, "room temperature" is a range of air temperatures that most people prefer for indoor settings. It feels comfortable to a person when they are wearing typical indoor clothing. Human comfort can extend beyond this range depending on ...
or lower, and when the relative humidity
Humidity is the concentration of water vapor present in the air. Water vapor, the gaseous state of water, is generally invisible to the human eye. Humidity indicates the likelihood for precipitation, dew, or fog to be present.
Humidity depe ...
is low (<50%).ethanol
Ethanol (abbr. EtOH; also called ethyl alcohol, grain alcohol, drinking alcohol, or simply alcohol) is an organic compound. It is an Alcohol (chemistry), alcohol with the chemical formula . Its formula can be also written as or (an ethyl ...
, 50–100 per cent isopropanol, 0.1 per cent sodium hypochlorite
Sodium hypochlorite (commonly known in a dilute solution as bleach) is an Inorganic chemistry, inorganic chemical compound with the chemical formula, formula NaOCl (or NaClO), comprising a sodium cation () and a hypochlorite anion (or ). It may ...
, 0.5 per cent hydrogen peroxide, 0.2–7.5 per cent povidone-iodine
Povidone-iodine (PVP-I), also known as iodopovidone, is an antiseptic used for skin disinfection before and after surgery. It may be used both to disinfect the hands of healthcare providers and the skin of the person they are caring for. It may a ...
, or 50–200 ppm hypochlorous acid
Hypochlorous acid (HClO, HOCl, or ClHO) is a weak acid that forms when chlorine dissolves in water, and itself partially dissociates, forming hypochlorite, ClO−. HClO and ClO− are oxidizers, and the primary disinfection agents of chlorine so ...
. Other solutions, such as benzalkonium chloride
Benzalkonium chloride (BZK, BKC, BAK, BAC), also known as alkyldimethylbenzylammonium chloride (ADBAC) and by the trade name Zephiran, is a type of cationic surfactant. It is an organic salt classified as a quaternary ammonium compound. ADBACs hav ...
and chlorhexidine gluconate
Chlorhexidine (CHX) (commonly known by the salt forms chlorhexidine gluconate and chlorhexidine digluconate (CHG) or chlorhexidine acetate) is a disinfectant and antiseptic that is used for skin disinfection before surgery and to sterilize surgi ...
, are less effective. Ultraviolet germicidal irradiation
Ultraviolet germicidal irradiation (UVGI) is a disinfection method that uses short-wavelength ultraviolet (ultraviolet C or UV-C) light to kill or inactivate microorganisms by destroying nucleic acids and disrupting their DNA, leaving them unabl ...
may also be used,
Self-isolation
Self-isolation
In health care facilities, isolation represents one of several measures that can be taken to implement in infection control: the prevention of communicable diseases from being transmitted from a patient to other patients, health care workers ...
at home has been recommended for those diagnosed with COVID‑19 and those who suspect they have been infected. Health agencies have issued detailed instructions for proper self-isolation.
International travel-related control measures
A 2021 Cochrane rapid review found that based upon low-certainty evidence, international travel-related control measures such as restricting cross-border travel may help to contain the spread of COVID‑19.
Treatment

Prognosis and risk factors
The severity of COVID‑19 varies. The disease may take a mild course with few or no symptoms, resembling other common upper respiratory diseases such as the common cold
The common cold or the cold is a viral infectious disease of the upper respiratory tract that primarily affects the respiratory mucosa of the nose, throat, sinuses, and larynx. Signs and symptoms may appear fewer than two days after exposu ...
. In 3–4% of cases (7.4% for those over age 65) symptoms are severe enough to cause hospitalisation.Istituto Superiore di Sanità
The ''Istituto Superiore di Sanità'' (Italian National Institute of Health, literally 'Higher Health Institute'), also ISS, is an Italian public institution that, as the leading technical-scientific body of the Italian National Health Service (' ...
reported that the median time between the onset of symptoms and death was twelve days, with seven being hospitalised. However, people transferred to an ICU had a median time of ten days between hospitalisation and death.prothrombin
Thrombin (, ''fibrinogenase'', ''thrombase'', ''thrombofort'', ''topical'', ''thrombin-C'', ''tropostasin'', ''activated blood-coagulation factor II'', ''blood-coagulation factor IIa'', ''factor IIa'', ''E thrombin'', ''beta-thrombin'', ''gamma- ...
time and elevated C-reactive protein
C-reactive protein (CRP) is an annular (ring-shaped) pentameric protein found in blood plasma, whose circulating concentrations rise in response to inflammation. It is an acute-phase protein of hepatic origin that increases following interleukin-6 ...
levels on admission to the hospital are associated with severe course of COVID‑19 and with a transfer to ICU.
Some early studies suggest 10% to 20% of people with COVID‑19 will experience symptoms lasting longer than a month.Tedros Adhanom
Tedros Adhanom Ghebreyesus ( ti, ቴዎድሮስ አድሓኖም ገብረኢየሱስ, sometimes spelt ti, ቴድሮስ ኣድሓኖም ገብረየሱስ, label=none; born 3 March 1965) is an Ethiopian public health official, researcher, and ...
warned that "to a significant number of people, the COVID virus poses a range of serious long-term effects." He has described the vast spectrum of COVID‑19 symptoms that fluctuate over time as "really concerning". They range from fatigue, a cough and shortness of breath, to inflammation and injury of major organsincluding the lungs and heart, and also neurological and psychologic effects. Symptoms often overlap and can affect any system in the body. Infected people have reported cyclical bouts of fatigue, headaches, months of complete exhaustion, mood swings, and other symptoms. Tedros therefore concluded that a strategy of achieving herd immunity
Herd immunity (also called herd effect, community immunity, population immunity, or mass immunity) is a form of indirect protection that applies only to contagious diseases. It occurs when a sufficient percentage of a population has become imm ...
by infection, rather than vaccination, is "morally unconscionable and unfeasible".scientific review
A review article is an article that summarizes the current state of understanding on a topic within a certain discipline. A review article is generally considered a secondary source since it may analyze and discuss the method and conclusions i ...
s smokers are more likely to require intensive care or die compared to non-smokers.obesity
Obesity is a medical condition, sometimes considered a disease, in which excess body fat has accumulated to such an extent that it may negatively affect health. People are classified as obese when their body mass index (BMI)—a person's we ...
, especially in conjunction with fatty liver disease
Fatty liver disease (FLD), also known as hepatic steatosis, is a condition where excess fat builds up in the liver. Often there are no or few symptoms. Occasionally there may be tiredness or pain in the upper right side of the abdomen. Complicat ...
, contributes to an increased health risk of COVID‑19.hypogonadism
Hypogonadism means diminished functional activity of the gonads—the testes or the ovaries—that may result in diminished production of sex hormones. Low androgen (e.g., testosterone) levels are referred to as hypoandrogenism and low estrogen ...
were 2.4 times more likely than men with eugonadism to be hospitalized if they contracted COVID-19; Hypogonad men treated with testosterone
Testosterone is the primary sex hormone and anabolic steroid in males. In humans, testosterone plays a key role in the development of Male reproductive system, male reproductive tissues such as testes and prostate, as well as promoting secondar ...
were less likely to be hospitalized for COVID-19 than men who were not treated for hypogonadism.
Genetic risk factors
Genetics
Genetics is the study of genes, genetic variation, and heredity in organisms.Hartl D, Jones E (2005) It is an important branch in biology because heredity is vital to organisms' evolution. Gregor Mendel, a Moravian Augustinian friar wor ...
plays an important role in the ability to fight off Covid.type I interferon
The type-I interferons (IFN) are cytokines which play essential roles in inflammation, immunoregulation, tumor cells recognition, and T cell, T-cell responses. In the human genome, a cluster of thirteen functional IFN genes is located at the 9p2 ...
s or produce auto-antibodies
An autoantibody is an antibody (a type of protein) produced by the immune system that is directed against one or more of the individual's own proteins. Many autoimmune diseases (notably lupus erythematosus) are associated with such antibodies.
Pr ...
against these may get much sicker from COVID‑19. Genetic screening
Genetic testing, also known as DNA testing, is used to identify changes in DNA sequence or chromosome structure. Genetic testing can also include measuring the results of genetic changes, such as RNA analysis as an output of gene expression, or ...
is able to detect interferon effector genes. Some genetic variants are risk factors in specific populations. For instance, and allele
An allele (, ; ; modern formation from Greek ἄλλος ''állos'', "other") is a variation of the same sequence of nucleotides at the same place on a long DNA molecule, as described in leading textbooks on genetics and evolution.
::"The chro ...
of the DOCK2 gene (dedicator of cytokinesis 2 gene) is a common risk factor in Asian populations but much less common in Europe. The mutation leads to lower expression of DOCK2 especially in younger patients with severe Covid. In fact, many other genes and genetic variants have been found that determine the outcome of SARS-CoV-2 infections.
Children
While very young children have experienced lower rates of infection, older children have a rate of infection that is similar to the population as a whole. Children are likely to have milder symptoms and are at lower risk of severe disease than adults.
Complications
 Complications may include
Complications may include pneumonia
Pneumonia is an inflammatory condition of the lung primarily affecting the small air sacs known as alveoli. Symptoms typically include some combination of productive or dry cough, chest pain, fever, and difficulty breathing. The severity ...
, acute respiratory distress syndrome
Acute respiratory distress syndrome (ARDS) is a type of respiratory failure characterized by rapid onset of widespread inflammation in the lungs. Symptoms include shortness of breath (dyspnea), rapid breathing (tachypnea), and bluish skin colo ...
(ARDS), multi-organ failure
Multiple organ dysfunction syndrome (MODS) is altered organ function in an acutely ill patient requiring medical intervention to achieve homeostasis.
Although Irwin and Rippe cautioned in 2005 that the use of "multiple organ failure" or "multisy ...
, septic shock
Septic shock is a potentially fatal medical condition that occurs when sepsis, which is organ injury or damage in response to infection, leads to dangerously low blood pressure and abnormalities in cellular metabolism. The Third International Con ...
, and death.arrhythmia
Arrhythmias, also known as cardiac arrhythmias, heart arrhythmias, or dysrhythmias, are irregularities in the heartbeat, including when it is too fast or too slow. A resting heart rate that is too fast – above 100 beats per minute in adults ...
s (including atrial fibrillation), heart inflammation, and thrombosis
Thrombosis (from Ancient Greek "clotting") is the formation of a blood clot inside a blood vessel, obstructing the flow of blood through the circulatory system. When a blood vessel (a vein or an artery) is injured, the body uses platelets (thro ...
, particularly venous thromboembolism
Venous thrombosis is blockage of a vein caused by a thrombus (blood clot). A common form of venous thrombosis is deep vein thrombosis (DVT), when a blood clot forms in the deep veins. If a thrombus breaks off (embolizes) and flows to the lungs to ...
.elevated liver enzymes
In medicine, the presence of elevated transaminases, commonly the transaminases alanine transaminase (ALT) and aspartate transaminase (AST), may be an indicator of liver dysfunction. Other terms include transaminasemia, transaminitis, and elevated ...
, reflecting liver injury.seizure
An epileptic seizure, informally known as a seizure, is a period of symptoms due to abnormally excessive or synchronous neuronal activity in the brain. Outward effects vary from uncontrolled shaking movements involving much of the body with los ...
, stroke, encephalitis
Encephalitis is inflammation of the brain. The severity can be variable with symptoms including reduction or alteration in consciousness, headache, fever, confusion, a stiff neck, and vomiting. Complications may include seizures, hallucinations, ...
, and Guillain–Barré syndrome
Guillain–Barré syndrome (GBS) is a rapid-onset muscle weakness caused by the immune system damaging the peripheral nervous system. Typically, both sides of the body are involved, and the initial symptoms are changes in sensation or pain often ...
(which includes loss of motor functions).paediatric multisystem inflammatory syndrome
Multisystem inflammatory syndrome in children (MIS-C), or paediatric inflammatory multisystem syndrome (PIMS / PIMS-TS), or systemic inflammatory syndrome in COVID-19 (SISCoV), is a rare systemic illness involving persistent fever and extreme i ...
, which has symptoms similar to Kawasaki disease
Kawasaki disease is a syndrome of unknown cause that results in a fever and mainly affects children under 5 years of age. It is a form of vasculitis, where blood vessels become inflamed throughout the body. The fever typically lasts for more tha ...
, which can be fatal. In very rare cases, acute encephalopathy
Encephalopathy (; from grc, ἐνκέφαλος "brain" + πάθος "suffering") means any disorder or disease of the brain, especially chronic degenerative conditions. In modern usage, encephalopathy does not refer to a single disease, but r ...
can occur, and it can be considered in those who have been diagnosed with COVID‑19 and have an altered mental status.
In the case of pregnant women, it is important to note that, according to the US Centers for Disease Control and Prevention
The Centers for Disease Control and Prevention (CDC) is the national public health agency of the United States. It is a United States federal agency, under the Department of Health and Human Services, and is headquartered in Atlanta, Georgi ...
, pregnant women are at increased risk of becoming seriously ill from COVID‑19.miscarriage
Miscarriage, also known in medical terms as a spontaneous abortion and pregnancy loss, is the death of an embryo or fetus before it is able to survive independently. Miscarriage before 6 weeks of gestation is defined by ESHRE as biochemical lo ...
, premature delivery
Preterm birth, also known as premature birth, is the birth of a baby at fewer than 37 weeks gestational age, as opposed to full-term delivery at approximately 40 weeks. Extreme preterm is less than 28 weeks, very early preterm birth is between 2 ...
and intrauterine growth restriction
Intrauterine growth restriction (IUGR), or fetal growth restriction, refers to poor growth of a fetus while in the womb during pregnancy. IUGR is defined by clinical features of malnutrition and evidence of reduced growth regardless of an infant's ...
.aspergillosis
Aspergillosis is a fungal infection of usually the lungs, caused by the genus ''Aspergillus'', a common mould that is breathed in frequently from the air around, but does not usually affect most people. It generally occurs in people with lung di ...
, candidiasis
Candidiasis is a fungal infection due to any type of '' Candida'' (a type of yeast). When it affects the mouth, in some countries it is commonly called thrush. Signs and symptoms include white patches on the tongue or other areas of the mouth ...
, cryptococcosis
Cryptococcosis is a potentially fatal fungal infection of mainly the lungs, presenting as a pneumonia, and brain, where it appears as a meningitis. Cough, difficulty breathing, chest pain and fever are seen when the lungs are infected. When the ...
and mucormycosis
Mucormycosis, also known as black fungus, is a serious fungal infection that comes under fulminant fungal sinusitis, usually in people who are immunocompromised. It is curable only when diagnosed early. Symptoms depend on where in the body the ...
have been recorded in patients recovering from COVID‑19.
Longer-term effects
Some early studies suggest that 10–20% of people with COVID‑19 will experience symptoms lasting longer than a month.pulmonary fibrosis
Pulmonary fibrosis is a condition in which the lungs become scarred over time. Symptoms include shortness of breath, a dry cough, feeling tired, weight loss, and nail clubbing. Complications may include pulmonary hypertension, respiratory failu ...
or reduced lung function as measured by DLCO DLCO or TLCO ( diffusing capacity or transfer factor of the lung for carbon monoxide (CO),) is the extent to which oxygen passes from the air sacs of the lungs into the blood. Commonly, it refers to the test used to determine this parameter. It was ...
, even in asymptomatic people, but with the suggestion of continuing improvement with the passing of more time.cognitive deficit
Cognitive deficit is an inclusive term to describe any characteristic that acts as a barrier to the cognition process.
The term may describe
* deficits in overall intelligence (as with intellectual disabilities),
* specific and restricted defici ...
, dementia
Dementia is a disorder which manifests as a set of related symptoms, which usually surfaces when the brain is damaged by injury or disease. The symptoms involve progressive impairments in memory, thinking, and behavior, which negatively affe ...
, psychotic disorders, and epilepsy
Epilepsy is a group of non-communicable neurological disorders characterized by recurrent epileptic seizures. Epileptic seizures can vary from brief and nearly undetectable periods to long periods of vigorous shaking due to abnormal electrical ...
or seizures persists at an increased level two years after infection.
Immunity
 The
The immune response
An immune response is a reaction which occurs within an organism for the purpose of defending against foreign invaders. These invaders include a wide variety of different microorganisms including viruses, bacteria, parasites, and fungi which could ...
by humans to SARS-CoV-2 virus occurs as a combination of the cell-mediated immunity
Cell-mediated immunity or cellular immunity is an immune response that does not involve antibodies. Rather, cell-mediated immunity is the activation of phagocytes, antigen-specific cytotoxic T-lymphocytes, and the release of various cytokines in ...
and antibody production, just as with most other infections. B cells interact with T cells and begin dividing before selection into the plasma cell, partly on the basis of their affinity for antigen. Since SARS-CoV-2 has been in the human population only since December 2019, it remains unknown if the immunity
Immunity may refer to:
Medicine
* Immunity (medical), resistance of an organism to infection or disease
* ''Immunity'' (journal), a scientific journal published by Cell Press
Biology
* Immune system
Engineering
* Radiofrequence immunity desc ...
is long-lasting in people who recover from the disease.Omicron variant
Omicron (B.1.1.529) is a variant of SARS-CoV-2 first reported to the World Health Organization (WHO) by the Network for Genomics Surveillance in South Africa on 24 November 2021. It was first detected in Botswana and has spread to become the ...
, as of 2022, reinfections have become common, albeit it is unclear how common.
Mortality
Several measures are commonly used to quantify mortality. These numbers vary by region and over time and are influenced by the volume of testing, healthcare system quality, treatment options, time since the initial outbreak, and population characteristics such as age, sex, and overall health.
The mortality rate
Mortality rate, or death rate, is a measure of the number of deaths (in general, or due to a specific cause) in a particular population, scaled to the size of that population, per unit of time. Mortality rate is typically expressed in units of de ...
reflects the number of deaths within a specific demographic group divided by the population of that demographic group. Consequently, the mortality rate reflects the prevalence as well as the severity of the disease within a given population. Mortality rates are highly correlated to age, with relatively low rates for young people and relatively high rates among the elderly.
Case fatality rate
The case fatality rate
In epidemiology, case fatality rate (CFR) – or sometimes more accurately case-fatality risk – is the proportion of people diagnosed with a certain disease, who end up dying of it. Unlike a disease's mortality rate, the CFR does not take int ...
(CFR) reflects the number of deaths divided by the number of diagnosed cases within a given time interval. Based on Johns Hopkins University statistics, the global death-to-case ratio is (/) as of . The number varies by region.
Cumulative confirmed COVID-19 cases.svg, Total confirmed cases over time
World map of total confirmed COVID-19 cases per million people.svg, Total confirmed cases of COVID‑19 per million people
Daily and total confirmed COVID-19 deaths, World.svg, Total deaths over time
World map of total confirmed COVID-19 deaths per million people by country.svg, Total confirmed deaths due to COVID‑19 per million people
Infection fatality rate
A key metric in gauging the severity of COVID‑19 is the infection fatality rate
In epidemiology, case fatality rate (CFR) – or sometimes more accurately case-fatality risk – is the proportion of people diagnosed with a certain disease, who end up dying of it. Unlike a disease's mortality rate, the CFR does not take int ...
(IFR), also referred to as the ''infection fatality ratio'' or ''infection fatality risk''. This metric is calculated by dividing the total number of deaths from the disease by the total number of infected individuals; hence, in contrast to the CFR, the IFR incorporates asymptomatic and undiagnosed infections as well as reported cases.
Estimates
 A December 2020 systematic review and meta-analysis estimated that population IFR during the first wave of the pandemic was about 0.5% to 1% in many locations (including France, Netherlands, New Zealand, and Portugal), 1% to 2% in other locations (Australia, England, Lithuania, and Spain), and exceeded 2% in Italy.
A December 2020 systematic review and meta-analysis estimated that population IFR during the first wave of the pandemic was about 0.5% to 1% in many locations (including France, Netherlands, New Zealand, and Portugal), 1% to 2% in other locations (Australia, England, Lithuania, and Spain), and exceeded 2% in Italy.[ ] Text was copied from this source, which is available under
Text was copied from this source, which is available under
Creative Commons Attribution 4.0 International License
That study also found that most of these differences in IFR reflected corresponding differences in the age composition of the population and age-specific infection rates; in particular, the metaregression estimate of IFR is very low for children and younger adults (e.g., 0.002% at age 10 and 0.01% at age 25) but increases progressively to 0.4% at age 55, 1.4% at age 65, 4.6% at age 75, and 15% at age 85.
Earlier estimates of IFR
At an early stage of the pandemic, the World Health Organization reported estimates of IFR between 0.3% and 1%. On 2July, The WHO's chief scientist reported that the average IFR estimate presented at a two-day WHO expert forum was about 0.6%.Centers for Disease Control and Prevention
The Centers for Disease Control and Prevention (CDC) is the national public health agency of the United States. It is a United States federal agency, under the Department of Health and Human Services, and is headquartered in Atlanta, Georgi ...
(CDC) reported preliminary estimates of age-specific IFRs for public health planning purposes.
Sex differences
COVID‑19 case fatality rate
In epidemiology, case fatality rate (CFR) – or sometimes more accurately case-fatality risk – is the proportion of people diagnosed with a certain disease, who end up dying of it. Unlike a disease's mortality rate, the CFR does not take int ...
s are higher among men than women in most countries. However, in a few countries like India, Nepal, Vietnam, and Slovenia the fatality cases are higher in women than men.Chinese Center for Disease Control and Prevention
The Chinese Center for Disease Control and Prevention (CCDC; ) is an institution directly under the National Health Commission, based in Changping District, Beijing, China.
Established in 1983, it works to protect public health and safety ...
reported the death rate was 2.8% for men and 1.7% for women.
Ethnic differences
In the US, a greater proportion of deaths due to COVID‑19 have occurred among African Americans and other minority groups.health insurance
Health insurance or medical insurance (also known as medical aid in South Africa) is a type of insurance that covers the whole or a part of the risk of a person incurring medical expenses. As with other types of insurance, risk is shared among ma ...
and care of underlying conditions such as diabetes
Diabetes, also known as diabetes mellitus, is a group of metabolic disorders characterized by a high blood sugar level ( hyperglycemia) over a prolonged period of time. Symptoms often include frequent urination, increased thirst and increased ap ...
,heart disease
Cardiovascular disease (CVD) is a class of diseases that involve the heart or blood vessels. CVD includes coronary artery diseases (CAD) such as angina and myocardial infarction (commonly known as a heart attack). Other CVDs include stroke, hea ...
also increase their risk of death. Similar issues affect Native American and Latino
Latino or Latinos most often refers to:
* Latino (demonym), a term used in the United States for people with cultural ties to Latin America
* Hispanic and Latino Americans in the United States
* The people or cultures of Latin America;
** Latin A ...
communities.Black
Black is a color which results from the absence or complete absorption of visible light. It is an achromatic color, without hue, like white and grey. It is often used symbolically or figuratively to represent darkness. Black and white have o ...
, Asian
Asian may refer to:
* Items from or related to the continent of Asia:
** Asian people, people in or descending from Asia
** Asian culture, the culture of the people from Asia
** Asian cuisine, food based on the style of food of the people from Asi ...
, and other ethnic minority background. More severe impacts upon patients including the relative incidence of the necessity of hospitalisation requirements, and vulnerability to the disease has been associated via DNA analysis to be expressed in genetic variants at chromosomal region 3, features that are associated with European Neanderthal
Neanderthals (, also ''Homo neanderthalensis'' and erroneously ''Homo sapiens neanderthalensis''), also written as Neandertals, are an extinct species or subspecies of archaic humans who lived in Eurasia until about 40,000 years ago. While th ...
heritage. That structure imposes greater risks that those affected will develop a more severe form of the disease.Max Planck Institute for Evolutionary Anthropology
The Max Planck Institute for Evolutionary Anthropology (german: Max-Planck-Institut für evolutionäre Anthropologie, shortened to MPI EVA) is a research institute based in Leipzig, Germany, that was founded in 1997. It is part of the Max Plan ...
and the Karolinska Institutet
The Karolinska Institute (KI; sv, Karolinska Institutet; sometimes known as the (Royal) Caroline Institute in English) is a research-led medical university in Solna within the Stockholm urban area of Sweden. The Karolinska Institute is consist ...
.
Comorbidities
Biological
Biology is the scientific study of life. It is a natural science with a broad scope but has several unifying themes that tie it together as a single, coherent field. For instance, all organisms are made up of cells that process hereditary in ...
factors (immune response) and the general behaviour (habits) can strongly determine the consequences of COVID‑19.diabetes mellitus
Diabetes, also known as diabetes mellitus, is a group of metabolic disorders characterized by a high blood sugar level ( hyperglycemia) over a prolonged period of time. Symptoms often include frequent urination, increased thirst and increased ap ...
,cardiovascular disease
Cardiovascular disease (CVD) is a class of diseases that involve the heart or blood vessels. CVD includes coronary artery diseases (CAD) such as angina and myocardial infarction (commonly known as a heart attack). Other CVDs include stroke, h ...
.comorbidity
In medicine, comorbidity - from Latin morbus ("sickness"), co ("together"), -ity (as if - several sicknesses together) - is the presence of one or more additional conditions often wikt:co-occur#Verb, co-occurring (that is, wikt:concomitant#Adjecti ...
with the average person having 3.4 diseases.ischaemic heart disease
Coronary artery disease (CAD), also called coronary heart disease (CHD), ischemic heart disease (IHD), myocardial ischemia, or simply heart disease, involves the reduction of blood flow to the heart muscle due to build-up of atherosclerotic pla ...
(27.6% of deaths), atrial fibrillation (23.1% of deaths) and chronic renal failure
Chronic kidney disease (CKD) is a type of kidney disease in which a gradual loss of kidney function occurs over a period of months to years. Initially generally no symptoms are seen, but later symptoms may include leg swelling, feeling tired, vo ...
(20.2% of deaths).
Most critical respiratory comorbidities according to the US Centers for Disease Control and Prevention
The Centers for Disease Control and Prevention (CDC) is the national public health agency of the United States. It is a United States federal agency, under the Department of Health and Human Services, and is headquartered in Atlanta, Georgi ...
(CDC), are: moderate or severe asthma
Asthma is a long-term inflammatory disease of the airways of the lungs. It is characterized by variable and recurring symptoms, reversible airflow obstruction, and easily triggered bronchospasms. Symptoms include episodes of wheezing, cou ...
, pre-existing COPD
Chronic obstructive pulmonary disease (COPD) is a type of progressive lung disease characterized by long-term respiratory symptoms and airflow limitation. The main symptoms include shortness of breath and a cough, which may or may not produce mu ...
, pulmonary fibrosis
Pulmonary fibrosis is a condition in which the lungs become scarred over time. Symptoms include shortness of breath, a dry cough, feeling tired, weight loss, and nail clubbing. Complications may include pulmonary hypertension, respiratory failu ...
, cystic fibrosis
Cystic fibrosis (CF) is a rare genetic disorder that affects mostly the lungs, but also the pancreas, liver, kidneys, and intestine. Long-term issues include difficulty breathing and coughing up mucus as a result of frequent lung infections. O ...
. Evidence stemming from meta-analysis
A meta-analysis is a statistical analysis that combines the results of multiple scientific studies. Meta-analyses can be performed when there are multiple scientific studies addressing the same question, with each individual study reporting me ...
of several smaller research papers also suggests that smoking can be associated with worse outcomes. When someone with existing respiratory problems is infected with COVID‑19, they might be at greater risk for severe symptoms. COVID‑19 also poses a greater risk to people who misuse opioids and amphetamines
Substituted amphetamines are a class of compounds based upon the amphetamine structure; it includes all derivative compounds which are formed by replacing, or substituting, one or more hydrogen atoms in the amphetamine core structure with sub ...
, insofar as their drug use may have caused lung damage.
In August 2020, the CDC issued a caution that tuberculosis
Tuberculosis (TB) is an infectious disease usually caused by '' Mycobacterium tuberculosis'' (MTB) bacteria. Tuberculosis generally affects the lungs, but it can also affect other parts of the body. Most infections show no symptoms, in ...
(TB) infections could increase the risk of severe illness or death. The WHO recommended that people with respiratory symptoms be screened for both diseases, as testing positive for COVID‑19 could not rule out co-infections. Some projections have estimated that reduced TB detection due to the pandemic could result in 6.3 million additional TB cases and 1.4 million TB-related deaths by 2025.
History
The virus is thought to be of natural animal origin, most likely through spillover infection
Spillover infection, also known as pathogen spillover and spillover event, occurs when a reservoir population with a high pathogen prevalence comes into contact with a novel host population. The pathogen is transmitted from the reservoir population ...
.World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level of h ...
indicated that the virus descended from a coronavirus that infects wild bats, and likely spread to humans through an intermediary wildlife host. There are several theories about where the index case
The index case or patient zero is the first documented patient in a disease epidemic within a population, or the first documented patient included in an epidemiological study.
It can also refer to the first case of a condition or syndrome (not n ...
originated and investigations into the origin of the pandemic are ongoing.Science
Science is a systematic endeavor that builds and organizes knowledge in the form of testable explanations and predictions about the universe.
Science may be as old as the human species, and some of the earliest archeological evidence for ...
, virus transmission into humans occurred through two spillover events in November 2019 and was likely due to live wildlife trade on the Huanan wet market in the city of Wuhan
Wuhan (, ; ; ) is the capital of Hubei, Hubei Province in the China, People's Republic of China. It is the largest city in Hubei and the most populous city in Central China, with a population of over eleven million, the List of cities in China ...
(Hubei, China). Doubts about the conclusions have mostly centred on the precise site of spillover. Earlier phylogenetics
In biology, phylogenetics (; from Greek language, Greek wikt:φυλή, φυλή/wikt:φῦλον, φῦλον [] "tribe, clan, race", and wikt:γενετικός, γενετικός [] "origin, source, birth") is the study of the evolutionary his ...
estimated that SARS-CoV-2 arose in October or November 2019.Guangdong
Guangdong (, ), alternatively romanized as Canton or Kwangtung, is a coastal province in South China on the north shore of the South China Sea. The capital of the province is Guangzhou. With a population of 126.01 million (as of 2020) ...
before Wuhan. U.S intelligence agencies and other scientists have found that the virus may have been unintentionally leaked from a laboratory such as the Wuhan Institute of Virology
The Wuhan Institute of Virology, Chinese Academy of Sciences (WIV; ) is a research institute on virology administered by the Chinese Academy of Sciences (CAS), which reports to the State Council of the People's Republic of China. The institute ...
, but that it was not developed as a biological weapon
A biological agent (also called bio-agent, biological threat agent, biological warfare agent, biological weapon, or bioweapon) is a bacterium, virus, protozoan, parasite, fungus, or toxin that can be used purposefully as a weapon in bioterroris ...
and is unlikely to have been genetically engineered
Genetic engineering, also called genetic modification or genetic manipulation, is the modification and manipulation of an organism's genes using technology. It is a set of technologies used to change the genetic makeup of cells, including t ...
.
The first confirmed human infections were in Wuhan. A study of the first 41 cases of confirmed COVID‑19, published in January 2020 in ''The Lancet'', reported the earliest date of onset of symptoms as 1December 2019.Huanan Seafood Wholesale Market
The Wuhan Huanan Seafood Wholesale Market (), simply known as the Huanan Seafood Market (''Huanan'' means 'South China'), was a live animal and seafood market in Jianghan District, Wuhan City, the capital of Hubei Province in Central China.
T ...
, which also sold live animals.superspreading event
A superspreading event (SSEV) is an event in which an infectious disease is spread much more than usual, while an unusually contagious organism infected with a disease is known as a superspreader. In the context of a human-borne illness, a super ...
, but that it was not the site of the initial outbreak. Traces of the virus have been found in wastewater samples that were collected in Milan
Milan ( , , Lombard: ; it, Milano ) is a city in northern Italy, capital of Lombardy, and the second-most populous city proper in Italy after Rome. The city proper has a population of about 1.4 million, while its metropolitan city h ...
and Turin
Turin ( , Piedmontese language, Piedmontese: ; it, Torino ) is a city and an important business and cultural centre in Northern Italy. It is the capital city of Piedmont and of the Metropolitan City of Turin, and was the first Italian capital ...
, Italy, on 18 December 2019.
By December 2019, the spread of infection was almost entirely driven by human-to-human transmission.Wuhan Central Hospital
The Central Hospital of Wuhan () is a tertiary hospital located in Jiang'an District in Wuhan, Hubei, China. It was established in 1880 as a clinic under the Hankow's Catholic church. In 1893, it was later expanded and renamed as Catholic Hospit ...
sent a bronchoalveolar lavage fluid
Bronchoalveolar lavage (BAL) (also known as bronchoalveolar washing) is a diagnostic method of the lower respiratory system in which a bronchoscope is passed through the mouth or nose into an appropriate airway in the lungs, with a measured amoun ...
(BAL) sample from an unresolved clinical case to sequencing company Vision Medicals. On 27 and 28 December, Vision Medicals informed the Wuhan Central Hospital and the Chinese CDC of the results of the test, showing a new coronavirus.Zhang Jixian
Zhang Jixian (, born 1966) is a Chinese pulmonologist. She is known to have discovered SARS‑CoV‑2, and was the director of the Department of Respiratory Medicine of Hubei Provincial Hospital of Integrated Chinese & Western Medicine. She is a ...
in Hubei Provincial Hospital, who informed the Wuhan Jianghan CDC on 27 December. On 30 December, a test report addressed to Wuhan Central Hospital, from company CapitalBio Medlab, stated an erroneous positive result for SARS
Severe acute respiratory syndrome (SARS) is a viral respiratory disease of zoonotic origin caused by the severe acute respiratory syndrome coronavirus (SARS-CoV or SARS-CoV-1), the first identified strain of the SARS coronavirus species, ''sever ...
, causing a group of doctors at Wuhan Central Hospital to alert their colleagues and relevant hospital authorities of the result. The Wuhan Municipal Health Commission issued a notice to various medical institutions on "the treatment of pneumonia of unknown cause" that same evening.Li Wenliang
Li Wenliang (; 12 October 1986 – 7 February 2020) was a Chinese ophthalmologist who warned his colleagues about early COVID-19 infections in Wuhan. On 30 December 2019, Wuhan CDC issued emergency warnings to local hospitals about a number ...
(punished on 3January),Ai Fen
Ai Fen () is a Chinese doctor and director of the emergency department of Central Hospital of Wuhan. In December 2019, she was one of the first doctors to encounter pneumonia patients infected with the then-unknown virus, SARS-CoV-2. On 30 Decem ...
, was reprimanded by her superiors for raising the alarm.Chinese provinces
The provincial level administrative divisions () are the highest-level administrative divisions of China. There are 34 such divisions claimed by the People's Republic of China, classified as 23 provinces (), five autonomous regions of China, au ...
, helped by the Chinese New Year migration and Wuhan being a transport hub and major rail interchange.Shenzhen
Shenzhen (; ; ; ), also historically known as Sham Chun, is a major sub-provincial city and one of the special economic zones of China. The city is located on the east bank of the Pearl River estuary on the central coast of southern province ...
.Public Health Emergency of International Concern
A public health emergency of international concern (PHEIC) is a formal declaration by the World Health Organization (WHO) of "an extraordinary event which is determined to constitute a public health risk to other States through the internatio ...
.New York
New York most commonly refers to:
* New York City, the most populous city in the United States, located in the state of New York
* New York (state), a state in the northeastern United States
New York may also refer to:
Film and television
* '' ...
came from European travellers, rather than directly from China or any other Asian country.Reuters
Reuters ( ) is a news agency owned by Thomson Reuters Corporation. It employs around 2,500 journalists and 600 photojournalists in about 200 locations worldwide. Reuters is one of the largest news agencies in the world.
The agency was estab ...
'' reported that it had estimated the worldwide total number of deaths due to COVID‑19 to have exceeded five million.
Misinformation
After the initial outbreak of COVID‑19, misinformation
Misinformation is incorrect or misleading information. It differs from disinformation, which is ''deliberately'' deceptive. Rumors are information not attributed to any particular source, and so are unreliable and often unverified, but can turn ou ...
and disinformation
Disinformation is false information deliberately spread to deceive people. It is sometimes confused with misinformation, which is false information but is not deliberate.
The English word ''disinformation'' comes from the application of the L ...
regarding the origin, scale, prevention, treatment, and other aspects of the disease rapidly spread online.Centers for Disease Control and Prevention
The Centers for Disease Control and Prevention (CDC) is the national public health agency of the United States. It is a United States federal agency, under the Department of Health and Human Services, and is headquartered in Atlanta, Georgi ...
(CDC) published preliminary estimates of the risk of death by age groups in the United States, but those estimates were widely misreported and misunderstood.
Other species
Humans appear to be capable of spreading the virus to some other animals, a type of disease transmission referred to as zooanthroponosis.
Some pets, especially cats and ferret
The ferret (''Mustela furo'') is a small, Domestication, domesticated species belonging to the family Mustelidae. The ferret is most likely a domesticated form of the wild European polecat (''Mustela putorius''), evidenced by their Hybrid (biol ...
s, can catch this virus from infected humans.respiratory
The respiratory system (also respiratory apparatus, ventilatory system) is a biological system consisting of specific organs and structures used for gas exchange in animals and plants. The anatomy and physiology that make this happen varies grea ...
(such as a cough) and digestive symptoms.pigs
The pig (''Sus domesticus''), often called swine, hog, or domestic pig when distinguishing from other members of the genus '' Sus'', is an omnivorous, domesticated, even-toed, hoofed mammal. It is variously considered a subspecies of ''Sus s ...
, ducks
Duck is the common name for numerous species of waterfowl in the family Anatidae. Ducks are generally smaller and shorter-necked than swans and geese, which are members of the same family. Divided among several subfamilies, they are a form t ...
, or chickens at all.Mice
A mouse ( : mice) is a small rodent. Characteristically, mice are known to have a pointed snout, small rounded ears, a body-length scaly tail, and a high breeding rate. The best known mouse species is the common house mouse (''Mus musculus' ...
, rats, and rabbits, if they can be infected at all, are unlikely to be involved in spreading the virus.great ape
The Hominidae (), whose members are known as the great apes or hominids (), are a taxonomic family of primates that includes eight extant species in four genera: '' Pongo'' (the Bornean, Sumatran and Tapanuli orangutan); ''Gorilla'' (the east ...
species such as orangutan
Orangutans are great apes native to the rainforests of Indonesia and Malaysia. They are now found only in parts of Borneo and Sumatra, but during the Pleistocene they ranged throughout Southeast Asia and South China. Classified in the genus ...
s can also be infected with the COVID‑19 virus.mink farm
Fur farming is the practice of breeding or raising certain types of animals for their fur.
Most of the world's farmed fur is produced by European farmers. In 2018, there were 5,000 fur farms in the European Union, EU, all located across 22 co ...
s.Denmark
)
, song = ( en, "King Christian stood by the lofty mast")
, song_type = National and royal anthem
, image_map = EU-Denmark.svg
, map_caption =
, subdivision_type = Sovereign state
, subdivision_name = Danish Realm, Kingdom of Denmark
...
, a major producer of mink pelts, ordered the slaughter of all minks over fears of viral mutations,Cluster 5
Cluster 5 is a designation used by the Danish Statens Serum Institut for a virus variant described by the institute in autumn 2020, in connection with investigations of SARS-CoV-2 infection among mink and humans in the north of Jutland, Denmark. ...
. A vaccine for mink and other animals is being researched.
Research
International research on vaccines and medicines in COVID‑19 is underway by government organisations, academic groups, and industry researchers.clinical trial
Clinical trials are prospective biomedical or behavioral research studies on human participants designed to answer specific questions about biomedical or behavioral interventions, including new treatments (such as novel vaccines, drugs, dietar ...
s have been undertaken, with research happening on every continent except Antarctica
Antarctica () is Earth's southernmost and least-populated continent. Situated almost entirely south of the Antarctic Circle and surrounded by the Southern Ocean, it contains the geographic South Pole. Antarctica is the fifth-largest contine ...
. , more than 200 possible treatments have been studied in humans.
Transmission and prevention research
Modelling research has been conducted with several objectives, including predictions of the dynamics of transmission, diagnosis and prognosis of infection, estimation of the impact of interventions, or allocation of resources. Modelling studies are mostly based on compartmental models in epidemiology
Compartmental models are a very general modelling technique. They are often applied to the mathematical modelling of infectious diseases. The population is assigned to compartments with labels – for example, S, I, or R, (Susceptible, Infectious, ...
, estimating the number of infected people over time under given conditions. Several other types of models have been developed and used during the COVID‑19 including computational fluid dynamics
Computational fluid dynamics (CFD) is a branch of fluid mechanics that uses numerical analysis and data structures to analyze and solve problems that involve fluid flows. Computers are used to perform the calculations required to simulate th ...
models to study the flow physics of COVID‑19, retrofits of crowd movement models to study occupant exposure, mobility-data based models to investigate transmission, or the use of macroeconomic
Macroeconomics (from the Greek prefix ''makro-'' meaning "large" + ''economics'') is a branch of economics dealing with performance, structure, behavior, and decision-making of an economy as a whole.
For example, using interest rates, taxes, and ...
models to assess the economic impact of the pandemic. Further, conceptual frameworks from crisis management research have been applied to better understand the effects of COVID‑19 on organisations worldwide.
Treatment-related research
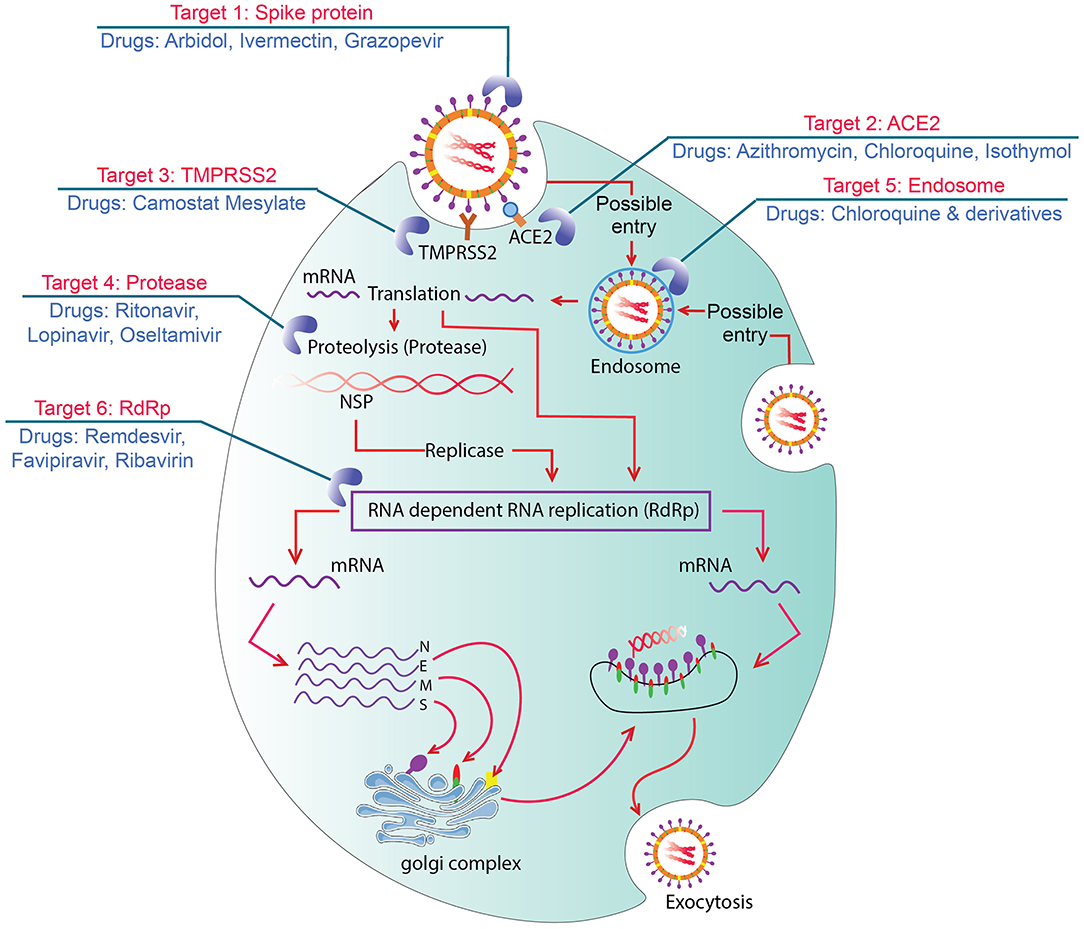 Repurposed
Repurposed antiviral drug
Antiviral drugs are a class of medication used for treating viral infections. Most antivirals target specific viruses, while a broad-spectrum antiviral is effective against a wide range of viruses. Unlike most antibiotics, antiviral drugs do n ...
s make up most of the research into COVID‑19 treatments.vasodilator
Vasodilation is the widening of blood vessels. It results from relaxation of smooth muscle cells within the vessel walls, in particular in the large veins, large arteries, and smaller arterioles. The process is the opposite of vasoconstriction, ...
s, corticosteroid
Corticosteroids are a class of steroid hormones that are produced in the adrenal cortex of vertebrates, as well as the synthetic analogues of these hormones. Two main classes of corticosteroids, glucocorticoids and mineralocorticoids, are involv ...
s, immune therapies, lipoic acid
Lipoic acid (LA), also known as α-lipoic acid, alpha-lipoic acid (ALA) and thioctic acid, is an organosulfur compound derived from caprylic acid (octanoic acid). ALA is made in animals normally, and is essential for aerobic metabolism. It is a ...
, bevacizumab
Bevacizumab, sold under the brand name Avastin among others, is a medication used to treat a number of types of cancers and a specific eye disease. For cancer, it is given by slow injection into a vein (intravenous) and used for colon cancer, l ...
, and recombinant angiotensin-converting enzyme 2.World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level of h ...
(WHO) initiated the Solidarity trial
The Solidarity trial for treatments is a multinational Phase III-IV clinical trial organized by the World Health Organization (WHO) and partners to compare four untested treatments for hospitalized people with severe COVID-19 illness. The tria ...
to assess the treatment effects of some promising drugs: an experimental drug
An experimental drug is a medicinal product (a drug or vaccine) that has not yet received approval from governmental regulatory authorities for routine use in human or veterinary medicine. A medicinal product may be approved for use in one disease ...
called remdesivir; anti-malarial drugs chloroquine and hydroxychloroquine; two anti-HIV drugs, lopinavir/ritonavir
Lopinavir/ritonavir (LPV/r), sold under the brand name Kaletra among others, is a fixed-dose combination antiretroviral medication for the treatment and prevention of HIV/AIDS. It combines lopinavir with a low dose of ritonavir. It is generall ...
; and interferon-beta
The type-I interferons (IFN) are cytokines which play essential roles in inflammation, immunoregulation, tumor cells recognition, and T-cell responses. In the human genome, a cluster of thirteen functional IFN genes is located at the 9p21.3 cyto ...
.hydroxychloroquine
Hydroxychloroquine, sold under the brand name Plaquenil among others, is a medication used to prevent and treat malaria in areas where malaria remains sensitive to chloroquine. Other uses include treatment of rheumatoid arthritis, lupus, an ...
and chloroquine
Chloroquine is a medication primarily used to prevent and treat malaria in areas where malaria remains sensitive to its effects. Certain types of malaria, resistant strains, and complicated cases typically require different or additional medi ...
showed that they were ineffective at best,RECOVERY Trial
The Randomised Evaluation of COVID-19 Therapy (RECOVERY Trial) is a large-enrollment clinical trial of possible treatments for people in the United Kingdom admitted to hospital with severe COVID-19 infection. The trial was later expanded to In ...
in the United Kingdom showed that dexamethasone reduced mortality by one third for people who are critically ill on ventilators and one fifth for those receiving supplemental oxygen. Because this is a well-tested and widely available treatment, it was welcomed by the WHO, which is in the process of updating treatment guidelines to include dexamethasone and other steroids. Based on those preliminary results, dexamethasone treatment has been recommended by the NIH for patients with COVID‑19 who are mechanically ventilated or who require supplemental oxygen but not in patients with COVID‑19 who do not require supplemental oxygen.
In September 2020, the WHO released updated guidance on using corticosteroids for COVID‑19.European Medicines Agency
The European Medicines Agency (EMA) is an agency of the European Union (EU) in charge of the evaluation and supervision of medicinal products. Prior to 2004, it was known as the European Agency for the Evaluation of Medicinal Products or Euro ...
(EMA) endorsed the use of dexamethasone in adults and adolescents from twelve years of age and weighing at least who require supplemental oxygen therapy.[ Text was copied from this source which is European Medicines Agency. Reproduction is authorized provided the source is acknowledged.] Dexamethasone can be taken by mouth
Oral administration is a route of administration where a substance is taken through the mouth. Per os abbreviated to P.O. is sometimes used as a direction for medication to be taken orally. Many medications are taken orally because they are i ...
or given as an injection or infusion (drip) into a vein.Food and Drug Administration
The United States Food and Drug Administration (FDA or US FDA) is a List of United States federal agencies, federal agency of the United States Department of Health and Human Services, Department of Health and Human Services. The FDA is respon ...
(FDA) issued an emergency use authorization for the investigational monoclonal antibody therapy bamlanivimab for the treatment of mild-to-moderate COVID‑19.etesevimab
Bamlanivimab/etesevimab is a combination of two monoclonal antibodies, bamlanivimab and etesevimab, administered together via intravenous infusion as a treatment for COVID-19. Both types of antibody target the surface spike protein of SAR ...
administered together for the treatment of mild to moderate COVID‑19 in people twelve years of age or older weighing at least who test positive for SARS‑CoV‑2 and who are at high risk for progressing to severe COVID‑19. The authorised use includes treatment for those who are 65 years of age or older or who have certain chronic medical conditions.
Cytokine storm
 A
A cytokine storm
A cytokine storm, also called hypercytokinemia, is a physiological reaction in humans and other animals in which the innate immune system causes an uncontrolled and excessive release of pro-inflammatory signaling molecules called cytokines. Norm ...
can be a complication in the later stages of severe COVID‑19. A cytokine storm is a potentially deadly immune reaction where a large amount of pro-inflammatory cytokines and chemokine
Chemokines (), or chemotactic cytokines, are a family of small cytokines or signaling proteins secreted by cells that induce directional movement of leukocytes, as well as other cell types, including endothelial and epithelial cells. In additio ...
s are released too quickly. A cytokine storm can lead to ARDS and multiple organ failure. Data collected from Jin Yin-tan Hospital in Wuhan, China indicates that patients who had more severe responses to COVID‑19 had greater amounts of pro-inflammatory cytokines and chemokines in their system than patients who had milder responses. These high levels of pro-inflammatory cytokines and chemokines indicate presence of a cytokine storm.
Tocilizumab
Tocilizumab, sold under the brand name Actemra among others, is an immunosuppressive drug, used for the treatment of rheumatoid arthritis, systemic juvenile idiopathic arthritis, a severe form of arthritis in children, and COVID19. It is a huma ...
has been included in treatment guidelines by China's National Health Commission
The National Health Commission of the People's Republic of China is a cabinet-level executive department of the State Council which is responsible for formulating national health policies. It was formed on 19 March 2018. The ministry is headqu ...
after a small study was completed.[Various sources:
*
*
* ] The interleukin-6 receptor
Interleukin 6 receptor (IL6R) also known as CD126 (Cluster of Differentiation 126) is a type I cytokine receptor.
Function
Interleukin 6 (IL6) is a potent pleiotropic cytokine that regulates cell growth and differentiation and plays an importa ...
(IL-6R) antagonist
An antagonist is a character in a story who is presented as the chief foe of the protagonist.
Etymology
The English word antagonist comes from the Greek ἀνταγωνιστής – ''antagonistēs'', "opponent, competitor, villain, enemy, riv ...
was approved by the FDA to undergo a PhaseIII clinical trial assessing its effectiveness on COVID‑19 based on retrospective case studies for the treatment of steroid-refractory cytokine release syndrome induced by a different cause, CAR T cell
In biology, chimeric antigen receptors (CARs)—also known as chimeric immunoreceptors, chimeric T cell receptors or artificial T cell receptors—are receptor (biochemistry), receptor proteins that have been engineered to give T cells the new abi ...
therapy
A therapy or medical treatment (often abbreviated tx, Tx, or Tx) is the attempted remediation of a health problem, usually following a medical diagnosis.
As a rule, each therapy has indications and contraindications. There are many different ...
, in 2017.blood–brain barrier
The blood–brain barrier (BBB) is a highly selective semipermeable membrane, semipermeable border of endothelium, endothelial cells that prevents solutes in the circulating blood from ''non-selectively'' crossing into the extracellular fluid of ...
, and exacerbating neurotoxicity
Neurotoxicity is a form of toxicity in which a biological, chemical, or physical agent produces an adverse effect on the structure or function of the central and/or peripheral nervous system. It occurs when exposure to a substance – specificall ...
while having no effect on the incidence of CRS.
Lenzilumab
Lenzilumab (International Nonproprietary Name, INN; development code KB003) is a humanized monoclonal antibody (class IgG1 kappa) that targets colony stimulating factor 2 (CSF2)/granulocyte-macrophage colony stimulating factor (Granulocyte macrop ...
, an anti-GM-CSF monoclonal antibody
A monoclonal antibody (mAb, more rarely called moAb) is an antibody produced from a cell Lineage made by cloning a unique white blood cell. All subsequent antibodies derived this way trace back to a unique parent cell.
Monoclonal antibodies ca ...
, is protective in murine models for CAR T cell-induced CRS and neurotoxicity and is a viable therapeutic option due to the observed increase of pathogenic GM-CSF secreting Tcells in hospitalised patients with COVID‑19.
Passive antibodies
 Transferring purified and concentrated
Transferring purified and concentrated antibodies
An antibody (Ab), also known as an immunoglobulin (Ig), is a large, Y-shaped protein used by the immune system to identify and neutralize foreign objects such as pathogenic bacteria and viruses. The antibody recognizes a unique molecule of the ...
produced by the immune systems of those who have recovered from COVID‑19 to people who need them is being investigated as a non-vaccine method of passive immunisation.mechanism of action
In pharmacology, the term mechanism of action (MOA) refers to the specific biochemical interaction through which a drug substance produces its pharmacological effect. A mechanism of action usually includes mention of the specific molecular targe ...
by which passive antibody therapy can mediate defence against SARS-CoV-2. The spike protein of SARS-CoV-2 is the primary target for neutralising antibodies.phagocytosis
Phagocytosis () is the process by which a cell uses its plasma membrane to engulf a large particle (≥ 0.5 μm), giving rise to an internal compartment called the phagosome. It is one type of endocytosis. A cell that performs phagocytosis is ...
, may be possible.convalescent serum
Antiserum is a blood serum containing monoclonal or polyclonal antibodies that is used to spread passive immunity to many diseases via blood donation (plasmapheresis). For example, convalescent serum, passive antibody transfusion from a previ ...
, which consists of the liquid portion of the blood from people who recovered from the infection and contains antibodies specific to this virus, which is then administered to active patients.
Bioethics
Since the outbreak of the COVID‑19 pandemic, scholars have explored the bioethics
Bioethics is both a field of study and professional practice, interested in ethical issues related to health (primarily focused on the human, but also increasingly includes animal ethics), including those emerging from advances in biology, med ...
, normative economics Normative economics (as opposed to positive economics) is the part of economics that deals with normative statements. It focuses on the idea of fairness and what the outcome of the economy or goals of public policy ''ought to be''.Paul A. Samuelson ...
, and political theories
Political philosophy or political theory is the philosophical study of government, addressing questions about the nature, scope, and legitimacy of public agents and institutions and the relationships between them. Its topics include politics, l ...
of healthcare policies related to the public health crisis. Academics have pointed to the moral distress of healthcare workers, ethics of distributing scarce healthcare resources such as ventilators, and the global justice of vaccine diplomacies. The socio-economic inequalities between genders, races, groups with disabilities, communities, regions, countries, and continents have also drawn attention in academia and the general public.
Effects on other diseases
The use of social distancing
In public health, social distancing, also called physical distancing, (NB. Regula Venske is president of the PEN Centre Germany.) is a set of non-pharmaceutical interventions or measures intended to prevent the spread of a contagious disea ...
and the wearing of surgical mask
A surgical mask, also known by other names such as a medical face mask or procedure mask, is a personal protective equipment used by healthcare professionals that serves as a mechanical barrier that interferes with direct airflow in and out of re ...
s and similar precautions against COVID‑19 may have caused a drop in the spread of the common cold
The common cold or the cold is a viral infectious disease of the upper respiratory tract that primarily affects the respiratory mucosa of the nose, throat, sinuses, and larynx. Signs and symptoms may appear fewer than two days after exposu ...
and the flu
Influenza, commonly known as "the flu", is an infectious disease caused by influenza viruses. Symptoms range from mild to severe and often include fever, runny nose, sore throat, muscle pain, headache, coughing, and fatigue. These symptom ...
.
See also
* Coronavirus diseases
Coronavirus diseases are caused by viruses in the coronavirus subfamily, a group of related RNA viruses that cause diseases in mammals and birds. In humans and birds, the group of viruses cause respiratory tract infections that can range fr ...
, a group of closely related syndromes
* Disease X
Disease X is a placeholder name that was adopted by the World Health Organization (WHO) in February 2018 on their shortlist of blueprint priority diseases to represent a hypothetical, unknown pathogen that could cause a future epidemic. The WHO ...
, a WHO term
*
*
References
Further reading
* Scholia
Scholia (singular scholium or scholion, from grc, σχόλιον, "comment, interpretation") are grammatical, critical, or explanatory comments – original or copied from prior commentaries – which are inserted in the margin of th ...
Q104287299.
*
*
External links
Health agencies
Coronavirus disease (COVID‑19)Facts
by the World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level of h ...
(WHO)
Coronavirus 2019 (COVID-19)
by the US Centers for Disease Control and Prevention
The Centers for Disease Control and Prevention (CDC) is the national public health agency of the United States. It is a United States federal agency, under the Department of Health and Human Services, and is headquartered in Atlanta, Georgi ...
(CDC)
Coronavirus (COVID‑19)
by the UK National Health Service
The National Health Service (NHS) is the umbrella term for the publicly funded healthcare systems of the United Kingdom (UK). Since 1948, they have been funded out of general taxation. There are three systems which are referred to using the " ...
(NHS)
Directories
Coronavirus Resource Center
at the Center for Inquiry
The Center for Inquiry (CFI) is a US nonprofit organization that works to mitigate belief in pseudoscience and the paranormal, as well as to fight the influence of religion in government.
History
The Center for Inquiry was established in 199 ...
*
COVID‑19 Resource Directory on OpenMD
Medical journals
Coronavirus Disease 2019 (COVID‑19)
by ''JAMA
''The Journal of the American Medical Association'' (''JAMA'') is a peer-reviewed medical journal published 48 times a year by the American Medical Association. It publishes original research, reviews, and editorials covering all aspects of biom ...
''
BMJ's Coronavirus (covid‑19) Hub
by the BMJ
''The BMJ'' is a weekly peer-reviewed medical trade journal, published by the trade union the British Medical Association (BMA). ''The BMJ'' has editorial freedom from the BMA. It is one of the world's oldest general medical journals. Origina ...
Novel Coronavirus Information Center
by Elsevier
Elsevier () is a Dutch academic publishing company specializing in scientific, technical, and medical content. Its products include journals such as ''The Lancet'', ''Cell'', the ScienceDirect collection of electronic journals, '' Trends'', th ...
COVID‑19 Resource Centre
by ''The Lancet
''The Lancet'' is a weekly peer-reviewed general medical journal and one of the oldest of its kind. It is also the world's highest-impact academic journal. It was founded in England in 1823.
The journal publishes original research articles, ...
''
Coronavirus (COVID‑19) Research Highlights
by Springer Nature
Springer Nature or the Springer Nature Group is a German-British academic publishing company created by the May 2015 merger of Springer Science+Business Media and Holtzbrinck Publishing Group's Nature Publishing Group, Palgrave Macmillan, and Macm ...
Coronavirus (Covid‑19)
by ''The New England Journal of Medicine
''The New England Journal of Medicine'' (''NEJM'') is a weekly medical journal published by the Massachusetts Medical Society. It is among the most prestigious peer-reviewed medical journals as well as the oldest continuously published one.
His ...
''
Covid‑19: Novel Coronavirus
by Wiley Publishing
John Wiley & Sons, Inc., commonly known as Wiley (), is an American multinational publishing company founded in 1807 that focuses on academic publishing and instructional materials. The company produces books, journals, and encyclopedias, in p ...
Treatment guidelines
*
*
*
*
*
*
{{Authority control
Occupational safety and health
Vaccine-preventable diseases
Viral respiratory tract infections
Zoonoses
Public health
Coronavirus-associated diseases

 The SARS-CoV-2 virus can infect a wide range of cells and systems of the body. COVID‑19 is most known for affecting the upper respiratory tract (sinuses, nose, and throat) and the lower respiratory tract (windpipe and lungs). The lungs are the organs most affected by COVID‑19 because the virus accesses host cells via the
The SARS-CoV-2 virus can infect a wide range of cells and systems of the body. COVID‑19 is most known for affecting the upper respiratory tract (sinuses, nose, and throat) and the lower respiratory tract (windpipe and lungs). The lungs are the organs most affected by COVID‑19 because the virus accesses host cells via the  Research conducted when Alpha was the dominant variant has suggested COVID-19 may cause brain damage. It is unknown if such damage is temporary or permanent, and whether Omicron has similar effects. Observed individuals infected with COVID-19 (most with mild cases) experienced an additional 0.2% to 2% of brain tissue lost in regions of the brain connected to the sense of smell compared with uninfected individuals, and the overall effect on the brain was equivalent on average to at least one extra year of normal ageing; infected individuals also scored lower on several cognitive tests. All effects were more pronounced among older ages.
Research conducted when Alpha was the dominant variant has suggested COVID-19 may cause brain damage. It is unknown if such damage is temporary or permanent, and whether Omicron has similar effects. Observed individuals infected with COVID-19 (most with mild cases) experienced an additional 0.2% to 2% of brain tissue lost in regions of the brain connected to the sense of smell compared with uninfected individuals, and the overall effect on the brain was equivalent on average to at least one extra year of normal ageing; infected individuals also scored lower on several cognitive tests. All effects were more pronounced among older ages.
 Although SARS-CoV-2 has a tropism for ACE2-expressing epithelial cells of the respiratory tract, people with severe COVID‑19 have symptoms of systemic hyperinflammation. Clinical laboratory findings of elevated IL2, IL7, IL6,
Although SARS-CoV-2 has a tropism for ACE2-expressing epithelial cells of the respiratory tract, people with severe COVID‑19 have symptoms of systemic hyperinflammation. Clinical laboratory findings of elevated IL2, IL7, IL6,  Multiple viral and host factors affect the pathogenesis of the virus. The S-protein, otherwise known as the spike protein, is the viral component that attaches to the host receptor via the
Multiple viral and host factors affect the pathogenesis of the virus. The S-protein, otherwise known as the spike protein, is the viral component that attaches to the host receptor via the  The severity of the inflammation can be attributed to the severity of what is known as the
The severity of the inflammation can be attributed to the severity of what is known as the 

 Chest CT scans may be helpful to diagnose COVID‑19 in individuals with a high clinical suspicion of infection but are not recommended for routine screening. Bilateral multilobar
Chest CT scans may be helpful to diagnose COVID‑19 in individuals with a high clinical suspicion of infection but are not recommended for routine screening. Bilateral multilobar  Preventive measures to reduce the chances of infection include getting vaccinated, staying at home, wearing a mask in public, avoiding crowded places, keeping distance from others, ventilating indoor spaces, managing potential exposure durations, washing hands with soap and water often and for at least twenty seconds, practising good respiratory hygiene, and avoiding touching the eyes, nose, or mouth with unwashed hands.
Those diagnosed with COVID‑19 or who believe they may be infected are advised by the CDC to stay home except to get medical care, call ahead before visiting a healthcare provider, wear a face mask before entering the healthcare provider's office and when in any room or vehicle with another person, cover coughs and sneezes with a tissue, regularly wash hands with soap and water and avoid sharing personal household items.
The first
Preventive measures to reduce the chances of infection include getting vaccinated, staying at home, wearing a mask in public, avoiding crowded places, keeping distance from others, ventilating indoor spaces, managing potential exposure durations, washing hands with soap and water often and for at least twenty seconds, practising good respiratory hygiene, and avoiding touching the eyes, nose, or mouth with unwashed hands.
Those diagnosed with COVID‑19 or who believe they may be infected are advised by the CDC to stay home except to get medical care, call ahead before visiting a healthcare provider, wear a face mask before entering the healthcare provider's office and when in any room or vehicle with another person, cover coughs and sneezes with a tissue, regularly wash hands with soap and water and avoid sharing personal household items.
The first 

 The WHO and the US CDC recommend individuals wear non-medical face coverings in public settings where there is an increased risk of transmission and where social distancing measures are difficult to maintain. This recommendation is meant to reduce the spread of the disease by asymptomatic and pre-symptomatic individuals and is complementary to established preventive measures such as social distancing. Face coverings limit the volume and travel distance of expiratory droplets dispersed when talking, breathing, and coughing. A face covering without vents or holes will also filter out particles containing the virus from inhaled and exhaled air, reducing the chances of infection. However, if the mask includes an exhalation valve, a wearer that is infected (and possibly asymptomatic) may transmit the virus through the valve. Many countries and local jurisdictions encourage or mandate the use of face masks or cloth face coverings by members of the public to limit the spread of the virus.
Masks are also strongly recommended for those who may have been infected and those taking care of someone who may have the disease. When not wearing a mask, the CDC recommends covering the mouth and nose with a tissue when coughing or sneezing and recommends using the inside of the elbow if no tissue is available. Proper hand hygiene after any cough or sneeze is encouraged. Healthcare professionals interacting directly with people who have COVID‑19 are advised to use
The WHO and the US CDC recommend individuals wear non-medical face coverings in public settings where there is an increased risk of transmission and where social distancing measures are difficult to maintain. This recommendation is meant to reduce the spread of the disease by asymptomatic and pre-symptomatic individuals and is complementary to established preventive measures such as social distancing. Face coverings limit the volume and travel distance of expiratory droplets dispersed when talking, breathing, and coughing. A face covering without vents or holes will also filter out particles containing the virus from inhaled and exhaled air, reducing the chances of infection. However, if the mask includes an exhalation valve, a wearer that is infected (and possibly asymptomatic) may transmit the virus through the valve. Many countries and local jurisdictions encourage or mandate the use of face masks or cloth face coverings by members of the public to limit the spread of the virus.
Masks are also strongly recommended for those who may have been infected and those taking care of someone who may have the disease. When not wearing a mask, the CDC recommends covering the mouth and nose with a tissue when coughing or sneezing and recommends using the inside of the elbow if no tissue is available. Proper hand hygiene after any cough or sneeze is encouraged. Healthcare professionals interacting directly with people who have COVID‑19 are advised to use  Thorough hand hygiene after any cough or sneeze is required. The WHO also recommends that individuals wash hands often with soap and water for at least twenty seconds, especially after going to the toilet or when hands are visibly dirty, before eating and after blowing one's nose. When soap and water are not available, the CDC recommends using an alcohol-based
Thorough hand hygiene after any cough or sneeze is required. The WHO also recommends that individuals wash hands often with soap and water for at least twenty seconds, especially after going to the toilet or when hands are visibly dirty, before eating and after blowing one's nose. When soap and water are not available, the CDC recommends using an alcohol-based 
 Complications may include
Complications may include  The
The  A December 2020 systematic review and meta-analysis estimated that population IFR during the first wave of the pandemic was about 0.5% to 1% in many locations (including France, Netherlands, New Zealand, and Portugal), 1% to 2% in other locations (Australia, England, Lithuania, and Spain), and exceeded 2% in Italy.
A December 2020 systematic review and meta-analysis estimated that population IFR during the first wave of the pandemic was about 0.5% to 1% in many locations (including France, Netherlands, New Zealand, and Portugal), 1% to 2% in other locations (Australia, England, Lithuania, and Spain), and exceeded 2% in Italy.  Repurposed
Repurposed  A
A  Transferring purified and concentrated
Transferring purified and concentrated