Classification
Definition
In the 1970s theIschemic
In an ischemic stroke, blood supply to part of the brain is decreased, leading to dysfunction of the brain tissue in that area. There are four reasons why this might happen: #Hemorrhagic
 There are two main types of hemorrhagic stroke:
* Intracerebral hemorrhage, which is basically bleeding within the brain itself (when an artery in the brain bursts, flooding the surrounding tissue with blood), due to either
There are two main types of hemorrhagic stroke:
* Intracerebral hemorrhage, which is basically bleeding within the brain itself (when an artery in the brain bursts, flooding the surrounding tissue with blood), due to either in
meninges that surround the brain). The above two main types of hemorrhagic stroke are also two different forms of
Signs and symptoms
Stroke symptoms typically start suddenly, over seconds to minutes, and in most cases do not progress further. The symptoms depend on the area of the brain affected. The more extensive the area of the brain affected, the more functions that are likely to be lost. Some forms of stroke can cause additional symptoms. For example, in intracranial hemorrhage, the affected area may compress other structures. Most forms of stroke are not associated with a headache, apart from subarachnoid hemorrhage and cerebral venous thrombosis and occasionally intracerebral hemorrhage.Early recognition
Various systems have been proposed to increase recognition of stroke. Different findings are able to predict the presence or absence of stroke to different degrees. Sudden-onset face weakness, arm drift (i.e., if a person, when asked to raise both arms, involuntarily lets one arm drift downward) and abnormal speech are the findings most likely to lead to the correct identification of a case of stroke, increasing the likelihood by 5.5 when at least one of these is present. Similarly, when all three of these are absent, the likelihood of stroke is decreased (–Subtypes
If the area of the brain affected includes one of the three prominentAssociated symptoms
Causes
Thrombotic stroke
 In thrombotic stroke, a thrombus (blood clot) usually forms around
In thrombotic stroke, a thrombus (blood clot) usually forms around in
vertebral artery dissection Vertebral artery dissection (VAD) is a flap-like tear of the inner lining of the vertebral artery, which is located in the neck and supplies blood to the brain. After the tear, blood enters the arterial wall and forms a blood clot, thickening t ...
Embolic stroke
An embolic stroke refers to an arterial embolism (a blockage of an artery) by anCerebral hypoperfusion
Cerebral hypoperfusion is the reduction of blood flow to all parts of the brain. The reduction could be to a particular part of the brain depending on the cause. It is most commonly due to heart failure fromVenous thrombosis
Cerebral venous sinus thrombosis leads to stroke due to locally increased venous pressure, which exceeds the pressure generated by the arteries. Infarcts are more likely to undergo hemorrhagic transformation (leaking of blood into the damaged area) than other types of ischemic stroke.Intracerebral hemorrhage
It generally occurs in small arteries or arterioles and is commonly due to hypertension, intracranial vascular malformations (including cavernous angiomas or arteriovenous malformations), cerebral amyloid angiopathy, or infarcts into which secondary hemorrhage has occurred. Other potential causes are trauma, Hemophilia, bleeding disorders, amyloid angiopathy, Recreational drug use, illicit drug use (e.g., amphetamines orOther
Other causes may include spasm of an artery. This may occur due toSilent stroke
A silent stroke is a stroke that does not have any outward symptoms, and people are typically unaware they have had a stroke. Despite not causing identifiable symptoms, a silent stroke still damages the brain and places the person at increased risk for bothPathophysiology
Ischemic
Ischemic stroke occurs because of a loss of blood supply to part of the brain, initiating the ischemic cascade. Atherosclerosis may disrupt the blood supply by narrowing the lumen of blood vessels leading to a reduction of blood flow by causing the formation of blood clots within the vessel or by releasing showers of small emboli through the disintegration of atherosclerotic plaques. Embolic infarction occurs when emboli formed elsewhere in the circulatory system, typically in the heart as a consequence of atrial fibrillation, or in the carotid arteries, break off, enter the cerebral circulation, then lodge in and block brain blood vessels. Since blood vessels in the brain are now blocked, the brain becomes low in energy, and thus it resorts to using anaerobic metabolism within the region of brain tissue affected by ischemia. Anaerobic metabolism produces less adenosine triphosphate (ATP) but releases a by-product called lactic acid. Lactic acid is an irritant which could potentially destroy cells since it is an acid and disrupts the normal acid-base balance in the brain. The ischemia area is referred to as the "ischemic penumbra (medicine), penumbra". After the initial ischemic event the penumbra transitions from a tissue remodeling characterized by damage to a remodeling characterized by repair. As oxygen or glucose becomes depleted in ischemic brain tissue, the production of high energy phosphate compounds such as adenosine triphosphate (ATP) fails, leading to failure of energy-dependent processes (such as ion pumping) necessary for tissue cell survival. This sets off a series of interrelated events that result in cellular injury and death. A major cause of neuronal injury is the release of the excitatory neurotransmitter glutamate. The concentration of glutamate outside the cells of the nervous system is normally kept low by so-called uptake carriers, which are powered by the concentration gradients of ions (mainly Na+) across the cell membrane. However, stroke cuts off the supply of oxygen and glucose which powers the ion pumps maintaining these gradients. As a result, the transmembrane ion gradients run down, and glutamate transporters reverse their direction, releasing glutamate into the extracellular space. Glutamate acts on receptors in nerve cells (especially NMDA receptors), producing an influx of calcium which activates enzymes that digest the cells' proteins, lipids, and nuclear material. Calcium influx can also lead to the failure of mitochondria, which can lead further toward energy depletion and may trigger cell death due to apoptosis, programmed cell death. Ischemia also induces production of Radical (chemistry), oxygen free radicals and other reactive oxygen species. These react with and damage a number of cellular and extracellular elements. Damage to the blood vessel lining or endothelium may occur. These processes are the same for any type of ischemic tissue and are referred to collectively as the ''ischemic cascade''. However, brain tissue is especially vulnerable to ischemia since it has little respiratory reserve and is completely dependent on aerobic metabolism, unlike most other organs.Hemorrhagic
Hemorrhagic strokes are classified based on their underlying pathology. Some causes of hemorrhagic stroke are Hypertensive, hypertensive hemorrhage, ruptured aneurysm, ruptured AV fistula, transformation of prior ischemic infarction, and drug-inducedDiagnosis

 Stroke is diagnosed through several techniques: a neurological examination (such as the NIHSS), CT scans (most often without contrast enhancements) or MRI scans, Doppler ultrasound, and arteriography. The diagnosis of stroke itself is clinical, with assistance from the imaging techniques. Imaging techniques also assist in determining the subtypes and cause of stroke. There is yet no commonly used blood test for the stroke diagnosis itself, though blood tests may be of help in finding out the likely cause of stroke. In deceased people, an autopsy of stroke may help establishing the time between stroke onset and death.
Stroke is diagnosed through several techniques: a neurological examination (such as the NIHSS), CT scans (most often without contrast enhancements) or MRI scans, Doppler ultrasound, and arteriography. The diagnosis of stroke itself is clinical, with assistance from the imaging techniques. Imaging techniques also assist in determining the subtypes and cause of stroke. There is yet no commonly used blood test for the stroke diagnosis itself, though blood tests may be of help in finding out the likely cause of stroke. In deceased people, an autopsy of stroke may help establishing the time between stroke onset and death.
Physical examination
A physical examination, including taking a medical history of the symptoms and a neurological status, helps giving an evaluation of the location and severity of a stroke. It can give a standard score on e.g., the NIH stroke scale.Imaging
For diagnosing ischemic (blockage) stroke in the emergency setting: * CT scans (''without'' contrast enhancements) : sensitivity (tests), sensitivity= 16% (less than 10% within first 3 hours of symptom onset) : specificity (tests), specificity= 96% * MRI scan : sensitivity= 83% : specificity= 98% For diagnosing hemorrhagic stroke in the emergency setting: * CT scans (''without'' contrast enhancements) : sensitivity= 89% : specificity= 100% * MRI scan : sensitivity= 81% : specificity= 100% For detecting chronic hemorrhages, an MRI scan is more sensitive. For the assessment of stable stroke, nuclear medicine scans SPECT and PET/CT may be helpful. SPECT documents cerebral blood flow, whereas PET with an FDG isotope shows cerebral glucose metabolism. CT scans may not detect an ischemic stroke, especially if it is small, of recent onset, or in the brainstem or cerebellum areas (Underlying cause
 When a stroke has been diagnosed, various other studies may be performed to determine the underlying cause. With the current treatment and diagnosis options available, it is of particular importance to determine whether there is a peripheral source of emboli. Test selection may vary since the cause of stroke varies with age, comorbidity and the clinical presentation. The following are commonly used techniques:
* an medical ultrasonography, ultrasound/doppler study of the carotid artery, carotid arteries (to detect carotid stenosis) or dissection of the precerebral arteries;
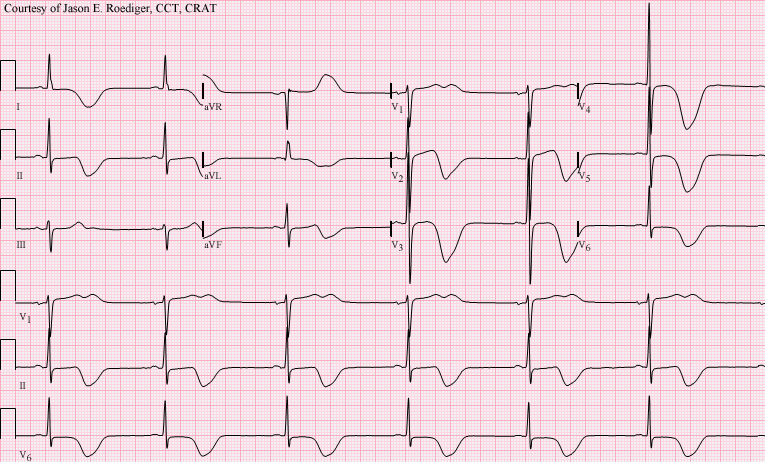
* an electrocardiogram (ECG) and echocardiogram (to identify cardiac arrhythmia, arrhythmias and resultant clots in the heart which may spread to the brain vessels through the bloodstream);
* a Holter monitor study to identify intermittent Heart arrhythmia, abnormal heart rhythms;
* an angiogram of the cerebral vasculature (if a bleed is thought to have originated from an aneurysm or arteriovenous malformation);
* blood tests to determine if hypercholesterolemia, blood cholesterol is high, if there is an abnormal bleeding diathesis, tendency to bleed, and if some rarer processes such as homocysteinuria, homocystinuria might be involved.
For hemorrhagic strokes, a Computed tomography angiography, CT or Magnetic resonance angiography, MRI scan with intravascular contrast may be able to identify abnormalities in the brain arteries (such as aneurysms) or other sources of bleeding, and structural MRI if this shows no cause. If this too does not identify an underlying reason for the bleeding, invasive cerebral angiography could be performed but this requires access to the bloodstream with an intravascular catheter and can cause further strokes as well as complications at the insertion site and this investigation is therefore reserved for specific situations. If there are symptoms suggesting that the hemorrhage might have occurred as a result of cerebral venous sinus thrombosis, venous thrombosis, CT or MRI venography can be used to examine the cerebral veins.
When a stroke has been diagnosed, various other studies may be performed to determine the underlying cause. With the current treatment and diagnosis options available, it is of particular importance to determine whether there is a peripheral source of emboli. Test selection may vary since the cause of stroke varies with age, comorbidity and the clinical presentation. The following are commonly used techniques:
* an medical ultrasonography, ultrasound/doppler study of the carotid artery, carotid arteries (to detect carotid stenosis) or dissection of the precerebral arteries;
* an electrocardiogram (ECG) and echocardiogram (to identify cardiac arrhythmia, arrhythmias and resultant clots in the heart which may spread to the brain vessels through the bloodstream);
* a Holter monitor study to identify intermittent Heart arrhythmia, abnormal heart rhythms;
* an angiogram of the cerebral vasculature (if a bleed is thought to have originated from an aneurysm or arteriovenous malformation);
* blood tests to determine if hypercholesterolemia, blood cholesterol is high, if there is an abnormal bleeding diathesis, tendency to bleed, and if some rarer processes such as homocysteinuria, homocystinuria might be involved.
For hemorrhagic strokes, a Computed tomography angiography, CT or Magnetic resonance angiography, MRI scan with intravascular contrast may be able to identify abnormalities in the brain arteries (such as aneurysms) or other sources of bleeding, and structural MRI if this shows no cause. If this too does not identify an underlying reason for the bleeding, invasive cerebral angiography could be performed but this requires access to the bloodstream with an intravascular catheter and can cause further strokes as well as complications at the insertion site and this investigation is therefore reserved for specific situations. If there are symptoms suggesting that the hemorrhage might have occurred as a result of cerebral venous sinus thrombosis, venous thrombosis, CT or MRI venography can be used to examine the cerebral veins.
Misdiagnosis
Among people with ischemic strokes, misdiagnosis occurs 2 to 26% of the time. A "stroke chameleon" (SC) is stroke which is diagnosed as something else. People not having a stroke may also be misdiagnosed as a stroke. Giving thrombolytics (clot-busting) in such cases causes intracerebral bleeding 1 to 2% of the time, which is less than that of people with strokes. This unnecessary treatment adds to health care costs. Even so, the AHA/ASA guidelines state that starting intravenous tPA in possible mimics is preferred to delaying treatment for additional testing. Women, African-Americans, Hispanic-Americans, Asian and Pacific Islanders are more often misdiagnosed for a condition other than stroke when in fact having a stroke. In addition, adults under 44 years of age are seven times more likely to have a stroke missed than are adults over 75 years of age. This is especially the case for younger people with posterior circulation infarcts. Some medical centers have used hyperacute MRI in experimental studies for persons initially thought to have a low likelihood of stroke. And in some of these persons, strokes have been found which were then treated with thrombolytic medication.Prevention
Given the disease burden of strokes, Prevention (medical), prevention is an important public health concern. Primary prevention is less effective than secondary prevention (as judged by the number needed to treat to prevent one stroke per year). Recent guidelines detail the evidence for primary prevention in stroke. In those who are otherwise healthy, aspirin does not appear beneficial and thus is not recommended. In people who have had a myocardial infarction or those with a high cardiovascular risk, it provides some protection against a first stroke.NPS Prescribing Practice Review 44: Antiplatelets and anticoagulants in stroke prevention (2009). Available anps.org.au
In those who have previously had a stroke, treatment with medications such as aspirin, clopidogrel, and dipyridamole may be beneficial. The U.S. Preventive Services Task Force (USPSTF) recommends against Screening (medicine), screening for carotid artery stenosis in those without symptoms.
Risk factors
The most important modifiable risk factors for stroke are high blood pressure and atrial fibrillation although the size of the effect is small; 833 people have to be treated for 1 year to prevent one stroke. Other modifiable risk factors include high blood cholesterol levels,Blood pressure
Hypertension, High blood pressure accounts for 35–50% of stroke risk. Blood pressure reduction of 10 mmHg systolic or 5 mmHg diastolic reduces the risk of stroke by ~40%. Lowering blood pressure has been conclusively shown to prevent both ischemic and hemorrhagic strokes. It is equally important in secondary prevention. Even people older than 80 years and those with isolated systolic hypertension benefit from antihypertensive therapy. The available evidence does not show large differences in stroke prevention between antihypertensive drugs—therefore, other factors such as protection against other forms of cardiovascular disease and cost should be considered. The routine use of beta-blockers following a stroke or TIA has not been shown to result in benefits.Blood lipids
High cholesterol levels have been inconsistently associated with (ischemic) stroke. Statins have been shown to reduce the risk of stroke by about 15%. Since earlier meta-analyses of other lipid-lowering drugs did not show a decreased risk, statins might exert their effect through mechanisms other than their lipid-lowering effects.Diabetes mellitus
Diabetes mellitus increases the risk of stroke by 2 to 3 times. While intensive blood sugar control has been shown to reduce small blood vessel complications such as Diabetic nephropathy, kidney damage and Diabetic retinopathy, damage to the retina of the eye it has not been shown to reduce large blood vessel complications such as stroke.Anticoagulation drugs
Oral anticoagulants such asSurgery
Carotid endarterectomy or carotid angioplasty can be used to remove atherosclerotic narrowing of the carotid artery. There is evidence supporting this procedure in selected cases. Endarterectomy for a significant stenosis has been shown to be useful in preventing further strokes in those who have already had one. Carotid artery stenting has not been shown to be equally useful. People are selected for surgery based on age, gender, degree of stenosis, time since symptoms and the person's preferences. Surgery is most efficient when not delayed too long—the risk of recurrent stroke in a person who has a 50% or greater stenosis is up to 20% after 5 years, but endarterectomy reduces this risk to around 5%. The number of procedures needed to cure one person was 5 for early surgery (within two weeks after the initial stroke), but 125 if delayed longer than 12 weeks. Screening (medicine), Screening for carotid artery narrowing has not been shown to be a useful test in the general population. Studies of surgical intervention for carotid artery stenosis without symptoms have shown only a small decrease in the risk of stroke. To be beneficial, the complication rate of the surgery should be kept below 4%. Even then, for 100 surgeries, 5 people will benefit by avoiding stroke, 3 will develop stroke despite surgery, 3 will develop stroke or die due to the surgery itself, and 89 will remain stroke-free but would also have done so without intervention.Diet
Nutrition, specifically the Mediterranean diet, Mediterranean-style diet, has the potential for decreasing the risk of having a stroke by more than half. It does not appear that lowering levels of homocysteine with folic acid affects the risk of stroke.Women
A number of specific recommendations have been made for women including taking aspirin after the 11th week of pregnancy if there is a history of previous chronic high blood pressure and taking blood pressure medications during pregnancy if the blood pressure is greater than 150 mmHg systolic or greater than 100 mmHg diastolic. In those who have previously had preeclampsia other risk factors should be treated more aggressively.Previous stroke or TIA
Keeping blood pressure below 140/90 mmHg is recommended. Anticoagulation can prevent recurrent ischemic strokes. Among people with nonvalvular atrial fibrillation, anticoagulation can reduce stroke by 60% while antiplatelet agents can reduce stroke by 20%. However, a recent meta-analysis suggests harm from anticoagulation started early after an embolic stroke. Stroke prevention treatment for atrial fibrillation is determined according to the CHA2DS2–VASc score. The most widely used anticoagulant to prevent thromboembolic stroke in people with nonvalvular atrial fibrillation is the oral agentManagement
Ischemic stroke
Aspirin reduces the overall risk of recurrence by 13% with greater benefit early on. Definitive therapy within the first few hours is aimed at removing the blockage by breaking the clot down (thrombolysis), or by removing it mechanically (thrombectomy). The philosophical premise underlying the importance of rapid stroke intervention was summed up as ''Time is Brain!'' in the early 1990s. Years later, that same idea, that rapid cerebral blood flow restoration results in fewer brain cells dying, has been proved and quantified. Tight blood sugar control in the first few hours does not improve outcomes and may cause harm. High blood pressure is also not typically lowered as this has not been found to be helpful. Cerebrolysin, a mixture of pig-derived neurotrophic factors used to treat acute ischemic stroke in many Asian and European countries, does not improve outcomes and may increase the risk of severe adverse events.Thrombolysis
Thrombolysis, such as with recombinant tissue plasminogen activator (rtPA), in acute ischemic stroke, when given within three hours of symptom onset, results in an overall benefit of 10% with respect to living without disability. It does not, however, improve chances of survival. Benefit is greater the earlier it is used. Between three and four and a half hours the effects are less clear. The AHA/ASA recommend it for certain people in this time frame. A 2014 review found a 5% increase in the number of people living without disability at three to six months; however, there was a 2% increased risk of death in the short term. After four and a half hours thrombolysis worsens outcomes. These benefits or lack of benefits occurred regardless of the age of the person treated. There is no reliable way to determine who will have an intracranial bleed post-treatment versus who will not. In those with findings of savable tissue on medical imaging between 4.5 hours and 9 hours or who wake up with a stroke, alteplase results in some benefit. Its use is endorsed by the American Heart Association, the American College of Emergency Physicians and the American Academy of Neurology as the recommended treatment for acute stroke within three hours of onset of symptoms as long as there are no other contraindications (such as abnormal lab values, high blood pressure, or recent surgery). This position for tPA is based upon the findings of two studies by one group of investigators which showed that tPA improves the chances for a good neurological outcome. When administered within the first three hours thrombolysis improves functional outcome without affecting mortality. 6.4% of people with large strokes developed substantial brain bleeding as a complication from being given tPA thus part of the reason for increased short term mortality. The American Academy of Emergency Medicine had previously stated that objective evidence regarding the applicability of tPA for acute ischemic stroke was insufficient. In 2013 the American College of Emergency Medicine refuted this position, acknowledging the body of evidence for the use of tPA in ischemic stroke; but debate continues. Intra-arterial fibrinolysis, where a catheter is passed up an artery into the brain and the medication is injected at the site of thrombosis, has been found to improve outcomes in people with acute ischemic stroke.Endovascular treatment
Mechanical removal of the blood clot causing the ischemic stroke, called Thrombectomy, mechanical thrombectomy, is a potential treatment for occlusion of a large artery, such as the middle cerebral artery. In 2015, one review demonstrated the safety and efficacy of this procedure if performed within 12 hours of the onset of symptoms. It did not change the risk of death, but reduced disability compared to the use of intravenous thrombolysis which is generally used in people evaluated for mechanical thrombectomy. Certain cases may benefit from thrombectomy up to 24 hours after the onset of symptoms.Craniectomy
Strokes affecting large portions of the brain can cause significant brain swelling with secondary brain injury in surrounding tissue. This phenomenon is mainly encountered in strokes affecting brain tissue dependent upon the middle cerebral artery for blood supply and is also called "malignant cerebral infarction" because it carries a dismal prognosis. Relief of the pressure may be attempted with medication, but some require hemicraniectomy, the temporary surgical removal of the skull on one side of the head. This decreases the risk of death, although some people – who would otherwise have died – survive with disability.Hemorrhagic stroke
People with intracerebral hemorrhage require supportive care, including blood pressure control if required. People are monitored for changes in the level of consciousness, and their blood sugar and oxygenation are kept at optimum levels. Anticoagulants and antithrombotics can make bleeding worse and are generally discontinued (and reversed if possible). A proportion may benefit from neurosurgery, neurosurgical intervention to remove the blood and treat the underlying cause, but this depends on the location and the size of the hemorrhage as well as patient-related factors, and ongoing research is being conducted into the question as to which people with intracerebral hemorrhage may benefit. In subarachnoid hemorrhage, early treatment for underlying cerebral aneurysms may reduce the risk of further hemorrhages. Depending on the site of the aneurysm this may be by craniotomy, surgery that involves opening the skull or Interventional neuroradiology, endovascularly (through the blood vessels).Stroke unit
Ideally, people who have had a stroke are admitted to a "stroke unit", a ward or dedicated area in a hospital staffed by nurses and therapists with experience in stroke treatment. It has been shown that people admitted to a stroke unit have a higher chance of surviving than those admitted elsewhere in hospital, even if they are being cared for by doctors without experience in stroke. Nursing care is fundamental in maintaining Skin, skin care, feeding, hydration, positioning, and monitoring vital signs such as temperature, pulse, and blood pressure.Rehabilitation
Stroke rehabilitation is the process by which those with disabling strokes undergo treatment to help them return to normal life as much as possible by regaining and relearning the skills of everyday living. It also aims to help the survivor understand and adapt to difficulties, prevent secondary complications, and educate family members to play a supporting role. Stroke rehabilitation should begin almost immediately with a multidisciplinary approach. The rehabilitation team may involve physicians trained in rehabilitation medicine, neurologists, clinical pharmacists, nursing staff, physiotherapists, occupational therapists, Speech-language pathology, speech-language pathologists, and orthotists. Some teams may also include psychologists and social workers, since at least one-third of affected people manifests post stroke depression. Validated instruments such as the Barthel scale may be used to assess the likelihood of a person who has had a stroke being able to manage at home with or without support subsequent to discharge from a hospital. Stroke rehabilitation should be started as quickly as possible and can last anywhere from a few days to over a year. Most return of function is seen in the first few months, and then improvement falls off with the "window" considered officially by U.S. state rehabilitation units and others to be closed after six months, with little chance of further improvement. However, some people have reported that they continue to improve for years, regaining and strengthening abilities like writing, walking, running, and talking. Daily rehabilitation exercises should continue to be part of the daily routine for people who have had a stroke. Complete recovery is unusual but not impossible and most people will improve to some extent: proper diet and exercise are known to help the brain to recover.Spatial neglect
The current body of evidence is uncertain on the efficacy of cognitive rehabilitation for reducing the disabling effects of neglect and increasing independence remains unproven. However, there is limited evidence that cognitive rehabilitation may have an immediate beneficial effect on tests of neglect. Overall, no rehabilitation approach can be supported by evidence for spatial neglect.Automobile driving
The current body of evidence is uncertain whether the use of rehabilitation can improve on-road driving skills following stroke. There is limited evidence that training on a driving simulator will improve performance on recognizing road signs after training. The findings are based on low-quality evidence as further research is needed involving large numbers of participants.Yoga
Based on low quality evidence, it is currently uncertain whether yoga has a significant benefit for stroke rehabilitation on measures of quality of life, balance, strength, endurance, pain, and disability scores. Yoga may reduce anxiety and could be included as part of patient-centred stroke rehabilitation. Further research is needed assessing the benefits and safety of yoga in stroke rehabilitation.Action observation for upper limbs
The latest scientific evidence indicates that action observation is beneficial in improving upper limb motor function and dependence in activities of daily living in patients with stroke. Thus, action observation therapy is generally associated with better arm and hand function, with no significant adverse events. The findings are based on low to moderate quality evidence.Cognitive rehabilitation for attention deficits
The current body of scientific evidence is uncertain on the effectiveness of cognitive rehabilitation for attention deficits in patients following stroke. While there may be an immediate effect after treatment on attention, the findings are based on low to moderate quality and small number of studies. Further research is needed to assess whether the effect can be sustained in day-to-day tasks requiring attention.Motor imagery for gait rehabilitation
The latest evidence supports the short-term benefits of motor imagery (MI) on walking speed in individuals who have had a stroke, in comparison to other therapies. MI does not improve motor function after stroke and does not seem to cause significant adverse events. The findings are based on low-quality evidence as further research is needed to estimate the effect of MI on walking endurance and the dependence on personal assistance.Physical and occupational therapy
Physical and occupational therapy have overlapping areas of expertise; however, physical therapy focuses on joint range of motion and strength by performing exercises and relearning functional tasks such as bed mobility, transferring, walking and other gross motor functions. Physiotherapists can also work with people who have had a stroke to improve awareness and use of the hemiplegic side. Rehabilitation involves working on the ability to produce strong movements or the ability to perform tasks using normal patterns. Emphasis is often concentrated on functional tasks and people's goals. One example physiotherapists employ to promote motor learning involves constraint-induced movement therapy. Through continuous practice the person relearns to use and adapt the hemiplegic limb during functional activities to create lasting permanent changes. Physical therapy is effective for recovery of function and mobility after stroke. Occupational therapy is involved in training to help relearn everyday activities known as the activities of daily living (ADLs) such as eating, drinking, dressing, bathing, cooking,= Interventions for age-related visual problems in patients with stroke
= With the prevalence of vision problems increasing with age in stroke patients, the overall effect of interventions for age-related visual problems is currently uncertain. It is also not sure whether people with stroke respond differently from the general population when treating eye problems. Further research in this area is needed as current body of evidence is very low quality.Speech and language therapy
Speech and language therapy is appropriate for people with the speech production disorders:Orthotics#Ankle–foot orthosis (AFO), Devices
Often, assistive technology such as wheelchairs, walkers and canes may be beneficial. Many mobility problems can be improved by the use of Orthotics#Ankle–foot orthosis (AFO), ankle foot orthoses.Physical fitness
A stroke can also reduce people's general fitness. Reduced fitness can reduce capacity for rehabilitation as well as general health. Physical exercises as part of a rehabilitation program following a stroke appear safe. Cardiorespiratory fitness training that involves walking in rehabilitation can improve speed, tolerance and independence during walking, and may improve balance. There are inadequate long-term data about the effects of exercise and training on death, dependence and disability after a stroke. The future areas of research may concentrate on the optimal exercise prescription and long-term health benefits of exercise. The effect of physical training on cognition also may be studied further. The ability to walk independently in their community, indoors or outdoors, is important following stroke. Although no negative effects have been reported, it is unclear if outcomes can improve with these walking programs when compared to usual treatment.Other therapy methods
Some current and future therapy methods include the use of virtual reality and video games for rehabilitation. These forms of rehabilitation offer potential for motivating people to perform specific therapy tasks that many other forms do not. While virtual reality and interactive video gaming are not more effective than conventional therapy for improving upper limb function, when used in conjunction with usual care these approaches may improve upper limb function and ADL function. There are inadequate data on the effect of virtual reality and interactive video gaming on gait speed, balance, participation and quality of life. Many clinics and hospitals are adopting the use of these off-the-shelf devices for exercise, social interaction, and rehabilitation because they are affordable, accessible and can be used within the clinic and home. Mirror box, Mirror therapy is associated with improved motor function of the upper extremity in people who have had a stroke. Other non-invasive rehabilitation methods used to augment physical therapy of motor function in people recovering from a stroke include transcranial magnetic stimulation and transcranial direct-current stimulation. and Rehabilitation robotics, robotic therapies. Constraint‐induced movement therapy (CIMT), mental practice, mirror therapy, interventions for sensory impairment, virtual reality and a relatively high dose of repetitive task practice may be effective in improving upper limb function. However, further primary research, specifically of CIMT, mental practice, mirror therapy and virtual reality is needed.Orthotics
 Clinical studies confirm the importance of Orthotics, orthoses in stroke rehabilitation. The orthosis supports the therapeutic applications and also helps to mobilize the patient at an early stage. With the help of an orthosis, physiological standing and walking can be learned again, and late health consequences caused by a wrong gait pattern can be prevented. A treatment with an orthosis can therefore be used to support the therapy.
Clinical studies confirm the importance of Orthotics, orthoses in stroke rehabilitation. The orthosis supports the therapeutic applications and also helps to mobilize the patient at an early stage. With the help of an orthosis, physiological standing and walking can be learned again, and late health consequences caused by a wrong gait pattern can be prevented. A treatment with an orthosis can therefore be used to support the therapy.
Self-management
A stroke can affect the ability to live independently and with quality. Self-management programs are a special training that educates stroke survivors about stroke and its consequences, helps them acquire skills to cope with their challenges, and helps them set and meet their own goals during their recovery process. These programs are tailored to the target audience, and led by someone trained and expert in stroke and its consequences (most commonly professionals, but also stroke survivors and peers). A 2016 review reported that these programs improve the quality of life after stroke, without negative effects. People with stroke felt more empowered, happy and satisfied with life after participating in this training.Prognosis
Disability affects 75% of stroke survivors enough to decrease their ability to work. Stroke can affect people physically, mentally, emotionally, or a combination of the three. The results of stroke vary widely depending on size and location of the lesion.Physical effects
Some of the physical disabilities that can result from stroke include muscle weakness, numbness, pressure sores,Emotional and mental effects
Emotional and mental dysfunctions correspond to areas in the brain that have been damaged. Emotional problems following a stroke can be due to direct damage to emotional centers in the brain or from frustration and difficulty adapting to new limitations. Post-stroke emotional difficulties include anxiety, panic attacks, flat affect (failure to express emotions), mania, apathy and psychosis. Other difficulties may include a decreased ability to communicate emotions through facial expression, body language and voice. Disruption in self-identity, relationships with others, and emotional well-being can lead to social consequences after stroke due to the lack of ability to communicate. Many people who experience communication impairments after a stroke find it more difficult to cope with the social issues rather than physical impairments. Broader aspects of care must address the emotional impact speech impairment has on those who experience difficulties with speech after a stroke. Those who experience a stroke are at risk of paralysis which could result in a self disturbed body image which may also lead to other social issues. 30 to 50% of stroke survivors develop post-stroke depression, which is characterized by lethargy, irritability, Sleep disorder, sleep disturbances, lowered self-esteem and withdrawal. Clinical depression, Depression can reduce motivation and worsen outcome, but can be treated with social and family support, psychotherapy and, in severe cases, antidepressants. Psychotherapy sessions may have a small effect on improving mood and preventing depression after a stroke, however psychotherapy does not appear to be effective at treating depression after a stroke. Antidepressant medications may be useful for treating depression after a stroke. Emotional lability, another consequence of stroke, causes the person to switch quickly between emotional highs and lows and to express emotions inappropriately, for instance with an excess of laughing or crying with little or no provocation. While these expressions of emotion usually correspond to the person's actual emotions, a more severe form of emotional lability causes the affected person to laugh and cry pathologically, without regard to context or emotion. Some people show the opposite of what they feel, for example crying when they are happy. Emotional lability occurs in about 20% of those who have had a stroke. Those with a right hemisphere stroke are more likely to have an empathy problems which can make communication harder. Cognitive deficits resulting from stroke include perceptual disorders,Epidemiology
History
 Episodes of stroke and familial stroke have been reported from the 2nd millennium BC onward in ancient Mesopotamia and Persia. Hippocrates (460 to 370 BC) was first to describe the phenomenon of sudden paralysis that is often associated with ischemia. Apoplexy, from the Greek language, Greek word meaning "struck down with violence", first appeared in Hippocratic writings to describe this phenomenon.
The word ''stroke'' was used as a synonym for apoplectic seizure as early as 1599, and is a fairly literal translation of the Greek term. The term ''apoplectic stroke'' is an archaic, nonspecific term, for a cerebrovascular accident accompanied by haemorrhage or haemorrhagic stroke. Martin Luther was described as having an ''apoplectic stroke'' that deprived him of his speech shortly before his death in 1546.
In 1658, in his ''Apoplexia'', Johann Jakob Wepfer, Johann Jacob Wepfer (1620–1695) identified the cause of hemorrhagic stroke when he suggested that people who had died of apoplexy had bleeding in their brains.
Wepfer also identified the main arteries supplying the brain, the vertebral and carotid arteries, and identified the cause of a type of ischemic stroke known as a cerebral infarction when he suggested that apoplexy might be caused by a blockage to those vessels. Rudolf Virchow first described the mechanism of thromboembolism as a major factor.
The term ''cerebrovascular accident'' was introduced in 1927, reflecting a "growing awareness and acceptance of vascular theories and (...) recognition of the consequences of a sudden disruption in the vascular supply of the brain". Its use is now discouraged by a number of neurology textbooks, reasoning that the connotation of fortuitousness carried by the word ''accident'' insufficiently highlights the modifiability of the underlying risk factors. ''Cerebrovascular insult'' may be used interchangeably.
The term ''brain attack'' was introduced for use to underline the acute nature of stroke according to the
Episodes of stroke and familial stroke have been reported from the 2nd millennium BC onward in ancient Mesopotamia and Persia. Hippocrates (460 to 370 BC) was first to describe the phenomenon of sudden paralysis that is often associated with ischemia. Apoplexy, from the Greek language, Greek word meaning "struck down with violence", first appeared in Hippocratic writings to describe this phenomenon.
The word ''stroke'' was used as a synonym for apoplectic seizure as early as 1599, and is a fairly literal translation of the Greek term. The term ''apoplectic stroke'' is an archaic, nonspecific term, for a cerebrovascular accident accompanied by haemorrhage or haemorrhagic stroke. Martin Luther was described as having an ''apoplectic stroke'' that deprived him of his speech shortly before his death in 1546.
In 1658, in his ''Apoplexia'', Johann Jakob Wepfer, Johann Jacob Wepfer (1620–1695) identified the cause of hemorrhagic stroke when he suggested that people who had died of apoplexy had bleeding in their brains.
Wepfer also identified the main arteries supplying the brain, the vertebral and carotid arteries, and identified the cause of a type of ischemic stroke known as a cerebral infarction when he suggested that apoplexy might be caused by a blockage to those vessels. Rudolf Virchow first described the mechanism of thromboembolism as a major factor.
The term ''cerebrovascular accident'' was introduced in 1927, reflecting a "growing awareness and acceptance of vascular theories and (...) recognition of the consequences of a sudden disruption in the vascular supply of the brain". Its use is now discouraged by a number of neurology textbooks, reasoning that the connotation of fortuitousness carried by the word ''accident'' insufficiently highlights the modifiability of the underlying risk factors. ''Cerebrovascular insult'' may be used interchangeably.
The term ''brain attack'' was introduced for use to underline the acute nature of stroke according to the Research
As of 2017, angioplasty and stents were under preliminary clinical research to determine the possible therapeutic advantages of these procedures in comparison to therapy withSee also
* Cerebrovascular disease * Dejerine–Roussy syndrome * Functional Independence Measure * Lipoprotein(a) * Mechanism of anoxic depolarization in the brain * Ultrasound-enhanced systemic thrombolysis * Weber's syndrome * World Stroke DayReferences
Further reading
* *External links
*DRAGON Score for Post-Thrombolysis
THRIVE score for stroke outcome
National Institute of Neurological Disorders and Stroke
{{Authority control Stroke, Causes of death Wikipedia medicine articles ready to translate Wikipedia emergency medicine articles ready to translate