Diabetes mellitus on:
[Wikipedia]
[Google]
[Amazon]
Diabetes, also known as diabetes mellitus, is a group of
 The classic symptoms of untreated diabetes are unintended weight loss,
The classic symptoms of untreated diabetes are unintended weight loss,
 All forms of diabetes increase the risk of long-term complications. These typically develop after many years (10–20) but may be the first symptom in those who have otherwise not received a diagnosis before that time.
The major long-term complications relate to damage to
All forms of diabetes increase the risk of long-term complications. These typically develop after many years (10–20) but may be the first symptom in those who have otherwise not received a diagnosis before that time.
The major long-term complications relate to damage to
 Type 1 diabetes is partly inherited, with multiple genes, including certain HLA genotypes, known to influence the risk of diabetes. In genetically susceptible people, the onset of diabetes can be triggered by one or more environmental factors, such as a viral infection or diet. Several viruses have been implicated, but to date there is no stringent evidence to support this hypothesis in humans. Among dietary factors, data suggest that gliadin (a protein present in gluten) may play a role in the development of type 1 diabetes, but the mechanism is not fully understood.
Type 1 diabetes can occur at any age, and a significant proportion is diagnosed during adulthood.
Type 1 diabetes is partly inherited, with multiple genes, including certain HLA genotypes, known to influence the risk of diabetes. In genetically susceptible people, the onset of diabetes can be triggered by one or more environmental factors, such as a viral infection or diet. Several viruses have been implicated, but to date there is no stringent evidence to support this hypothesis in humans. Among dietary factors, data suggest that gliadin (a protein present in gluten) may play a role in the development of type 1 diabetes, but the mechanism is not fully understood.
Type 1 diabetes can occur at any age, and a significant proportion is diagnosed during adulthood.
 Type 2 diabetes is characterized by insulin resistance, which may be combined with relatively reduced insulin secretion. The defective responsiveness of body tissues to insulin is believed to involve the
Type 2 diabetes is characterized by insulin resistance, which may be combined with relatively reduced insulin secretion. The defective responsiveness of body tissues to insulin is believed to involve the
 Insulin is the principal hormone that regulates the uptake of
Insulin is the principal hormone that regulates the uptake of
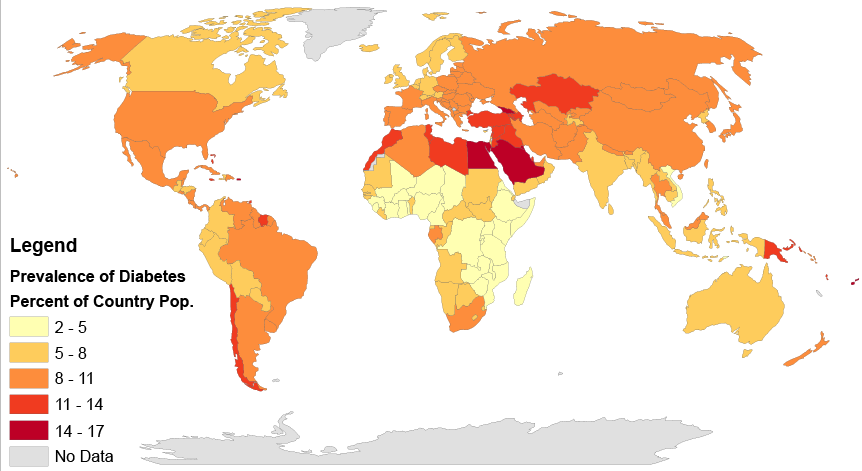
 In 2017, 425 million people had diabetes worldwide, up from an estimated 382 million people in 2013 and from 108 million in 1980. Accounting for the shifting age structure of the global population, the prevalence of diabetes is 8.8% among adults, nearly double the rate of 4.7% in 1980. Type 2 makes up about 90% of the cases. Some data indicate rates are roughly equal in women and men, but male excess in diabetes has been found in many populations with higher type 2 incidence, possibly due to sex-related differences in insulin sensitivity, consequences of obesity and regional body fat deposition, and other contributing factors such as high blood pressure, tobacco smoking, and alcohol intake.
The WHO estimates that diabetes resulted in 1.5 million deaths in 2012, making it the 8th leading cause of death. However another 2.2 million deaths worldwide were attributable to high blood glucose and the increased risks of cardiovascular disease and other associated complications (e.g. kidney failure), which often lead to premature death and are often listed as the underlying cause on death certificates rather than diabetes. For example, in 2017, the
In 2017, 425 million people had diabetes worldwide, up from an estimated 382 million people in 2013 and from 108 million in 1980. Accounting for the shifting age structure of the global population, the prevalence of diabetes is 8.8% among adults, nearly double the rate of 4.7% in 1980. Type 2 makes up about 90% of the cases. Some data indicate rates are roughly equal in women and men, but male excess in diabetes has been found in many populations with higher type 2 incidence, possibly due to sex-related differences in insulin sensitivity, consequences of obesity and regional body fat deposition, and other contributing factors such as high blood pressure, tobacco smoking, and alcohol intake.
The WHO estimates that diabetes resulted in 1.5 million deaths in 2012, making it the 8th leading cause of death. However another 2.2 million deaths worldwide were attributable to high blood glucose and the increased risks of cardiovascular disease and other associated complications (e.g. kidney failure), which often lead to premature death and are often listed as the underlying cause on death certificates rather than diabetes. For example, in 2017, the
American Diabetes Association
IDF Diabetes Atlas
National Diabetes Education Program
ADA's Standards of Medical Care in Diabetes 2019
* * {{DEFAULTSORT:Diabetes Mellitus Wikipedia medicine articles ready to translate Metabolic disorders Wikipedia emergency medicine articles ready to translate Endocrine diseases Cardiovascular diseases Disability by type
metabolic disorder
A metabolic disorder is a disorder that negatively alters the body's processing and distribution of macronutrients, such as proteins, fats, and carbohydrates. Metabolic disorders can happen when abnormal chemical reactions in the body alter t ...
s characterized by a high blood sugar level ( hyperglycemia) over a prolonged period of time. Symptoms often include frequent urination, increased thirst and increased appetite. If left untreated, diabetes can cause many health complications. Acute
Acute may refer to:
Science and technology
* Acute angle
** Acute triangle
** Acute, a leaf shape in the glossary of leaf morphology
* Acute (medicine), a disease that it is of short duration and of recent onset.
** Acute toxicity, the adverse ef ...
complications can include diabetic ketoacidosis, hyperosmolar hyperglycemic state, or death. Serious long-term complications include cardiovascular disease, stroke
A stroke is a disease, medical condition in which poor cerebral circulation, blood flow to the brain causes cell death. There are two main types of stroke: brain ischemia, ischemic, due to lack of blood flow, and intracranial hemorrhage, hemorr ...
, chronic kidney disease, foot ulcers
The foot ( : feet) is an anatomical structure found in many vertebrates. It is the terminal portion of a limb which bears weight and allows locomotion. In many animals with feet, the foot is a separate organ at the terminal part of the leg made ...
, damage to the nerves, damage to the eyes, and cognitive impairment.
Diabetes is due to either the pancreas
The pancreas is an organ of the digestive system and endocrine system of vertebrates. In humans, it is located in the abdomen behind the stomach and functions as a gland. The pancreas is a mixed or heterocrine gland, i.e. it has both an ...
not producing enough insulin, or the cells of the body not responding properly to the insulin produced. Insulin is a hormone which is responsible for helping glucose
Glucose is a simple sugar with the molecular formula . Glucose is overall the most abundant monosaccharide, a subcategory of carbohydrates. Glucose is mainly made by plants and most algae during photosynthesis from water and carbon dioxide, u ...
from food get into cells to be used for energy. There are three main types of diabetes mellitus:
* Type 1 diabetes
Type 1 diabetes (T1D), formerly known as juvenile diabetes, is an autoimmune disease that originates when cells that make insulin (beta cells) are destroyed by the immune system. Insulin is a hormone required for the cells to use blood sugar f ...
results from failure of the pancreas to produce enough insulin due to loss of beta cell
Beta cells (β-cells) are a type of cell found in pancreatic islets that synthesize and secrete insulin and amylin. Beta cells make up 50–70% of the cells in human islets. In patients with Type 1 diabetes, beta-cell mass and function are di ...
s. This form was previously referred to as "insulin-dependent diabetes mellitus" or "juvenile diabetes". The loss of beta cells is caused by an autoimmune response. The cause of this autoimmune response is unknown. Although Type 1 diabetes usually appears during childhood or adolescence, it can also develop in adults.
* Type 2 diabetes begins with insulin resistance, a condition in which cells fail to respond to insulin properly. As the disease progresses, a lack of insulin may also develop. This form was previously referred to as "non insulin-dependent diabetes mellitus" or "adult-onset diabetes". Type 2 diabetes is more common in older adults, but a significant increase in the prevalence of obesity among children has led to more cases of type 2 diabetes in younger people. The most common cause is a combination of excessive body weight and insufficient exercise.
* Gestational diabetes
Gestational diabetes is a condition in which a woman without diabetes develops high blood sugar levels during pregnancy. Gestational diabetes generally results in few symptoms; however, it increases the risk of pre-eclampsia, depression, and ...
is the third main form, and occurs when pregnant women without a previous history of diabetes develop high blood sugar levels. In women with gestational diabetes, blood sugar usually returns to normal soon after delivery. However, women who had gestational diabetes during pregnancy have a higher risk of developing type 2 diabetes later in life.
Type 1 diabetes must be managed with insulin injections. Prevention and treatment of type 2 diabetes involves maintaining a healthy diet, regular physical exercise, a normal body weight, and avoiding use of tobacco. Type 2 diabetes may be treated with oral antidiabetic medications, with or without insulin. Control of blood pressure and maintaining proper foot and eye care are important for people with the disease. Insulin and some oral medications can cause low blood sugar (hypoglycemia). Weight loss surgery in those with obesity
Obesity is a medical condition, sometimes considered a disease, in which excess body fat has accumulated to such an extent that it may negatively affect health. People are classified as obese when their body mass index (BMI)—a person's ...
is sometimes an effective measure in those with type 2 diabetes. Gestational diabetes usually resolves after the birth of the baby.
, an estimated 463 million people had diabetes worldwide (8.8% of the adult population), with type 2 diabetes making up about 90% of the cases. Rates are similar in women and men. Trends suggest that rates will continue to rise. Diabetes at least doubles a person's risk of early death. In 2019, diabetes resulted in approximately 4.2 million deaths. It is the 7th leading cause of death globally. The global economic cost of diabetes-related health expenditure in 2017 was estimated at billion. In the United States, diabetes cost nearly US$327 billion in 2017. Average medical expenditures among people with diabetes are about 2.3 times higher.
Signs and symptoms
polyuria
Polyuria () is excessive or an abnormally large production or passage of urine (greater than 2.5 L or 3 L over 24 hours in adults). Increased production and passage of urine may also be termed diuresis. Polyuria often appears in conjunction wi ...
(increased urination), polydipsia
Polydipsia is excessive thirst or excess drinking.Porth, C. M. (1990). ''Pathophysiology: Concepts of altered health states''. Philadelphia: J.B. Lippincott Company. The word derives from the Greek () "very thirsty", which is derived from (, " ...
(increased thirst), and polyphagia
Polyphagia or hyperphagia is an abnormally strong, incessant sensation of hunger or desire to eat often leading to overeating. In contrast to an increase in appetite following exercise, polyphagia does not subside after eating and often leads t ...
(increased hunger). Symptoms may develop rapidly (weeks or months) in type 1 diabetes, while they usually develop much more slowly and may be subtle or absent in type 2 diabetes.
Several other signs and symptoms can mark the onset of diabetes although they are not specific to the disease. In addition to the known symptoms listed above, they include blurred vision, headache, fatigue, slow healing of cuts, and itchy skin. Prolonged high blood glucose can cause glucose absorption in the lens of the eye, which leads to changes in its shape, resulting in vision changes
A vision disorder is an impairment of the sense of vision.
Vision disorder is not the same as an eye disease. Although many vision disorders do have their immediate cause in the eye, there are many other causes that may occur at other locations in ...
. Long-term vision loss can also be caused by diabetic retinopathy. A number of skin rashes that can occur in diabetes are collectively known as diabetic dermadrome Diabetic dermadromes constitute a group of cutaneous conditions commonly seen in people with diabetes with longstanding disease. Conditions included in this group are:
:* Acral dry gangrene
:* Carotenosis
:* Diabetic dermopathy
:* Diabetic bul ...
s.
Diabetic emergencies
People with diabetes (usually but not exclusively in type 1 diabetes) may also experience diabetic ketoacidosis (DKA), a metabolic disturbance characterized by nausea, vomiting andabdominal pain
Abdominal pain, also known as a stomach ache, is a symptom associated with both non-serious and serious medical issues.
Common causes of pain in the abdomen include gastroenteritis and irritable bowel syndrome. About 15% of people have a m ...
, the smell of acetone
Acetone (2-propanone or dimethyl ketone), is an organic compound with the formula . It is the simplest and smallest ketone (). It is a colorless, highly volatile and flammable liquid with a characteristic pungent odour.
Acetone is miscibl ...
on the breath, deep breathing known as Kussmaul breathing, and in severe cases a decreased level of consciousness. DKA requires emergency treatment in hospital. A rarer but more dangerous condition is hyperosmolar hyperglycemic state (HHS), which is more common in type 2 diabetes and is mainly the result of dehydration
In physiology, dehydration is a lack of total body water, with an accompanying disruption of metabolic processes. It occurs when free water loss exceeds free water intake, usually due to exercise, disease, or high environmental temperature. Mil ...
caused by high blood sugars.
Treatment-related low blood sugar (hypoglycemia) is common in people with type 1 and also type 2 diabetes depending on the medication being used. Most cases are mild and are not considered medical emergencies. Effects can range from feelings of unease, sweating
Perspiration, also known as sweating, is the production of fluids secreted by the sweat glands in the skin of mammals.
Two types of sweat glands can be found in humans: eccrine glands and apocrine glands. The eccrine sweat glands are distri ...
, trembling
A tremor is an involuntary, somewhat rhythmic, muscle contraction and relaxation involving oscillations or twitching movements of one or more body parts. It is the most common of all involuntary movements and can affect the hands, arms, eyes, fa ...
, and increased appetite in mild cases to more serious effects such as confusion, changes in behavior such as aggressiveness, seizures
An epileptic seizure, informally known as a seizure, is a period of symptoms due to abnormally excessive or synchronous neuronal activity in the brain. Outward effects vary from uncontrolled shaking movements involving much of the body with lo ...
, unconsciousness
Unconsciousness is a state in which a living individual exhibits a complete, or near-complete, inability to maintain an awareness of self and environment or to respond to any human or environmental stimulus. Unconsciousness may occur as the r ...
, and rarely permanent brain damage or death in severe cases. Rapid breathing
Tachypnea, also spelt tachypnoea, is a respiratory rate greater than normal, resulting in abnormally rapid and shallow breathing.
In adult humans at rest, any respiratory rate of 1220 per minute is considered clinically normal, with tachypnea b ...
, sweating, and cold, pale skin are characteristic of low blood sugar but not definitive. Mild to moderate cases are self-treated by eating or drinking something high in rapidly absorbed carbohydrates. Severe cases can lead to unconsciousness and must be treated with intravenous glucose or injections with glucagon.
Complications
 All forms of diabetes increase the risk of long-term complications. These typically develop after many years (10–20) but may be the first symptom in those who have otherwise not received a diagnosis before that time.
The major long-term complications relate to damage to
All forms of diabetes increase the risk of long-term complications. These typically develop after many years (10–20) but may be the first symptom in those who have otherwise not received a diagnosis before that time.
The major long-term complications relate to damage to blood vessel
The blood vessels are the components of the circulatory system that transport blood throughout the human body. These vessels transport blood cells, nutrients, and oxygen to the tissues of the body. They also take waste and carbon dioxide awa ...
s. Diabetes doubles the risk of cardiovascular disease and about 75% of deaths in people with diabetes are due to coronary artery disease. Other macrovascular disease
Macrovascular disease is a disease of any large (''macro'') blood vessels in the body. It is a disease of the large blood vessels, including the coronary arteries, the aorta, and the sizable arteries in the brain and in the limbs.
This sometimes ...
s include stroke
A stroke is a disease, medical condition in which poor cerebral circulation, blood flow to the brain causes cell death. There are two main types of stroke: brain ischemia, ischemic, due to lack of blood flow, and intracranial hemorrhage, hemorr ...
, and peripheral artery disease. These complications are also a strong risk factor for severe COVID-19
Coronavirus disease 2019 (COVID-19) is a contagious disease caused by a virus, the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). The first known case was identified in Wuhan, China, in December 2019. The disease quick ...
illness.
The primary complications of diabetes due to damage in small blood vessels include damage to the eyes, kidneys, and nerves. Damage to the eyes, known as diabetic retinopathy, is caused by damage to the blood vessels in the retina
The retina (from la, rete "net") is the innermost, light-sensitive layer of tissue of the eye of most vertebrates and some molluscs. The optics of the eye create a focused two-dimensional image of the visual world on the retina, which the ...
of the eye, and can result in gradual vision loss
Visual impairment, also known as vision impairment, is a medical definition primarily measured based on an individual's better eye visual acuity; in the absence of treatment such as correctable eyewear, assistive devices, and medical treatment� ...
and eventual blindness
Visual impairment, also known as vision impairment, is a medical definition primarily measured based on an individual's better eye visual acuity; in the absence of treatment such as correctable eyewear, assistive devices, and medical treatment� ...
. Diabetes also increases the risk of having glaucoma
Glaucoma is a group of eye diseases that result in damage to the optic nerve (or retina) and cause vision loss. The most common type is open-angle (wide angle, chronic simple) glaucoma, in which the drainage angle for aqueous humor, fluid withi ...
, cataracts, and other eye problems. It is recommended that people with diabetes visit an eye doctor once a year. Damage to the kidneys, known as diabetic nephropathy, can lead to tissue scarring, urine protein loss, and eventually chronic kidney disease, sometimes requiring dialysis or kidney transplantation. Damage to the nerves of the body, known as diabetic neuropathy, is the most common complication of diabetes. The symptoms can include numbness, tingling
Paresthesia is an abnormal sensation of the skin (tingling, pricking, chilling, burning, numbness) with no apparent physical cause. Paresthesia may be transient or chronic, and may have any of dozens of possible underlying causes. Paresthesias a ...
, sudomotor dysfunction, pain, and altered pain sensation, which can lead to damage to the skin. Diabetes-related foot problems (such as diabetic foot ulcers) may occur, and can be difficult to treat, occasionally requiring amputation. Additionally, proximal diabetic neuropathy causes painful muscle atrophy and weakness
Weakness is a symptom of a number of different conditions. The causes are many and can be divided into conditions that have true or perceived muscle weakness. True muscle weakness is a primary symptom of a variety of skeletal muscle diseases, i ...
.
There is a link between cognitive deficit
Cognitive deficit is an inclusive term to describe any characteristic that acts as a barrier to the cognition process.
The term may describe
* deficits in overall intelligence (as with intellectual disabilities),
* specific and restricted defic ...
and diabetes. Compared to those without diabetes, those with the disease have a 1.2 to 1.5-fold greater rate of decline in cognitive function. Having diabetes, especially when on insulin, increases the risk of falls in older people.
Causes
Diabetes mellitus is classified into six categories:type 1 diabetes
Type 1 diabetes (T1D), formerly known as juvenile diabetes, is an autoimmune disease that originates when cells that make insulin (beta cells) are destroyed by the immune system. Insulin is a hormone required for the cells to use blood sugar f ...
, type 2 diabetes, hybrid forms of diabetes, hyperglycemia first detected during pregnancy, "unclassified diabetes", and "other specific types". "Hybrid forms of diabetes" include slowly evolving, immune-mediated diabetes of adults and ketosis-prone type 2 diabetes. "Hyperglycemia first detected during pregnancy" includes gestational diabetes mellitus and diabetes mellitus in pregnancy (type 1 or type 2 diabetes first diagnosed during pregnancy). The "other specific types" are a collection of a few dozen individual causes. Diabetes is a more variable disease than once thought and people may have combinations of forms.
Type 1
Type 1 diabetes is characterized by loss of the insulin-producingbeta cell
Beta cells (β-cells) are a type of cell found in pancreatic islets that synthesize and secrete insulin and amylin. Beta cells make up 50–70% of the cells in human islets. In patients with Type 1 diabetes, beta-cell mass and function are di ...
s of the pancreatic islets, leading to insulin deficiency. This type can be further classified as immune-mediated or idiopathic. The majority of type 1 diabetes is of an immune-mediated nature, in which a T cell-mediated autoimmune attack leads to the loss of beta cells and thus insulin. It causes approximately 10% of diabetes mellitus cases in North America and Europe. Most affected people are otherwise healthy and of a healthy weight when onset occurs. Sensitivity and responsiveness to insulin are usually normal, especially in the early stages. Although it has been called "juvenile diabetes" due to the frequent onset in children, the majority of individuals living with type 1 diabetes are now adults.
"Brittle" diabetes, also known as unstable diabetes or labile diabetes, is a term that was traditionally used to describe the dramatic and recurrent swings in glucose
Glucose is a simple sugar with the molecular formula . Glucose is overall the most abundant monosaccharide, a subcategory of carbohydrates. Glucose is mainly made by plants and most algae during photosynthesis from water and carbon dioxide, u ...
levels, often occurring for no apparent reason in insulin-dependent diabetes. This term, however, has no biologic basis and should not be used. Still, type 1 diabetes can be accompanied by irregular and unpredictable high blood sugar levels, and the potential for diabetic ketoacidosis or serious low blood sugar levels. Other complications include an impaired counterregulatory response to low blood sugar, infection, gastroparesis (which leads to erratic absorption of dietary carbohydrates), and endocrinopathies (e.g., Addison's disease
Addison's disease, also known as primary adrenal insufficiency, is a rare long-term endocrine disorder characterized by inadequate production of the steroid hormones cortisol and aldosterone by the two outer layers of the cells of the adrena ...
). These phenomena are believed to occur no more frequently than in 1% to 2% of persons with type 1 diabetes.
 Type 1 diabetes is partly inherited, with multiple genes, including certain HLA genotypes, known to influence the risk of diabetes. In genetically susceptible people, the onset of diabetes can be triggered by one or more environmental factors, such as a viral infection or diet. Several viruses have been implicated, but to date there is no stringent evidence to support this hypothesis in humans. Among dietary factors, data suggest that gliadin (a protein present in gluten) may play a role in the development of type 1 diabetes, but the mechanism is not fully understood.
Type 1 diabetes can occur at any age, and a significant proportion is diagnosed during adulthood.
Type 1 diabetes is partly inherited, with multiple genes, including certain HLA genotypes, known to influence the risk of diabetes. In genetically susceptible people, the onset of diabetes can be triggered by one or more environmental factors, such as a viral infection or diet. Several viruses have been implicated, but to date there is no stringent evidence to support this hypothesis in humans. Among dietary factors, data suggest that gliadin (a protein present in gluten) may play a role in the development of type 1 diabetes, but the mechanism is not fully understood.
Type 1 diabetes can occur at any age, and a significant proportion is diagnosed during adulthood. Latent autoimmune diabetes of adults
Slowly evolving immune-mediated diabetes, or latent autoimmune diabetes in adults (LADA), is a form of diabetes that exhibits clinical features similar to both type 1 diabetes (T1D) and type 2 diabetes (T2D), and is sometimes referred to as typ ...
(LADA) is the diagnostic term applied when type 1 diabetes develops in adults; it has a slower onset than the same condition in children. Given this difference, some use the unofficial term "type 1.5 diabetes" for this condition. Adults with LADA are frequently initially misdiagnosed as having type 2 diabetes, based on age rather than a cause.
Type 2
 Type 2 diabetes is characterized by insulin resistance, which may be combined with relatively reduced insulin secretion. The defective responsiveness of body tissues to insulin is believed to involve the
Type 2 diabetes is characterized by insulin resistance, which may be combined with relatively reduced insulin secretion. The defective responsiveness of body tissues to insulin is believed to involve the insulin receptor
The insulin receptor (IR) is a transmembrane receptor that is activated by insulin, IGF-I, IGF-II and belongs to the large class of receptor tyrosine kinase. Metabolically, the insulin receptor plays a key role in the regulation of glucose ho ...
. However, the specific defects are not known. Diabetes mellitus cases due to a known defect are classified separately. Type 2 diabetes is the most common type of diabetes mellitus accounting for 95% of diabetes. Many people with type 2 diabetes have evidence of prediabetes (impaired fasting glucose and/or impaired glucose tolerance) before meeting the criteria for type 2 diabetes. The progression of prediabetes to overt type 2 diabetes can be slowed or reversed by lifestyle changes or medications that improve insulin sensitivity or reduce the liver's glucose production.
Type 2 diabetes is primarily due to lifestyle factors and genetics. A number of lifestyle factors are known to be important to the development of type 2 diabetes, including obesity
Obesity is a medical condition, sometimes considered a disease, in which excess body fat has accumulated to such an extent that it may negatively affect health. People are classified as obese when their body mass index (BMI)—a person's ...
(defined by a body mass index of greater than 30), lack of physical activity
Physical activity is defined as any voluntary bodily movement produced by skeletal muscles that requires energy expenditure.Global Recommendations on Physical Activity for Health, 2009. World Health Organization. Geneva, Switzerland. Accessed 13/ ...
, poor diet, stress, and urbanization
Urbanization (or urbanisation) refers to the population shift from rural to urban areas, the corresponding decrease in the proportion of people living in rural areas, and the ways in which societies adapt to this change. It is predominantly th ...
. Excess body fat is associated with 30% of cases in people of Chinese and Japanese descent, 60–80% of cases in those of European and African descent, and 100% of Pima Indians and Pacific Islanders. Even those who are not obese may have a high waist–hip ratio.
Dietary factors such as sugar
Sugar is the generic name for sweet-tasting, soluble carbohydrates, many of which are used in food. Simple sugars, also called monosaccharides, include glucose, fructose, and galactose. Compound sugars, also called disaccharides or do ...
-sweetened drinks are associated with an increased risk. The type of fats in the diet is also important, with saturated fat and trans fats increasing the risk and polyunsaturated and monounsaturated fat decreasing the risk. Eating white rice excessively may increase the risk of diabetes, especially in Chinese and Japanese people. Lack of physical activity may increase the risk of diabetes in some people.
Adverse childhood experiences, including abuse, neglect, and household difficulties, increase the likelihood of type 2 diabetes later in life by 32%, with neglect
In the context of caregiving, neglect is a form of abuse where the perpetrator, who is responsible for caring for someone who is unable to care for themselves, fails to do so. It can be a result of carelessness, indifference, or unwillingness a ...
having the strongest effect.
Antipsychotic medication
Antipsychotics, also known as neuroleptics, are a class of psychotropic medication primarily used to manage psychosis (including delusions, hallucinations, paranoia or disordered thought), principally in schizophrenia but also in a range of oth ...
side effects (specifically metabolic abnormalities, dyslipidemia and weight gain) and unhealthy lifestyles (including poor diet and decreased physical activity
Physical activity is defined as any voluntary bodily movement produced by skeletal muscles that requires energy expenditure.Global Recommendations on Physical Activity for Health, 2009. World Health Organization. Geneva, Switzerland. Accessed 13/ ...
), are potential risk factors.
Gestational diabetes
Gestational diabetes resembles type 2 diabetes in several respects, involving a combination of relatively inadequate insulin secretion and responsiveness. It occurs in about 2–10% of all pregnancies and may improve or disappear after delivery. It is recommended that all pregnant women get tested starting around 24–28 weeks gestation. It is most often diagnosed in the second or third trimester because of the increase in insulin-antagonist hormone levels that occurs at this time. However, after pregnancy approximately 5–10% of women with gestational diabetes are found to have another form of diabetes, most commonly type 2. Gestational diabetes is fully treatable, but requires careful medical supervision throughout the pregnancy. Management may include dietary changes, blood glucose monitoring, and in some cases, insulin may be required. Though it may be transient, untreated gestational diabetes can damage the health of the fetus or mother. Risks to the baby include macrosomia (high birth weight), congenital heart andcentral nervous system
The central nervous system (CNS) is the part of the nervous system consisting primarily of the brain and spinal cord. The CNS is so named because the brain integrates the received information and coordinates and influences the activity of all p ...
abnormalities, and skeletal muscle malformations. Increased levels of insulin in a fetus's blood may inhibit fetal surfactant production and cause infant respiratory distress syndrome
Infantile respiratory distress syndrome (IRDS), also called respiratory distress syndrome of newborn, or increasingly surfactant deficiency disorder (SDD), and previously called hyaline membrane disease (HMD), is a syndrome in premature infants ...
. A high blood bilirubin level may result from red blood cell destruction. In severe cases, perinatal death may occur, most commonly as a result of poor placental perfusion due to vascular impairment. Labor induction
Labor induction is the process or treatment that stimulates childbirth and delivery. Inducing (starting) labor can be accomplished with pharmaceutical or non-pharmaceutical methods. In Western countries, it is estimated that one-quarter of pregna ...
may be indicated with decreased placental function. A caesarean section may be performed if there is marked fetal distress or an increased risk of injury associated with macrosomia, such as shoulder dystocia.
Other types
Maturity onset diabetes of the young
Maturity-onset diabetes of the young (MODY) refers to any of several hereditary forms of diabetes mellitus caused by mutations in an autosomal dominant gene disrupting insulin production. MODY is often referred to as monogenic diabetes to disting ...
(MODY) is a rare autosomal dominant inherited form of diabetes, due to one of several single-gene mutations causing defects in insulin production. It is significantly less common than the three main types, constituting 1–2% of all cases. The name of this disease refers to early hypotheses as to its nature. Being due to a defective gene, this disease varies in age at presentation and in severity according to the specific gene defect; thus, there are at least 13 subtypes of MODY. People with MODY often can control it without using insulin.
Some cases of diabetes are caused by the body's tissue receptors not responding to insulin (even when insulin levels are normal, which is what separates it from type 2 diabetes); this form is very uncommon. Genetic mutations ( autosomal or mitochondrial) can lead to defects in beta cell function. Abnormal insulin action may also have been genetically determined in some cases. Any disease that causes extensive damage to the pancreas may lead to diabetes (for example, chronic pancreatitis and cystic fibrosis). Diseases associated with excessive secretion of insulin-antagonistic hormone
A hormone (from the Greek participle , "setting in motion") is a class of signaling molecules in multicellular organisms that are sent to distant organs by complex biological processes to regulate physiology and behavior. Hormones are required ...
s can cause diabetes (which is typically resolved once the hormone excess is removed). Many drugs impair insulin secretion and some toxins damage pancreatic beta cells, whereas others increase insulin resistance (especially glucocorticoids which can provoke "steroid diabetes
Steroid diabetes is a medical term referring to prolonged hyperglycemia due to glucocorticoid therapy for another medical condition. It is usually, but not always, a transient condition.
Cause
The most common glucocorticoids which cause steroi ...
"). The ICD-10
ICD-10 is the 10th revision of the International Statistical Classification of Diseases and Related Health Problems (ICD), a medical classification list by the World Health Organization (WHO). It contains codes for diseases, signs and symptoms ...
(1992) diagnostic entity, ''malnutrition-related diabetes mellitus'' (ICD-10 code E12), was deprecated by the World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level o ...
(WHO) when the current taxonomy was introduced in 1999.
Yet another form of diabetes that people may develop is double diabetes. This is when a type 1 diabetic becomes insulin resistant, the hallmark for type 2 diabetes or has a family history for type 2 diabetes. It was first discovered in 1990 or 1991.
The following is a list of disorders that may increase the risk of diabetes:Unless otherwise specified, reference is: Table 20-5 in
* Genetic defects of β-cell function
** Maturity onset diabetes of the young
Maturity-onset diabetes of the young (MODY) refers to any of several hereditary forms of diabetes mellitus caused by mutations in an autosomal dominant gene disrupting insulin production. MODY is often referred to as monogenic diabetes to disting ...
** Mitochondrial DNA mutations
* Genetic defects in insulin processing or insulin action
** Defects in proinsulin conversion
** Insulin gene mutations
** Insulin receptor mutations
* Exocrine pancreatic defects (see Type 3c diabetes
Type 3c diabetes (also known as pancreatogenic diabetes) is diabetes that comes secondary to pancreatic diseases, involving the exocrine and digestive functions of the pancreas.
Around 5–10% of cases of diabetes in the Western world are related ...
, i.e. pancreatogenic diabetes)
** Chronic pancreatitis
** Pancreatectomy
** Pancreatic neoplasia
Pancreatic cancer arises when cells in the pancreas, a glandular organ behind the stomach, begin to multiply out of control and form a mass. These cancerous cells have the ability to invade other parts of the body. A number of types of pancr ...
** Cystic fibrosis
** Hemochromatosis
Iron overload or hemochromatosis (also spelled ''haemochromatosis'' in British English) indicates increased total accumulation of iron in the body from any cause and resulting organ damage. The most important causes are hereditary haemochromatosi ...
** Fibrocalculous pancreatopathy Fibrocalculous pancreatopathy (FCPP) is a secondary form of diabetes mellitus of unresolved etiology that has historically been considered an issue specific to the impoverished agricultural tropics of India, but also occurs in the countries of Bang ...
* Endocrinopathies
** Growth hormone excess ( acromegaly)
** Cushing syndrome
** Hyperthyroidism
Hyperthyroidism is the condition that occurs due to excessive production of thyroid hormones by the thyroid gland. Thyrotoxicosis is the condition that occurs due to excessive thyroid hormone of any cause and therefore includes hyperthyroidis ...
** Hypothyroidism
** Pheochromocytoma
Pheochromocytoma (PHEO or PCC) is a rare tumor of the adrenal medulla composed of chromaffin cells, also known as pheochromocytes. When a tumor composed of the same cells as a pheochromocytoma develops outside the adrenal gland, it is referred t ...
** Glucagonoma
* Infections
** Cytomegalovirus infection
''Cytomegalovirus'' (''CMV'') (from ''cyto-'' 'cell' via Greek - 'container' + 'big, megalo-' + -''virus'' via Latin 'poison') is a genus of viruses in the order ''Herpesvirales'', in the family ''Herpesviridae'', in the subfamily ''Betaherpe ...
** Coxsackievirus B
* Drugs
** Glucocorticoids
** Thyroid hormone
** β-adrenergic agonists
** Statins
Pathophysiology
 Insulin is the principal hormone that regulates the uptake of
Insulin is the principal hormone that regulates the uptake of glucose
Glucose is a simple sugar with the molecular formula . Glucose is overall the most abundant monosaccharide, a subcategory of carbohydrates. Glucose is mainly made by plants and most algae during photosynthesis from water and carbon dioxide, u ...
from the blood into most cells of the body, especially liver, adipose tissue and muscle, except smooth muscle, in which insulin acts via the IGF-1. Therefore, deficiency of insulin or the insensitivity of its receptors play a central role in all forms of diabetes mellitus.
The body obtains glucose from three main sources: the intestinal absorption of food; the breakdown of glycogen ( glycogenolysis), the storage form of glucose found in the liver; and gluconeogenesis, the generation of glucose from non-carbohydrate substrates in the body. Insulin plays a critical role in regulating glucose levels in the body. Insulin can inhibit the breakdown of glycogen or the process of gluconeogenesis, it can stimulate the transport of glucose into fat and muscle cells, and it can stimulate the storage of glucose in the form of glycogen.
Insulin is released into the blood by beta cells (β-cells), found in the islets of Langerhans in the pancreas, in response to rising levels of blood glucose, typically after eating. Insulin is used by about two-thirds of the body's cells to absorb glucose from the blood for use as fuel, for conversion to other needed molecules, or for storage. Lower glucose levels result in decreased insulin release from the beta cells and in the breakdown of glycogen to glucose. This process is mainly controlled by the hormone glucagon, which acts in the opposite manner to insulin.
If the amount of insulin available is insufficient, or if cells respond poorly to the effects of insulin ( insulin resistance), or if the insulin itself is defective, then glucose is not absorbed properly by the body cells that require it, and is not stored appropriately in the liver and muscles. The net effect is persistently high levels of blood glucose, poor protein synthesis, and other metabolic derangements, such as metabolic acidosis
Acidosis is a process causing increased acidity in the blood and other body tissues (i.e., an increase in hydrogen ion concentration). If not further qualified, it usually refers to acidity of the blood plasma.
The term ''acidemia'' describe ...
in cases of complete insulin deficiency.
When glucose concentration in the blood remains high over time, the kidneys reach a threshold of reabsorption, and the body excretes glucose in the urine
Urine is a liquid by-product of metabolism in humans and in many other animals. Urine flows from the kidneys through the ureters to the urinary bladder. Urination results in urine being excreted from the body through the urethra.
Cellul ...
( glycosuria). This increases the osmotic pressure of the urine and inhibits reabsorption of water by the kidney, resulting in increased urine production (polyuria
Polyuria () is excessive or an abnormally large production or passage of urine (greater than 2.5 L or 3 L over 24 hours in adults). Increased production and passage of urine may also be termed diuresis. Polyuria often appears in conjunction wi ...
) and increased fluid loss. Lost blood volume is replaced osmotically from water in body cells and other body compartments, causing dehydration
In physiology, dehydration is a lack of total body water, with an accompanying disruption of metabolic processes. It occurs when free water loss exceeds free water intake, usually due to exercise, disease, or high environmental temperature. Mil ...
and increased thirst (polydipsia
Polydipsia is excessive thirst or excess drinking.Porth, C. M. (1990). ''Pathophysiology: Concepts of altered health states''. Philadelphia: J.B. Lippincott Company. The word derives from the Greek () "very thirsty", which is derived from (, " ...
). In addition, intracellular glucose deficiency stimulates appetite leading to excessive food intake (polyphagia).
Diagnosis
Diabetes mellitus is diagnosed with a test for the glucose content in the blood, and is diagnosed by demonstrating any one of the following: * Fasting plasma glucose level ≥ 7.0 mmol/L (126 mg/dL). For this test, blood is taken after a period of fasting, i.e. in the morning before breakfast, after the patient had sufficient time to fast overnight. *Plasma glucose
Glycaemia, also known as blood sugar level, blood sugar concentration, or blood glucose level is the measure of glucose concentrated in the blood of humans or other animals. Approximately 4 grams of glucose, a simple sugar, is present in the blo ...
≥ 11.1 mmol/L (200 mg/dL) two hours after a 75 gram oral glucose load as in a glucose tolerance test (OGTT)
* Symptoms of high blood sugar and plasma glucose ≥ 11.1 mmol/L (200 mg/dL) either while fasting or not fasting
* Glycated hemoglobin
Glycated hemoglobin, also known as HbA1c, glycohemoglobin, hemoglobin A1c, A1C, is a form of hemoglobin (Hb) that is chemically linked to a sugar. Most monosaccharides, including glucose, galactose and fructose, spontaneously (i.e. non-enzymat ...
(HbA1C) ≥ 48 mmol/mol (≥ 6.5 DCCT %).
A positive result, in the absence of unequivocal high blood sugar, should be confirmed by a repeat of any of the above methods on a different day. It is preferable to measure a fasting glucose level because of the ease of measurement and the considerable time commitment of formal glucose tolerance testing, which takes two hours to complete and offers no prognostic advantage over the fasting test. According to the current definition, two fasting glucose measurements above 7.0 mmol/L (126 mg/dL) is considered diagnostic for diabetes mellitus.
Per the WHO, people with fasting glucose levels from 6.1 to 6.9 mmol/L (110 to 125 mg/dL) are considered to have impaired fasting glucose. People with plasma glucose at or above 7.8 mmol/L (140 mg/dL), but not over 11.1 mmol/L (200 mg/dL), two hours after a 75 gram oral glucose load are considered to have impaired glucose tolerance. Of these two prediabetic states, the latter in particular is a major risk factor for progression to full-blown diabetes mellitus, as well as cardiovascular disease. The American Diabetes Association (ADA) since 2003 uses a slightly different range for impaired fasting glucose of 5.6 to 6.9 mmol/L (100 to 125 mg/dL).
Glycated hemoglobin
Glycated hemoglobin, also known as HbA1c, glycohemoglobin, hemoglobin A1c, A1C, is a form of hemoglobin (Hb) that is chemically linked to a sugar. Most monosaccharides, including glucose, galactose and fructose, spontaneously (i.e. non-enzymat ...
is better than fasting glucose
Many types of glucose tests exist and they can be used to estimate blood sugar levels at a given time or, over a longer period of time, to obtain average levels or to see how fast body is able to normalize changed glucose levels. Eating food for e ...
for determining risks of cardiovascular disease and death from any cause.
Prevention
There is no known preventive measure for type 1 diabetes. Type 2 diabetes—which accounts for 85–90% of all cases worldwide—can often be prevented or delayed by maintaining a normal body weight, engaging in physical activity, and eating a healthy diet. Higher levels of physical activity (more than 90 minutes per day) reduce the risk of diabetes by 28%. Dietary changes known to be effective in helping to prevent diabetes include maintaining a diet rich in whole grains andfiber
Fiber or fibre (from la, fibra, links=no) is a natural or artificial substance that is significantly longer than it is wide. Fibers are often used in the manufacture of other materials. The strongest engineering materials often incorporate ...
, and choosing good fats, such as the polyunsaturated fats found in nuts, vegetable oils, and fish. Limiting sugary beverages and eating less red meat and other sources of saturated fat can also help prevent diabetes. Tobacco smoking is also associated with an increased risk of diabetes and its complications, so smoking cessation can be an important preventive measure as well.
The relationship between type 2 diabetes and the main modifiable risk factors (excess weight, unhealthy diet, physical inactivity and tobacco use) is similar in all regions of the world. There is growing evidence that the underlying determinants of diabetes are a reflection of the major forces driving social, economic and cultural change: globalization
Globalization, or globalisation (Commonwealth English; see spelling differences), is the process of interaction and integration among people, companies, and governments worldwide. The term ''globalization'' first appeared in the early 20t ...
, urbanization, population aging, and the general health policy environment.
Management
Diabetes management concentrates on keeping blood sugar levels as close to normal, without causing low blood sugar. This can usually be accomplished with dietary changes, exercise, weight loss, and use of appropriate medications (insulin, oral medications). Learning about the disease and actively participating in the treatment is important, since complications are far less common and less severe in people who have well-managed blood sugar levels. Per theAmerican College of Physicians
The American College of Physicians (ACP) is a national organization of internists, who specialize in the diagnosis, treatment, and care of adults.Sokanu "What is an Internist?" Retrieved October 20, 2014 With 161,000 members, ACP is the largest ...
, the goal of treatment is an HbA1C level of 7-8%. Attention is also paid to other health problems that may accelerate the negative effects of diabetes. These include smoking, high blood pressure, metabolic syndrome obesity
Obesity is a medical condition, sometimes considered a disease, in which excess body fat has accumulated to such an extent that it may negatively affect health. People are classified as obese when their body mass index (BMI)—a person's ...
, and lack of regular exercise. Specialized footwear is widely used to reduce the risk of diabetic foot ulcers by relieving the pressure on the foot. Foot examination for patients living with diabetes should be done annually which includes sensation testing, foot biomechanics, vascular integrity and foot structure.
The principles of managing diabetes may be similar across the general population with diabetes, however some considerations may need to be addressed when tailoring intervention, mainly in special populations.
Considering those with severe mental illness, the efficacy of type 2 diabetes self-management interventions is still poorly explored, with insufficient scientific evidence to show whether these interventions have similar results to those observed in general population.
Lifestyle
People with diabetes can benefit from education about the disease and treatment, dietary changes, and exercise, with the goal of keeping both short-term and long-term blood glucose levels within acceptable bounds. In addition, given the associated higher risks of cardiovascular disease, lifestyle modifications are recommended to control blood pressure. Weight loss can prevent progression from prediabetes to diabetes type 2, decrease the risk of cardiovascular disease, or result in a partial remission in people with diabetes. No single dietary pattern is best for all people with diabetes. Healthy dietary patterns, such as the Mediterranean diet, low-carbohydrate diet, or DASH diet, are often recommended, although evidence does not support one over the others. According to the ADA, "reducing overall carbohydrate intake for individuals with diabetes has demonstrated the most evidence for improving glycemia", and for individuals with type 2 diabetes who cannot meet the glycemic targets or where reducing anti-glycemic medications is a priority, low or very-low carbohydrate diets are a viable approach. For overweight people with type 2 diabetes, any diet that achieves weight loss is effective.Medications
Glucose control
Most medications used to treat diabetes act by loweringblood sugar levels
Glycaemia, also known as blood sugar level, blood sugar concentration, or blood glucose level is the measure of glucose concentrated in the blood of humans or other animals. Approximately 4 grams of glucose, a simple sugar, is present in the b ...
through different mechanisms. There is broad consensus that when people with diabetes maintain tight glucose control – keeping the glucose levels in their blood within normal ranges – they experience fewer complications, such as kidney problems or eye problems. There is however debate as to whether this is appropriate and cost effective
Cost-effectiveness analysis (CEA) is a form of economic analysis that compares the relative costs and outcomes (effects) of different courses of action. Cost-effectiveness analysis is distinct from cost–benefit analysis, which assigns a moneta ...
for people later in life in whom the risk of hypoglycemia may be more significant.
There are a number of different classes of anti-diabetic medications. Type 1 diabetes requires treatment with insulin, ideally using a "basal bolus" regimen that most closely matches normal insulin release: long-acting insulin for the basal rate
Basal rate, in biology, is the rate of continuous supply of some chemical or process. In the case of diabetes mellitus, it is a low rate of continuous insulin supply needed for such purposes as controlling cellular glucose and amino acid
...
and short-acting insulin with meals. Type 2 diabetes is generally treated with medication that is taken by mouth (e.g. metformin) although some eventually require injectable treatment with insulin or GLP-1 agonist
Glucagon-like peptide-1 receptor agonists, also known as GLP-1 receptor agonists (GLP-1-RA) or incretin mimetics, are agonists of the GLP-1 receptor. This class of medications is used for the treatment of type 2 diabetes Some drugs are also approv ...
s.
Metformin is generally recommended as a first-line treatment for type 2 diabetes, as there is good evidence that it decreases mortality. It works by decreasing the liver's production of glucose. Several other groups of drugs, mostly given by mouth, may also decrease blood sugar in type 2 diabetes. These include agents that increase insulin release ( sulfonylureas), agents that decrease absorption of sugar from the intestines (acarbose
Acarbose ( INN) is an anti-diabetic drug used to treat diabetes mellitus type 2 and, in some countries, prediabetes. It is a generic sold in Europe and China as Glucobay (Bayer AG), in North America as Precose ( Bayer Pharmaceuticals), and in Can ...
), agents that inhibit the enzyme dipeptidyl peptidase-4 (DPP-4) that inactivates incretins such as GLP-1 and GIP (sitagliptin
Sitagliptin, sold under the brand name Januvia among others, is an anti-diabetic medication used to treat type 2 diabetes. In the United Kingdom it is listed as less preferred than metformin or a sulfonylurea. It is taken by mouth. It is also a ...
), agents that make the body more sensitive to insulin ( thiazolidinedione) and agents that increase the excretion of glucose in the urine ( SGLT2 inhibitors). When insulin is used in type 2 diabetes, a long-acting formulation is usually added initially, while continuing oral medications. Doses of insulin are then increased until glucose targets are reached.
Blood pressure lowering
Cardiovascular disease is a serious complication associated with diabetes, and many international guidelines recommend blood pressure treatment targets that are lower than 140/90 mmHg for people with diabetes. However, there is only limited evidence regarding what the lower targets should be. A 2016 systematic review found potential harm to treating to targets lower than 140 mmHg, and a subsequent systematic review in 2019 found no evidence of additional benefit from blood pressure lowering to between 130 – 140mmHg, although there was an increased risk of adverse events. 2015 American Diabetes Association recommendations are that people with diabetes and albuminuria should receive an inhibitor of the renin-angiotensin system to reduce the risks of progression to end-stage renal disease, cardiovascular events, and death. There is some evidence that angiotensin converting enzyme inhibitors (ACEIs) are superior to other inhibitors of the renin-angiotensin system such as angiotensin receptor blockers (ARBs), or aliskiren in preventing cardiovascular disease. Although a more recent review found similar effects of ACEIs and ARBs on major cardiovascular and renal outcomes. There is no evidence that combining ACEIs and ARBs provides additional benefits.Aspirin
The use ofaspirin
Aspirin, also known as acetylsalicylic acid (ASA), is a nonsteroidal anti-inflammatory drug (NSAID) used to reduce pain, fever, and/or inflammation, and as an antithrombotic. Specific inflammatory conditions which aspirin is used to treat inc ...
to prevent cardiovascular disease in diabetes is controversial. Aspirin is recommended by some in people at high risk of cardiovascular disease, however routine use of aspirin has not been found to improve outcomes in uncomplicated diabetes. 2015 American Diabetes Association recommendations for aspirin use (based on expert consensus or clinical experience) are that low-dose aspirin use is reasonable in adults with diabetes who are at intermediate risk of cardiovascular disease (10-year cardiovascular disease risk, 5–10%). National guidelines for England and Wales by the National Institute for Health and Care Excellence (NICE) recommend against the use of aspirin in people with type 1 or type 2 diabetes who do not have confirmed cardiovascular disease.
Surgery
Weight loss surgery in those withobesity
Obesity is a medical condition, sometimes considered a disease, in which excess body fat has accumulated to such an extent that it may negatively affect health. People are classified as obese when their body mass index (BMI)—a person's ...
and type 2 diabetes is often an effective measure. Many are able to maintain normal blood sugar levels with little or no medications following surgery and long-term mortality is decreased. There is, however, a short-term mortality risk of less than 1% from the surgery. The body mass index cutoffs for when surgery is appropriate are not yet clear. It is recommended that this option be considered in those who are unable to get both their weight and blood sugar under control.
A pancreas transplant is occasionally considered for people with type 1 diabetes who have severe complications of their disease, including end stage kidney disease requiring kidney transplantation.
Self-management and support
In countries using a general practitioner system, such as the United Kingdom, care may take place mainly outside hospitals, with hospital-based specialist care used only in case of complications, difficult blood sugar control, or research projects. In other circumstances, general practitioners and specialists share care in a team approach. Hometelehealth
Telehealth is the distribution of health-related services and information via electronic information and telecommunication technologies. It allows long-distance patient and clinician contact, care, advice, reminders, education, intervention, mon ...
support can be an effective management technique.
The use of technology
Technology is the application of knowledge to reach practical goals in a specifiable and reproducible way. The word ''technology'' may also mean the product of such an endeavor. The use of technology is widely prevalent in medicine, scien ...
to deliver educational programs for adults with type 2 diabetes includes computer-based self-management interventions to collect for tailored responses to facilitate self-management. There is no adequate evidence to support effects on cholesterol
Cholesterol is any of a class of certain organic molecules called lipids. It is a sterol (or modified steroid), a type of lipid. Cholesterol is biosynthesized by all animal cells and is an essential structural component of animal cell memb ...
, blood pressure, behavioral change (such as physical activity
Physical activity is defined as any voluntary bodily movement produced by skeletal muscles that requires energy expenditure.Global Recommendations on Physical Activity for Health, 2009. World Health Organization. Geneva, Switzerland. Accessed 13/ ...
levels and dietary), depression, weight and health-related quality of life
In general, quality of life (QoL or QOL) is the perceived quality of an individual's daily life, that is, an assessment of their well-being or lack thereof. This includes all emotional, social and physical aspects of the individual's life. In h ...
, nor in other biological, cognitive or emotional outcomes.
Epidemiology

International Diabetes Federation
The International Diabetes Federation (IDF) is an umbrella organization of over 230 national diabetes associations in more than 160 countries and territories. The Federation has been leading the global diabetes community since 1950. It is headqu ...
(IDF) estimated that diabetes resulted in 4.0 million deaths worldwide, using modeling to estimate the total number of deaths that could be directly or indirectly attributed to diabetes.
Diabetes occurs throughout the world but is more common (especially type 2) in more developed countries. The greatest increase in rates has however been seen in low- and middle-income countries, where more than 80% of diabetic deaths occur. The fastest prevalence increase is expected to occur in Asia and Africa, where most people with diabetes will probably live in 2030. The increase in rates in developing countries follows the trend of urbanization and lifestyle changes, including increasingly sedentary lifestyles, less physically demanding work and the global nutrition transition, marked by increased intake of foods that are high energy-dense but nutrient-poor (often high in sugar and saturated fats, sometimes referred to as the "Western-style" diet). The global number of diabetes cases might increase by 48% between 2017 and 2045.
As of 2020, 38% of all US adults had prediabetes. Prediabetes is an early stage of diabetes.
History
Diabetes was one of the first diseases described, with an Egyptian manuscript from 1500 BCE mentioning "too great emptying of the urine." The Ebers papyrus includes a recommendation for a drink to take in such cases. The first described cases are believed to have been type 1 diabetes. Indian physicians around the same time identified the disease and classified it as ''madhumeha'' or "honey urine", noting the urine would attract ants. The term "diabetes" or "to pass through" was first used in 230 BCE by the Greek Apollonius of Memphis. The disease was considered rare during the time of theRoman empire
The Roman Empire ( la, Imperium Romanum ; grc-gre, Βασιλεία τῶν Ῥωμαίων, Basileía tôn Rhōmaíōn) was the post-Roman Republic, Republican period of ancient Rome. As a polity, it included large territorial holdings aro ...
, with Galen
Aelius Galenus or Claudius Galenus ( el, Κλαύδιος Γαληνός; September 129 – c. AD 216), often Anglicized as Galen () or Galen of Pergamon, was a Greek physician, surgeon and philosopher in the Roman Empire. Considered to be o ...
commenting he had only seen two cases during his career. This is possibly due to the diet and lifestyle of the ancients, or because the clinical symptoms were observed during the advanced stage of the disease. Galen named the disease "diarrhea of the urine" (diarrhea urinosa).
The earliest surviving work with a detailed reference to diabetes is that of Aretaeus of Cappadocia (2nd or early 3rdcentury CE). He described the symptoms and the course of the disease, which he attributed to the moisture and coldness, reflecting the beliefs of the " Pneumatic School". He hypothesized a correlation between diabetes and other diseases, and he discussed differential diagnosis from the snakebite, which also provokes excessive thirst. His work remained unknown in the West until 1552, when the first Latin edition was published in Venice.
Two types of diabetes were identified as separate conditions for the first time by the Indian physicians Sushruta
Sushruta, or ''Suśruta'' (Sanskrit: सुश्रुत, IAST: , ) was an ancient Indian physician. The '' Sushruta Samhita'' (''Sushruta's Compendium''), a treatise ascribed to him, is one of the most important surviving ancient treatises o ...
and Charaka in 400–500 CE with one type being associated with youth and another type with being overweight. Effective treatment was not developed until the early part of the 20th century when Canadians Frederick Banting
Sir Frederick Grant Banting (November 14, 1891 – February 21, 1941) was a Canadian medical scientist, physician, painter, and Nobel laureate noted as the co-discoverer of insulin and its therapeutic potential.
In 1923, Banting and Joh ...
and Charles Herbert Best
Charles Herbert Best (February 27, 1899 – March 31, 1978) was an American-Canadian medical scientist and one of the co-discoverers of insulin.
Biography
Born in West Pembroke, Maine on February 27, 1899 to Luella Fisher and Herbert Huestis ...
isolated and purified insulin in 1921 and 1922. This was followed by the development of the long-acting insulin NPH in the 1940s.
Etymology
The word ''diabetes'' ( or ) comes fromLatin
Latin (, or , ) is a classical language belonging to the Italic languages, Italic branch of the Indo-European languages. Latin was originally a dialect spoken in the lower Tiber area (then known as Latium) around present-day Rome, but through ...
''diabētēs'', which in turn comes from Ancient Greek
Ancient Greek includes the forms of the Greek language used in ancient Greece and the ancient world from around 1500 BC to 300 BC. It is often roughly divided into the following periods: Mycenaean Greek (), Dark Ages (), the Archaic pe ...
διαβήτης (''diabētēs''), which literally means "a passer through; a siphon".Oxford English Dictionary. ''diabetes''. Retrieved 2011-06-10. Ancient Greek
Ancient Greek includes the forms of the Greek language used in ancient Greece and the ancient world from around 1500 BC to 300 BC. It is often roughly divided into the following periods: Mycenaean Greek (), Dark Ages (), the Archaic pe ...
physician Aretaeus of Cappadocia (fl.
''Floruit'' (; abbreviated fl. or occasionally flor.; from Latin for "they flourished") denotes a date or period during which a person was known to have been alive or active. In English, the unabbreviated word may also be used as a noun indicatin ...
1stcentury CE) used that word, with the intended meaning "excessive discharge of urine", as the name for the disease. Ultimately, the word comes from Greek διαβαίνειν (''diabainein''), meaning "to pass through", which is composed of δια- (''dia''-), meaning "through" and βαίνειν (''bainein''), meaning "to go". The word "diabetes" is first recorded in English, in the form ''diabete'', in a medical text written around 1425.
The word '' mellitus'' ( or ) comes from the classical Latin word ''mellītus'', meaning "mellite"Oxford English Dictionary. ''mellite''. Retrieved 2011-06-10. (i.e. sweetened with honey; honey-sweet). The Latin word comes from ''mell''-, which comes from ''mel'', meaning "honey"; sweetness; pleasant thing, and the suffix -''ītus'', whose meaning is the same as that of the English suffix "-ite".Oxford English Dictionary. ''-ite''. Retrieved 2011-06-10. It was Thomas Willis who in 1675 added "mellitus" to the word "diabetes" as a designation for the disease, when he noticed the urine of a person with diabetes had a sweet taste (glycosuria). This sweet taste had been noticed in urine by the ancient Greeks, Chinese, Egyptians, Indians, and Persians .
Society and culture
The 1989 " St. Vincent Declaration" was the result of international efforts to improve the care accorded to those with diabetes. Doing so is important not only in terms of quality of life and life expectancy but also economicallyexpenses due to diabetes have been shown to be a major drain on healthand productivity-related resources for healthcare systems and governments. Several countries established more and less successful national diabetes programmes to improve treatment of the disease. People with diabetes who have neuropathic symptoms such as numbness or tingling in feet or hands are twice as likely to be unemployed as those without the symptoms. In 2010, diabetes-related emergency room (ER) visit rates in the United States were higher among people from the lowest income communities (526 per 10,000 population) than from the highest income communities (236 per 10,000 population). Approximately 9.4% of diabetes-related ER visits were for the uninsured.Naming
The term "type 1 diabetes" has replaced several former terms, including childhood-onset diabetes, juvenile diabetes, and insulin-dependent diabetes mellitus. Likewise, the term "type 2 diabetes" has replaced several former terms, including adult-onset diabetes, obesity-related diabetes, and noninsulin-dependent diabetes mellitus. Beyond these two types, there is no agreed-upon standard nomenclature. Diabetes mellitus is also occasionally known as "sugar diabetes" to differentiate it fromdiabetes insipidus
Diabetes insipidus (DI), recently renamed to Arginine Vasopressin Deficiency (AVP-D) and Arginine Vasopressin Resistance (AVP-R), is a condition characterized by large amounts of dilute urine and increased thirst. The amount of urine produced ...
.
Other animals
Diabetes can occur in mammals or reptiles. Birds do not develop diabetes because of their unusually high tolerance for elevated blood glucose levels. In animals, diabetes is most commonly encountered in dogs and cats. Middle-aged animals are most commonly affected. Female dogs are twice as likely to be affected as males, while according to some sources, male cats are more prone than females. In both species, all breeds may be affected, but some small dog breeds are particularly likely to develop diabetes, such as Miniature Poodles. Feline diabetes is strikingly similar to human type 2 diabetes. The Burmese,Russian Blue
The Russian Blue Cat (russian: Русская голубая кошка, Russkaya golubaya koshka), commonly referred to as just Russian Blue, is a cat breed with colors that vary from a light shimmering silver to a darker, slate grey. The shor ...
, Abyssinian, and Norwegian Forest cat breeds are at higher risk than other breeds. Overweight cats are also at higher risk.
The symptoms may relate to fluid loss and polyuria, but the course may also be insidious. Diabetic animals are more prone to infections. The long-term complications recognized in humans are much rarer in animals. The principles of treatment (weight loss, oral antidiabetics, subcutaneous insulin) and management of emergencies (e.g. ketoacidosis) are similar to those in humans.
References
External links
American Diabetes Association
IDF Diabetes Atlas
National Diabetes Education Program
ADA's Standards of Medical Care in Diabetes 2019
* * {{DEFAULTSORT:Diabetes Mellitus Wikipedia medicine articles ready to translate Metabolic disorders Wikipedia emergency medicine articles ready to translate Endocrine diseases Cardiovascular diseases Disability by type