Atherosclerosis on:
[Wikipedia]
[Google]
[Amazon]
Atherosclerosis is a pattern of the disease
arteriosclerosis
Arteriosclerosis is the thickening, hardening, and loss of elasticity of the walls of Artery, arteries. This process gradually restricts the blood flow to one's organs and tissues and can lead to severe health risks brought on by atherosclerosis ...
in which the wall of the artery
An artery (plural arteries) () is a blood vessel in humans and most animals that takes blood away from the heart to one or more parts of the body (tissues, lungs, brain etc.). Most arteries carry oxygenated blood; the two exceptions are the pul ...
develops abnormalities, called lesion
A lesion is any damage or abnormal change in the tissue of an organism, usually caused by disease or trauma. ''Lesion'' is derived from the Latin "injury". Lesions may occur in plants as well as animals.
Types
There is no designated classifi ...
s. These lesion
A lesion is any damage or abnormal change in the tissue of an organism, usually caused by disease or trauma. ''Lesion'' is derived from the Latin "injury". Lesions may occur in plants as well as animals.
Types
There is no designated classifi ...
s may lead to narrowing due to the buildup of atheromatous plaque
An atheroma, or atheromatous plaque, is an abnormal and reversible accumulation of material in the inner layer of an arterial wall.
The material consists of mostly macrophage cells, or debris, containing lipids, calcium and a variable amount o ...
. At onset there are usually no symptoms, but if they develop, symptoms generally begin around middle age. When severe, it can result in coronary artery disease
Coronary artery disease (CAD), also called coronary heart disease (CHD), ischemic heart disease (IHD), myocardial ischemia, or simply heart disease, involves the reduction of blood flow to the heart muscle due to build-up of atherosclerotic pla ...
, stroke
A stroke is a medical condition in which poor blood flow to the brain causes cell death. There are two main types of stroke: ischemic, due to lack of blood flow, and hemorrhagic, due to bleeding. Both cause parts of the brain to stop functionin ...
, peripheral artery disease
Peripheral artery disease (PAD) is an abnormal narrowing of arteries other than those that supply the heart or brain. When narrowing occurs in the heart, it is called coronary artery disease, and in the brain, it is called cerebrovascular diseas ...
, or kidney problems
Kidney failure, also known as end-stage kidney disease, is a medical condition in which the kidneys can no longer adequately filter waste products from the blood, functioning at less than 15% of normal levels. Kidney failure is classified as eit ...
, depending on which arteries
An artery (plural arteries) () is a blood vessel in humans and most animals that takes blood away from the heart to one or more parts of the body (tissues, lungs, brain etc.). Most arteries carry oxygenated blood; the two exceptions are the pu ...
are affected.
The exact cause is not known and is proposed to be multifactorial. Risk factors include abnormal cholesterol levels, elevated levels of inflammatory markers
Acute-phase proteins (APPs) are a class of proteins whose concentrations in blood plasma either increase (positive acute-phase proteins) or decrease (negative acute-phase proteins) in response to inflammation. This response is called the ''acute-p ...
, high blood pressure
Hypertension (HTN or HT), also known as high blood pressure (HBP), is a long-term medical condition in which the blood pressure in the arteries is persistently elevated. High blood pressure usually does not cause symptoms. Long-term high bl ...
, diabetes
Diabetes, also known as diabetes mellitus, is a group of metabolic disorders characterized by a high blood sugar level ( hyperglycemia) over a prolonged period of time. Symptoms often include frequent urination, increased thirst and increased ap ...
, smoking
Smoking is a practice in which a substance is burned and the resulting smoke is typically breathed in to be tasted and absorbed into the bloodstream. Most commonly, the substance used is the dried leaves of the tobacco plant, which have bee ...
, obesity
Obesity is a medical condition, sometimes considered a disease, in which excess body fat has accumulated to such an extent that it may negatively affect health. People are classified as obese when their body mass index (BMI)—a person's we ...
, family history, genetic, and an unhealthy diet. Plaque
Plaque may refer to:
Commemorations or awards
* Commemorative plaque, a plate or tablet fixed to a wall to mark an event, person, etc.
* Memorial Plaque (medallion), issued to next-of-kin of dead British military personnel after World War I
* Pla ...
is made up of fat, cholesterol
Cholesterol is any of a class of certain organic molecules called lipids. It is a sterol (or modified steroid), a type of lipid. Cholesterol is biosynthesized by all animal cells and is an essential structural component of animal cell mem ...
, calcium
Calcium is a chemical element with the symbol Ca and atomic number 20. As an alkaline earth metal, calcium is a reactive metal that forms a dark oxide-nitride layer when exposed to air. Its physical and chemical properties are most similar to ...
, and other substances found in the blood
Blood is a body fluid in the circulatory system of humans and other vertebrates that delivers necessary substances such as nutrients and oxygen to the cells, and transports metabolic waste products away from those same cells. Blood in the c ...
. The narrowing of arteries
An artery (plural arteries) () is a blood vessel in humans and most animals that takes blood away from the heart to one or more parts of the body (tissues, lungs, brain etc.). Most arteries carry oxygenated blood; the two exceptions are the pu ...
limits the flow of oxygen-rich blood to parts of the body. Diagnosis is based upon a physical exam, electrocardiogram, and exercise stress test
A cardiac stress test (also referred to as a cardiac diagnostic test, cardiopulmonary exercise test, or abbreviated CPX test) is a cardiological test that measures the heart's ability to respond to external stress in a controlled clinical environ ...
, among others.
Prevention is generally by eating a healthy diet, exercising, not smoking, and maintaining a normal weight
Body mass index (BMI) is a value derived from the mass (weight) and height of a person. The BMI is defined as the body mass divided by the square of the body height, and is expressed in units of kg/m2, resulting from mass in kilograms and he ...
. Treatment of established disease may include medications to lower cholesterol
Cholesterol is any of a class of certain organic molecules called lipids. It is a sterol (or modified steroid), a type of lipid. Cholesterol is biosynthesized by all animal cells and is an essential structural component of animal cell mem ...
such as statin
Statins, also known as HMG-CoA reductase inhibitors, are a class of lipid-lowering medications that reduce illness and mortality in those who are at high risk of cardiovascular disease. They are the most common cholesterol-lowering drugs.
Low- ...
s, blood pressure medication
Antihypertensives are a class of drugs that are used to treat hypertension (high blood pressure). Antihypertensive therapy seeks to prevent the complications of high blood pressure, such as stroke and myocardial infarction. Evidence suggests that r ...
, or medications that decrease clotting, such as aspirin
Aspirin, also known as acetylsalicylic acid (ASA), is a nonsteroidal anti-inflammatory drug (NSAID) used to reduce pain, fever, and/or inflammation, and as an antithrombotic. Specific inflammatory conditions which aspirin is used to treat inc ...
. A number of procedures may also be carried out such as percutaneous coronary intervention
Percutaneous coronary intervention (PCI) is a non-surgical procedure used to treat narrowing of the coronary arteries of the heart found in coronary artery disease. The process involves combining coronary angioplasty with stenting, which is the ...
, coronary artery bypass graft
Coronary artery bypass surgery, also known as coronary artery bypass graft (CABG, pronounced "cabbage") is a surgical procedure to treat coronary artery disease (CAD), the buildup of plaques in the arteries of the heart. It can relieve chest pai ...
, or carotid endarterectomy
Carotid endarterectomy is a surgery, surgical procedure used to reduce the risk of stroke from carotid artery stenosis (narrowing the internal carotid artery). In endarterectomy, the surgeon opens the artery and removes the plaque. The plaque for ...
.
Atherosclerosis generally starts when a person is young and worsens with age. Almost all people are affected to some degree by the age of 65. It is the number one cause of death
In law, medicine, and statistics, cause of death is an official determination of conditions resulting in a human's death, which may be recorded on a death certificate. A cause of death is determined by a medical examiner. The cause of death is ...
and disability in the developed world
A developed country (or industrialized country, high-income country, more economically developed country (MEDC), advanced country) is a sovereign state that has a high quality of life, developed economy and advanced technological infrastruct ...
. Though it was first described in 1575, there is evidence that the condition occurred in people more than 5,000 years ago.
Signs and symptoms
Atherosclerosis isasymptomatic
In medicine, any disease is classified asymptomatic if a patient tests as carrier for a disease or infection but experiences no symptoms. Whenever a medical condition fails to show noticeable symptoms after a diagnosis it might be considered asy ...
for decades because the arteries enlarge at all plaque locations, thus there is no effect on blood flow. Even most plaque ruptures do not produce symptoms until enough narrowing or closure of an artery, due to clots, occurs. Signs and symptoms only occur after severe narrowing or closure impedes blood flow to different organs enough to induce symptoms. Most of the time, patients realize that they have the disease only when they experience other cardiovascular disorders
Cardiovascular disease (CVD) is a class of diseases that involve the heart or blood vessels. CVD includes coronary artery diseases (CAD) such as angina and myocardial infarction (commonly known as a heart attack). Other CVDs include stroke, hea ...
such as stroke
A stroke is a medical condition in which poor blood flow to the brain causes cell death. There are two main types of stroke: ischemic, due to lack of blood flow, and hemorrhagic, due to bleeding. Both cause parts of the brain to stop functionin ...
or heart attack
A myocardial infarction (MI), commonly known as a heart attack, occurs when blood flow decreases or stops to the coronary artery of the heart, causing damage to the heart muscle. The most common symptom is chest pain or discomfort which may tr ...
. These symptoms, however, still vary depending on which artery or organ is affected.
Abnormalities associated with atherosclerosis begin in childhood. Fibrous and gelatinous lesions have been observed in the coronary arteries
The coronary arteries are the arterial blood vessels of coronary circulation, which transport oxygenated blood to the heart muscle. The heart requires a continuous supply of oxygen to function and survive, much like any other tissue or organ of ...
of children aged 6–10. Fatty streaks have been observed in the coronary arteries of juveniles aged 11–15, though they appear at a much younger age within the aorta
The aorta ( ) is the main and largest artery in the human body, originating from the left ventricle of the heart and extending down to the abdomen, where it splits into two smaller arteries (the common iliac arteries). The aorta distributes ...
.
Clinically, given enlargement of the arteries for decades, symptomatic atherosclerosis is typically associated with men in their 40s and women in their 50s to 60s. Sub-clinically, the disease begins to appear in childhood and rarely is already present at birth. Noticeable signs can begin developing at puberty. Though symptoms are rarely exhibited in children, early screening of children for cardiovascular diseases could be beneficial to both the child and his/her relatives. While coronary artery disease
Coronary artery disease (CAD), also called coronary heart disease (CHD), ischemic heart disease (IHD), myocardial ischemia, or simply heart disease, involves the reduction of blood flow to the heart muscle due to build-up of atherosclerotic pla ...
is more prevalent in men than women, atherosclerosis of the cerebral arteries
The cerebral arteries describe three main pairs of arteries and their branches, which perfuse the cerebrum of the brain.
The three main arteries are the:
* '' Anterior cerebral artery'' (ACA)
* ''Middle cerebral artery
The middle cerebral arte ...
and strokes equally affect both sexes.
Marked narrowing in the coronary arteries, which are responsible for bringing oxygenated blood to the heart, can produce symptoms such as chest pain of angina
Angina, also known as angina pectoris, is chest pain or pressure, usually caused by ischemia, insufficient blood flow to the Cardiac muscle, heart muscle (myocardium). It is most commonly a symptom of coronary artery disease.
Angina is typical ...
and shortness of breath, sweating, nausea
Nausea is a diffuse sensation of unease and discomfort, sometimes perceived as an urge to vomit. While not painful, it can be a debilitating symptom if prolonged and has been described as placing discomfort on the chest, abdomen, or back of the ...
, dizziness or light-headedness, breathlessness or palpitations
Palpitations are perceived abnormalities of the heartbeat characterized by awareness of cardiac muscle contractions in the chest, which is further characterized by the hard, fast and/or irregular beatings of the heart.
Symptoms include a rapi ...
. Abnormal heart rhythms called arrhythmia
Arrhythmias, also known as cardiac arrhythmias, heart arrhythmias, or dysrhythmias, are irregularities in the heartbeat, including when it is too fast or too slow. A resting heart rate that is too fast – above 100 beats per minute in adults ...
s—the heart beating either too slowly or too quickly—are another consequence of ischemia
Ischemia or ischaemia is a restriction in blood supply to any tissue, muscle group, or organ of the body, causing a shortage of oxygen that is needed for cellular metabolism (to keep tissue alive). Ischemia is generally caused by problems wi ...
.Arrhythmia. Heart and Stroke Foundation. (2011)
Carotid arteries
In anatomy, the left and right common carotid arteries (carotids) (Entry "carotid"
in
Marked narrowing of the carotid arteries can present with symptoms such as: a feeling of weakness; being unable to think straight; difficulty speaking; dizziness; difficulty in walking or standing up straight; blurred vision; numbness of the face, arms and legs; severe headache; and loss of consciousness. These symptoms are also related to stroke (death of brain cells). Stroke is caused by marked narrowing or closure of arteries going to the brain; lack of adequate blood supply leads to the death of the cells of the affected tissue.
 The atherosclerotic process is not well understood. Atherosclerosis is associated with inflammatory processes in the
The atherosclerotic process is not well understood. Atherosclerosis is associated with inflammatory processes in the
 Early atherogenesis is characterized by the adherence of blood circulating
Early atherogenesis is characterized by the adherence of blood circulating
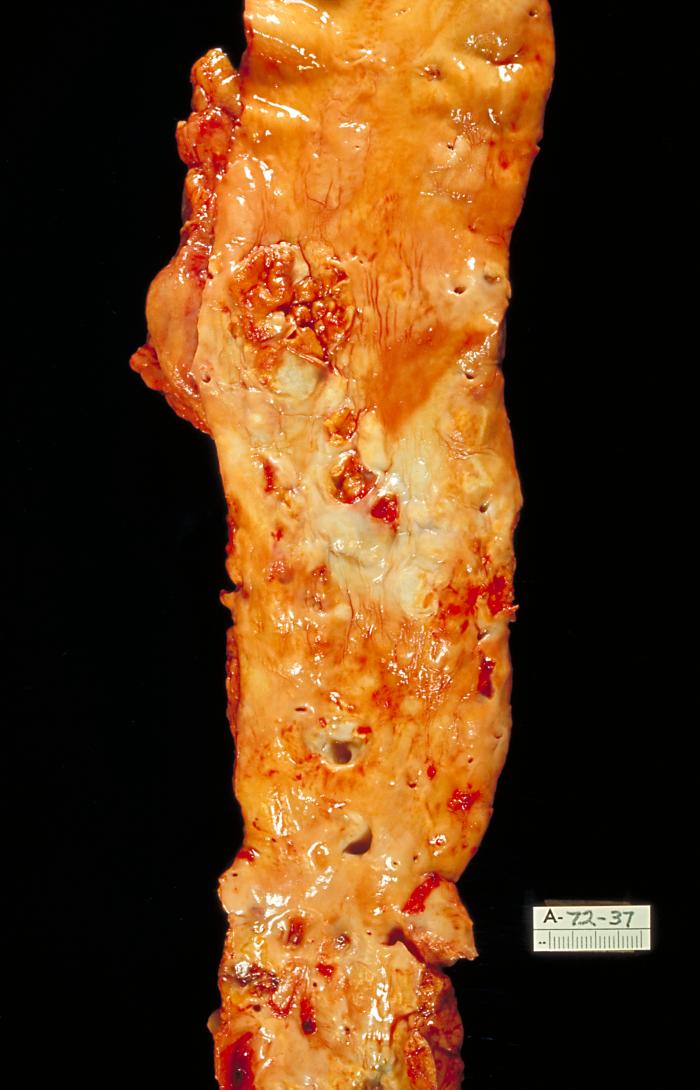 Although arteries are not typically studied microscopically, two plaque types can be distinguished:
# The fibro-lipid (fibro-fatty) plaque is characterized by an accumulation of lipid-laden cells underneath the
Although arteries are not typically studied microscopically, two plaque types can be distinguished:
# The fibro-lipid (fibro-fatty) plaque is characterized by an accumulation of lipid-laden cells underneath the
 Although the disease process tends to be slowly progressive over decades, it usually remains asymptomatic until an atheroma ulcerates, which leads to immediate blood clotting at the site of the atheroma ulcer. This triggers a cascade of events that leads to clot enlargement, which may quickly obstruct the flow of blood. A complete blockage leads to ischemia of the myocardial (heart) muscle and damage. This process is the
Although the disease process tends to be slowly progressive over decades, it usually remains asymptomatic until an atheroma ulcerates, which leads to immediate blood clotting at the site of the atheroma ulcer. This triggers a cascade of events that leads to clot enlargement, which may quickly obstruct the flow of blood. A complete blockage leads to ischemia of the myocardial (heart) muscle and damage. This process is the

 Areas of severe narrowing,
Areas of severe narrowing,  Lumen
Lumen
Atherosclerosis
pathophysiology-stages and types {{Authority control Diseases of arteries, arterioles and capillaries Vascular diseases Medical conditions related to obesity Inflammations Wikipedia medicine articles ready to translate
in
Marked narrowing of the carotid arteries can present with symptoms such as: a feeling of weakness; being unable to think straight; difficulty speaking; dizziness; difficulty in walking or standing up straight; blurred vision; numbness of the face, arms and legs; severe headache; and loss of consciousness. These symptoms are also related to stroke (death of brain cells). Stroke is caused by marked narrowing or closure of arteries going to the brain; lack of adequate blood supply leads to the death of the cells of the affected tissue.
Peripheral arteries
The peripheral vascular system is the part of the circulatory system that consists of the veins and arteries not in the chest or abdomen (i.e. in the arms, hands, legs and feet). The peripheral arteries supply oxygenated blood to the body, and ...
, which supply blood to the legs, arms and pelvis, also experience marked narrowing due to plaque rupture and clots. Symptoms of the narrowing are numbness within the arms or legs, as well as pain. Another significant location for plaque formation is the renal arteries
The renal arteries are paired arteries that supply the kidneys with blood. Each is directed across the crus of the diaphragm, so as to form nearly a right angle.
The renal arteries carry a large portion of total blood flow to the kidneys. Up to a ...
, which supply blood to the kidneys. Plaque occurrence and accumulation lead to decreased kidney blood flow and chronic kidney disease
Chronic kidney disease (CKD) is a type of kidney disease in which a gradual loss of kidney function occurs over a period of months to years. Initially generally no symptoms are seen, but later symptoms may include leg swelling, feeling tired, vo ...
, which, like in all other areas, is typically asymptomatic until late stages.
According to United States data for 2004, in about 66% of men and 47% of women, the first symptom of atherosclerotic cardiovascular disease is a heart attack
A myocardial infarction (MI), commonly known as a heart attack, occurs when blood flow decreases or stops to the coronary artery of the heart, causing damage to the heart muscle. The most common symptom is chest pain or discomfort which may tr ...
or sudden cardiac death
Cardiac arrest is when the heart suddenly and unexpectedly stops beating. It is a medical emergency that, without immediate medical intervention, will result in sudden cardiac death within minutes. Cardiopulmonary resuscitation (CPR) and possib ...
(death within one hour of onset of the symptom).
Cardiac stress test
A cardiac stress test (also referred to as a cardiac diagnostic test, cardiopulmonary exercise test, or abbreviated CPX test) is a cardiological test that measures the heart's ability to respond to external stress in a controlled clinical environ ...
ing, traditionally the most commonly performed non-invasive
A medical procedure is defined as ''non-invasive'' when no break in the skin is created and there is no contact with the mucosa, or skin break, or internal body cavity beyond a natural or artificial body orifice. For example, deep palpation and p ...
testing method for blood flow limitations, in general, detects only lumen narrowing of ≈75% or greater, although some physicians claim that nuclear stress methods can detect as little as 50%.
Case studies have included autopsies
An autopsy (post-mortem examination, obduction, necropsy, or autopsia cadaverum) is a surgical procedure that consists of a thorough examination of a corpse by dissection to determine the cause, mode, and manner of death or to evaluate any d ...
of U.S. soldiers killed in World War II
World War II or the Second World War, often abbreviated as WWII or WW2, was a world war that lasted from 1939 to 1945. It involved the vast majority of the world's countries—including all of the great powers—forming two opposin ...
and the Korean War
, date = {{Ubl, 25 June 1950 – 27 July 1953 (''de facto'')({{Age in years, months, weeks and days, month1=6, day1=25, year1=1950, month2=7, day2=27, year2=1953), 25 June 1950 – present (''de jure'')({{Age in years, months, weeks a ...
. A much-cited report involved the autopsies of 300 U.S. soldiers killed in Korea. Although the average age of the men was 22.1 years, 77.3 percent had "gross evidence of coronary arteriosclerosis". The average age was calculated from the ages of 200 of the soldiers. No age was recorded in nearly 100 of the men. Other studies done of soldiers in the Vietnam War
The Vietnam War (also known by #Names, other names) was a conflict in Vietnam, Laos, and Cambodia from 1 November 1955 to the fall of Saigon on 30 April 1975. It was the second of the Indochina Wars and was officially fought between North Vie ...
showed similar results, although often worse than the ones from the earlier wars. Theories include high rates of tobacco use
Tobacco smoking is the practice of burning tobacco and ingesting the resulting smoke. The smoke may be inhaled, as is done with cigarettes, or simply released from the mouth, as is generally done with pipes and cigars. The practice is believed ...
and (in the case of the Vietnam soldiers) the advent of processed foods after World War II.
Risk factors
 The atherosclerotic process is not well understood. Atherosclerosis is associated with inflammatory processes in the
The atherosclerotic process is not well understood. Atherosclerosis is associated with inflammatory processes in the endothelial cells
The endothelium is a single layer of squamous endothelial cells that line the interior surface of blood vessels and lymphatic vessels. The endothelium forms an interface between circulating blood or lymph in the lumen and the rest of the vessel ...
of the vessel wall associated with retained low-density lipoprotein
Low-density lipoprotein (LDL) is one of the five major groups of lipoprotein that transport all fat molecules around the body in extracellular water. These groups, from least dense to most dense, are chylomicrons (aka ULDL by the overall densit ...
(LDL) particles. This retention may be a cause, an effect, or both, of the underlying inflammatory process.
The presence of the plaque induces the muscle cells
A muscle cell is also known as a myocyte when referring to either a cardiac muscle cell (cardiomyocyte), or a smooth muscle cell as these are both small cells. A skeletal muscle cell is long and threadlike with many nuclei and is called a mus ...
of the blood vessel to stretch, compensating for the additional bulk. The endothelial lining then thickens, increasing the separation between the plaque and lumen. The thickening somewhat offsets the narrowing caused by the growth of the plaque, but moreover, it causes the wall to stiffen and become less compliant to stretching with each heartbeat.
Modifiable
*Western pattern diet
The Western pattern diet is a modern dietary pattern that is generally characterized by high intakes of pre-packaged foods, refined grains, red meat, processed meat, high-sugar drinks, candy and sweets, fried foods, conventionally-raised ani ...
* Abdominal obesity
Abdominal obesity, also known as central obesity and truncal obesity, is a condition when excessive visceral fat around the stomach and abdomen has built up to the extent that it is likely to have a negative impact on health. Abdominal obesity has ...
* Insulin resistance
Insulin resistance (IR) is a pathological condition in which cell (biology), cells fail to respond normally to the hormone insulin.
Insulin is a hormone that facilitates the transport of glucose from blood into cells, thereby reducing blood gluco ...
* Diabetes
Diabetes, also known as diabetes mellitus, is a group of metabolic disorders characterized by a high blood sugar level ( hyperglycemia) over a prolonged period of time. Symptoms often include frequent urination, increased thirst and increased ap ...
* Dyslipidemia
Dyslipidemia is an abnormal amount of lipids (e.g. triglycerides, cholesterol and/or fat phospholipids) in the blood. Dyslipidemia is a risk factor for the development of atherosclerotic cardiovascular disease ( ASCVD). ASCVD includes coronary ar ...
* Hypertension
Hypertension (HTN or HT), also known as high blood pressure (HBP), is a long-term medical condition in which the blood pressure in the arteries is persistently elevated. High blood pressure usually does not cause symptoms. Long-term high bl ...
* Trans fat
Trans fat, also called trans-unsaturated fatty acids, or trans fatty acids, is a type of unsaturated fat that naturally occurs in small amounts in meat and milk fat. It became widely produced as an unintentional byproduct in the industrial pro ...
* Tobacco smoking
Tobacco smoking is the practice of burning tobacco and ingesting the resulting smoke. The smoke may be inhaled, as is done with cigarettes, or simply released from the mouth, as is generally done with pipes and cigars. The practice is believed ...
* Bacterial infections
Pathogenic bacteria are bacteria that can cause disease. This article focuses on the bacteria that are pathogenic to humans. Most species of bacteria are harmless and are often beneficial but others can cause infectious diseases. The number of t ...
* HIV/AIDS
Human immunodeficiency virus infection and acquired immunodeficiency syndrome (HIV/AIDS) is a spectrum of conditions caused by infection with the human immunodeficiency virus (HIV), a retrovirus. Following initial infection an individual ...
Nonmodifiable
*South Asian
South Asia is the southern Subregion#Asia, subregion of Asia, which is defined in both geography, geographical and culture, ethno-cultural terms. The region consists of the countries of Afghanistan, Bangladesh, Bhutan, India, Maldives, Nepal, ...
descentIndian Heart Association Why South Asians Facts Web. 30 April 2015. http://indianheartassociation.org/why-indians-why-south-asians/overview/
* Advanced age
* Genetic abnormalities
A genetic disorder is a health problem caused by one or more abnormalities in the genome. It can be caused by a mutation in a single gene (monogenic) or multiple genes (polygenic) or by a chromosomal abnormality. Although polygenic disorders ...
* Family history
* Coronary anatomy and branch pattern
Lesser or uncertain
* Thrombophilia *Saturated fat
A saturated fat is a type of fat in which the fatty acid chains have all single bonds. A fat known as a glyceride is made of two kinds of smaller molecules: a short glycerol backbone and fatty acids that each contain a long linear or branched c ...
* Excessive carbohydrate
In organic chemistry, a carbohydrate () is a biomolecule consisting of carbon (C), hydrogen (H) and oxygen (O) atoms, usually with a hydrogen–oxygen atom ratio of 2:1 (as in water) and thus with the empirical formula (where ''m'' may or ma ...
s
* Elevated triglycerides
A triglyceride (TG, triacylglycerol, TAG, or triacylglyceride) is an ester derived from glycerol and three fatty acids (from ''tri-'' and ''glyceride'').
Triglycerides are the main constituents of body fat in humans and other vertebrates, as we ...
* Systemic inflammation
* Hyperinsulinemia
Hyperinsulinemia is a condition in which there are excess levels of insulin circulating in the blood relative to the level of glucose. While it is often mistaken for diabetes or hyperglycaemia, hyperinsulinemia can result from a variety of metabol ...
* Sleep deprivation
Sleep deprivation, also known as sleep insufficiency or sleeplessness, is the condition of not having adequate duration and/or quality of sleep to support decent alertness, performance, and health. It can be either chronic or acute and may vary ...
* Air pollution
Air pollution is the contamination of air due to the presence of substances in the atmosphere that are harmful to the health of humans and other living beings, or cause damage to the climate or to materials. There are many different types ...
* Sedentary lifestyle
Sedentary lifestyle is a lifestyle type, in which one is physically inactive and does little or no physical movement and or exercise. A person living a sedentary lifestyle is often sitting or lying down while engaged in an activity like socia ...
* Arsenic poisoning
Arsenic is a chemical element with the symbol As and atomic number 33. Arsenic occurs in many minerals, usually in combination with sulfur and metals, but also as a pure elemental crystal. Arsenic is a metalloid. It has various allotropes, bu ...
* Alcohol
* Chronic stress
Chronic stress is the physiological or psychological response induced by a long-term internal or external stressor. The stressor, either physically present or recollected, will produce the same effect and trigger a chronic stress response. There i ...
* Hypothyroidism
Hypothyroidism (also called ''underactive thyroid'', ''low thyroid'' or ''hypothyreosis'') is a disorder of the endocrine system in which the thyroid gland does not produce enough thyroid hormone. It can cause a number of symptoms, such as po ...
* Periodontal disease
Periodontal disease, also known as gum disease, is a set of inflammatory conditions affecting the tissues surrounding the teeth. In its early stage, called gingivitis, the gums become swollen and red and may bleed. It is considered the main caus ...
Dietary
The relation between dietary fat and atherosclerosis is controversial. TheUSDA
The United States Department of Agriculture (USDA) is the federal executive department responsible for developing and executing federal laws related to farming, forestry, rural economic development, and food. It aims to meet the needs of com ...
, in its food pyramid, promotes a diet of about 64% carbohydrate
In organic chemistry, a carbohydrate () is a biomolecule consisting of carbon (C), hydrogen (H) and oxygen (O) atoms, usually with a hydrogen–oxygen atom ratio of 2:1 (as in water) and thus with the empirical formula (where ''m'' may or ma ...
s from total calories. The American Heart Association
The American Heart Association (AHA) is a nonprofit organization in the United States that funds cardiovascular medical research, educates consumers on healthy living and fosters appropriate cardiac care in an effort to reduce disability and death ...
, the American Diabetes Association
The American Diabetes Association (ADA) is a United States-based nonprofit that seeks to educate the public about diabetes and to help those affected by it through funding research to manage, cure and prevent diabetes (including type 1 diabetes, ...
and the National Cholesterol Education Program {{Primary sources, article, date=May 2011The National Cholesterol Education Program is a program managed by the National Heart, Lung and Blood Institute, a division of the National Institutes of Health. Its goal is to reduce increased cardiovascula ...
make similar recommendations. In contrast, Prof Walter Willett
Walter C. Willett (born June 20, 1945) is an American physician and nutrition researcher. Currently, Willett is the Fredrick John Stare Professor of Epidemiology and Nutrition at the Harvard School of Public Health and was the chair of its departm ...
(Harvard School of Public Health, PI of the second Nurses' Health Study
The Nurses Health Study is a series of prospective studies that examine epidemiology and the long-term effects of nutrition, hormones, environment, and nurses' work-life on health and disease development. The studies have been among the largest in ...
) recommends much higher levels of fat, especially of monounsaturated
In nutrition, biology, and chemistry, fat usually means any ester of fatty acids, or a mixture of such compounds, most commonly those that occur in living beings or in food.
The term often refers specifically to triglycerides (triple est ...
and polyunsaturated fat
Polyunsaturated fats are fats in which the constituent hydrocarbon chain possesses two or more carbon–carbon double bonds. Polyunsaturated fat can be found mostly in nuts, seeds, fish, seed oils, and oysters. "Unsaturated" refers to the fact tha ...
. These dietary recommendations reach a consensus, though, against consumption of trans fat
Trans fat, also called trans-unsaturated fatty acids, or trans fatty acids, is a type of unsaturated fat that naturally occurs in small amounts in meat and milk fat. It became widely produced as an unintentional byproduct in the industrial pro ...
s.
The role of eating oxidized fats ( rancid fats) in humans is not clear.
Rabbits fed rancid fats develop atherosclerosis faster. Rats fed DHA DHA, Dha and dha may refer to:
Chemicals
* Docosahexaenoic acid, a 22:6 omega-3 fatty acid
* Dehydroandrosterone, an endogenous androgenic steroid
* Dehydroascorbic acid, an oxidized form of ascorbic acid
* Dehydroacetic acid, a pyrone derivati ...
-containing oils experienced marked disruptions to their antioxidant
Antioxidants are compounds that inhibit oxidation, a chemical reaction that can produce free radicals. This can lead to polymerization and other chain reactions. They are frequently added to industrial products, such as fuels and lubricant ...
systems, and accumulated significant amounts of phospholipid
Phospholipids, are a class of lipids whose molecule has a hydrophilic "head" containing a phosphate group and two hydrophobic "tails" derived from fatty acids, joined by an alcohol residue (usually a glycerol molecule). Marine phospholipids typ ...
hydroperoxide
Hydroperoxides or peroxols are compounds containing the hydroperoxide functional group (ROOH). If the R is organic, the compounds are called organic hydroperoxides. Such compounds are a subset of organic peroxides, which have the formula ROOR. ...
in their blood, livers and kidneys.
Rabbits fed atherogenic diets containing various oils were found to undergo the most oxidative susceptibility of LDL
Low-density lipoprotein (LDL) is one of the five major groups of lipoprotein that transport all fat molecules around the body in extracellular water. These groups, from least dense to most dense, are chylomicrons (aka ULDL by the overall densit ...
via polyunsaturated oils. In another study, rabbits fed heated soybean oil "grossly induced atherosclerosis and marked liver damage were histologically and clinically demonstrated." However, Fred Kummerow
Fred August Kummerow (October 4, 1914 – May 31, 2017) was a German-born American biochemist. A longtime professor of comparative biosciences at the University of Illinois at Urbana–Champaign, Kummerow was best known as an opponent of the ...
claims that it is not dietary cholesterol, but oxysterol
An oxysterol is a derivative of cholesterol obtained by oxidation involving enzymes and / or pro-oxidants. Such compounds play important roles in various biological processes such as cholesterol homeostasis, lipid metabolism (sphingolipids, fatty ...
s, or oxidized cholesterols, from fried foods and smoking, that are the culprit.
Rancid fats and oils taste very unpleasant in even small amounts, so people avoid eating them.
It is very difficult to measure or estimate the actual human consumption of these substances. Highly unsaturated omega-3
Omega−3 fatty acids, also called Omega-3 oils, ω−3 fatty acids or ''n''−3 fatty acids, are polyunsaturated fatty acids (PUFAs) characterized by the presence of a double bond, three atoms away from the terminal methyl group in their chem ...
rich oils such as fish oil, when being sold in pill form, can hide the taste of oxidized or rancid fat that might be present. In the US, the health food industry's dietary supplements are self-regulated and outside of FDA regulations. To properly protect unsaturated fats from oxidation, it is best to keep them cool and in oxygen-free environments.
Pathophysiology
Atherogenesis is the developmental process ofatheromatous plaques
An atheroma, or atheromatous plaque, is an abnormal and reversible accumulation of material in the inner layer of an arterial wall.
The material consists of mostly macrophage cells, or debris, containing lipids, calcium and a variable amount o ...
. It is characterized by a remodeling of arteries leading to subendothelial accumulation of fatty substances called plaques. The buildup of an atheromatous plaque is a slow process, developed over a period of several years through a complex series of cellular events occurring within the arterial wall and in response to a variety of local vascular circulating factors. One recent hypothesis suggests that, for unknown reasons, leukocytes
White blood cells, also called leukocytes or leucocytes, are the cells of the immune system that are involved in protecting the body against both infectious disease and foreign invaders. All white blood cells are produced and derived from mult ...
, such as monocytes
Monocytes are a type of leukocyte or white blood cell. They are the largest type of leukocyte in blood and can differentiate into macrophages and conventional dendritic cells. As a part of the vertebrate innate immune system monocytes also infl ...
or basophils
Basophils are a type of white blood cell. Basophils are the least common type of granulocyte, representing about 0.5% to 1% of circulating white blood cells. However, they are the largest type of granulocyte. They are responsible for inflammator ...
, begin to attack the endothelium
The endothelium is a single layer of squamous endothelial cells that line the interior surface of blood vessels and lymphatic vessels. The endothelium forms an interface between circulating blood or lymph in the lumen and the rest of the vessel ...
of the artery lumen in cardiac muscle
Cardiac muscle (also called heart muscle, myocardium, cardiomyocytes and cardiac myocytes) is one of three types of vertebrate muscle tissues, with the other two being skeletal muscle and smooth muscle. It is an involuntary, striated muscle th ...
. The ensuing inflammation
Inflammation (from la, wikt:en:inflammatio#Latin, inflammatio) is part of the complex biological response of body tissues to harmful stimuli, such as pathogens, damaged cells, or Irritation, irritants, and is a protective response involving im ...
leads to the formation of atheromatous plaques in the arterial tunica intima
The tunica intima (New Latin "inner coat"), or intima for short, is the innermost tunica (layer) of an artery or vein. It is made up of one layer of endothelial cells and is supported by an internal elastic lamina. The endothelial cells are in ...
, a region of the vessel wall located between the endothelium
The endothelium is a single layer of squamous endothelial cells that line the interior surface of blood vessels and lymphatic vessels. The endothelium forms an interface between circulating blood or lymph in the lumen and the rest of the vessel ...
and the tunica media
The tunica media (New Latin "middle coat"), or media for short, is the middle tunica (layer) of an artery or vein. It lies between the tunica intima on the inside and the tunica externa on the outside.
Artery
Tunica media is made up of smooth m ...
. The bulk of these lesions is made of excess fat, collagen
Collagen () is the main structural protein in the extracellular matrix found in the body's various connective tissues. As the main component of connective tissue, it is the most abundant protein in mammals, making up from 25% to 35% of the whole ...
, and elastin
Elastin is a protein that in humans is encoded by the ''ELN'' gene. Elastin is a key component of the extracellular matrix in gnathostomes (jawed vertebrates). It is highly elastic and present in connective tissue allowing many tissues in the bod ...
. At first, as the plaques grow, only wall thickening occurs without any narrowing. Stenosis
A stenosis (from Ancient Greek στενός, "narrow") is an abnormal narrowing in a blood vessel or other tubular organ or structure such as foramina and canals. It is also sometimes called a stricture (as in urethral stricture).
''Stricture'' ...
is a late event, which may never occur and is often the result of repeated plaque rupture and healing responses, not just the atherosclerotic process by itself.
Cellular
 Early atherogenesis is characterized by the adherence of blood circulating
Early atherogenesis is characterized by the adherence of blood circulating monocytes
Monocytes are a type of leukocyte or white blood cell. They are the largest type of leukocyte in blood and can differentiate into macrophages and conventional dendritic cells. As a part of the vertebrate innate immune system monocytes also infl ...
(a type of white blood cell
White blood cells, also called leukocytes or leucocytes, are the cell (biology), cells of the immune system that are involved in protecting the body against both infectious disease and foreign invaders. All white blood cells are produced and de ...
) to the vascular bed lining, the endothelium
The endothelium is a single layer of squamous endothelial cells that line the interior surface of blood vessels and lymphatic vessels. The endothelium forms an interface between circulating blood or lymph in the lumen and the rest of the vessel ...
, then by their migration to the sub-endothelial space, and further activation into monocyte-derived macrophage
Macrophages (abbreviated as M φ, MΦ or MP) ( el, large eaters, from Greek ''μακρός'' (') = large, ''φαγεῖν'' (') = to eat) are a type of white blood cell of the immune system that engulfs and digests pathogens, such as cancer cel ...
s. The primary documented driver of this process is oxidized lipoprotein particles within the wall, beneath the endothelial
The endothelium is a single layer of squamous endothelial cells that line the interior surface of blood vessels and lymphatic vessels. The endothelium forms an interface between circulating blood or lymph in the lumen and the rest of the vessel ...
cells, though upper normal or elevated concentrations of blood glucose
Glycaemia, also known as blood sugar level, blood sugar concentration, or blood glucose level is the measure of glucose concentrated in the blood of humans or other animals. Approximately 4 grams of glucose, a simple sugar, is present in the blo ...
also plays a major role and not all factors are fully understood. Fatty streaks may appear and disappear.
Low-density lipoprotein
Low-density lipoprotein (LDL) is one of the five major groups of lipoprotein that transport all fat molecules around the body in extracellular water. These groups, from least dense to most dense, are chylomicrons (aka ULDL by the overall densit ...
(LDL) particles in blood plasma invade the endothelium
The endothelium is a single layer of squamous endothelial cells that line the interior surface of blood vessels and lymphatic vessels. The endothelium forms an interface between circulating blood or lymph in the lumen and the rest of the vessel ...
and become oxidized, creating risk of cardiovascular disease
Cardiovascular disease (CVD) is a class of diseases that involve the heart or blood vessels. CVD includes coronary artery diseases (CAD) such as angina and myocardial infarction (commonly known as a heart attack). Other CVDs include stroke, h ...
. A complex set of biochemical reactions regulates the oxidation of LDL
Low-density lipoprotein (LDL) is one of the five major groups of lipoprotein that transport all fat molecules around the body in extracellular water. These groups, from least dense to most dense, are chylomicrons (aka ULDL by the overall densit ...
, involving enzymes (such as Lp-LpA2
Lipoprotein Associated Phospholipase A2 has been identified and verified in multiple human trials as an enzymatic activity which is an independent predictor of atherosclerotic disease progression and events in humans, including coronary heart d ...
) and free radical
A daughter category of ''Ageing'', this category deals only with the biological aspects of ageing.
Ageing
Ailments of unknown cause
Biogerontology
Biological processes
Causes of death
Cellular processes
Gerontology
Life extension
Metabo ...
s in the endothelium.
Initial damage to the endothelium results in an inflammatory response. Monocytes enter the artery wall from the bloodstream, with platelet
Platelets, also called thrombocytes (from Greek θρόμβος, "clot" and κύτος, "cell"), are a component of blood whose function (along with the coagulation factors) is to react to bleeding from blood vessel injury by clumping, thereby ini ...
s adhering to the area of insult. This may be promoted by redox signaling
''Antioxidants & Redox Signaling '' is a peer-reviewed scientific journal covering reduction–oxidation (redox) signaling and antioxidant research. It covers topics such as reactive oxygen species/reactive nitrogen species (ROS/RNS) as messenge ...
induction of factors such as VCAM-1
Vascular cell adhesion protein 1 also known as vascular cell adhesion molecule 1 (VCAM-1) or cluster of differentiation 106 (CD106) is a protein that in humans is encoded by the ''VCAM1'' gene. VCAM-1 functions as a cell adhesion molecule.
Stru ...
, which recruit circulating monocytes, and M-CSF
The colony stimulating factor 1 (CSF1), also known as macrophage colony-stimulating factor (M-CSF), is a secreted cytokine which causes hematopoietic stem cells to differentiate into macrophages or other related cell types. Eukaryotic cells also ...
, which is selectively required for the differentiation of monocytes to macrophages. The monocytes differentiate into macrophage
Macrophages (abbreviated as M φ, MΦ or MP) ( el, large eaters, from Greek ''μακρός'' (') = large, ''φαγεῖν'' (') = to eat) are a type of white blood cell of the immune system that engulfs and digests pathogens, such as cancer cel ...
s, which proliferate locally, ingest oxidized LDL, slowly turning into large "foam cell
Foam cells, also called lipid-laden macrophages, are a type of cell that contain cholesterol. These can form a plaque that can lead to atherosclerosis and trigger heart attacks and stroke.
Foam cells are fat-laden cells with a M2 macrophage-like ...
s" – so-called because of their changed appearance resulting from the numerous internal cytoplasmic vesicles
Vesicle may refer to:
; In cellular biology or chemistry
* Vesicle (biology and chemistry), a supramolecular assembly of lipid molecules, like a cell membrane
* Synaptic vesicle
; In human embryology
* Vesicle (embryology), bulge-like features o ...
and resulting high lipid
Lipids are a broad group of naturally-occurring molecules which includes fats, waxes, sterols, fat-soluble vitamins (such as vitamins A, D, E and K), monoglycerides, diglycerides, phospholipids, and others. The functions of lipids include ...
content. Under the microscope, the lesion now appears as a fatty streak. Foam cells eventually die and further propagate the inflammatory process.
In addition to these cellular activities, there is also smooth muscle
Smooth muscle is an involuntary non-striated muscle, so-called because it has no sarcomeres and therefore no striations (''bands'' or ''stripes''). It is divided into two subgroups, single-unit and multiunit smooth muscle. Within single-unit mus ...
proliferation and migration from the tunica media
The tunica media (New Latin "middle coat"), or media for short, is the middle tunica (layer) of an artery or vein. It lies between the tunica intima on the inside and the tunica externa on the outside.
Artery
Tunica media is made up of smooth m ...
into the intima
The tunica intima (New Latin "inner coat"), or intima for short, is the innermost tunica (layer) of an artery or vein. It is made up of one layer of endothelial cells and is supported by an internal elastic lamina. The endothelial cells are in ...
in response to cytokine
Cytokines are a broad and loose category of small proteins (~5–25 kDa) important in cell signaling. Cytokines are peptides and cannot cross the lipid bilayer of cells to enter the cytoplasm. Cytokines have been shown to be involved in autocrin ...
s secreted by damaged endothelial cells. This causes the formation of a fibrous capsule covering the fatty streak. Intact endothelium can prevent this smooth muscle proliferation by releasing nitric oxide
Nitric oxide (nitrogen oxide or nitrogen monoxide) is a colorless gas with the formula . It is one of the principal oxides of nitrogen. Nitric oxide is a free radical: it has an unpaired electron, which is sometimes denoted by a dot in its che ...
.
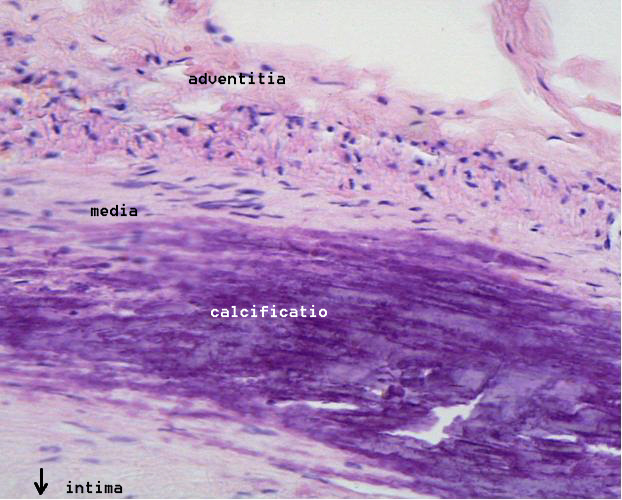
Calcification and lipids
Calcification
Calcification is the accumulation of calcium salts in a body tissue. It normally occurs in the formation of bone, but calcium can be deposited abnormally in soft tissue,Miller, J. D. Cardiovascular calcification: Orbicular origins. ''Nature Mat ...
forms among vascular smooth muscle
Vascular smooth muscle is the type of smooth muscle that makes up most of the walls of blood vessels.
Structure
Vascular smooth muscle refers to the particular type of smooth muscle found within, and composing the majority of the wall of blood ...
cells of the surrounding muscular layer, specifically in the muscle cells adjacent to atheromas and on the surface of atheroma plaques and tissue. In time, as cells die, this leads to extracellular calcium deposits between the muscular wall and outer portion of the atheromatous plaques. With the atheromatous plaque interfering with the regulation of the calcium deposition, it accumulates and crystallizes. A similar form of intramural calcification, presenting the picture of an early phase of arteriosclerosis, appears to be induced by many drugs that have an antiproliferative mechanism of action ( Rainer Liedtke 2008).
Cholesterol is delivered into the vessel wall by cholesterol-containing low-density lipoprotein
Low-density lipoprotein (LDL) is one of the five major groups of lipoprotein that transport all fat molecules around the body in extracellular water. These groups, from least dense to most dense, are chylomicrons (aka ULDL by the overall densit ...
(LDL) particles. To attract and stimulate macrophages, the cholesterol must be released from the LDL particles and oxidized, a key step in the ongoing inflammatory process. The process is worsened if it is insufficient high-density lipoprotein
High-density lipoprotein (HDL) is one of the five major groups of lipoproteins. Lipoproteins are complex particles composed of multiple proteins which transport all fat molecules (lipids) around the body within the water outside cells. They are ty ...
(HDL), the lipoprotein particle that removes cholesterol from tissues and carries it back to the liver.
The foam cell
Foam cells, also called lipid-laden macrophages, are a type of cell that contain cholesterol. These can form a plaque that can lead to atherosclerosis and trigger heart attacks and stroke.
Foam cells are fat-laden cells with a M2 macrophage-like ...
s and platelet
Platelets, also called thrombocytes (from Greek θρόμβος, "clot" and κύτος, "cell"), are a component of blood whose function (along with the coagulation factors) is to react to bleeding from blood vessel injury by clumping, thereby ini ...
s encourage the migration and proliferation of smooth muscle
Smooth muscle is an involuntary non-striated muscle, so-called because it has no sarcomeres and therefore no striations (''bands'' or ''stripes''). It is divided into two subgroups, single-unit and multiunit smooth muscle. Within single-unit mus ...
cells, which in turn ingest lipids, become replaced by collagen
Collagen () is the main structural protein in the extracellular matrix found in the body's various connective tissues. As the main component of connective tissue, it is the most abundant protein in mammals, making up from 25% to 35% of the whole ...
, and transform into foam cells themselves. A protective fibrous cap normally forms between the fatty deposits and the artery lining (the intima
The tunica intima (New Latin "inner coat"), or intima for short, is the innermost tunica (layer) of an artery or vein. It is made up of one layer of endothelial cells and is supported by an internal elastic lamina. The endothelial cells are in ...
).
These capped fatty deposits (now called 'atheromas') produce enzymes that cause the artery to enlarge over time. As long as the artery enlarges sufficiently to compensate for the extra thickness of the atheroma, then no narrowing ("stenosis
A stenosis (from Ancient Greek στενός, "narrow") is an abnormal narrowing in a blood vessel or other tubular organ or structure such as foramina and canals. It is also sometimes called a stricture (as in urethral stricture).
''Stricture'' ...
") of the opening ("lumen") occurs. The artery becomes expanded with an egg-shaped cross-section, still with a circular opening. If the enlargement is beyond proportion to the atheroma thickness, then an aneurysm
An aneurysm is an outward bulging, likened to a bubble or balloon, caused by a localized, abnormal, weak spot on a blood vessel wall. Aneurysms may be a result of a hereditary condition or an acquired disease. Aneurysms can also be a nidus (s ...
is created.
Visible features
 Although arteries are not typically studied microscopically, two plaque types can be distinguished:
# The fibro-lipid (fibro-fatty) plaque is characterized by an accumulation of lipid-laden cells underneath the
Although arteries are not typically studied microscopically, two plaque types can be distinguished:
# The fibro-lipid (fibro-fatty) plaque is characterized by an accumulation of lipid-laden cells underneath the intima
The tunica intima (New Latin "inner coat"), or intima for short, is the innermost tunica (layer) of an artery or vein. It is made up of one layer of endothelial cells and is supported by an internal elastic lamina. The endothelial cells are in ...
of the arteries, typically without narrowing the lumen due to compensatory expansion of the bounding muscular layer of the artery wall. Beneath the endothelium, there is a "fibrous cap" covering the atheromatous "core" of the plaque. The core consists of lipid-laden cells (macrophages and smooth muscle cells) with elevated tissue cholesterol and cholesterol ester
300px, Cholesterol oleate, a member of the cholesteryl ester family
Cholesteryl ester, a dietary lipid, is an ester of cholesterol. The ester bond is formed between the carboxylate group of a fatty acid and the hydroxyl group of cholesterol. Chole ...
content, fibrin
Fibrin (also called Factor Ia) is a fibrous, non-globular protein involved in the clotting of blood. It is formed by the action of the protease thrombin on fibrinogen, which causes it to polymerize. The polymerized fibrin, together with platele ...
, proteoglycan
Proteoglycans are proteins that are heavily glycosylated. The basic proteoglycan unit consists of a "core protein" with one or more covalently attached glycosaminoglycan (GAG) chain(s). The point of attachment is a serine (Ser) residue to whic ...
s, collagen
Collagen () is the main structural protein in the extracellular matrix found in the body's various connective tissues. As the main component of connective tissue, it is the most abundant protein in mammals, making up from 25% to 35% of the whole ...
, elastin
Elastin is a protein that in humans is encoded by the ''ELN'' gene. Elastin is a key component of the extracellular matrix in gnathostomes (jawed vertebrates). It is highly elastic and present in connective tissue allowing many tissues in the bod ...
, and cellular debris. In advanced plaques, the central core of the plaque usually contains extracellular cholesterol deposits (released from dead cells), which form areas of cholesterol crystals with empty, needle-like clefts. At the periphery of the plaque are younger "foamy" cells and capillaries. These plaques usually produce the most damage to the individual when they rupture. Cholesterol crystals may also play a role.
# The fibrous plaque is also localized under the intima, within the wall of the artery resulting in thickening and expansion of the wall and, sometimes, spotty localized narrowing of the lumen with some atrophy of the muscular layer. The fibrous plaque contains collagen fibers (eosinophilic
Eosinophilic (Greek suffix -phil-, meaning ''loves eosin'') is the staining of tissues, cells, or organelles after they have been washed with eosin, a dye.
Eosin is an acidic dye for staining cell cytoplasm, collagen, and muscle fibers. ''E ...
), precipitates of calcium (hematoxylinophilic), and rarely, lipid-laden cells.
In effect, the muscular portion of the artery wall forms small aneurysm
An aneurysm is an outward bulging, likened to a bubble or balloon, caused by a localized, abnormal, weak spot on a blood vessel wall. Aneurysms may be a result of a hereditary condition or an acquired disease. Aneurysms can also be a nidus (s ...
s just large enough to hold the atheroma
An atheroma, or atheromatous plaque, is an abnormal and reversible accumulation of material in the inner layer of an arterial wall.
The material consists of mostly macrophage cells, or debris, containing lipids, calcium and a variable amount o ...
that are present. The muscular portion of artery walls usually remains strong, even after they have remodeled to compensate for the atheromatous plaques.
However, atheromas within the vessel wall are soft and fragile with little elasticity. Arteries constantly expand and contract with each heartbeat, i.e., the pulse. In addition, the calcification deposits between the outer portion of the atheroma and the muscular wall, as they progress, lead to a loss of elasticity and stiffening of the artery as a whole.
The calcification deposits, after they have become sufficiently advanced, are partially visible on coronary artery computed tomography or electron beam tomography
Electron beam computed tomography (EBCT) is a specific form of computed tomography (CT) in which the X-ray tube is not mechanically spun in order to rotate the source of X-ray photons. This different design was explicitly developed to better im ...
(EBT) as rings of increased radiographic density, forming halos around the outer edges of the atheromatous plaques, within the artery wall. On CT, >130 units on the Hounsfield scale The Hounsfield scale , named after Sir Godfrey Hounsfield, is a quantitative scale for describing radiodensity. It is frequently used in CT scans, where its value is also termed CT number.
Definition
The Hounsfield unit (HU) scale is a linear tr ...
(some argue for 90 units) has been the radiographic density usually accepted as clearly representing tissue calcification within arteries. These deposits demonstrate unequivocal evidence of the disease, relatively advanced, even though the lumen of the artery is often still normal by angiography.
Rupture and stenosis
myocardial infarction
A myocardial infarction (MI), commonly known as a heart attack, occurs when blood flow decreases or stops to the coronary artery of the heart, causing damage to the heart muscle. The most common symptom is chest pain or discomfort which may ...
or "heart attack".
If the heart attack is not fatal, fibrous organization of the clot within the lumen ensues, covering the rupture but also producing stenosis
A stenosis (from Ancient Greek στενός, "narrow") is an abnormal narrowing in a blood vessel or other tubular organ or structure such as foramina and canals. It is also sometimes called a stricture (as in urethral stricture).
''Stricture'' ...
or closure of the lumen, or over time and after repeated ruptures, resulting in a persistent, usually localized stenosis or blockage of the artery lumen. Stenoses can be slowly progressive, whereas plaque ulceration is a sudden event that occurs specifically in atheromas with thinner/weaker fibrous caps that have become "unstable".
Repeated plaque ruptures, ones not resulting in total lumen closure, combined with the clot patch over the rupture and healing response to stabilize the clot is the process that produces most stenoses over time. The stenotic areas tend to become more stable despite increased flow velocities at these narrowings. Most major blood-flow-stopping events occur at large plaques, which, before their rupture, produced very little if any stenosis.
From clinical trials, 20% is the average stenosis at plaques that subsequently rupture with resulting complete artery closure. Most severe clinical events do not occur at plaques that produce high-grade stenosis. From clinical trials, only 14% of heart attacks occur from artery closure at plaques producing a 75% or greater stenosis before the vessel closing.
If the fibrous cap separating a soft atheroma from the bloodstream within the artery ruptures, tissue fragments are exposed and released. These tissue fragments are very clot-promoting, containing collagen
Collagen () is the main structural protein in the extracellular matrix found in the body's various connective tissues. As the main component of connective tissue, it is the most abundant protein in mammals, making up from 25% to 35% of the whole ...
and tissue factor; they activate platelet
Platelets, also called thrombocytes (from Greek θρόμβος, "clot" and κύτος, "cell"), are a component of blood whose function (along with the coagulation factors) is to react to bleeding from blood vessel injury by clumping, thereby ini ...
s and activate the system of coagulation. The result is the formation of a thrombus
A thrombus (plural thrombi), colloquially called a blood clot, is the final product of the blood coagulation step in hemostasis. There are two components to a thrombus: aggregated platelets and red blood cells that form a plug, and a mesh of c ...
(blood clot) overlying the atheroma, which obstructs blood flow acutely. With the obstruction of blood flow, downstream tissues are starved of oxygen
Oxygen is the chemical element with the symbol O and atomic number 8. It is a member of the chalcogen group in the periodic table, a highly reactive nonmetal, and an oxidizing agent that readily forms oxides with most elements as wel ...
and nutrients. If this is the myocardium
Cardiac muscle (also called heart muscle, myocardium, cardiomyocytes and cardiac myocytes) is one of three types of vertebrate muscle tissues, with the other two being skeletal muscle and smooth muscle. It is an involuntary, striated muscle that ...
(heart muscle) angina
Angina, also known as angina pectoris, is chest pain or pressure, usually caused by ischemia, insufficient blood flow to the Cardiac muscle, heart muscle (myocardium). It is most commonly a symptom of coronary artery disease.
Angina is typical ...
(cardiac chest pain) or myocardial infarction
A myocardial infarction (MI), commonly known as a heart attack, occurs when blood flow decreases or stops to the coronary artery of the heart, causing damage to the heart muscle. The most common symptom is chest pain or discomfort which may ...
(heart attack) develops.
Accelerated growth of plaques
The distribution of atherosclerotic plaques in a part of arterial endothelium is inhomogeneous. The multiple and focal development of atherosclerotic changes is similar to that in the development of amyloid plaques in the brain and that of age spots on the skin. Misrepair-accumulation aging theory suggests that misrepair mechanisms play an important role in the focal development of atherosclerosis. Development of a plaque is a result of repair of injured endothelium. Because of the infusion of lipids into sub-endothelium, the repair has to end up with altered remodeling of local endothelium. This is the manifestation of a misrepair. Important is this altered remodeling makes the local endothelium have increased fragility to damage and have reduced repair efficiency. As a consequence, this part of endothelium has an increased risk factor of being injured and improperly repaired. Thus, the accumulation of misrepairs of endothelium is focalized and self-accelerating. In this way, the growing of a plaque is also self-accelerating. Within a part of the arterial wall, the oldest plaque is always the biggest, and is the most dangerous one to cause blockage of a local artery.Components
The plaque is divided into three distinct components: # Theatheroma
An atheroma, or atheromatous plaque, is an abnormal and reversible accumulation of material in the inner layer of an arterial wall.
The material consists of mostly macrophage cells, or debris, containing lipids, calcium and a variable amount o ...
("lump of gruel", ), which is the nodular accumulation of a soft, flaky, yellowish material at the center of large plaques, composed of macrophages nearest the lumen of the artery
# Underlying areas of cholesterol crystals
# Calcification at the outer base of older or more advanced lesions
A lesion is any damage or abnormal change in the tissue of an organism, usually caused by disease or trauma. ''Lesion'' is derived from the Latin "injury". Lesions may occur in plants as well as animals.
Types
There is no designated classifi ...
. Atherosclerotic lesions, or atherosclerotic plaques, are separated into two broad categories: Stable and unstable (also called vulnerable). The pathobiology of atherosclerotic lesions is very complicated, but generally, stable atherosclerotic plaques, which tend to be asymptomatic, are rich in extracellular matrix
In biology, the extracellular matrix (ECM), also called intercellular matrix, is a three-dimensional network consisting of extracellular macromolecules and minerals, such as collagen, enzymes, glycoproteins and hydroxyapatite that provide stru ...
and smooth muscle cells
Smooth muscle is an involuntary non-striated muscle, so-called because it has no sarcomeres and therefore no striations (''bands'' or ''stripes''). It is divided into two subgroups, single-unit and multiunit smooth muscle. Within single-unit mus ...
. On the other hand, unstable plaques are rich in macrophages and foam cell
Foam cells, also called lipid-laden macrophages, are a type of cell that contain cholesterol. These can form a plaque that can lead to atherosclerosis and trigger heart attacks and stroke.
Foam cells are fat-laden cells with a M2 macrophage-like ...
s, and the extracellular matrix separating the lesion from the arterial lumen (also known as the fibrous cap The fibrous cap is a layer of fibrous connective tissue, which is thicker and less cellular than the normal intima, found in atherosclerotic plaques. The fibrous cap contains macrophages and smooth muscle cells.
The fibrous cap of an atheroma is c ...
) is usually weak and prone to rupture. Ruptures of the fibrous cap expose thrombogenic material, such as collagen
Collagen () is the main structural protein in the extracellular matrix found in the body's various connective tissues. As the main component of connective tissue, it is the most abundant protein in mammals, making up from 25% to 35% of the whole ...
, to the circulation and eventually induce thrombus
A thrombus (plural thrombi), colloquially called a blood clot, is the final product of the blood coagulation step in hemostasis. There are two components to a thrombus: aggregated platelets and red blood cells that form a plug, and a mesh of c ...
formation in the lumen. Upon formation, intraluminal thrombi can occlude arteries outright (e.g., coronary occlusion), but more often they detach, move into the circulation, and eventually occlude smaller downstream branches causing thromboembolism
Thrombosis (from Ancient Greek "clotting") is the formation of a blood clot inside a blood vessel, obstructing the flow of blood through the circulatory system. When a blood vessel (a vein or an artery) is injured, the body uses platelets (t ...
.
Apart from thromboembolism, chronically expanding atherosclerotic lesions can cause complete closure of the lumen. Chronically expanding lesions are often asymptomatic until lumen stenosis
A stenosis (from Ancient Greek στενός, "narrow") is an abnormal narrowing in a blood vessel or other tubular organ or structure such as foramina and canals. It is also sometimes called a stricture (as in urethral stricture).
''Stricture'' ...
is so severe (usually over 80%) that blood supply to downstream tissue(s) is insufficient, resulting in ischemia
Ischemia or ischaemia is a restriction in blood supply to any tissue, muscle group, or organ of the body, causing a shortage of oxygen that is needed for cellular metabolism (to keep tissue alive). Ischemia is generally caused by problems wi ...
. These complications of advanced atherosclerosis are chronic, slowly progressive, and cumulative. Most commonly, soft plaque suddenly ruptures (see vulnerable plaque
A vulnerable plaque is a kind of atheromatous plaque – a collection of white blood cells (primarily macrophages) and lipids (including cholesterol) in the wall of an artery – that is particularly unstable and prone to produce sudden major pro ...
), causing the formation of a thrombus that will rapidly slow or stop blood flow, leading to the death of the tissues fed by the artery in approximately five minutes. This event is called an infarction
Infarction is tissue death (necrosis) due to inadequate blood supply to the affected area. It may be caused by artery blockages, rupture, mechanical compression, or vasoconstriction. The resulting lesion is referred to as an infarct
(from the ...
.
Diagnosis
 Areas of severe narrowing,
Areas of severe narrowing, stenosis
A stenosis (from Ancient Greek στενός, "narrow") is an abnormal narrowing in a blood vessel or other tubular organ or structure such as foramina and canals. It is also sometimes called a stricture (as in urethral stricture).
''Stricture'' ...
, detectable by angiography
Angiography or arteriography is a medical imaging technique used to visualize the inside, or lumen, of blood vessels and organs of the body, with particular interest in the arteries, veins, and the heart chambers. Modern angiography is performe ...
, and to a lesser extent "stress testing
Stress testing (sometimes called torture testing) is a form of deliberately intense or thorough testing used to determine the stability of a given system, critical infrastructure or entity. It involves testing beyond normal operational capacity, ...
" have long been the focus of human diagnostic techniques for cardiovascular disease
Cardiovascular disease (CVD) is a class of diseases that involve the heart or blood vessels. CVD includes coronary artery diseases (CAD) such as angina and myocardial infarction (commonly known as a heart attack). Other CVDs include stroke, h ...
, in general. However, these methods focus on detecting only severe narrowing, not the underlying atherosclerosis disease. As demonstrated by human clinical studies, most severe events occur in locations with heavy plaque, yet little or no lumen narrowing present before debilitating events suddenly occur. Plaque rupture can lead to artery lumen occlusion within seconds to minutes, and potential permanent debility, and sometimes sudden death.
Plaques that have ruptured are called complicated lesions. The extracellular matrix
In biology, the extracellular matrix (ECM), also called intercellular matrix, is a three-dimensional network consisting of extracellular macromolecules and minerals, such as collagen, enzymes, glycoproteins and hydroxyapatite that provide stru ...
of the lesion breaks, usually at the shoulder of the fibrous cap that separates the lesion from the arterial lumen, where the exposed thrombogenic components of the plaque, mainly collagen
Collagen () is the main structural protein in the extracellular matrix found in the body's various connective tissues. As the main component of connective tissue, it is the most abundant protein in mammals, making up from 25% to 35% of the whole ...
, will trigger thrombus
A thrombus (plural thrombi), colloquially called a blood clot, is the final product of the blood coagulation step in hemostasis. There are two components to a thrombus: aggregated platelets and red blood cells that form a plug, and a mesh of c ...
formation. The thrombus then travels downstream to other blood vessels, where the blood clot may partially or completely block blood flow. If the blood flow is completely blocked, cell deaths occur due to the lack of oxygen
Oxygen is the chemical element with the symbol O and atomic number 8. It is a member of the chalcogen group in the periodic table, a highly reactive nonmetal, and an oxidizing agent that readily forms oxides with most elements as wel ...
supply to nearby cells, resulting in necrosis
Necrosis () is a form of cell injury which results in the premature death of cells in living tissue by autolysis. Necrosis is caused by factors external to the cell or tissue, such as infection, or trauma which result in the unregulated dige ...
. The narrowing or obstruction of blood flow can occur in any artery within the body. Obstruction of arteries supplying the heart muscle results in a heart attack
A myocardial infarction (MI), commonly known as a heart attack, occurs when blood flow decreases or stops to the coronary artery of the heart, causing damage to the heart muscle. The most common symptom is chest pain or discomfort which may tr ...
, while the obstruction of arteries supplying the brain results in an ischaemic stroke
A stroke is a medical condition in which poor blood flow to the brain causes cell death. There are two main types of stroke: ischemic, due to lack of blood flow, and hemorrhagic, due to bleeding. Both cause parts of the brain to stop functionin ...
.
 Lumen
Lumen stenosis
A stenosis (from Ancient Greek στενός, "narrow") is an abnormal narrowing in a blood vessel or other tubular organ or structure such as foramina and canals. It is also sometimes called a stricture (as in urethral stricture).
''Stricture'' ...
that is greater than 75% was considered the hallmark of clinically significant disease in the past because recurring episodes of angina
Angina, also known as angina pectoris, is chest pain or pressure, usually caused by ischemia, insufficient blood flow to the Cardiac muscle, heart muscle (myocardium). It is most commonly a symptom of coronary artery disease.
Angina is typical ...
and abnormalities in stress tests are only detectable at that particular severity of stenosis.
However, clinical trials have shown that only about 14% of clinically debilitating events occur at sites with more than 75% stenosis. The majority of cardiovascular events that involve sudden rupture of the atheroma plaque do not display any evident narrowing of the lumen.
Thus, greater attention has been focused on "vulnerable plaque" from the late 1990s onwards.
Besides the traditional diagnostic methods such as angiography
Angiography or arteriography is a medical imaging technique used to visualize the inside, or lumen, of blood vessels and organs of the body, with particular interest in the arteries, veins, and the heart chambers. Modern angiography is performe ...
and stress-testing, other detection techniques have been developed in the past decades for earlier detection of atherosclerotic disease. Some of the detection approaches include anatomical detection and physiologic measurement.
Examples of anatomical detection methods include coronary calcium scoring by CT, carotid IMT ( intimal media thickness) measurement by ultrasound, and intravascular ultrasound
Intravascular ultrasound (IVUS) or intravascular echocardiography is a medical imaging methodology using a specially designed catheter with a miniaturized ultrasound probe attached to the distal end of the catheter. The proximal end of the cath ...
(IVUS). Examples of physiologic measurement methods include lipoprotein subclass analysis, HbA1c
Glycated hemoglobin, also known as HbA1c, glycohemoglobin, hemoglobin A1c, A1C, is a form of hemoglobin (Hb) that is chemically linked to a sugar. Most monosaccharides, including glucose, galactose and fructose, spontaneously (i.e. non-enzymati ...
, hs-CRP, and homocysteine
Homocysteine is a non-proteinogenic α-amino acid. It is a homologue of the amino acid cysteine, differing by an additional methylene bridge (-CH2-). It is biosynthesized from methionine by the removal of its terminal Cε methyl group. In th ...
. Both anatomic and physiologic methods allow early detection before symptoms show up, disease staging, and tracking of disease progression. Anatomic methods are more expensive and some of them are invasive in nature, such as IVUS. On the other hand, physiologic methods are often less expensive and safer. But they do not quantify the current state of the disease or directly track progression. In recent years, developments in nuclear imaging
Nuclear medicine or nucleology is a medical specialty involving the application of radioactive substances in the diagnosis and treatment of disease. Nuclear imaging, in a sense, is "radiology done inside out" because it records radiation emittin ...
techniques such as PET and SPECT have provided ways of estimating the severity of atherosclerotic plaques.
Prevention
Up to 90% of cardiovascular disease may be preventable if established risk factors are avoided. Medical management of atherosclerosis first involves modification to risk factors–for example, via smoking cessation and diet restrictions. Prevention then is generally by eating a healthy diet, exercising, not smoking, and maintaining a normal weight.Diet
Changes in diet may help prevent the development of atherosclerosis. Tentative evidence suggests that a diet containing dairy products has no effect on or decreases the risk ofcardiovascular disease
Cardiovascular disease (CVD) is a class of diseases that involve the heart or blood vessels. CVD includes coronary artery diseases (CAD) such as angina and myocardial infarction (commonly known as a heart attack). Other CVDs include stroke, h ...
.
A diet high in fruits and vegetables decreases the risk of cardiovascular disease and death. Evidence suggests that the Mediterranean diet
The Mediterranean diet is a diet inspired by the eating habits of people who live near the Mediterranean Sea. When initially formulated in the 1960s, it drew on the cuisines of Greece, Italy, France and Spain. In decades since, it has also incor ...
may improve cardiovascular results. There is also evidence that a Mediterranean diet may be better than a low-fat diet
A low-fat diet is one that restricts fat, and often saturated fat and cholesterol as well. Low-fat diets are intended to reduce the occurrence of conditions such as heart disease and obesity. For weight loss, they perform similarly to a low-carb ...
in bringing about long-term changes to cardiovascular risk factors (e.g., lower cholesterol level and blood pressure
Blood pressure (BP) is the pressure of circulating blood against the walls of blood vessels. Most of this pressure results from the heart pumping blood through the circulatory system. When used without qualification, the term "blood pressure" r ...
).
Exercise
A controlled exercise program combats atherosclerosis by improving circulation and functionality of the vessels. Exercise is also used to manage weight in patients who are obese, lower blood pressure, and decrease cholesterol. Often lifestyle modification is combined with medication therapy. For example, statins help to lower cholesterol. Antiplatelet medications likeaspirin
Aspirin, also known as acetylsalicylic acid (ASA), is a nonsteroidal anti-inflammatory drug (NSAID) used to reduce pain, fever, and/or inflammation, and as an antithrombotic. Specific inflammatory conditions which aspirin is used to treat inc ...
help to prevent clots, and a variety of antihypertensive medications are routinely used to control blood pressure. If the combined efforts of risk factor modification and medication therapy are not sufficient to control symptoms or fight imminent threats of ischemic events, a physician may resort to interventional or surgical procedures to correct the obstruction.
Treatment
Treatment of established disease may include medications to lower cholesterol such asstatin
Statins, also known as HMG-CoA reductase inhibitors, are a class of lipid-lowering medications that reduce illness and mortality in those who are at high risk of cardiovascular disease. They are the most common cholesterol-lowering drugs.
Low- ...
s, blood pressure medication
Antihypertensives are a class of drugs that are used to treat hypertension (high blood pressure). Antihypertensive therapy seeks to prevent the complications of high blood pressure, such as stroke and myocardial infarction. Evidence suggests that r ...
, or medications that decrease clotting, such as aspirin
Aspirin, also known as acetylsalicylic acid (ASA), is a nonsteroidal anti-inflammatory drug (NSAID) used to reduce pain, fever, and/or inflammation, and as an antithrombotic. Specific inflammatory conditions which aspirin is used to treat inc ...
. A number of procedures may also be carried out such as percutaneous coronary intervention
Percutaneous coronary intervention (PCI) is a non-surgical procedure used to treat narrowing of the coronary arteries of the heart found in coronary artery disease. The process involves combining coronary angioplasty with stenting, which is the ...
, coronary artery bypass graft
Coronary artery bypass surgery, also known as coronary artery bypass graft (CABG, pronounced "cabbage") is a surgical procedure to treat coronary artery disease (CAD), the buildup of plaques in the arteries of the heart. It can relieve chest pai ...
, or carotid endarterectomy
Carotid endarterectomy is a surgery, surgical procedure used to reduce the risk of stroke from carotid artery stenosis (narrowing the internal carotid artery). In endarterectomy, the surgeon opens the artery and removes the plaque. The plaque for ...
.
Medical treatments often focus on alleviating symptoms. However measures which focus on decreasing underlying atherosclerosis—as opposed to simply treating symptoms—are more effective. Non-pharmaceutical means are usually the first method of treatment, such as stopping smoking and practicing regular exercise. If these methods do not work, medicines are usually the next step in treating cardiovascular diseases and, with improvements, have increasingly become the most effective method over the long term.
The key to the more effective approaches is to combine multiple different treatment strategies. In addition, for those approaches, such as lipoprotein transport behaviors, which have been shown to produce the most success, adopting more aggressive combination treatment strategies taken on a daily basis and indefinitely has generally produced better results, both before and especially after people are symptomatic.
Statins
The group of medications referred to asstatin
Statins, also known as HMG-CoA reductase inhibitors, are a class of lipid-lowering medications that reduce illness and mortality in those who are at high risk of cardiovascular disease. They are the most common cholesterol-lowering drugs.
Low- ...
s are widely prescribed for treating atherosclerosis. They have shown benefit in reducing cardiovascular disease and mortality in those with high cholesterol
Hypercholesterolemia, also called high cholesterol, is the presence of high levels of cholesterol in the blood. It is a form of hyperlipidemia (high levels of lipids in the blood), hyperlipoproteinemia (high levels of lipoproteins in the blood), ...
with few side effects. Secondary prevention therapy, which includes high-intensity statins and aspirin, is recommended by multi-society guidelines for all patients with history of ASCVD (atherosclerotic cardiovascular disease) to prevent recurrence of coronary artery disease, ischemic stroke, or peripheral arterial disease. However, prescription of and adherence to these guideline-concordant therapies is lacking, particularly among young patients and women.
Statin
Statins, also known as HMG-CoA reductase inhibitors, are a class of lipid-lowering medications that reduce illness and mortality in those who are at high risk of cardiovascular disease. They are the most common cholesterol-lowering drugs.
Low- ...
s work by inhibiting HMG-CoA (hydroxymethylglutaryl-coenzyme A) reductase, a hepatic rate-limiting enzyme in cholesterol's biochemical production pathway. By inhibiting this rate-limiting enzyme, the body is unable to produce cholesterol endogenously, therefore reducing serum LDL-cholesterol. This reduced endogenous cholesterol production triggers the body to then pull cholesterol from other cellular sources, enhancing serum HDL-cholesterol. These data are primarily in middle-age men and the conclusions are less clear for women and people over the age of 70.
Surgery
When atherosclerosis has become severe and caused irreversibleischemia
Ischemia or ischaemia is a restriction in blood supply to any tissue, muscle group, or organ of the body, causing a shortage of oxygen that is needed for cellular metabolism (to keep tissue alive). Ischemia is generally caused by problems wi ...
, such as tissue loss
Chronic limb threatening ischemia (CLTI), also known as critical limb ischemia (CLI), is an advanced stage of peripheral artery disease (PAD). It is defined as ischemic rest pain, arterial insufficiency ulcers, and gangrene. The latter two cond ...
in the case of peripheral artery disease
Peripheral artery disease (PAD) is an abnormal narrowing of arteries other than those that supply the heart or brain. When narrowing occurs in the heart, it is called coronary artery disease, and in the brain, it is called cerebrovascular diseas ...
, surgery may be indicated. Vascular bypass surgery can re-establish flow around the diseased segment of artery, and angioplasty
Angioplasty, is also known as balloon angioplasty and percutaneous transluminal angioplasty (PTA), is a minimally invasive endovascular procedure used to widen narrowed or obstructed arteries or veins, typically to treat arterial atheroscle ...
with or without stent
In medicine, a stent is a metal or plastic tube inserted into the lumen of an anatomic vessel or duct to keep the passageway open, and stenting is the placement of a stent. A wide variety of stents are used for different purposes, from expandab ...
ing can reopen narrowed arteries and improve blood flow. Coronary artery bypass grafting
Coronary artery bypass surgery, also known as coronary artery bypass graft (CABG, pronounced "cabbage") is a surgical procedure to treat coronary artery disease (CAD), the buildup of plaques in the arteries of the heart. It can relieve chest p ...
without manipulation of the ascending aorta has demonstrated reduced rates of postoperative stroke and mortality compared to traditional on-pump coronary revascularization.
Other
There is evidence that someanticoagulant
Anticoagulants, commonly known as blood thinners, are chemical substances that prevent or reduce coagulation of blood, prolonging the clotting time. Some of them occur naturally in blood-eating animals such as leeches and mosquitoes, where the ...
s, particularly warfarin
Warfarin, sold under the brand name Coumadin among others, is a medication that is used as an anticoagulant (blood thinner). It is commonly used to prevent blood clots such as deep vein thrombosis and pulmonary embolism, and to prevent strok ...
, which inhibit clot formation by interfering with Vitamin K
Vitamin K refers to structurally similar, fat-soluble vitamers found in foods and marketed as dietary supplements. The human body requires vitamin K for post-synthesis modification of certain proteins that are required for blood coagulation ...
metabolism, may actually promote arterial calcification in the long term despite reducing clot formation in the short term. Also, small molecules such as 3-hydroxybenzaldehyde and protocatechuic aldehyde
Protocatechuic aldehyde is a phenolic aldehyde, a compound released from cork stoppers into wine.
This molecule can be used as a precursor in the vanillin synthesis by biotransformation by cell cultures of ''Capsicum frutescens'', a type of Chili ...
have shown vasculoprotective effects to reduce risk of atherosclerosis.
Epidemiology
Cardiovascular disease, which is predominantly the clinical manifestation of atherosclerosis, is one of the leading causes of death worldwide. Almost all children older than age 10 indeveloped countries
A developed country (or industrialized country, high-income country, more economically developed country (MEDC), advanced country) is a sovereign state that has a high quality of life, developed economy and advanced technological infrastruct ...
have aortic fatty streaks, with coronary Coronary () may, as shorthand in English, be used to mean:
* Coronary circulation, the system of arteries and veins in mammals
** Coronary artery disease
**Coronary occlusion
** A myocardial infarction, a heart attack
As adjective
* Referring to ...
fatty streaks beginning in adolescence
Adolescence () is a transitional stage of physical and psychological development that generally occurs during the period from puberty to adulthood (typically corresponding to the age of majority). Adolescence is usually associated with the t ...
.Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; & Mitchell, Richard N. (2007). ''Robbins Basic Pathology'' (8th ed.). Saunders Elsevier. pp. 348-351
In 1953, a study was published which examined the results of 300 autopsies performed on U.S. soldiers who had died in the Korean War
, date = {{Ubl, 25 June 1950 – 27 July 1953 (''de facto'')({{Age in years, months, weeks and days, month1=6, day1=25, year1=1950, month2=7, day2=27, year2=1953), 25 June 1950 – present (''de jure'')({{Age in years, months, weeks a ...
. Despite the average age of the soldiers being just 22 years old, 77% of them had visible signs of coronary atherosclerosis. This study showed that heart disease could affect people at a younger age and was not just a problem for older individuals.
In 1992, a report had shown that microscopic fatty streaks were seen in the left anterior descending artery
The left anterior descending artery (also LAD, anterior interventricular branch of left coronary artery, or anterior descending branch) is a branch of the left coronary artery. Blockage of this artery is often called the ''widow-maker infarction' ...
in over 50% of children aged 10–14 and 8% had even more advanced lesions with more accumulations of extracellular lipid.
In a 2005 report of a study done between 1985–1995, it was found that around 87% of aortas and 30% of coronary arteries in age group 5–14 years had fatty streaks which increased with age.
Etymology
The following terms are similar, yet distinct, in both spelling and meaning, and can be easily confused:arteriosclerosis
Arteriosclerosis is the thickening, hardening, and loss of elasticity of the walls of Artery, arteries. This process gradually restricts the blood flow to one's organs and tissues and can lead to severe health risks brought on by atherosclerosis ...
, arteriolosclerosis
Arteriolosclerosis is a form of cardiovascular disease involving hardening and loss of elasticity of arterioles or small arteries and is most often associated with hypertension and diabetes mellitus.
Types include hyaline arteriolosclerosis and hyp ...
, and atherosclerosis. ''Arteriosclerosis'' is a general term describing any hardening (and loss of elasticity) of medium or large arteries (); ''arteriolosclerosis'' is any hardening (and loss of elasticity) of arteriole
An arteriole is a small-diameter blood vessel in the microcirculation that extends and branches out from an artery and leads to capillaries.
Arterioles have muscular walls (usually only one to two layers of smooth muscle cells) and are the primar ...
s (small arteries); ''atherosclerosis'' is a hardening of an artery specifically due to an atheromatous plaque
An atheroma, or atheromatous plaque, is an abnormal and reversible accumulation of material in the inner layer of an arterial wall.
The material consists of mostly macrophage cells, or debris, containing lipids, calcium and a variable amount o ...
(). The term ''atherogenic'' is used for substances or processes that cause formation of atheroma
An atheroma, or atheromatous plaque, is an abnormal and reversible accumulation of material in the inner layer of an arterial wall.
The material consists of mostly macrophage cells, or debris, containing lipids, calcium and a variable amount o ...
.
Economics
In 2011, coronary atherosclerosis was one of the top ten most expensive conditions seen during inpatient hospitalizations in the US, with aggregate inpatient hospital costs of $10.4 billion.Research
Lipids
An indication of the role ofhigh-density lipoprotein
High-density lipoprotein (HDL) is one of the five major groups of lipoproteins. Lipoproteins are complex particles composed of multiple proteins which transport all fat molecules (lipids) around the body within the water outside cells. They are ty ...
(HDL) on atherosclerosis has been with the rare Apo-A1 Milano human genetic variant of this HDL protein. A small short-term trial using bacterial synthesized human Apo-A1 Milano HDL in people with unstable angina produced a fairly dramatic reduction in measured coronary plaque volume in only six weeks vs. the usual increase in plaque volume in those randomized to placebo. The trial was published in ''JAMA
''The Journal of the American Medical Association'' (''JAMA'') is a peer-reviewed medical journal published 48 times a year by the American Medical Association. It publishes original research, reviews, and editorials covering all aspects of biom ...
'' in early 2006. Ongoing work starting in the 1990s may lead to human clinical trials—probably by about 2008. These may use synthesized Apo-A1 Milano HDL directly, or they may use gene-transfer methods to pass the ability to synthesize the Apo-A1 Milano HDLipoprotein.
Methods to increase HDL particle concentrations, which in some animal studies largely reverses and removes atheromas, are being developed and researched. However, increasing HDL by any means is not necessarily helpful. For example, the drug torcetrapib
Torcetrapib (CP-529,414, Pfizer) was a drug being developed to treat hypercholesterolemia (elevated cholesterol levels) and prevent cardiovascular disease. Its development was halted in 2006 when phase III studies showed excessive all-cause mor ...
is the most effective agent currently known for raising HDL (by up to 60%). However, in clinical trials, it also raised deaths by 60%. All studies regarding this drug were halted in December 2006.
The actions of macrophage
Macrophages (abbreviated as M φ, MΦ or MP) ( el, large eaters, from Greek ''μακρός'' (') = large, ''φαγεῖν'' (') = to eat) are a type of white blood cell of the immune system that engulfs and digests pathogens, such as cancer cel ...
s drive atherosclerotic plaque progression.
''Immunomodulation of atherosclerosis'' is the term for techniques that modulate immune system function to suppress this macrophage action.
Involvement of lipid peroxidation chain reaction in atherogenesis triggered research on the protective role of the heavy isotope (deuterated
Isotopic labeling (or isotopic labelling) is a technique used to track the passage of an isotope (an atom with a detectable variation in neutron count) through a reaction, metabolic pathway, or cell. The reactant is 'labeled' by replacing specific ...
) polyunsaturated fatty acid
Polyunsaturated fatty acids (PUFAs) are fatty acids that contain more than one double bond in their backbone. This class includes many important compounds, such as essential fatty acids and those that give drying oils their characteristic proper ...
s (D-PUFAs) that are less prone to oxidation than ordinary PUFAs (H-PUFAs). PUFAs are essential nutrients
A nutrient is a substance used by an organism to survive, grow, and reproduce. The requirement for dietary nutrient intake applies to animals, plants, fungi, and protists. Nutrients can be incorporated into cells for metabolic purposes or excre ...
– they are involved in metabolism in that very form as they are consumed with food. In transgenic mice
A genetically modified mouse or genetically engineered mouse model (GEMM) is a mouse (''Mus musculus'') that has had its genome altered through the use of genetic engineering techniques. Genetically modified mice are commonly used for research or ...
, that are a model for human-like lipoprotein metabolism, adding D-PUFAs to diet indeed reduced body weight gain, improved cholesterol handling and reduced atherosclerotic damage to the aorta.
miRNA
MicroRNA
MicroRNA (miRNA) are small, single-stranded, non-coding RNA molecules containing 21 to 23 nucleotides. Found in plants, animals and some viruses, miRNAs are involved in RNA silencing and post-transcriptional regulation of gene expression. miRN ...
s (miRNAs) have complementary sequences in the 3' UTR and 5' UTR of target mRNAs of protein-coding genes, and cause mRNA cleavage or repression of translational machinery. In diseased vascular vessels, miRNAs are dysregulated and highly expressed. miR-33
miR-33 is a family of microRNA precursors, which are processed by the Dicer enzyme to give mature microRNAs. miR-33 is found in several animal species, including humans. In some species there is a single member of this family which gives the ma ...
is found in cardiovascular diseases. It is involved in atherosclerotic initiation and progression including lipid metabolism
Lipid metabolism is the synthesis and degradation of lipids in cells, involving the breakdown or storage of fats for energy and the synthesis of structural and functional lipids, such as those involved in the construction of cell membranes. In anim ...
, insulin signaling and glucose homeostatis, cell type progression and proliferation, and myeloid cell
A myelocyte is a young cell of the granulocytic series, occurring normally in bone marrow (can be found in circulating blood when caused by certain diseases).
Structure
When stained with the usual dyes, the cytoplasm is distinctly basophili ...
differentiation. It was found in rodents that the inhibition of miR-33
miR-33 is a family of microRNA precursors, which are processed by the Dicer enzyme to give mature microRNAs. miR-33 is found in several animal species, including humans. In some species there is a single member of this family which gives the ma ...
will raise HDL level and the expression of miR-33 is down-regulated in humans with atherosclerotic plaques.
miR-33a and miR-33b are located on intron
An intron is any nucleotide sequence within a gene that is not expressed or operative in the final RNA product. The word ''intron'' is derived from the term ''intragenic region'', i.e. a region inside a gene."The notion of the cistron .e., gene. ...
16 of human sterol regulatory element-binding protein 2 ( SREBP2) gene on chromosome 22
Chromosome 22 is one of the 23 pairs of chromosomes in human cell (biology), cells. Humans normally have two copies of chromosome 22 in each cell. Chromosome 22 is the second smallest human chromosome, spanning about 49 million DNA base pairs and ...
and intron 17 of SREBP1 gene on chromosome 17. miR-33a/b regulates cholesterol/lipid homeostatis by binding in the 3'UTRs of genes involved in cholesterol transport such as ATP binding cassette
The ATP-binding cassette transporters (ABC transporters) are a transport system superfamily that is one of the largest and possibly one of the oldest gene families. It is represented in all extant phyla, from prokaryotes to humans. ABC transpo ...
(ABC) transporters and enhance or represses its expression. Study have shown that ABCA1 mediates transport of cholesterol from peripheral tissues to Apolipoprotein-1 and it is also important in the reverse cholesterol transport pathway, where cholesterol is delivered from peripheral tissue to the liver, where it can be excreted into bile or converted to bile acids prior to excretion. Therefore, we know that ABCA1 plays an important role in preventing cholesterol accumulation in macrophages. By enhancing miR-33 function, the level of ABCA1 is decreased, leading to decrease cellular cholesterol efflux to apoA-1. On the other hand, by inhibiting miR-33 function, the level of ABCA1 is increased and increases the cholesterol efflux to Apolipoprotein A1, apoA-1. Suppression of miR-33 will lead to less cellular cholesterol and higher plasma HDL level through the regulation of ABCA1 expression.
The sugar, cyclodextrin, removed cholesterol that had built up in the arteries of mice fed a high-fat diet.
DNA damage
Aging is the most important risk factor for cardiovascular problems. The causative basis by which aging mediates its impact, independently of other recognized risk factors, remains to be determined. Evidence has been reviewed for a key role of DNA damage (naturally occurring), DNA damage in vascular aging. 8-Oxoguanine, 8-oxoG, a common type of oxidative damage in DNA, is found to accumulate in plaquevascular smooth muscle
Vascular smooth muscle is the type of smooth muscle that makes up most of the walls of blood vessels.
Structure
Vascular smooth muscle refers to the particular type of smooth muscle found within, and composing the majority of the wall of blood ...
cells, macrophage
Macrophages (abbreviated as M φ, MΦ or MP) ( el, large eaters, from Greek ''μακρός'' (') = large, ''φαγεῖν'' (') = to eat) are a type of white blood cell of the immune system that engulfs and digests pathogens, such as cancer cel ...
s and endothelium, endothelial cells, thus linking DNA damage to plaque formation. DNA strand breaks also increased in atherosclerotic plaques. Werner syndrome (WS) is a premature aging condition in humans. WS is caused by a genetic defect in a RecQ helicase that is employed in several DNA repair, repair processes that remove damages from DNA. WS patients develop a considerable burden of atherosclerotic plaques in their Coronary circulation, coronary arteries and aorta
The aorta ( ) is the main and largest artery in the human body, originating from the left ventricle of the heart and extending down to the abdomen, where it splits into two smaller arteries (the common iliac arteries). The aorta distributes ...
: calcification of the aortic valve is also frequently observed. These findings link excessive unrepaired DNA damage to premature aging and early atherosclerotic plaque development (see DNA damage theory of aging).
Microorganisms
The human microbiota, microbiota – all the microorganisms in the body, can contribute to atherosclerosis in many ways: modulation of the immune system, changes in metabolism, processing of nutrients and production of certain metabolites that can get into blood circulation. One such metabolite, produced by gut flora, gut bacteria, is trimethylamine N-oxide (TMAO). Its levels have been associated with atherosclerosis in human studies and animal research suggest that there can be a causal relation. An association between the bacterial genes encoding trimethylamine lyases — the enzymes involved in TMAO generation — and atherosclerosis has been noted.Vascular smooth muscle cells
Vascular smooth muscle, Vascular smooth muscle cells play a key role in atherogenesis and were historically considered to be beneficial for plaque stability by forming a protective fibrous cap and synthesising strength-givingextracellular matrix
In biology, the extracellular matrix (ECM), also called intercellular matrix, is a three-dimensional network consisting of extracellular macromolecules and minerals, such as collagen, enzymes, glycoproteins and hydroxyapatite that provide stru ...
components. However, in addition to the fibrous cap, vascular smooth muscle cells also give rise to many of the cell types found within the plaque core and can modulate their phenotype to both promote and reduce plaque stability. Vascular smooth muscle cells exhibit pronounced plasticity within atherosclerotic plaque and can modify their gene expression profile to resemble various other cell types, including macrophage
Macrophages (abbreviated as M φ, MΦ or MP) ( el, large eaters, from Greek ''μακρός'' (') = large, ''φαγεῖν'' (') = to eat) are a type of white blood cell of the immune system that engulfs and digests pathogens, such as cancer cel ...
s, myofibroblasts, mesenchymal stem cells and osteochondrocytes. Importantly, genetic lineage‐tracing experiments have unequivocally shown that 40-90% of plaque-resident cells are vascular smooth muscle cell derived. Therefore, it is important to research the role of vascular smooth muscle cells in atherosclerosis to identify new therapeutic targets.
References
External links
* *Atherosclerosis
pathophysiology-stages and types {{Authority control Diseases of arteries, arterioles and capillaries Vascular diseases Medical conditions related to obesity Inflammations Wikipedia medicine articles ready to translate