Endocardium on:
[Wikipedia]
[Google]
[Amazon]
 The endocardium is the innermost layer of tissue that lines the chambers of the
The endocardium is the innermost layer of tissue that lines the chambers of the
 The endocardium, which is primarily made up of endothelial cells, controls myocardial function. This modulating role is separate from the homeometric and heterometric regulatory mechanisms that control
The endocardium, which is primarily made up of endothelial cells, controls myocardial function. This modulating role is separate from the homeometric and heterometric regulatory mechanisms that control
 The endocardium is the innermost layer of tissue that lines the chambers of the
The endocardium is the innermost layer of tissue that lines the chambers of the heart
The heart is a muscular organ in most animals. This organ pumps blood through the blood vessels of the circulatory system. The pumped blood carries oxygen and nutrients to the body, while carrying metabolic waste such as carbon dioxide t ...
. Its cells are embryologically and biologically similar to the endothelial
The endothelium is a single layer of squamous endothelial cells that line the interior surface of blood vessels and lymphatic vessels. The endothelium forms an interface between circulating blood or lymph in the lumen and the rest of the vessel ...
cells that line blood vessel
The blood vessels are the components of the circulatory system that transport blood throughout the human body. These vessels transport blood cells, nutrients, and oxygen to the tissues of the body. They also take waste and carbon dioxide away ...
s. The endocardium also provides protection to the valves and heart chambers.
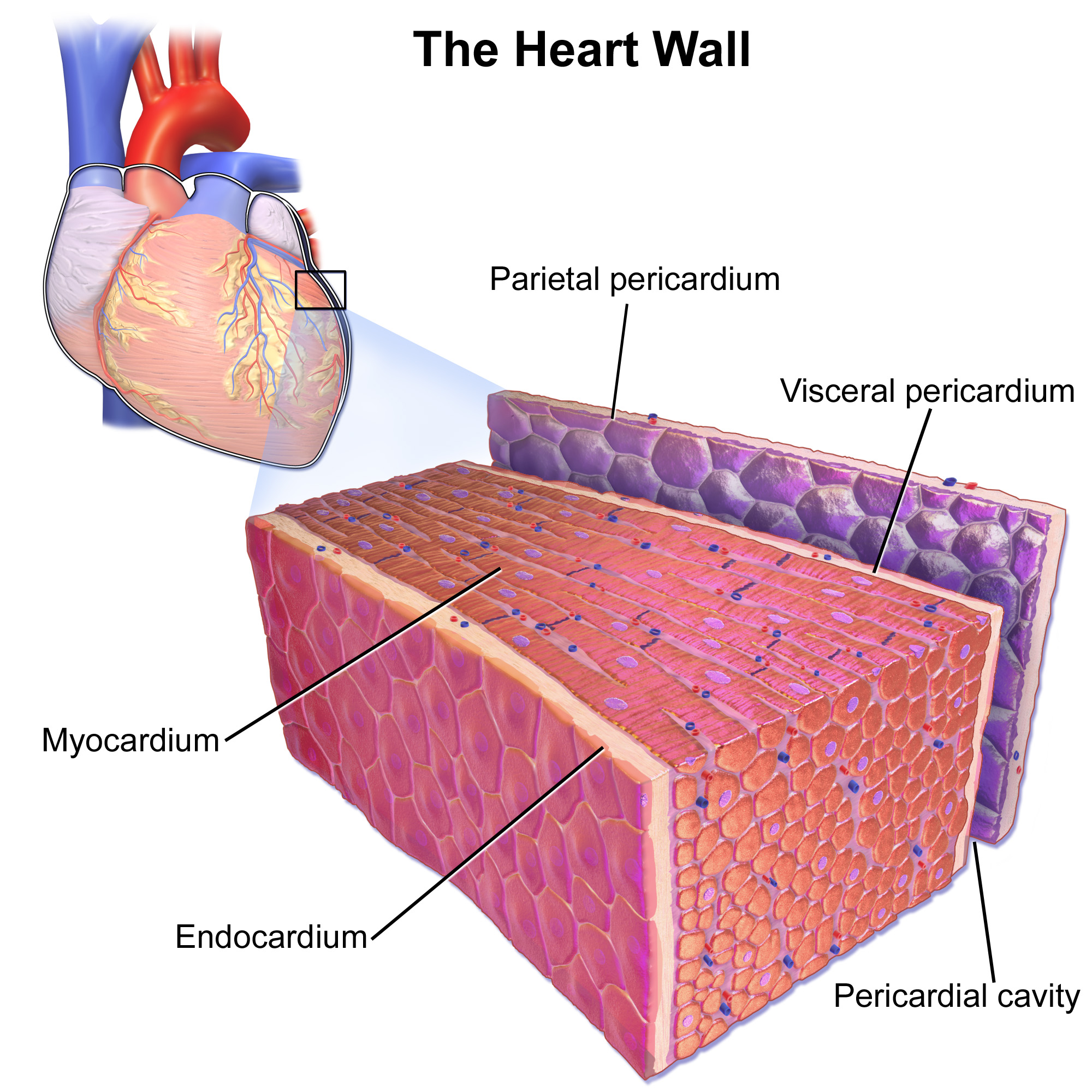
The endocardium underlies the much more voluminous myocardium
Cardiac muscle (also called heart muscle, myocardium, cardiomyocytes and cardiac myocytes) is one of three types of vertebrate muscle tissues, with the other two being skeletal muscle and smooth muscle. It is an involuntary, striated muscle that ...
, the muscular tissue responsible for the contraction of the heart. The outer layer of the heart is termed epicardium
The pericardium, also called pericardial sac, is a double-walled sac containing the heart and the roots of the great vessels. It has two layers, an outer layer made of strong connective tissue (fibrous pericardium), and an inner layer made of ...
and the heart is surrounded by a small amount of fluid enclosed by a fibrous sac called the pericardium
The pericardium, also called pericardial sac, is a double-walled sac containing the heart and the roots of the great vessels. It has two layers, an outer layer made of strong connective tissue (fibrous pericardium), and an inner layer made of ...
.
Function
 The endocardium, which is primarily made up of endothelial cells, controls myocardial function. This modulating role is separate from the homeometric and heterometric regulatory mechanisms that control
The endocardium, which is primarily made up of endothelial cells, controls myocardial function. This modulating role is separate from the homeometric and heterometric regulatory mechanisms that control myocardial contractility Myocardial contractility represents the innate ability of the heart muscle (cardiac muscle or myocardium) to contract. The ability to produce changes in force during contraction result from incremental degrees of binding between different types of t ...
. Moreover, the endothelium of the myocardial (heart muscle) capillaries, which is also closely appositioned to the cardiomyocytes (heart muscle cells), is involved in this modulatory role. Thus, the cardiac endothelium (both the endocardial endothelium and the endothelium of the myocardial capillaries) controls the development of the heart in the embryo as well as in the adult, for example during hypertrophy. Additionally, the contractility and electrophysiological environment of the cardiomyocyte are regulated by the cardiac endothelium.
The endocardial endothelium may also act as a kind of blood–heart barrier (analogous to the blood–brain barrier
The blood–brain barrier (BBB) is a highly selective semipermeable membrane, semipermeable border of endothelium, endothelial cells that prevents solutes in the circulating blood from ''non-selectively'' crossing into the extracellular fluid of ...
), thus controlling the ionic composition of the extracellular fluid in which the cardiomyocytes
Cardiac muscle (also called heart muscle, myocardium, cardiomyocytes and cardiac myocytes) is one of three types of vertebrate muscle tissues, with the other two being skeletal muscle and smooth muscle. It is an involuntary, striated muscle tha ...
bathe.
Clinical significance
Inmyocardial infarction
A myocardial infarction (MI), commonly known as a heart attack, occurs when blood flow decreases or stops to the coronary artery of the heart, causing damage to the heart muscle. The most common symptom is chest pain or discomfort which may ...
, ischemia
Ischemia or ischaemia is a restriction in blood supply to any tissue, muscle group, or organ of the body, causing a shortage of oxygen that is needed for cellular metabolism (to keep tissue alive). Ischemia is generally caused by problems wi ...
of the myocardium
Cardiac muscle (also called heart muscle, myocardium, cardiomyocytes and cardiac myocytes) is one of three types of vertebrate muscle tissues, with the other two being skeletal muscle and smooth muscle. It is an involuntary, striated muscle that ...
starts at the endocardium and might extend up to the epicardium, disrupting the entire heart wall ("transmural" infarction
Infarction is tissue death (necrosis) due to inadequate blood supply to the affected area. It may be caused by artery blockages, rupture, mechanical compression, or vasoconstriction. The resulting lesion is referred to as an infarct
(from the ...
). Less extensive infarctions are often "subendocardial" and do not affect the epicardium. In the acute setting, subendocardial infarctions are more dangerous than transmural infarctions because they create an area of dead tissue surrounded by a boundary region of damaged myocyte
A muscle cell is also known as a myocyte when referring to either a cardiac muscle cell (cardiomyocyte), or a smooth muscle cell as these are both small cells. A skeletal muscle cell is long and threadlike with many nuclei and is called a muscl ...
s. This damaged region will conduct impulses more slowly, resulting in irregular rhythms. The damaged region may enlarge or extend and become more life-threatening. In the chronic setting, transmural infarctions are more dangerous due to the greater amount of muscular damage and the development of scar tissue leading to impaired systolic contractility, impaired diastolic relaxation, and increased risk for rupture and thrombus formation.
During depolarization the impulse is carried from endocardium to epicardium, and during repolarization the impulse moves from epicardium to endocardium.
In infective endocarditis
Infective endocarditis is an infection of the inner surface of the heart, usually the valves. Signs and symptoms may include fever, small areas of bleeding into the skin, heart murmur, feeling tired, and low red blood cell count. Complications ...
, the ''endocardium'' (especially the endocardium lining the heart valve
A heart valve is a one-way valve that allows blood to flow in one direction through the chambers of the heart. Four valves are usually present in a mammalian heart and together they determine the pathway of blood flow through the heart. A heart v ...
s) is affected by bacteria
Bacteria (; singular: bacterium) are ubiquitous, mostly free-living organisms often consisting of one biological cell. They constitute a large domain of prokaryotic microorganisms. Typically a few micrometres in length, bacteria were among ...
.
References
External links
* - "Heart and AV valve" (atrial endocardium) * - "Heart and AV valve" (ventricular endocardium) {{Authority control Cardiac anatomy