Broadmoor Hospital on:
[Wikipedia]
[Google]
[Amazon]
Broadmoor Hospital is a high-security
 The hospital was first known as the Broadmoor Criminal
The hospital was first known as the Broadmoor Criminal
Report of the Committee of Inquiry into the Personality Disorder Unit, Ashworth Special Hospital
published by the Stationery Office. Accessed 12 November 2007Langlands, Alan (22 May 2000)
Report of the review of security at the high security hospitals
Department of Health. Accessed 12 November 2007 This review was made the personal responsibility of Sir
''

 Much of Broadmoor's architecture is still Victorian, including the gatehouse, which has a clock tower.
Following long-standing reports that the old buildings were unfit for purpose (for therapy or safety), planning permission was granted in 2012 for a £242 million redevelopment, involving a new unit comprising 10 wards to adjoin the existing 6 wards of the modern Paddock Unit, resulting in total bed numbers of 234. Building company Kier reported in 2013 a sum of £115 million for the new unit of 162 beds, ready to accept patients by the start of 2017, and £43 million for a separate new medium secure unit for men nearby.
A new unit called the Paddock Centre already opened on 12 December 2005 to contain and treat patients classed as having a 'dangerous severe personality disorder' (DSPD). This was a new and much debated category invented on behalf of the UK government, based on an individual being considered a 'Grave and Immediate Danger' to the general public, and meeting some combination of criteria for
Much of Broadmoor's architecture is still Victorian, including the gatehouse, which has a clock tower.
Following long-standing reports that the old buildings were unfit for purpose (for therapy or safety), planning permission was granted in 2012 for a £242 million redevelopment, involving a new unit comprising 10 wards to adjoin the existing 6 wards of the modern Paddock Unit, resulting in total bed numbers of 234. Building company Kier reported in 2013 a sum of £115 million for the new unit of 162 beds, ready to accept patients by the start of 2017, and £43 million for a separate new medium secure unit for men nearby.
A new unit called the Paddock Centre already opened on 12 December 2005 to contain and treat patients classed as having a 'dangerous severe personality disorder' (DSPD). This was a new and much debated category invented on behalf of the UK government, based on an individual being considered a 'Grave and Immediate Danger' to the general public, and meeting some combination of criteria for
Accessed 1 November 2012 In 1987 a minister in the
June 2014, ''The Guardian'' After an
First steps to work – a study at Broadmoor Hospital
(119KB). Accessed 2007-06-15
Broadmoor Revealed
Accessed 2011-07-15
Inspection reports
from the
Berkshire Record Office's Broadmoor History pages
Accessed 2011-04-18 * Fallon, Peter; Bluglass, Robert; Edwards, Brian; Daniels, Granville (January 1999
published by The Stationery Office. Accessed 2007-11-12 *Home Office. National offenders management service
Dangerous People with Severe Personality Disorder Programme
Accessed 2007-06-07 *All in the mind (Wednesday 3 March 2004, 5.00 pm). BBC – Live cha
''The rehabilitation of the mentally ill in Broadmoor and elsewhere''
Accessed 2007-05-19
background on Broadmoor Hospital
Architectural listing for Broadmoor Hospital
University of York. Accessed 2007-05-19
BBC News story on scandals and controversy regarding Broadmoor and other secure hospitals
*Together-U
Independent Patients' Advocacy Service
for Broadmoor Hospital. Accessed 2007-06-15 *Fallon, Peter; Bluglass, Robert; Edwards, Brian; Daniels, Granville (January 1999) – overview of the History of the Hospitals in the context of the Ashworth Inquir
Accessed June 2008 {{Authority control Hospitals established in 1863 Buildings and structures in Berkshire Hospitals in Berkshire Bracknell Forest Jimmy Savile NHS hospitals in England Psychiatric hospitals in England 1863 establishments in England
psychiatric hospital
Psychiatric hospitals, also known as mental health hospitals, behavioral health hospitals, are hospitals or wards specializing in the treatment of severe mental disorders, such as schizophrenia, bipolar disorder, eating disorders, dissociat ...
in Crowthorne
Crowthorne is a large village and civil parish in the Bracknell Forest district of south-eastern Berkshire, England. It had a population of 6,711 at the 2001 census, which rose to 6,902 at the 2011 census. A 2020 estimate put it at 7,808. Cr ...
, Berkshire
Berkshire ( ; in the 17th century sometimes spelt phonetically as Barkeshire; abbreviated Berks.) is a historic county in South East England. One of the home counties, Berkshire was recognised by Queen Elizabeth II as the Royal County of Ber ...
, England. It is the oldest of the three high-security psychiatric hospitals in England, the other two being Ashworth Hospital
Ashworth Hospital is a high-security psychiatric hospital in Maghull, 10 miles (16 km) northeast of Liverpool. It is a part of Mersey Care NHS Foundation Trust, catering to patients with psychiatric health needs that require treatment in c ...
near Liverpool and Rampton Secure Hospital
Rampton Secure Hospital is a high-security psychiatric hospital near the village of Woodbeck between Retford and Rampton in Nottinghamshire, England. It is one of three high-security psychiatric hospitals in England, alongside Ashworth Hospita ...
in Nottinghamshire. The hospital's catchment area consists of four National Health Service
The National Health Service (NHS) is the umbrella term for the publicly funded healthcare systems of the United Kingdom (UK). Since 1948, they have been funded out of general taxation. There are three systems which are referred to using the " ...
regions: London
London is the capital and List of urban areas in the United Kingdom, largest city of England and the United Kingdom, with a population of just under 9 million. It stands on the River Thames in south-east England at the head of a estuary dow ...
, Eastern
Eastern may refer to:
Transportation
*China Eastern Airlines, a current Chinese airline based in Shanghai
*Eastern Air, former name of Zambia Skyways
*Eastern Air Lines, a defunct American airline that operated from 1926 to 1991
*Eastern Air Li ...
, South East and South West
The points of the compass are a set of horizontal, radially arrayed compass directions (or azimuths) used in navigation and cartography. A compass rose is primarily composed of four cardinal directions—north, east, south, and west—each sep ...
. It is managed by the West London NHS Trust
West London NHS Trust is aNHS trustwhich provides mental and physical health services to the London boroughs of Ealing, Hammersmith and Fulham and Hounslow. It also provides some services on a national basis, including forensic and high-secur ...
.
History
 The hospital was first known as the Broadmoor Criminal
The hospital was first known as the Broadmoor Criminal Lunatic Asylum
The lunatic asylum (or insane asylum) was an early precursor of the modern psychiatric hospital.
The fall of the lunatic asylum and its eventual replacement by modern psychiatric hospitals explains the rise of organized, institutional psychiatr ...
. Completed in 1863, it was built to a design by Sir Joshua Jebb, an officer of the Corps of Royal Engineers
The Corps of Royal Engineers, usually called the Royal Engineers (RE), and commonly known as the ''Sappers'', is a corps of the British Army. It provides military engineering and other technical support to the British Armed Forces and is head ...
, and covered within its secure perimeter.
The first patient was a female admitted for infanticide
Infanticide (or infant homicide) is the intentional killing of infants or offspring. Infanticide was a widespread practice throughout human history that was mainly used to dispose of unwanted children, its main purpose is the prevention of resou ...
on 27 May 1863. Notes described her as being 'feeble minded'. It has been suggested by an analysis of her records that she most likely had congenital syphilis
Congenital syphilis is syphilis present ''in utero'' and at birth, and occurs when a child is born to a mother with syphilis. Untreated early syphilis infections results in a high risk of poor pregnancy outcomes, including saddle nose, lower extr ...
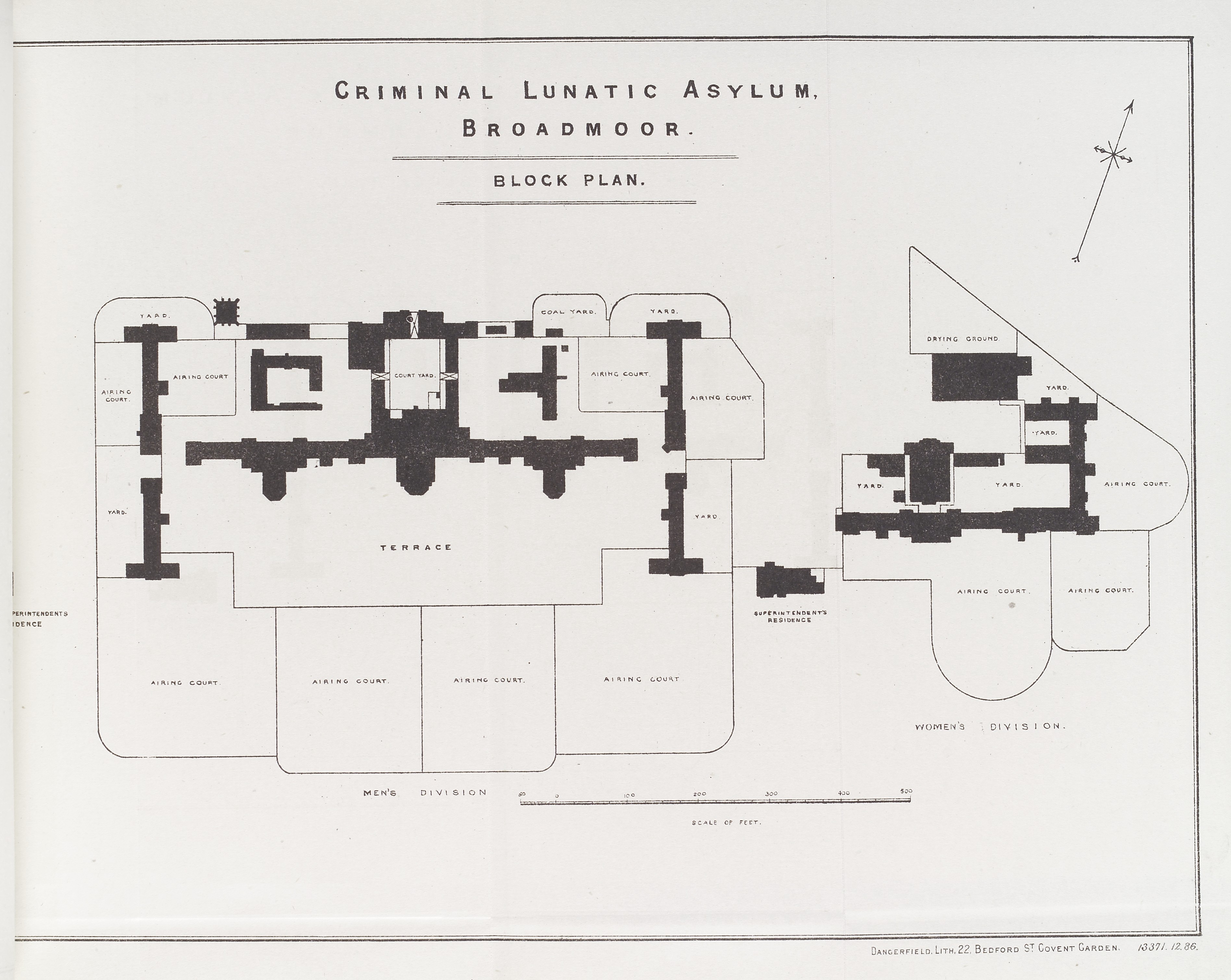
. The first male patients arrived on 27 February 1864. The original building plan of five blocks (four for men and one for women) was completed in 1868. An additional male block was built in 1902.
Due to overcrowding at Broadmoor, an extending asylum branch was constructed at Rampton Secure Hospital
Rampton Secure Hospital is a high-security psychiatric hospital near the village of Woodbeck between Retford and Rampton in Nottinghamshire, England. It is one of three high-security psychiatric hospitals in England, alongside Ashworth Hospita ...
and opened in 1912. Rampton was closed as a branch asylum at the end of 1919 and reopened as an institution for " mental defectives" rather than lunatics. During the First World War
World War I (28 July 1914 11 November 1918), often abbreviated as WWI, was List of wars and anthropogenic disasters by death toll, one of the deadliest global conflicts in history. Belligerents included much of Europe, the Russian Empire, ...
Broadmoor's block 1 was also used as a Prisoner-of-war camp
A prisoner-of-war camp (often abbreviated as POW camp) is a site for the containment of enemy fighters captured by a belligerent power in time of war.
There are significant differences among POW camps, internment camps, and military prisons. ...
, called Crowthorne War Hospital, for mentally ill German soldiers.
After the escape in 1952 of John Straffen
John Thomas Straffen (27 February 1930 – 19 November 2007) was a British serial killer who was the longest-serving prisoner in British history. After killing two young girls in the summer of 1951, he was found unfit to plead at trial and com ...
, who murdered a local child, the hospital set up an alarm system, which is activated to alert people in the vicinity, as well as the public including those in the surrounding towns of Sandhurst, Wokingham
Wokingham is a market town in Berkshire, England, west of London, southeast of Reading, north of Camberley and west of Bracknell.
History
Wokingham means 'Wocca's people's home'. Wocca was apparently a Saxon chieftain who may ...
, Bracknell
Bracknell () is a large town and civil parish in Berkshire, England, the westernmost area within the Greater London Urban Area and the administrative centre of the Borough of Bracknell Forest. It lies to the east of Reading, south of Maiden ...
, Camberley
Camberley is a town in the Borough of Surrey Heath in Surrey, England, approximately south-west of Central London. The town is in the far west of the county, close to the borders of Hampshire and Berkshire. Once part of Windsor Forest, Camb ...
and Bagshot
Bagshot is a town in the Surrey Heath borough of Surrey, England, approximately southwest of central London. In the past, Bagshot served as an important staging post between London, Southampton and the West Country, evidenced by the original ...
, when any potentially dangerous patient escapes. It is based on Second World War
World War II or the Second World War, often abbreviated as WWII or WW2, was a world war that lasted from 1939 to 1945. It involved the vast majority of the world's countries—including all of the great powers—forming two opposi ...
air raid sirens
A civil defense siren, also known as an air-raid siren or tornado siren, is a siren used to provide an emergency population warning to the general population of approaching danger. It is sometimes sounded again to indicate the danger has pas ...
, and a two-tone alarm sounds across the whole area in the event of an escape. Until 2018, it was tested every Monday morning at 10 am for two minutes, after which a single tone 'all-clear' was sounded for a further two minutes. All schools in the area must keep procedures designed to ensure that in the event of a Broadmoor escape no child is ever out of the direct supervision of a member of staff. Sirens were located at Sandhurst School, Wellington College Wellington College may refer to:
* Wellington College, Berkshire, an independent school in Crowthorne, Berkshire, England
** Wellington College International Shanghai
** Wellington College International Tianjin
*Wellington College, Wellington, New ...
, Bracknell Forest Council
Bracknell Forest Council, also known as Bracknell Forest Borough Council is the local authority of Bracknell Forest in Berkshire, England. It is a unitary authority, having the powers of a non-metropolitan county and district council combined.
It ...
depot and other sites until they were decommissioned upon the opening of the hospital's new site.
Following the Peter Fallon QC inquiry into Ashworth Special Hospital which reported in 1999, and found serious concerns about security and abuses resulting from poor management, it was decided to review the security at all three of the special hospitals in England. Until this time each was responsible for maintaining its own security policies.Fallon, Peter; Bluglass, Robert; Edwards, Brian; Daniels, Granville (January 1999Report of the Committee of Inquiry into the Personality Disorder Unit, Ashworth Special Hospital
published by the Stationery Office. Accessed 12 November 2007Langlands, Alan (22 May 2000)
Report of the review of security at the high security hospitals
Department of Health. Accessed 12 November 2007 This review was made the personal responsibility of Sir
Alan Langlands
Sir Robert Alan Langlands FRSE FRCP (Hon.) FRCGP (Hon.) FRCS (Edin.) (Hon.) FRCPSG (Hon.) FFPH FCGI FIA is a former vice-chancellor of the University of Leeds. He is notable for past service as the fourth chief executive of the National ...
, who at the time was chief executive of the NHS England
NHS England, officially the NHS Commissioning Board, is an executive non-departmental public body of the Department of Health and Social Care. It oversees the budget, planning, delivery and day-to-day operation of the commissioning side of the ...
. The report that came out of the review initiated a new partnership whereby the Department of Health sets out a policy of safety, and security directions, that all three special hospitals must adhere to.
In 2003, the Commission for Healthcare Improvement declared the Victorian buildings at Broadmoor Hospital 'unfit for purpose'.
In 2018 the hospital was rated as Good overall by the Care Quality Commission.
Therapies
Broadmoor uses bothpsychiatric medication
A psychiatric or psychotropic medication is a psychoactive drug taken to exert an effect on the chemical makeup of the brain and nervous system. Thus, these medications are used to treat mental illnesses. These medications are typically made of ...
and psychotherapy
Psychotherapy (also psychological therapy, talk therapy, or talking therapy) is the use of psychological methods, particularly when based on regular personal interaction, to help a person change behavior, increase happiness, and overcome pro ...
, as well as occupational therapy. One of the therapies available is the arts, and patients are encouraged to participate in the Koestler Awards Scheme. One of the longest-detained patients at Broadmoor is Albert Haines, who set a legal precedent in 2011 when his mental health tribunal hearing was allowed to be fully public; he argued there that he had never been given the type of counselling he had always sought, and the panel urged the clinicians to work more collaboratively and clearly towards his psychiatric rehabilitation.Broadmoor patient Albert Haines loses appeal bid''
The Independent
''The Independent'' is a British online newspaper. It was established in 1986 as a national morning printed paper. Nicknamed the ''Indy'', it began as a broadsheet and changed to tabloid format in 2003. The last printed edition was publish ...
'', Jerome Taylor, 26 October 2011
The nature of the facility
Because of its high walls and other visible security features, and the news reporting it has received in the past, the hospital is often assumed to be a prison by members of the public. Many of its patients are sent to it via the criminal justice system, and its original design brief incorporated an essence of addressing criminality in addition to mental illness. However, the layout inside and the daily routine are intended to assist the therapy practised there rather than to be run as a prison. Nearly all staff are members of the Prison Officers' Association, as opposed to other health service unions such asUNISON
In music, unison is two or more musical parts that sound either the same pitch or pitches separated by intervals of one or more octaves, usually at the same time. ''Rhythmic unison'' is another term for homorhythm.
Definition
Unison or per ...
and the Royal College of Nursing
The Royal College of Nursing (RCN) is a registered trade union in the United Kingdom for those in the profession of nursing. It was founded in 1916, receiving its royal charter in 1928. Queen Elizabeth II was the patron until her death in 2022. ...
.
Governance
Historical governance
The first medical superintendent was John Meyer. His assistant, William Orange, succeeded him. Orange established "a management style that was greatly admired". He also advised the Home Office on how to approach criminal insanity. Orange was in charge from 1870 to 1886. From its opening, until 1948, Broadmoor was managed by a council of supervision, appointed by and reporting to theHome Secretary
The secretary of state for the Home Department, otherwise known as the home secretary, is a senior minister of the Crown in the Government of the United Kingdom. The home secretary leads the Home Office, and is responsible for all nationa ...
. Thereafter, the Criminal Justice Act of 1948 transferred ownership of the hospital to the Department of Health (and the newly formed NHS) and oversight to the Board of Control for Lunacy and Mental Deficiency
The Board of Control for Lunacy and Mental Deficiency was a body overseeing the treatment of the mentally ill in England and Wales. It was created by the Mental Deficiency Act 1913 to replace the Commissioners in Lunacy, under the Home Office how ...
established under the Mental Deficiency Act 1913. It also renamed the hospital Broadmoor Institution. The hospital remained under direct control of the Department of Health – a situation that reportedly "combined notional central control with actual neglect" – until the establishment of the Special Hospitals Service Authority in 1989, with Charles Kaye as its first chief executive.
Alan Franey ran the hospital from 1989 to 1997, having been recommended for the post by his friend Jimmy Savile
Sir James Wilson Vincent Savile (; 31 October 1926 – 29 October 2011) was an English DJ, television and radio personality who hosted BBC shows including ''Top of the Pops'' and '' Jim'll Fix It''. During his lifetime, he was well kno ...
. His leadership was undermined by persistent rumours of sexual impropriety on the hospital grounds. Allegedly he ignored at least three sexual assaults that he had been informed about.
The Special Hospitals Service Authority was abolished in 1996, being replaced by individual special health authorities in each of the high-security hospitals. The Broadmoor Hospital Authority was itself dissolved on 31 March 2001.
Current governance
On 1 April 2001,West London Mental Health (NHS) Trust
West London NHS Trust is aNHS trustwhich provides mental and physical health services to the London boroughs of Ealing, Hammersmith and Fulham and Hounslow. It also provides some services on a national basis, including forensic and high-securit ...
took over the responsibility for the hospital. The trust reports to the NHS Executive
The National Health Service Executive (NHS Executive) was part of the British Department of Health established in 1996. It advised Ministers on the development of NHS policy and was responsible for the effective management of the NHS. The Executive ...
through NHS England London. The former director, who then became the CEO of the trust, quit in 2009 after Healthcare Commission/Care Quality Commission findings of serious failures to ensure patient safety at Broadmoor. In 2014 the director of specialist and forensic services resigned (and was employed elsewhere in the NHS) just prior to the conclusions of an investigation into a bullying culture. The next permanent CEO retired in 2015 in the wake of poor Care Quality Commission
The Care Quality Commission (CQC) is an executive non-departmental public body of the Department of Health and Social Care of the United Kingdom. It was established in 2009 to regulate and inspect health and social care services in England.
I ...
findings and other problems in the Trust.
A new head of security was appointed in March 2013, John Hourihan, who had thirty years' experience at Scotland Yard
Scotland Yard (officially New Scotland Yard) is the headquarters of the Metropolitan Police, the territorial police force responsible for policing Greater London's 32 boroughs, but not the City of London, the square mile that forms London's ...
and had worked as a bodyguard for members of the royal family.
Meanwhile, the trust allowed ITV to film a two-part documentary within Broadmoor in 2014. Press releases stated that on average there are four 'assaults' per week on staff. Psychiatrist Amlan Basu, clinical director of Broadmoor since March 2014, promoted the documentary but then decided to leave the NHS in 2015 amidst funding and staffing problems, despite the trust having just highlighted investment in his skills through its 'prestigious initiative to improve the quality of patient care in the NHS.'
Buildings

 Much of Broadmoor's architecture is still Victorian, including the gatehouse, which has a clock tower.
Following long-standing reports that the old buildings were unfit for purpose (for therapy or safety), planning permission was granted in 2012 for a £242 million redevelopment, involving a new unit comprising 10 wards to adjoin the existing 6 wards of the modern Paddock Unit, resulting in total bed numbers of 234. Building company Kier reported in 2013 a sum of £115 million for the new unit of 162 beds, ready to accept patients by the start of 2017, and £43 million for a separate new medium secure unit for men nearby.
A new unit called the Paddock Centre already opened on 12 December 2005 to contain and treat patients classed as having a 'dangerous severe personality disorder' (DSPD). This was a new and much debated category invented on behalf of the UK government, based on an individual being considered a 'Grave and Immediate Danger' to the general public, and meeting some combination of criteria for
Much of Broadmoor's architecture is still Victorian, including the gatehouse, which has a clock tower.
Following long-standing reports that the old buildings were unfit for purpose (for therapy or safety), planning permission was granted in 2012 for a £242 million redevelopment, involving a new unit comprising 10 wards to adjoin the existing 6 wards of the modern Paddock Unit, resulting in total bed numbers of 234. Building company Kier reported in 2013 a sum of £115 million for the new unit of 162 beds, ready to accept patients by the start of 2017, and £43 million for a separate new medium secure unit for men nearby.
A new unit called the Paddock Centre already opened on 12 December 2005 to contain and treat patients classed as having a 'dangerous severe personality disorder' (DSPD). This was a new and much debated category invented on behalf of the UK government, based on an individual being considered a 'Grave and Immediate Danger' to the general public, and meeting some combination of criteria for personality disorder
Personality disorders (PD) are a class of mental disorders characterized by enduring maladaptive patterns of behavior, cognition, and inner experience, exhibited across many contexts and deviating from those accepted by the individual's cultu ...
s and/or high scores on the Hare Psychopathy Check list – Revised.
The Paddock Centre was designed to eventually house 72 patients, but never opened more than four of its six 12-bedded wards. The Department of Health
A health department or health ministry is a part of government which focuses on issues related to the general health of the citizenry. Subnational entities, such as states, counties and cities, often also operate a health department of their ow ...
and Ministry of Justice A Ministry of Justice is a common type of government department that serves as a justice ministry.
Lists of current ministries of justice
Named "Ministry"
* Ministry of Justice (Abkhazia)
* Ministry of Justice (Afghanistan)
* Ministry of Just ...
National Personality Disorder Strategy published in October 2011 concluded that the resources invested in the DSPD programme should instead be used in prison based treatment programmes and the DSPD service at Broadmoor was required to close by 31 March 2012.
The trust took possession of the first phase of the new buildings, with 16 wards and 234 beds, in May 2019.
Misconduct by staff
Abuse
From at least 1968 the television presenter and disc jockeyJimmy Savile
Sir James Wilson Vincent Savile (; 31 October 1926 – 29 October 2011) was an English DJ, television and radio personality who hosted BBC shows including ''Top of the Pops'' and '' Jim'll Fix It''. During his lifetime, he was well kno ...
undertook voluntary work at the hospital and was allocated his own room, supported by Broadmoor CEO Pat McGrath, who thought it would be good publicity.''Daily Telegraph'', "Broadmoor staff said Jimmy Savile was a 'psychopath' with a 'liking for children'", 1 November 2012Accessed 1 November 2012 In 1987 a minister in the
Department of Health and Social Security
The Department of Health and Social Security (commonly known as the DHSS) was a ministry of the British government in existence for twenty years from 1968 until 1988, and was headed by the Secretary of State for Health and Social Services.
Hi ...
(DHSS), Baroness Trumpington, appointed Savile to the management board in charge of Broadmoor. He was being referred to as 'Dr Savile' by both the DHSS and Broadmoor, despite having no medical qualifications or training. In August 1988, following a recommendation by Cliff Graham, the senior civil servant in charge of mental health at the DHSS, Savile was appointed by the department's health minister Edwina Currie
Edwina Currie (' Cohen; born 13 October 1946) is a British writer, broadcaster and former politician, serving as Conservative Party Member of Parliament for South Derbyshire from 1983 until 1997. She was a Junior Health Minister for two years ...
to chair an interim task force overseeing the management of the hospital following the suspension of its board. Currie privately supported Savile's attempts to 'blackmail' the Prison Officers Association and publicly declared her 'full confidence' in him.Jimmy Savile: detailed investigation reveals reign of abuse across NHSJune 2014, ''The Guardian'' After an
ITV1
ITV1 (formerly known as ITV) is a British free-to-air public broadcast television channel owned and operated by the British media company ITV plc. It provides the Channel 3 public broadcast service across all of the United Kingdom except for t ...
documentary '' Exposure: The Other Side of Jimmy Savile'' in October 2012, allegations of sexual abuse by Savile were made or re-made by former patients and staff. The civil servant who first proposed Savile's appointment to the task force at Broadmoor, Brian McGinnis, who ran the mental health division of the DHSS in 1987 before Cliff Graham, has since been investigated by police and prevented from working with children.
A Department of Health investigation led by former barrister
A barrister is a type of lawyer in common law jurisdictions. Barristers mostly specialise in courtroom advocacy and litigation. Their tasks include taking cases in superior courts and tribunals, drafting legal pleadings, researching law and ...
Kate Lampard into Savile's activities at Broadmoor and other hospitals and facilities in England, with Bill Kirkup leading the Broadmoor aspects, reported in 2014 that Savile had use of a personal set of keys to Broadmoor from 1968 to 2004 (not formally revoked until 2009), with full unsupervised access to some wards. Eleven allegations of sexual abuse were known; this is thought to be a substantial under-estimate, due to how psychiatric patients in particular were disbelieved or put off from coming forward. In five cases the identity of the alleged victim could not be traced, but of the other six it was concluded they had all been abused by Savile, repeatedly in the case of two patients.
The investigation also concluded that 'the institutional culture in Broadmoor was previously inappropriately tolerant of staff–patient sexual relationships,' and that when there were female patients they were required to undress and bathe in front of staff and sometimes visitors. A 'shocking' failure to ensure a safe or therapeutic environment for female patients had already been revealed in a 2002 inquiry prior to Broadmoor becoming male-only.
In 2010 a female charge nurse received a suspended prison sentence for engaging in sexual activity with a patient at the hospital.
Violating patient confidentiality
Journalists invading the privacy of patients or reporting false information about them have been the subject of dozens of complaints from Broadmoor. Healthcare assistant Robert Neave took payments from '' The Sun'' for several years to provide them with information, including copies of psychiatric reports; this was subsequently investigated byOperation Elveden
Operation Elveden was a British police investigation into allegations of inappropriate payments to police officers and other public officials. It was opened as a result of documents provided by News International to the Operation Weeting investiga ...
. Mental health nurse Kenneth Hall was imprisoned in June 2015 for having repeatedly sold stories to the tabloids based on stolen medical notes and fabricated documents.
Former and current patients
*Michael Adebowale
On the afternoon of 22 May 2013, a British Army soldier, Fusilier Lee Rigby of the Royal Regiment of Fusiliers, was attacked and killed by Michael Adebolajo and Michael Adebowale near the Royal Artillery Barracks in Woolwich, southeast London ...
, Islamic terrorist who was one of two men convicted for the murder of Lee Rigby in 2013.
*Haroon Rashid Aswat
Haroon Rashid Aswat (born in Britain) is a British citizen of South Asian origin with ancestral ethnic roots to Gujarat, born and raised in Yorkshire. American officials allege that he has ties to al Qaeda,
and have sought his extraditi ...
, jihadist wanted by the United States.
*Antony Baekeland, great-grandson of Leo Baekeland
Leo Hendrik Baekeland (November 14, 1863 – February 23, 1944) was a Belgian chemist. He is best known for the inventions of Velox photographic paper in 1893, and Bakelite in 1907. He has been called "The Father of the Plastics Industry" ...
, who stabbed his mother
]
A mother is the female parent of a child. A woman may be considered a mother by virtue of having given childbirth, birth, by raising a child who may or may not be her biological offspring, or by supplying her ovum for fertilisation in the cas ...
to death
* William Rutherford Benn, father of Dame Margaret Rutherford
*Peter Bryan
Peter Bryan (born 4 October 1969) is a British serial killer with schizophrenia who committed three murders between 1993 and 2004.
Early life
Bryan was born in London on 4 October 1969, the youngest of seven children of immigrant parents from ...
, serial killer and cannibal who killed an inmate 10 days after being admitted
*Sharon Carr
Sharon Louise Carr (born 1981), also known as "The Devil's Daughter", is a British woman who is Britain's youngest female murderer. In June 1992, aged only 12, she murdered 18-year-old Katie Rackliff after picking her out at random as she walke ...
, who at age 12 became Britain's youngest female murderer
*David Copeland
The 1999 London nail bombings were a series of bomb explosions in London, England. Over three successive weekends between 17 and 30 April 1999, homemade nail bombs were detonated respectively in Brixton in South London; at Brick Lane, Spitalfiel ...
, who killed three people with homemade nail bombs
*Richard Dadd
Richard Dadd (1 August 1817 – 7 January 1886) was an English painter of the Victorian era, noted for his depictions of fairies and other supernatural subjects, Orientalism, Orientalist scenes, and enigmatic genre works, genre scenes, rendered w ...
, artist
* Gregory Davis, spree killer
* James Kelly, who escaped from the hospital in 1888 after having murdered his wife, and is a Jack the Ripper
Jack the Ripper was an unidentified serial killer active in and around the impoverished Whitechapel district of London, England, in the autumn of 1888. In both criminal case files and the contemporaneous journalistic accounts, the killer wa ...
suspect proposed by later theorists.
*Christiana Edmunds
Christiana Edmunds (3 October 1828 – 19 September 1907), was an English murderer, popularly known as the "Chocolate Cream Killer", who carried out a series of poisonings in Brighton during the early 1870s. Edmunds purchased confectionery from a ...
, the 'Chocolate Cream Poisoner'
*Ibrahim Eidarous
Ibrahim Hussein Abdel Hadi Eidarous () (c. 1957 – July 2008) was an Egyptian militant who was alleged to have led the London-based chapter of al-Jihad. He was held in the custody of the United Kingdom from 1999,
, alleged member of al-Jihad
*Kenneth Erskine
Kenneth Erskine (born 1 July 1963) is a British serial killer who became known as The Stockwell Strangler. He committed the murders of 7–11 senior citizens in London between April and July 1986.
Early life
Erskine was born in Hammersmith''The ...
, serial killer
*Frankie Fraser
Frank Davidson Fraser (13 December 1923 – 26 November 2014), better known as "Mad" Frankie Fraser, was an English gangster who spent 42 years in prison for numerous violent offences.
, gangster
* June and Jennifer Gibbons, known as the silent twins
* Daniel Gonzalez, spree killer
* Ronald Kray, one of the Kray twins
*Thomas John Ley
Thomas John Ley (28 October 188024 July 1947) was an Australian politician who was convicted of murder in England. He is widely suspected to have been involved in the deaths of a number of people in Australia, including political rivals.
Early ...
, politician and murderer committed after a case known as the Chalk Pit Murder
*Robert Maudsley
Robert John Maudsley (born 26 June 1953) is an English serial killer. Maudsley killed four people, with one of the killings taking place in a psychiatric hospital and two in prison after receiving a life sentence for a murder. Initial reports fa ...
, serial killer who tortured and murdered an inmate in the hospital over a period of 9 hours
*Roderick Maclean
Roderick Edward Maclean ( – 8 June 1921) was a Scotsman who attempted to assassinate Queen Victoria on 2 March 1882, at Windsor, England, with a pistol. This was the last of eight attempts by separate people to kill or assault Victoria over a ...
, poet who attempted to assassinate Queen Victoria
Victoria (Alexandrina Victoria; 24 May 1819 – 22 January 1901) was Queen of the United Kingdom of Great Britain and Ireland from 20 June 1837 until Death and state funeral of Queen Victoria, her death in 1901. Her reign of 63 years and 21 ...
*William Chester Minor
William Chester Minor (also known as W. C. Minor; 22 June 1834 – 26 March 1920), was an American army surgeon, psychiatric-hospital patient, and lexicographical researcher.
After serving in the Union Army during the American Civil War, Minor m ...
, amateur lexicographer
Lexicography is the study of lexicons, and is divided into two separate academic disciplines. It is the art of compiling dictionaries.
* Practical lexicography is the art or craft of compiling, writing and editing dictionaries.
* Theoreti ...
known as the Surgeon of Crowthorne
* Daniel M'Naghten, Scottish wood-turner and assassin
* Robert Napper, serial killer
*Edward Oxford
Edward Oxford (18 April 1822 – 23 April 1900) was the first of seven people who tried to assassinate Queen Victoria. After Oxford was arrested and charged with treason, a jury found that Oxford was not guilty by reason of insanity and he ...
, barman who attempted to assassinate Queen Victoria
* Richard Archer Prince, actor and murderer''The New York Times'', 17 December 1897, p. 3
* Nicky Reilly, failed suicide attacker
* Damian Rzeszowski, family murderer
* Charles Salvador, armed robber, born Michael Peterson and formerly known as Charles Bronson
*Nicholas Salvador, convicted of killing Palmira Silva
*John Straffen
John Thomas Straffen (27 February 1930 – 19 November 2007) was a British serial killer who was the longest-serving prisoner in British history. After killing two young girls in the summer of 1951, he was found unfit to plead at trial and com ...
, serial killer who escaped and killed a young girl some hours later
*Peter Sutcliffe
Peter William Sutcliffe (2 June 1946 – 13 November 2020) was an English serial killer who was dubbed the Yorkshire Ripper (an allusion to Jack the Ripper) by the press. Sutcliffe was convicted of murdering 13 women and attempting t ...
, serial killer known as the 'Yorkshire Ripper', survived multiple attempts on his life from other inmates
* Roy Shaw, gangster
*Ronald True
Ronald True (17 June 1891 – 8 January 1951) was an English murderer who was convicted of the 1922 bludgeoning and murder by asphyxiation of a 25-year-old prostitute and call girl named Gertrude Yates. He was initially sentenced to death for Ya ...
, murderer
* Robert Torto, who claimed to be the son of God after killing two men
*Callum Wheeler, moved from HM Prison Belmarsh
His Majesty's Prison Belmarsh is a Category-A men's prison in Thamesmead, south-east London, England. The prison is used in high-profile cases, particularly those concerning national security. Within the prison grounds there is a unique unit ca ...
whilst on remand for the murder of Kent PCSO Julia James in April 2021.
* Barry Williams, spree killer
*Graham Young
Graham Frederick Young (7 September 1947 – 1 August 1990), best known as the Teacup Poisoner and later the St Albans Poisoner, was an English serial killer who used poison to kill his victims.
Obsessed with poisons from an early age, Young be ...
, serial killer
See also
* Ashworth high security hospital *Forensic psychiatry
Forensic psychiatry is a subspeciality of psychiatry and is related to criminology. It encompasses the interface between law and psychiatry. According to the American Academy of Psychiatry and the Law, it is defined as "a subspecialty of psychiat ...
*Bethlem Royal Hospital
Bethlem Royal Hospital, also known as St Mary Bethlehem, Bethlehem Hospital and Bedlam, is a psychiatric hospital in London. Its famous history has inspired several horror books, films and TV series, most notably '' Bedlam'', a 1946 film with ...
References
Further reading
* Dewey Class 365/.942294 19. Sum: authors describe the treatment of some Broadmoor patients and together with their psychiatric and criminal histories. * *The Sainsbury Centre for Mental Health (2006First steps to work – a study at Broadmoor Hospital
(119KB). Accessed 2007-06-15
Broadmoor Revealed
Accessed 2011-07-15
External links
*Inspection reports
from the
Care Quality Commission
The Care Quality Commission (CQC) is an executive non-departmental public body of the Department of Health and Social Care of the United Kingdom. It was established in 2009 to regulate and inspect health and social care services in England.
I ...
Berkshire Record Office's Broadmoor History pages
Accessed 2011-04-18 * Fallon, Peter; Bluglass, Robert; Edwards, Brian; Daniels, Granville (January 1999
published by The Stationery Office. Accessed 2007-11-12 *Home Office. National offenders management service
Dangerous People with Severe Personality Disorder Programme
Accessed 2007-06-07 *All in the mind (Wednesday 3 March 2004, 5.00 pm). BBC – Live cha
''The rehabilitation of the mentally ill in Broadmoor and elsewhere''
Accessed 2007-05-19
background on Broadmoor Hospital
BBC News
BBC News is an operational business division of the British Broadcasting Corporation (BBC) responsible for the gathering and broadcasting of news and current affairs in the UK and around the world. The department is the world's largest broadca ...
*Landscapes & Gardens (2002Architectural listing for Broadmoor Hospital
University of York. Accessed 2007-05-19
BBC News story on scandals and controversy regarding Broadmoor and other secure hospitals
*Together-U
Independent Patients' Advocacy Service
for Broadmoor Hospital. Accessed 2007-06-15 *Fallon, Peter; Bluglass, Robert; Edwards, Brian; Daniels, Granville (January 1999) – overview of the History of the Hospitals in the context of the Ashworth Inquir
Accessed June 2008 {{Authority control Hospitals established in 1863 Buildings and structures in Berkshire Hospitals in Berkshire Bracknell Forest Jimmy Savile NHS hospitals in England Psychiatric hospitals in England 1863 establishments in England