Bubonic plague on:
[Wikipedia]
[Google]
[Amazon]
Bubonic plague is one of three types of
 Bubonic plague is an infection of the
Bubonic plague is an infection of the
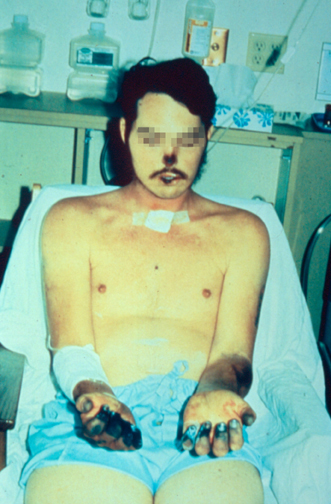 After being transmitted via the bite of an infected flea, the ''Y. pestis'' bacteria become localized in an inflamed
After being transmitted via the bite of an infected flea, the ''Y. pestis'' bacteria become localized in an inflamed
 Samples taken for testing include:
* Buboes: Swollen lymph nodes (buboes) characteristic of bubonic plague, a fluid sample can be taken from them with a needle.
* Blood
* Lungs
Samples taken for testing include:
* Buboes: Swollen lymph nodes (buboes) characteristic of bubonic plague, a fluid sample can be taken from them with a needle.
* Blood
* Lungs
 Globally between 2010 and 2015, there were 3,248 documented cases, which resulted in 584 deaths. The countries with the greatest number of cases are the
Globally between 2010 and 2015, there were 3,248 documented cases, which resulted in 584 deaths. The countries with the greatest number of cases are the  In July 2020, in
In July 2020, in
 In the
In the
 The scale of death and social upheaval associated with plague outbreaks has made the topic prominent in many historical and fictional accounts since the disease was first recognized. The
The scale of death and social upheaval associated with plague outbreaks has made the topic prominent in many historical and fictional accounts since the disease was first recognized. The
plague
Plague or The Plague may refer to:
Agriculture, fauna, and medicine
*Plague (disease), a disease caused by ''Yersinia pestis''
* An epidemic of infectious disease (medical or agricultural)
* A pandemic caused by such a disease
* A swarm of pe ...
caused by the plague bacterium
Bacteria (; singular: bacterium) are ubiquitous, mostly free-living organisms often consisting of one biological cell. They constitute a large domain of prokaryotic microorganisms. Typically a few micrometres in length, bacteria were among ...
(''Yersinia pestis
''Yersinia pestis'' (''Y. pestis''; formerly '' Pasteurella pestis'') is a gram-negative, non-motile, coccobacillus bacterium without spores that is related to both ''Yersinia pseudotuberculosis'' and ''Yersinia enterocolitica''. It is a facult ...
''). One to seven days after exposure to the bacteria, flu-like symptoms
Influenza-like illness (ILI), also known as flu-like syndrome or flu-like symptoms, is a medical diagnosis of possible influenza or other illness causing a set of common symptoms. These include fever, shivering, chills, malaise, dry cough, loss ...
develop. These symptoms include fever
Fever, also referred to as pyrexia, is defined as having a body temperature, temperature above the human body temperature, normal range due to an increase in the body's temperature Human body temperature#Fever, set point. There is not a single ...
, headache
Headache is the symptom of pain in the face, head, or neck. It can occur as a migraine, tension-type headache, or cluster headache. There is an increased risk of depression in those with severe headaches.
Headaches can occur as a result ...
s, and vomiting
Vomiting (also known as emesis and throwing up) is the involuntary, forceful expulsion of the contents of one's stomach through the mouth and sometimes the nose.
Vomiting can be the result of ailments like food poisoning, gastroenteri ...
, as well as swollen and painful lymph nodes occurring in the area closest to where the bacteria entered the skin. Acral necrosis
Acral necrosis is a symptom common in bubonic plague. The striking black discoloration of skin and tissue, primarily on the extremities ("acral"), is commonly thought to have given rise to the name "Black Death," associated both with the disease ...
, the dark discoloration of skin, is another symptom. Occasionally, swollen lymph nodes, known as "bubo
A bubo (Greek βουβών, ''boubṓn'', 'groin') is adenitis or inflammation of the lymph nodes and is an example of reactive lymphadenopathy.
Classification
Buboes are a symptom of bubonic plague and occur as painful swellings in the thigh ...
es," may break open.
The three types of plague are the result of the route of infection: bubonic plague, septicemic plague
Septicemic plague is one of the three forms of plague, and is caused by '' Yersinia pestis'', a gram-negative species of bacterium. Septicemic plague is a systemic disease involving infection of the blood, and is most commonly spread by bites fro ...
, and pneumonic plague
Pneumonic plague is a severe lung infection caused by the bacterium ''Yersinia pestis''. Symptoms include fever, headache, shortness of breath, chest pain, and coughing. They typically start about three to seven days after exposure. It is one ...
. Bubonic plague is mainly spread by infected flea
Flea, the common name for the order Siphonaptera, includes 2,500 species of small flightless insects that live as external parasites of mammals and birds. Fleas live by ingesting the blood of their hosts. Adult fleas grow to about long, a ...
s from small animal
Animals are multicellular, eukaryotic organisms in the Kingdom (biology), biological kingdom Animalia. With few exceptions, animals Heterotroph, consume organic material, Cellular respiration#Aerobic respiration, breathe oxygen, are Motilit ...
s. It may also result from exposure to the body fluids from a dead plague-infected animal. Mammals such as rabbit
Rabbits, also known as bunnies or bunny rabbits, are small mammals in the family Leporidae (which also contains the hares) of the order Lagomorpha (which also contains the pikas). ''Oryctolagus cuniculus'' includes the European rabbit speci ...
s, hare
Hares and jackrabbits are mammals belonging to the genus ''Lepus''. They are herbivores, and live solitarily or in pairs. They nest in slight depressions called forms, and their young are able to fend for themselves shortly after birth. The ge ...
s, and some cat
The cat (''Felis catus'') is a domestic species of small carnivorous mammal. It is the only domesticated species in the family Felidae and is commonly referred to as the domestic cat or house cat to distinguish it from the wild members of ...
species are susceptible to bubonic plague, and typically die upon contraction. In the bubonic form of plague, the bacteria enter through the skin through a flea bite and travel via the lymphatic vessels
The lymphatic vessels (or lymph vessels or lymphatics) are thin-walled vessels (tubes), structured like blood vessels, that carry lymph. As part of the lymphatic system, lymph vessels are complementary to the cardiovascular system. Lymph vessel ...
to a lymph node
A lymph node, or lymph gland, is a kidney-shaped organ of the lymphatic system and the adaptive immune system. A large number of lymph nodes are linked throughout the body by the lymphatic vessels. They are major sites of lymphocytes that inclu ...
, causing it to swell. Diagnosis is made by finding the bacteria in the blood, sputum, or fluid from lymph nodes.
Prevention is through public health measures such as not handling dead animals in areas where plague is common. While vaccines against the plague have been developed, the World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level of h ...
recommends that only high-risk groups, such as certain laboratory personnel and health care workers, get inoculated. Several antibiotic
An antibiotic is a type of antimicrobial substance active against bacteria. It is the most important type of antibacterial agent for fighting bacterial infections, and antibiotic medications are widely used in the treatment and prevention of ...
s are effective for treatment, including streptomycin
Streptomycin is an antibiotic medication used to treat a number of bacterial infections, including tuberculosis, ''Mycobacterium avium'' complex, endocarditis, brucellosis, ''Burkholderia'' infection, plague, tularemia, and rat bite fever. Fo ...
, gentamicin
Gentamicin is an antibiotic used to treat several types of bacterial infections. This may include bone infections, endocarditis, pelvic inflammatory disease, meningitis, pneumonia, urinary tract infections, and sepsis among others. It is not e ...
, and doxycycline
Doxycycline is a broad-spectrum tetracycline class antibiotic used in the treatment of infections caused by bacteria and certain parasites. It is used to treat bacterial pneumonia, acne, chlamydia infections, Lyme disease, cholera, typhus, an ...
.
Without treatment, plague results in the death of 30% to 90% of those infected. Death, if it occurs, is typically within 10 days. With treatment, the risk of death is around 10%. Globally between 2010 and 2015 there were 3,248 documented cases, which resulted in 584 deaths. The countries with the greatest number of cases are the Democratic Republic of the Congo
The Democratic Republic of the Congo (french: République démocratique du Congo (RDC), colloquially "La RDC" ), informally Congo-Kinshasa, DR Congo, the DRC, the DROC, or the Congo, and formerly and also colloquially Zaire, is a country in ...
, Madagascar
Madagascar (; mg, Madagasikara, ), officially the Republic of Madagascar ( mg, Repoblikan'i Madagasikara, links=no, ; french: République de Madagascar), is an island country in the Indian Ocean, approximately off the coast of East Africa ...
, and Peru
, image_flag = Flag of Peru.svg
, image_coat = Escudo nacional del Perú.svg
, other_symbol = Great Seal of the State
, other_symbol_type = Seal (emblem), National seal
, national_motto = "Fi ...
.
The plague is considered the likely cause of the Black Death
The Black Death (also known as the Pestilence, the Great Mortality or the Plague) was a bubonic plague pandemic occurring in Western Eurasia and North Africa from 1346 to 1353. It is the most fatal pandemic recorded in human history, causi ...
that swept through Asia, Europe, and Africa in the 14th century and killed an estimated 50 million people, including about 25% to 60% of the European population. Because the plague killed so many of the working population, wages rose due to the demand for labor. Some historians see this as a turning point in European economic development. The disease is also considered to have been responsible for the Plague of Justinian
The plague of Justinian or Justinianic plague (541–549 AD) was the first recorded major outbreak of the first plague pandemic, the first Old World pandemic of plague, the contagious disease caused by the bacterium ''Yersinia pestis''. The dis ...
, originating in the Eastern Roman Empire
The Byzantine Empire, also referred to as the Eastern Roman Empire or Byzantium, was the continuation of the Roman Empire primarily in its eastern provinces during Late Antiquity and the Middle Ages, when its capital city was Constantinopl ...
in the 6th century CE, as well as the third epidemic, affecting China
China, officially the People's Republic of China (PRC), is a country in East Asia. It is the world's most populous country, with a population exceeding 1.4 billion, slightly ahead of India. China spans the equivalent of five time zones and ...
, Mongolia
Mongolia; Mongolian script: , , ; lit. "Mongol Nation" or "State of Mongolia" () is a landlocked country in East Asia, bordered by Russia to the north and China to the south. It covers an area of , with a population of just 3.3 million, ...
, and India
India, officially the Republic of India (Hindi: ), is a country in South Asia. It is the seventh-largest country by area, the second-most populous country, and the most populous democracy in the world. Bounded by the Indian Ocean on the so ...
, originating in the Yunnan Province
Yunnan , () is a landlocked province in the southwest of the People's Republic of China. The province spans approximately and has a population of 48.3 million (as of 2018). The capital of the province is Kunming. The province borders the C ...
in 1855. The term ''bubonic'' is derived from the Greek word βουβών, meaning "groin".
Cause
 Bubonic plague is an infection of the
Bubonic plague is an infection of the lymphatic system
The lymphatic system, or lymphoid system, is an organ system in vertebrates that is part of the immune system, and complementary to the circulatory system. It consists of a large network of lymphatic vessels, lymph nodes, lymphatic or lymphoid o ...
, usually resulting from the bite of an infected flea, ''Xenopsylla cheopis'' (the Oriental rat flea
The Oriental rat flea (''Xenopsylla cheopis''), also known as the tropical rat flea or the rat flea, is a parasite of rodents, primarily of the genus ''Rattus'', and is a primary vector for bubonic plague and murine typhus. This occurs when a fl ...
). Several flea species carried the bubonic plague, such as ''Pulex irritans'' (the human flea
The human flea (''Pulex irritans'') – once also called the house flea – is a cosmopolitan flea species that has, in spite of the common name, a wide host spectrum. It is one of six species in the genus '' Pulex''; the other five are all confi ...
), ''Xenopsylla cheopis'', and '' Ceratophyllus fasciatus''. ''Xenopsylla cheopis'' was the most effective flea species for transmittal. In very rare circumstances, as in septicemic plague
Septicemic plague is one of the three forms of plague, and is caused by '' Yersinia pestis'', a gram-negative species of bacterium. Septicemic plague is a systemic disease involving infection of the blood, and is most commonly spread by bites fro ...
, the disease can be transmitted by direct contact with infected tissue or exposure to the cough of another human. The flea is parasitic on house and field rats and seeks out other prey when its rodent hosts die. Rats were an amplifying factor to bubonic plague due to their common association with humans as well as the nature of their blood. The rat's blood allowed the rat to withstand a major concentration
In chemistry, concentration is the abundance of a constituent divided by the total volume of a mixture. Several types of mathematical description can be distinguished: '' mass concentration'', ''molar concentration'', ''number concentration'', an ...
of the plague. The bacteria form aggregates in the gut of infected fleas and this results in the flea regurgitating ingested blood, which is now infected, into the bite site of a rodent or human host. Once established, bacteria rapidly spread to the lymph node
A lymph node, or lymph gland, is a kidney-shaped organ of the lymphatic system and the adaptive immune system. A large number of lymph nodes are linked throughout the body by the lymphatic vessels. They are major sites of lymphocytes that inclu ...
s and multiply. The fleas that transmit the disease only directly infect humans when the rat population in the area is wiped out from a mass infection. Furthermore, in areas of a large population of rats, the animals can harbor low levels of the plague infection without causing human outbreaks. With no new rat inputs being added to the population from other areas, the infection would only spread to humans in very rare cases of overcrowding.
Signs and symptoms
 After being transmitted via the bite of an infected flea, the ''Y. pestis'' bacteria become localized in an inflamed
After being transmitted via the bite of an infected flea, the ''Y. pestis'' bacteria become localized in an inflamed lymph node
A lymph node, or lymph gland, is a kidney-shaped organ of the lymphatic system and the adaptive immune system. A large number of lymph nodes are linked throughout the body by the lymphatic vessels. They are major sites of lymphocytes that inclu ...
, where they begin to colonize and reproduce. Infected lymph nodes develop hemorrhages, which result in the death of tissue.'' Y. pestis'' bacilli
Bacilli is a taxonomic class of bacteria that includes two orders, Bacillales and Lactobacillales, which contain several well-known pathogens such as ''Bacillus anthracis'' (the cause of anthrax). ''Bacilli'' are almost exclusively gram-positi ...
can resist phagocytosis and even reproduce inside phagocyte
Phagocytes are cells that protect the body by ingesting harmful foreign particles, bacteria, and dead or dying cells. Their name comes from the Greek ', "to eat" or "devour", and "-cyte", the suffix in biology denoting "cell", from the Greek ...
s and kill them. As the disease progresses, the lymph nodes can hemorrhage
Bleeding, hemorrhage, haemorrhage or blood loss, is blood escaping from the circulatory system from damaged blood vessels. Bleeding can occur internally, or externally either through a natural opening such as the mouth, nose, ear, urethra, vag ...
and become swollen and necrotic
Necrosis () is a form of cell injury which results in the premature death of cells in living tissue by autolysis. Necrosis is caused by factors external to the cell or tissue, such as infection, or trauma which result in the unregulated dige ...
. Bubonic plague can progress to lethal septicemic plague
Septicemic plague is one of the three forms of plague, and is caused by '' Yersinia pestis'', a gram-negative species of bacterium. Septicemic plague is a systemic disease involving infection of the blood, and is most commonly spread by bites fro ...
in some cases. The plague is also known to spread to the lungs and become the disease known as the pneumonic plague
Pneumonic plague is a severe lung infection caused by the bacterium ''Yersinia pestis''. Symptoms include fever, headache, shortness of breath, chest pain, and coughing. They typically start about three to seven days after exposure. It is one ...
. Symptoms appear 2–7 days after getting bitten and they include:Sebbane, Florent et al. "Kinetics of disease progression and host response in a rat model of bubonic plague." ''The American journal of pathology'' vol. 166,5 (2005)
* Chills
* General ill feeling (malaise
As a medical term, malaise is a feeling of general discomfort, uneasiness or lack of wellbeing and often the first sign of an infection or other disease. The word has existed in French since at least the 12th century.
The term is often used ...
)
* High fever
Fever, also referred to as pyrexia, is defined as having a body temperature, temperature above the human body temperature, normal range due to an increase in the body's temperature Human body temperature#Fever, set point. There is not a single ...
>
* Muscle cramps
* Seizures
An epileptic seizure, informally known as a seizure, is a period of symptoms due to abnormally excessive or neural oscillation, synchronous neuronal activity in the brain. Outward effects vary from uncontrolled shaking movements involving much o ...
* Smooth, painful lymph gland swelling called a bubo, commonly found in the groin, but may occur in the armpits or neck, most often near the site of the initial infection (bite or scratch)
* Pain may occur in the area before the swelling appears
* Gangrene
Gangrene is a type of tissue death caused by a lack of blood supply. Symptoms may include a change in skin color to red or black, numbness, swelling, pain, skin breakdown, and coolness. The feet and hands are most commonly affected. If the ga ...
of the extremities such as toes, fingers, lips, and tip of the nose.
The best-known symptom of bubonic plague is one or more infected, enlarged, and painful lymph nodes, known as buboes
A bubo (Greek βουβών, ''boubṓn'', 'groin') is adenitis or inflammation of the lymph nodes and is an example of reactive lymphadenopathy.
Classification
Buboes are a symptom of bubonic plague and occur as painful swellings in the thighs ...
. Buboes associated with the bubonic plague are commonly found in the armpits, upper femoral, groin, and neck region. Symptoms include heavy breathing, continuous vomiting of blood (hematemesis
Hematemesis is the vomiting of blood. It is always an important sign. It can be confused with hemoptysis (coughing up blood) or epistaxis (nosebleed), which are more common. The source is generally the upper gastrointestinal tract, typically abo ...
), aching limbs, coughing, and extreme pain caused by the decay or decomposition of the skin while the person is still alive. Additional symptoms include extreme fatigue, gastrointestinal problems, spleen inflammation, lenticulae (black dots scattered throughout the body), delirium, coma
A coma is a deep state of prolonged unconsciousness in which a person cannot be awakened, fails to respond normally to painful stimuli, light, or sound, lacks a normal wake-sleep cycle and does not initiate voluntary actions. Coma patients exhi ...
, organ failure, and death. Organ failure is a result of the bacteria infecting organs through the bloodstream. Other forms of the disease include septicemic plague
Septicemic plague is one of the three forms of plague, and is caused by '' Yersinia pestis'', a gram-negative species of bacterium. Septicemic plague is a systemic disease involving infection of the blood, and is most commonly spread by bites fro ...
and pneumonic plague
Pneumonic plague is a severe lung infection caused by the bacterium ''Yersinia pestis''. Symptoms include fever, headache, shortness of breath, chest pain, and coughing. They typically start about three to seven days after exposure. It is one ...
in which the bacterium reproduces in the person's blood and lungs respectively.
Diagnosis
Laboratory testing is required in order todiagnose
Diagnosis is the identification of the nature and cause of a certain phenomenon. Diagnosis is used in many different disciplines, with variations in the use of logic, analytics, and experience, to determine " cause and effect". In systems enginee ...
and confirm plague. Ideally, confirmation is through the identification of ''Y. pestis'' culture
Culture () is an umbrella term which encompasses the social behavior, institutions, and norms found in human societies, as well as the knowledge, beliefs, arts, laws, customs, capabilities, and habits of the individuals in these groups.Tyl ...
from a patient sample. Confirmation of infection can be done by examining serum taken during the early and late stages of infection
An infection is the invasion of tissues by pathogens, their multiplication, and the reaction of host tissues to the infectious agent and the toxins they produce. An infectious disease, also known as a transmissible disease or communicable dise ...
. To quickly screen for the ''Y. pestis'' antigen
In immunology, an antigen (Ag) is a molecule or molecular structure or any foreign particulate matter or a pollen grain that can bind to a specific antibody or T-cell receptor. The presence of antigens in the body may trigger an immune response. ...
in patients, rapid dipstick
A dipstick is one of several measurement devices.
Some dipsticks are dipped into a liquid to perform a chemical test or to provide a measure of quantity of the liquid.
Since the late 20th century, a flatness/levelness measuring device trademarke ...
tests have been developed for field use. Samples taken for testing include:
* Buboes: Swollen lymph nodes (buboes) characteristic of bubonic plague, a fluid sample can be taken from them with a needle.
* Blood
* Lungs
Samples taken for testing include:
* Buboes: Swollen lymph nodes (buboes) characteristic of bubonic plague, a fluid sample can be taken from them with a needle.
* Blood
* Lungs
Prevention
Bubonic plague outbreaks are controlled by pest control and modern sanitation techniques. This disease uses fleas commonly found on rats as a vector to jump from animals to humans. The mortality rate hits its peak during the hot and humid months of June, July, and August. Furthermore, the plague most affected those of poor upbringing due to greater exposure, poor sanitation techniques and lack of a healthy immune system due to a poor diet. The successful control of rat populations in dense urban areas is essential to outbreak prevention. One example is the use of a machine called the Sulfurozador, used to deliversulphur dioxide
Sulfur dioxide (IUPAC-recommended spelling) or sulphur dioxide (traditional Commonwealth English) is the chemical compound with the formula . It is a toxic gas responsible for the odor of burnt matches. It is released naturally by volcanic activ ...
to eradicate the pest that spread the bubonic plague, in Buenos Aires, Argentina during the early 18th century. Targeted chemoprophylaxis
Chemoprevention (also chemoprophylaxis) refers to the administration of a medication for the purpose of preventing disease or infection. Antibiotics, for example, may be administered to patients with disorders of immune system function to prevent b ...
, sanitation
Sanitation refers to public health conditions related to clean drinking water and treatment and disposal of human excreta and sewage. Preventing human contact with feces is part of sanitation, as is hand washing with soap. Sanitation systems ...
, and vector control
Vector control is any method to limit or eradicate the mammals, birds, insects or other arthropods (here collectively called " vectors") which transmit disease pathogens. The most frequent type of vector control is mosquito control using a varie ...
also played a role in controlling the 2003 Oran
Oran ( ar, وَهران, Wahrān) is a major coastal city located in the north-west of Algeria. It is considered the second most important city of Algeria after the capital Algiers, due to its population and commercial, industrial, and cultural ...
outbreak of the bubonic plague. Another means of prevention in large European cities was a city-wide quarantine to not only limit interaction with people who were infected, but also to limit the interaction with the infected rats.
Treatment
Several classes ofantibiotics
An antibiotic is a type of antimicrobial substance active against bacteria. It is the most important type of antibacterial agent for fighting bacterial infections, and antibiotic medications are widely used in the treatment and prevention o ...
are effective in treating bubonic plague. These include aminoglycoside
Aminoglycoside is a medicinal and bacteriologic category of traditional Gram-negative antibacterial medications that inhibit protein synthesis and contain as a portion of the molecule an amino-modified glycoside (sugar). The term can also refer ...
s such as streptomycin
Streptomycin is an antibiotic medication used to treat a number of bacterial infections, including tuberculosis, ''Mycobacterium avium'' complex, endocarditis, brucellosis, ''Burkholderia'' infection, plague, tularemia, and rat bite fever. Fo ...
and gentamicin
Gentamicin is an antibiotic used to treat several types of bacterial infections. This may include bone infections, endocarditis, pelvic inflammatory disease, meningitis, pneumonia, urinary tract infections, and sepsis among others. It is not e ...
, tetracycline
Tetracycline, sold under various brand names, is an oral antibiotic in the tetracyclines family of medications, used to treat a number of infections, including Acne vulgaris, acne, cholera, brucellosis, plague (disease), plague, malaria, and sy ...
s (especially doxycycline
Doxycycline is a broad-spectrum tetracycline class antibiotic used in the treatment of infections caused by bacteria and certain parasites. It is used to treat bacterial pneumonia, acne, chlamydia infections, Lyme disease, cholera, typhus, an ...
), and the fluoroquinolone
A quinolone antibiotic is a member of a large group of broad-spectrum bacteriocidals that share a bicyclic core structure related to the substance 4-quinolone. They are used in human and veterinary medicine to treat bacterial infections, as wel ...
ciprofloxacin
Ciprofloxacin is a fluoroquinolone antibiotic used to treat a number of bacterial infections. This includes bone and joint infections, intra abdominal infections, certain types of infectious diarrhea, respiratory tract infections, skin inf ...
. Mortality associated with treated cases of bubonic plague is about 1–15%, compared to a mortality of 40–60% in untreated cases.
People potentially infected with the plague need immediate treatment and should be given antibiotics within 24 hours of the first symptoms to prevent death. Other treatments include oxygen, intravenous fluids, and respiratory support. People who have had contact with anyone infected by pneumonic plague are given prophylactic antibiotics. Using the broad-based antibiotic streptomycin has proven to be dramatically successful against the bubonic plague within 12 hours of infection.Echenberg, Myron (2002). Pestis Redux: The Initial Years of the Third Bubonic Plague Pandemic, 1894–1901. Journal of World History, vol 13,2
Epidemiology
Democratic Republic of the Congo
The Democratic Republic of the Congo (french: République démocratique du Congo (RDC), colloquially "La RDC" ), informally Congo-Kinshasa, DR Congo, the DRC, the DROC, or the Congo, and formerly and also colloquially Zaire, is a country in ...
, Madagascar
Madagascar (; mg, Madagasikara, ), officially the Republic of Madagascar ( mg, Repoblikan'i Madagasikara, links=no, ; french: République de Madagascar), is an island country in the Indian Ocean, approximately off the coast of East Africa ...
, and Peru
, image_flag = Flag of Peru.svg
, image_coat = Escudo nacional del Perú.svg
, other_symbol = Great Seal of the State
, other_symbol_type = Seal (emblem), National seal
, national_motto = "Fi ...
.
For over a decade since 2001, Zambia, India, Malawi, Algeria, China, Peru, and the Democratic Republic of the Congo had the most plague cases with over 1,100 cases in the Democratic Republic of the Congo alone. From 1,000 to 2,000 cases are conservatively reported per year to the WHO
Who or WHO may refer to:
* Who (pronoun), an interrogative or relative pronoun
* Who?, one of the Five Ws in journalism
* World Health Organization
Arts and entertainment Fictional characters
* Who, a creature in the Dr. Seuss book '' Horton He ...
. From 2012 to 2017, reflecting political unrest and poor hygienic conditions, Madagascar began to host regular epidemics.
Between 1900 and 2015, the United States had 1,036 human plague cases with an average of 9 cases per year. In 2015, 16 people in the Western United States developed plague, including 2 cases in Yosemite National Park
Yosemite National Park ( ) is an American national park in California, surrounded on the southeast by Sierra National Forest and on the northwest by Stanislaus National Forest. The park is managed by the National Park Service and covers an ar ...
. These US cases usually occur in rural northern New Mexico, northern Arizona, southern Colorado, California, southern Oregon, and far western Nevada.
In November 2017, the Madagascar Ministry of Health reported an outbreak to the WHO (World Health Organization) with more cases and deaths than any recent outbreak in the country. Unusually, most of the cases were pneumonic rather than bubonic.
In June 2018, a child was confirmed to be the first person in Idaho
Idaho ( ) is a state in the Pacific Northwest region of the Western United States. To the north, it shares a small portion of the Canada–United States border with the province of British Columbia. It borders the states of Montana and Wyom ...
to be infected by bubonic plague in nearly 30 years.
A couple died in May 2019, in Mongolia, while hunting marmot
Marmots are large ground squirrels in the genus ''Marmota'', with 15 species living in Asia, Europe, and North America. These herbivores are active during the summer, when they can often be found in groups, but are not seen during the winter, w ...
s. Another two people in the province of Inner Mongolia, China were treated in November 2019 for the disease.
Bayannur
Bayannur or Bayannao'er (; mn, ''Bayannaɣur qota'', Mongolian Cyrillic Баяннуур хот) is a prefecture-level city in western Inner Mongolia, People's Republic of China. Until 1 December 2003, the area was called Bayannur League.
...
, Inner Mongolia
Inner Mongolia, officially the Inner Mongolia Autonomous Region, is an autonomous region of the People's Republic of China. Its border includes most of the length of China's border with the country of Mongolia. Inner Mongolia also accounts for a ...
of China, a human case of bubonic plague was reported. Officials responded by activating a city-wide plague-prevention system for the remainder of the year. Also in July 2020, in Mongolia, a teenager died from bubonic plague after consuming infected marmot meat.
History
''Yersinia pestis'' has been discovered in archaeological finds from the Late Bronze Age (~3800 BP). The bacteria is identified by ancient DNA in human teeth from Asia and Europe dating from 2,800 to 5,000 years ago. Some authors have suggested that the plague was responsible for theNeolithic decline
The Neolithic decline was a rapid collapse in populations between five and six thousand years ago (approximately 3000 BC) during the Neolithic period in western Eurasia. The specific causes of that broad population decline are still debated. While ...
.
First pandemic
The first recorded epidemic affected theSasanian Empire
The Sasanian () or Sassanid Empire, officially known as the Empire of Iranians (, ) and also referred to by historians as the Neo-Persian Empire, was the History of Iran, last Iranian empire before the early Muslim conquests of the 7th-8th cen ...
and their arch-rivals, the Eastern Roman Empire (Byzantine Empire) and was named the Plague of Justinian
The plague of Justinian or Justinianic plague (541–549 AD) was the first recorded major outbreak of the first plague pandemic, the first Old World pandemic of plague, the contagious disease caused by the bacterium ''Yersinia pestis''. The dis ...
after emperor Justinian I
Justinian I (; la, Iustinianus, ; grc-gre, Ἰουστινιανός ; 48214 November 565), also known as Justinian the Great, was the Byzantine emperor from 527 to 565.
His reign is marked by the ambitious but only partly realized ''renovat ...
, who was infected but survived through extensive treatment. The pandemic resulted in the deaths of an estimated 25 million (6th century outbreak) to 50 million people (two centuries of recurrence). The historian Procopius
Procopius of Caesarea ( grc-gre, Προκόπιος ὁ Καισαρεύς ''Prokópios ho Kaisareús''; la, Procopius Caesariensis; – after 565) was a prominent late antique Greek scholar from Caesarea Maritima. Accompanying the Roman gener ...
wrote, in Volume II of ''History of the Wars'', of his personal encounter with the plague and the effect it had on the rising empire. In the spring of 542, the plague arrived in Constantinople, working its way from port city to port city and spreading around the Mediterranean Sea
The Mediterranean Sea is a sea connected to the Atlantic Ocean, surrounded by the Mediterranean Basin and almost completely enclosed by land: on the north by Western and Southern Europe and Anatolia, on the south by North Africa, and on the ea ...
, later migrating inland eastward into Asia Minor and west into Greece and Italy. The Plague of Justinian is said to have been "completed" in the middle of the 8th century. Because the infectious disease spread inland by the transferring of merchandise through Justinian's efforts in acquiring luxurious goods of the time and exporting supplies, his capital became the leading exporter of the bubonic plague. Procopius, in his work ''Secret History'', declared that Justinian was a demon of an emperor who either created the plague himself or was being punished for his sinfulness.
Second pandemic
 In the
In the Late Middle Ages
The Late Middle Ages or Late Medieval Period was the Periodization, period of European history lasting from AD 1300 to 1500. The Late Middle Ages followed the High Middle Ages and preceded the onset of the early modern period (and in much of Eur ...
Europe experienced the deadliest disease outbreak in history when the Black Death, the infamous pandemic of bubonic plague, hit in 1347, killing one-third of the European human population. Some historians believe that society subsequently became more violent as the mass mortality rate cheapened life and thus increased warfare, crime, popular revolt, waves of flagellants, and persecution. The Black Death originated in Central Asia and spread from Italy and then throughout other European countries. Arab historians Ibn Al-Wardni and Almaqrizi believed the Black Death originated in Mongolia. Chinese records also showed a huge outbreak in Mongolia
Mongolia; Mongolian script: , , ; lit. "Mongol Nation" or "State of Mongolia" () is a landlocked country in East Asia, bordered by Russia to the north and China to the south. It covers an area of , with a population of just 3.3 million, ...
in the early 1330s.
In 2022, researchers presented evidence that the plague originated near Lake Issyk-Kul
Issyk-Kul (also Ysyk-Köl, ky, Ысык-Көл, lit=warm lake, translit=Ysyk-Köl, , zh, 伊塞克湖) is an endorheic lake (i.e., without outflow) in the Northern Tian Shan mountains in Eastern Kyrgyzstan. It is the seventh-deepest lake in th ...
in Kyrgyzstan
Kyrgyzstan,, pronounced or the Kyrgyz Republic, is a landlocked country in Central Asia. Kyrgyzstan is bordered by Kazakhstan to the north, Uzbekistan to the west, Tajikistan to the south, and the People's Republic of China to the east. ...
. The Mongols had cut the trade route (the Silk Road
The Silk Road () was a network of Eurasian trade routes active from the second century BCE until the mid-15th century. Spanning over 6,400 kilometers (4,000 miles), it played a central role in facilitating economic, cultural, political, and reli ...
) between China and Europe, which halted the spread of the Black Death from eastern Russia to Western Europe. The European epidemic began with an attack that Mongol
The Mongols ( mn, Монголчууд, , , ; ; russian: Монголы) are an East Asian ethnic group native to Mongolia, Inner Mongolia in China and the Buryatia Republic of the Russian Federation. The Mongols are the principal member of ...
s launched on the Italian merchants' last trading station in the region, Caffa
uk, Феодосія, Теодосія crh, Kefe
, official_name = ()
, settlement_type=
, image_skyline = THEODOSIA 01.jpg
, imagesize = 250px
, image_caption = Genoese fortress of Caffa
, image_shield = Fe ...
in the Crimea
Crimea, crh, Къырым, Qırım, grc, Κιμμερία / Ταυρική, translit=Kimmería / Taurikḗ ( ) is a peninsula in Ukraine, on the northern coast of the Black Sea, that has been occupied by Russia since 2014. It has a pop ...
.
In late 1346, plague broke out among the besiegers and from them penetrated the town. The Mongol forces catapulted plague-infested corpses into Caffa as a form of attack, one of the first known instances of biological warfare. When spring arrived, the Italian merchants fled on their ships, unknowingly carrying the Black Death. Carried by the fleas on rats, the plague initially spread to humans near the Black Sea and then outwards to the rest of Europe as a result of people fleeing from one area to another. Rats migrated with humans, traveling among grain bags, clothing, ships, wagons, and grain husks. Continued research indicates that black rat
The black rat (''Rattus rattus''), also known as the roof rat, ship rat, or house rat, is a common long-tailed rodent of the stereotypical rat genus ''Rattus'', in the subfamily Murinae. It likely originated in the Indian subcontinent, but is n ...
s, those that primarily transmitted the disease, prefer grain as a primary meal. Due to this, the major bulk grain fleets that transported major city's food shipments from Africa and Alexandria
Alexandria ( or ; ar, ٱلْإِسْكَنْدَرِيَّةُ ; grc-gre, Αλεξάνδρεια, Alexándria) is the second largest city in Egypt, and the largest city on the Mediterranean coast. Founded in by Alexander the Great, Alexandria ...
to heavily populated areas, and were then unloaded by hand, played a role in increasing the transmission effectiveness of the plague.
Third pandemic
The plague resurfaced for a third time in the mid-19th century; this is also known as "the modern pandemic". Like the two previous outbreaks, this one also originated inEastern Asia
East Asia is the eastern region of Asia, which is defined in both Geography, geographical and culture, ethno-cultural terms. The modern State (polity), states of East Asia include China, Japan, Mongolia, North Korea, South Korea, and Taiwan. ...
, most likely in Yunnan
Yunnan , () is a landlocked Provinces of China, province in Southwest China, the southwest of the People's Republic of China. The province spans approximately and has a population of 48.3 million (as of 2018). The capital of the province is ...
, a province of China, where there are several natural plague foci. The initial outbreaks
In epidemiology, an outbreak is a sudden increase in occurrences of a disease when cases are in excess of normal expectancy for the location or season. It may affect a small and localized group or impact upon thousands of people across an entire ...
occurred in the second half of the 18th century. The disease remained localized in Southwest China
Southwest China () is a region in the south of the People's Republic of China.
Geography
Southwest China is a rugged and mountainous region, transitioning between the Tibetan Plateau to the west and the Chinese coastal hills (东南丘陵) and ...
for several years before spreading. In the city of Canton, beginning in January 1894, the disease had killed 80,000 people by June. Daily water-traffic with the nearby city of Hong Kong
Hong Kong ( (US) or (UK); , ), officially the Hong Kong Special Administrative Region of the People's Republic of China ( abbr. Hong Kong SAR or HKSAR), is a city and special administrative region of China on the eastern Pearl River Delt ...
rapidly spread the plague there, killing over 2,400 within two months during the 1894 Hong Kong plague.
The third pandemic spread the disease to port cities throughout the world in the second half of the 19th century and the early 20th century via shipping routes. The plague infected people in Chinatown in San Francisco from 1900 to 1904, and in the nearby locales of Oakland
Oakland is the largest city and the county seat of Alameda County, California, United States. A major West Coast port, Oakland is the largest city in the East Bay region of the San Francisco Bay Area, the third largest city overall in the Bay A ...
and the East Bay
The East Bay is the eastern region of the San Francisco Bay Area and includes cities along the eastern shores of the San Francisco Bay and San Pablo Bay. The region has grown to include inland communities in Alameda and Contra Costa countie ...
again from 1907 to 1909. During the former outbreak, in 1902, authorities made permanent the Chinese Exclusion Act
The Chinese Exclusion Act was a United States federal law signed by President Chester A. Arthur on May 6, 1882, prohibiting all immigration of Chinese laborers for 10 years. The law excluded merchants, teachers, students, travelers, and diplom ...
, a law originally signed into existence by President Chester A. Arthur
Chester Alan Arthur (October 5, 1829 – November 18, 1886) was an American lawyer and politician who served as the 21st president of the United States from 1881 to 1885. He previously served as the 20th vice president under President James ...
in 1882. The Act was supposed to last for 10 years, but was renewed in 1892 with the Geary Act
The Geary Act was a United States law that extended the Chinese Exclusion Act of 1882 by adding onerous new requirements. It was written by California Representative Thomas J. Geary and was passed by Congress on .
The law required all Chinese r ...
, then followed by the 1902 decision. The last major outbreak in the United States occurred in Los Angeles in 1924, though the disease is still present in wild rodents and can be passed to humans that come in contact with them. According to the World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level of h ...
, the pandemic was considered active until 1959, when worldwide casualties dropped to 200 per year. In 1994, a plague outbreak in five Indian states caused an estimated 700 infections (including 52 deaths) and triggered a large migration of Indians within India as they tried to avoid the disease.
It was during the 1894 Hong Kong plague outbreak that Alexandre Yersin
Alexandre Emile Jean Yersin (22 September 1863 – 1 March 1943) was a Swiss- French physician and bacteriologist. He is remembered as the co-discoverer of the bacillus responsible for the bubonic plague or pest, which was later named in hi ...
isolated the bacterium responsible (''Yersinia pestis
''Yersinia pestis'' (''Y. pestis''; formerly '' Pasteurella pestis'') is a gram-negative, non-motile, coccobacillus bacterium without spores that is related to both ''Yersinia pseudotuberculosis'' and ''Yersinia enterocolitica''. It is a facult ...
''), a few days after Japanese bacteriologist Kitasato Shibasaburō
Baron was a Japanese physician and bacteriologist. He is remembered as the co-discoverer of the infectious agent of bubonic plague in Hong Kong during an outbreak in 1894, almost simultaneously with Alexandre Yersin.
Kitasato was nominate ...
had isolated it. However, the latter's description was imprecise and also expressed doubts of its relation to the disease, and thus the bacterium is today only named after Yersin.
Society and culture
 The scale of death and social upheaval associated with plague outbreaks has made the topic prominent in many historical and fictional accounts since the disease was first recognized. The
The scale of death and social upheaval associated with plague outbreaks has made the topic prominent in many historical and fictional accounts since the disease was first recognized. The Black Death
The Black Death (also known as the Pestilence, the Great Mortality or the Plague) was a bubonic plague pandemic occurring in Western Eurasia and North Africa from 1346 to 1353. It is the most fatal pandemic recorded in human history, causi ...
in particular is described and referenced in numerous contemporary sources, some of which, including works by Chaucer
Geoffrey Chaucer (; – 25 October 1400) was an English poet, author, and civil servant best known for '' The Canterbury Tales''. He has been called the "father of English literature", or, alternatively, the "father of English poetry". He w ...
, Boccaccio
Giovanni Boccaccio (, , ; 16 June 1313 – 21 December 1375) was an Italian people, Italian writer, poet, correspondent of Petrarch, and an important Renaissance humanism, Renaissance humanist. Born in the town of Certaldo, he became so we ...
, and Petrarch
Francesco Petrarca (; 20 July 1304 – 18/19 July 1374), commonly anglicized as Petrarch (), was a scholar and poet of early Renaissance Italy, and one of the earliest humanists.
Petrarch's rediscovery of Cicero's letters is often credited w ...
, are considered part of the Western canon
The Western canon is the body of high culture literature, music, philosophy, and works of art that are highly valued in the West; works that have achieved the status of classics. However, not all these works originate in the Western world, and ...
. ''The Decameron
''The Decameron'' (; it, label=Italian, Decameron or ''Decamerone'' ), subtitled ''Prince Galehaut'' (Old it, Prencipe Galeotto, links=no ) and sometimes nicknamed ''l'Umana commedia'' ("the Human comedy", as it was Boccaccio that dubbed Dan ...
'', by Boccaccio, is notable for its use of a frame story
A frame is often a structural system that supports other components of a physical construction and/or steel frame that limits the construction's extent.
Frame and FRAME may also refer to:
Physical objects
In building construction
*Framing (con ...
involving individuals who have fled Florence for a secluded villa to escape the Black Death. First-person, sometimes sensationalized or fictionalized, accounts of living through plague years have also been popular across centuries and cultures. For example, Samuel Pepys
Samuel Pepys (; 23 February 1633 – 26 May 1703) was an English diarist and naval administrator. He served as administrator of the Royal Navy and Member of Parliament and is most famous for the diary he kept for a decade. Pepys had no mariti ...
's diary makes several references to his first-hand experiences of the Great Plague of London
The Great Plague of London, lasting from 1665 to 1666, was the last major epidemic of the bubonic plague to occur in England. It happened within the centuries-long Second Pandemic, a period of intermittent bubonic plague epidemics that origi ...
in 1665–6.
Later works, such as Albert Camus
Albert Camus ( , ; ; 7 November 1913 – 4 January 1960) was a French philosopher, author, dramatist, and journalist. He was awarded the 1957 Nobel Prize in Literature at the age of 44, the second-youngest recipient in history. His work ...
's novel '' The Plague'' or Ingmar Bergman
Ernst Ingmar Bergman (14 July 1918 – 30 July 2007) was a Swedish film director, screenwriter, Film producer, producer and playwright. Widely considered one of the greatest and most influential filmmakers of all time, his films are known ...
's film ''The Seventh Seal
''The Seventh Seal'' ( sv, Det sjunde inseglet) is a 1957 Swedish historical fantasy film written and directed by Ingmar Bergman. Set in Sweden during the Black Death, it tells of the journey of a medieval knight (Max von Sydow) and a game of ch ...
'' have used bubonic plague in settings, such as quarantined cities in either medieval or modern times, as a backdrop to explore a variety of concepts. Common themes include the breakdown of society, institutions, and individuals during the plague, the cultural and psychological existential
Existentialism ( ) is a form of philosophical inquiry that explores the problem of human existence and centers on human thinking, feeling, and acting. Existentialist thinkers frequently explore issues related to the meaning, purpose, and valu ...
confrontation with mortality, and the allegorical use of the plague about contemporary moral or spiritual questions.
Biological warfare
Some of the earliest instances of biological warfare were said to have been products of the plague, as armies of the 14th century were recorded catapulting diseased corpses over the walls of towns and villages to spread the pestilence. This was done byJani Beg
Jani Beg ( fa, , tt-Latn, Canibäk), also known as Djanibek Khan, was a Khan of the Golden Horde from 1342 to 1357, succeeding his father Öz Beg Khan.
Reign
With the support of his mother Taydula Khatun, Jani Beg made himself khan after eli ...
when he attacked the city of Kaffa in 1343.
Later, plague was used during the Second Sino-Japanese War
The Second Sino-Japanese War (1937–1945) or War of Resistance (Chinese term) was a military conflict that was primarily waged between the Republic of China and the Empire of Japan. The war made up the Chinese theater of the wider Pacific Th ...
as a bacteriological weapon
Biological warfare, also known as germ warfare, is the use of biological toxins or infectious agents such as bacteria, viruses, insects, and fungi with the intent to kill, harm or incapacitate humans, animals or plants as an act of war. Bio ...
by the Imperial Japanese Army
The was the official ground-based armed force of the Empire of Japan from 1868 to 1945. It was controlled by the Imperial Japanese Army General Staff Office and the Ministry of the Army, both of which were nominally subordinate to the Emperor o ...
. These weapons were provided by Shirō Ishii
Surgeon General was a Japanese microbiologist and army medical officer who served as the director of Unit 731, a biological warfare unit of the Imperial Japanese Army.
Ishii led the development and application of biological weapons at Unit 73 ...
's units
Unit may refer to:
Arts and entertainment
* UNIT, a fictional military organization in the science fiction television series ''Doctor Who''
* Unit of action, a discrete piece of action (or beat) in a theatrical presentation
Music
* Unit (album), ...
and used in experiments on humans before being used in the field. For example, in 1940, the Imperial Japanese Army Air Service
The Imperial Japanese Army Air Service (IJAAS) or Imperial Japanese Army Air Force (IJAAF; ja, 大日本帝國陸軍航空部隊, Dainippon Teikoku Rikugun Kōkūbutai, lit=Greater Japan Empire Army Air Corps) was the aviation force of the Im ...
bombed Ningbo
Ningbo (; Ningbonese: ''gnin² poq⁷'' , Standard Mandarin pronunciation: ), formerly romanized as Ningpo, is a major sub-provincial city in northeast Zhejiang province, People's Republic of China. It comprises 6 urban districts, 2 sate ...
with fleas carrying the bubonic plague. During the Khabarovsk War Crime Trials
The Khabarovsk war crimes trials were the Soviet hearings of twelve Japanese Kwantung Army officers and medical staff charged with the manufacture and use of biological weapons, and human experimentation, during World War II. The war crimes tri ...
, the accused, such as Major General Kiyoshi Kawashima, testified that, in 1941, 40 members of Unit 731
, short for Manshu Detachment 731 and also known as the Kamo Detachment and Ishii Unit, was a covert Biological warfare, biological and chemical warfare research and development unit of the Imperial Japanese Army that engaged in unethical h ...
air-dropped plague
Plague or The Plague may refer to:
Agriculture, fauna, and medicine
*Plague (disease), a disease caused by ''Yersinia pestis''
* An epidemic of infectious disease (medical or agricultural)
* A pandemic caused by such a disease
* A swarm of pe ...
-contaminated fleas on Changde
Changde ( ) is a prefecture-level city in the northwest of Hunan province, People's Republic of China. In addition to the urban districts, Changde also administers the county-level city of Jinshi City, Jinshi and six counties. Changde is adjacent ...
. These operations caused epidemic plague outbreaks.
Continued research
Substantial research has been done regarding the origin of the plague and how it traveled through the continent. Mitochondrial DNA of modern rats in Western Europe indicated that these rats came from two different areas, one being Africa and the other being unclear of a specific origin. The research regarding this pandemic has greatly increased with technology. Through archaeo-molecular investigation, researchers have discovered the DNA of plague bacillus in the dental core of those that fell ill to the plague. Analysis of teeth of the deceased allows researchers to further understand both the demographics and mortuary patterns of the disease. For example, in 2013 in England, archeologists uncovered a burial mound to reveal 17 bodies, mainly children, who had died of the Bubonic plague. They analyzed these burial remains usingradiocarbon dating
Radiocarbon dating (also referred to as carbon dating or carbon-14 dating) is a method for determining the age of an object containing organic material by using the properties of radiocarbon, a radioactive isotope of carbon.
The method was dev ...
to determine they were from the 1530s, and dental core analysis revealed the presence of Yersinia pestis.
Other evidence for rats that are currently still being researched consists of gnaw marks on bones, predator pellets and rat remains that were preserved in situ. This research allows individuals to trace early rat remains to track the path traveled and in turn connect the impact of the Bubonic Plague to specific breeds of rats. Burial sites, known as plague pits, offer archaeologists an opportunity to study the remains of people who died from the plague.
Another research study indicates that these separate pandemics were all interconnected. A current computer model indicates that the disease did not go away in between these pandemics. It rather lurked within the rat population for years without causing human epidemics.
See also
*List of cutaneous conditions
Many skin conditions affect the human integumentary system—the organ system covering the entire surface of the body and composed of skin, hair, nails, and related muscle and glands. The major function of this system is as a barrier against t ...
* List of epidemics
This is a list of the largest known epidemics and pandemics caused by an infectious disease. Widespread non-communicable diseases such as cardiovascular disease and cancer are not included. An epidemic is the rapid spread of disease to a large nu ...
* Miasma theory
The miasma theory (also called the miasmatic theory) is an obsolete medical theory that held that diseases—such as cholera, chlamydia, or the Black Death—were caused by a ''miasma'' (, Ancient Greek for 'pollution'), a noxious form of "bad ...
* Plague (disease)
Plague is an infectious disease caused by the bacterium ''Yersinia pestis''. Symptoms include fever, weakness and headache. Usually this begins one to seven days after exposure. There are three forms of plague, each affecting a different par ...
* Plague doctor
A plague doctor was a physician who treated victims of bubonic plague during epidemics mainly in the 16th and 17th centuries. These physicians were hired by cities to treat infected patients regardless of income, especially the poor that could not ...
References
Further reading
* * * * * * * *External links
{{DEFAULTSORT:Bubonic Plague History of medieval medicine Plague (disease) Rodent-carried diseases Zoonotic bacterial diseases Wikipedia medicine articles ready to translate Wikipedia emergency medicine articles ready to translate